-
Special Article
Brazilian guidelines for the management of brain-dead potential organ donors. The task force of the Associação de Medicina Intensiva Brasileira, Associação Brasileira de Transplantes de Órgãos, Brazilian Research in Critical Care Network, and the General Coordination of the National Transplant System
Rev Bras Ter Intensiva. 2021;33(1):1-11
Abstract
Special ArticleBrazilian guidelines for the management of brain-dead potential organ donors. The task force of the Associação de Medicina Intensiva Brasileira, Associação Brasileira de Transplantes de Órgãos, Brazilian Research in Critical Care Network, and the General Coordination of the National Transplant System
Rev Bras Ter Intensiva. 2021;33(1):1-11
DOI 10.5935/0103-507X.20210001
Views5See moreAbstract
Objective:
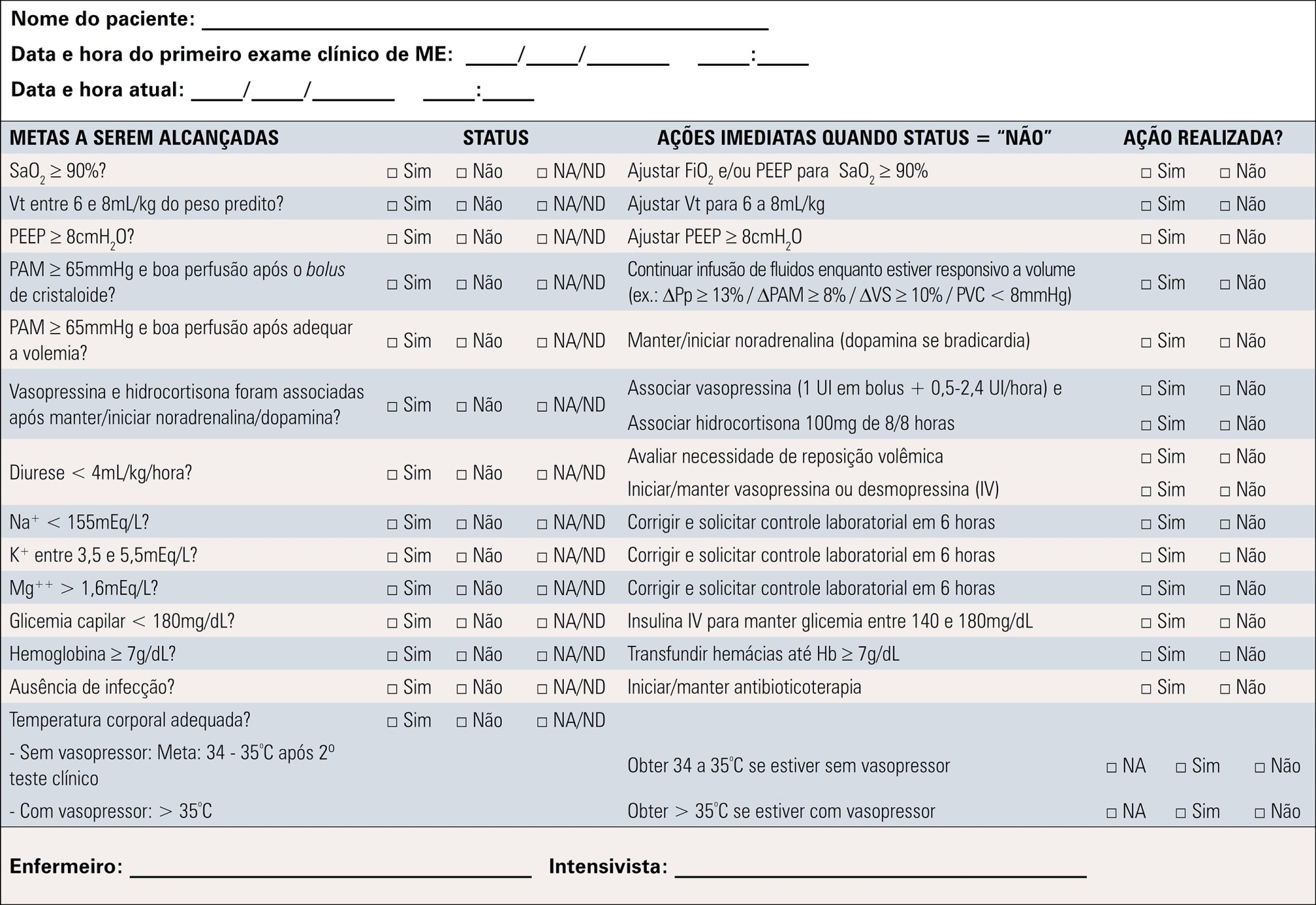
To contribute to updating the recommendations for brain-dead potential organ donor management.
Methods:
A group of 27 experts, including intensivists, transplant coordinators, transplant surgeons, and epidemiologists, answered questions related to the following topics were divided into mechanical ventilation, hemodynamics, endocrine-metabolic management, infection, body temperature, blood transfusion, and checklists use. The outcomes considered were cardiac arrests, number of organs removed or transplanted as well as function / survival of transplanted organs. The quality of evidence of the recommendations was assessed using the Grading of Recommendations Assessment, Development, and Evaluation system to classify the recommendations.
Results:
A total of 19 recommendations were drawn from the expert panel. Of these, 7 were classified as strong, 11 as weak and 1 was considered a good clinical practice.
Conclusion:
Despite the agreement among panel members on most recommendations, the grade of recommendation was mostly weak.
-
Special Article
First Brazilian recommendation on physiotherapy with sensory motor stimulation in newborns and infants in the intensive care unit
Rev Bras Ter Intensiva. 2021;33(1):12-30
Abstract
Special ArticleFirst Brazilian recommendation on physiotherapy with sensory motor stimulation in newborns and infants in the intensive care unit
Rev Bras Ter Intensiva. 2021;33(1):12-30
DOI 10.5935/0103-507X.20210002
Views2Abstract
Objective:
To present guidelines on sensory motor stimulation for newborns and infants in the intensive care unit.
Methods:
We employed a mixed methods design with a systematic review of the literature and recommendations based on scientific evidence and the opinions of physiotherapists with neonatal expertise. The research included studies published between 2010 and 2018 in the MEDLINE® and Cochrane databases that included newborns (preterm and term) and infants (between 28 days and 6 months of age) hospitalized in the intensive care unit and submitted to sensory motor stimulation methods. The studies found were classified according to the GRADE score by five physiotherapists in different regions of Brazil and presented at eight Scientific Congresses held to discuss the clinical practice guidelines.
Results:
We included 89 articles to construct the clinical practice guidelines. Auditory, gustatory and skin-to-skin stimulation stand out for enhancing vital signs, and tactile-kinesthetic massage and multisensory stimulation stand out for improving weight or sucking.
Conclusion:
Although all modalities have good ratings for pain or stress control, it is recommended that sensory motor stimulation procedures be tailored to the infant’s specific needs and that interventions and be carried out by expert professionals.
Keywords:Child developmentInfantInfant, newbornIntensive care units, neonatalNeuropsychomotor developmentPsychomotor performanceSensory motor stimulationSee more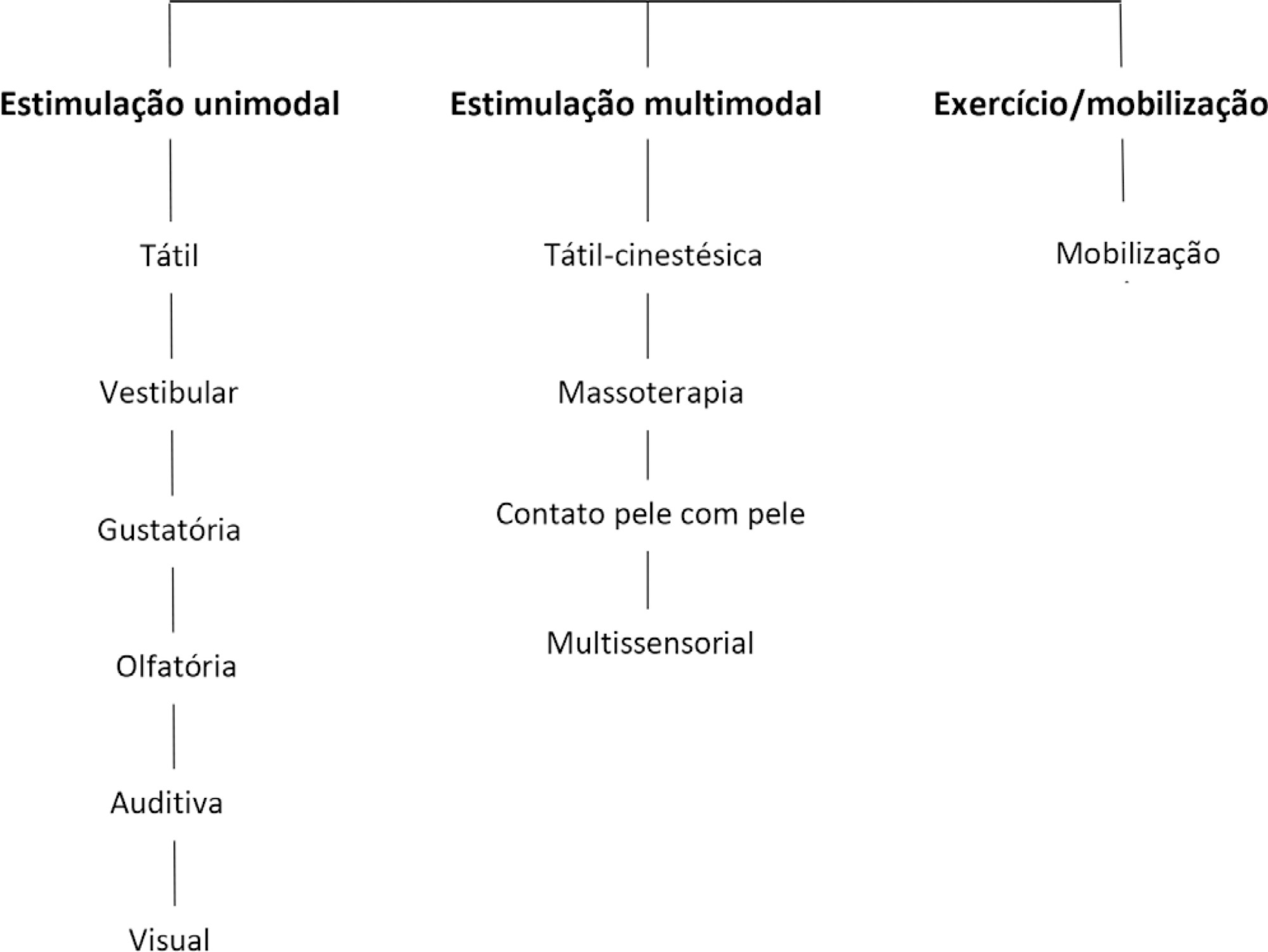
-
Special Article
Quality of life and long-term outcomes after hospitalization for COVID-19: Protocol for a prospective cohort study (Coalition VII)
Rev Bras Ter Intensiva. 2021;33(1):31-37
Abstract
Special ArticleQuality of life and long-term outcomes after hospitalization for COVID-19: Protocol for a prospective cohort study (Coalition VII)
Rev Bras Ter Intensiva. 2021;33(1):31-37
DOI 10.5935/0103-507X.20210003
Views0See moreAbstract
Introduction:
The long-term effects caused by COVID-19 are unknown. The present study aims to assess factors associated with health-related quality of life and long-term outcomes among survivors of hospitalization for COVID-19 in Brazil.
Methods:
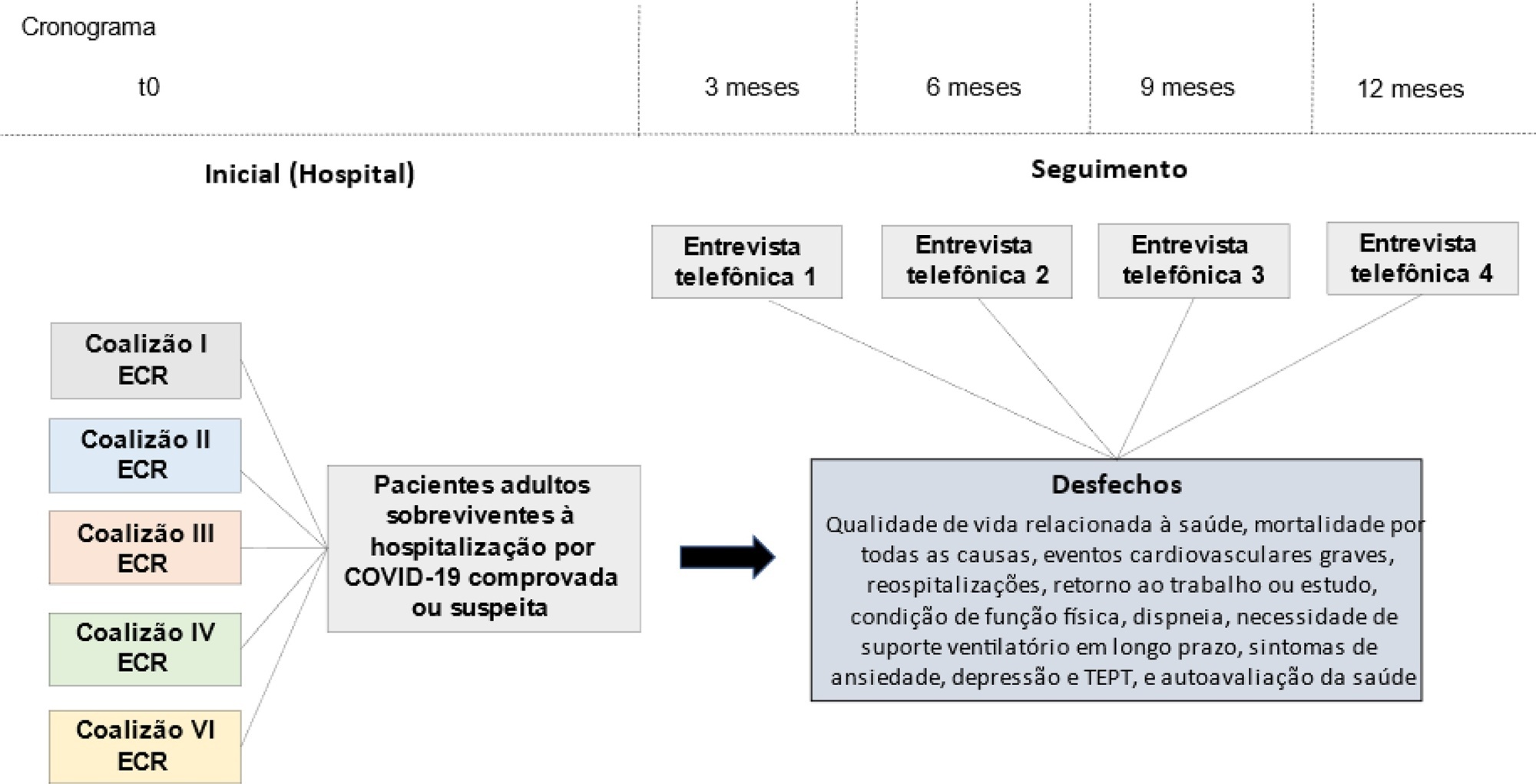
This is a multicenter prospective cohort study nested in five randomized clinical trials designed to assess the effects of specific COVID-19 treatments in over 50 centers in Brazil. Adult survivors of hospitalization due to proven or suspected SARS-CoV-2 infection will be followed-up for a period of 1 year by means of structured telephone interviews. The primary outcome is the 1-year utility score of health-related quality of life assessed by the EuroQol-5D3L. Secondary outcomes include all-cause mortality, major cardiovascular events, rehospitalizations, return to work or study, physical functional status assessed by the Lawton-Brody Instrumental Activities of Daily Living, dyspnea assessed by the modified Medical Research Council dyspnea scale, need for long-term ventilatory support, symptoms of anxiety and depression assessed by the Hospital Anxiety and Depression Scale, symptoms of posttraumatic stress disorder assessed by the Impact of Event Scale-Revised, and self-rated health assessed by the EuroQol-5D3L Visual Analog Scale. Generalized estimated equations will be performed to test the association between five sets of variables (1- demographic characteristics, 2- premorbid state of health, 3- characteristics of acute illness, 4- specific COVID-19 treatments received, and 5- time-updated postdischarge variables) and outcomes.
Ethics and dissemination:
The study protocol was approved by the Research Ethics Committee of all participant institutions. The results will be disseminated through conferences and peer-reviewed journals.
-
Special Article
Accountability for reasonableness and criteria for admission, triage and discharge in intensive care units: an analysis of current ethical recommendations
Rev Bras Ter Intensiva. 2021;33(1):38-47
Abstract
Special ArticleAccountability for reasonableness and criteria for admission, triage and discharge in intensive care units: an analysis of current ethical recommendations
Rev Bras Ter Intensiva. 2021;33(1):38-47
DOI 10.5935/0103-507X.20210004
Views0See moreAbstract
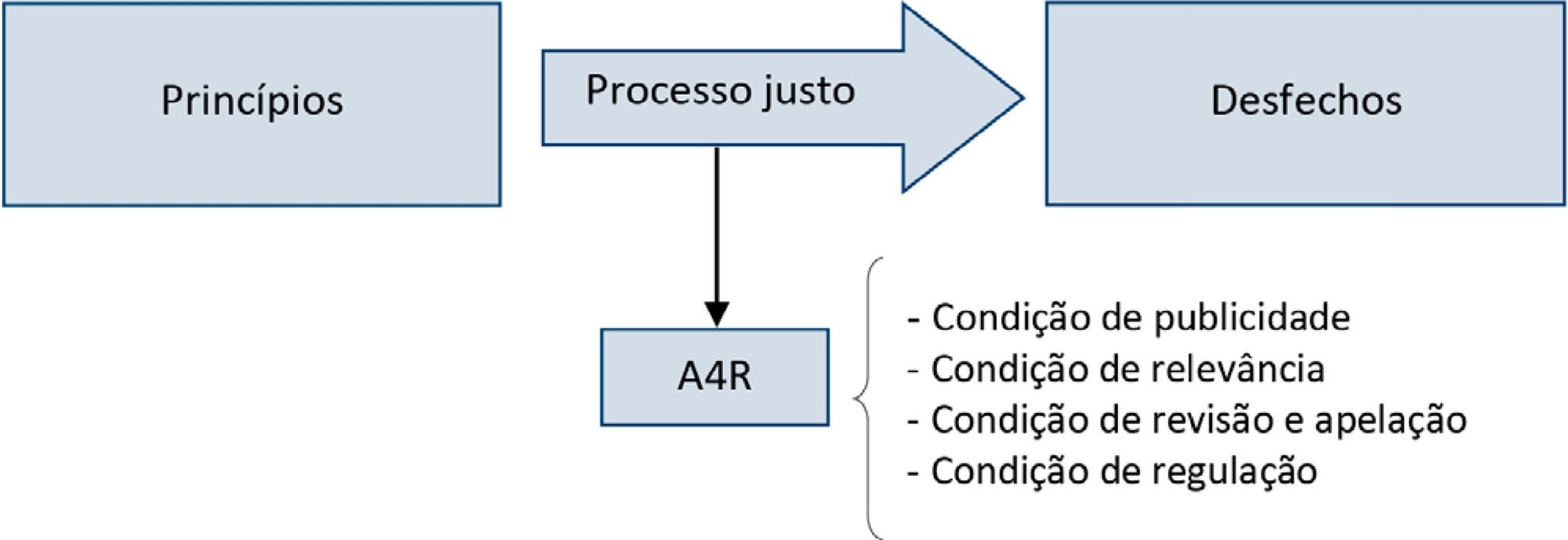
Triage for intensive care unit admission is a frequent event and is associated to worse clinical outcomes. The process of triage is variable and may be influenced by biases and prejudices, which could lead to potentially unfair decisions. The Brazilian Federal Council of Medicine (Conselho Federal de Medicina) has recently released a guideline for intensive care unit admission and discharge. The aim of this paper is to evaluate the ethical dilemmas related to the implementation of this guideline, through the accountability for reasonabless approach, known as A4R, as elaborated by Norman Daniels. We conclude that the guideline contemplates A4R conditions, but we observe that there is a need for indication of A4R-concordant criteria to operationalize the guidelines.
-
Special Article
Consensus for the management of analgesia, sedation and delirium in adults with COVID-19-associated acute respiratory distress syndrome
Rev Bras Ter Intensiva. 2021;33(1):48-67
Abstract
Special ArticleConsensus for the management of analgesia, sedation and delirium in adults with COVID-19-associated acute respiratory distress syndrome
Rev Bras Ter Intensiva. 2021;33(1):48-67
DOI 10.5935/0103-507X.20210005
Views2See moreABSTRACT
Objective:
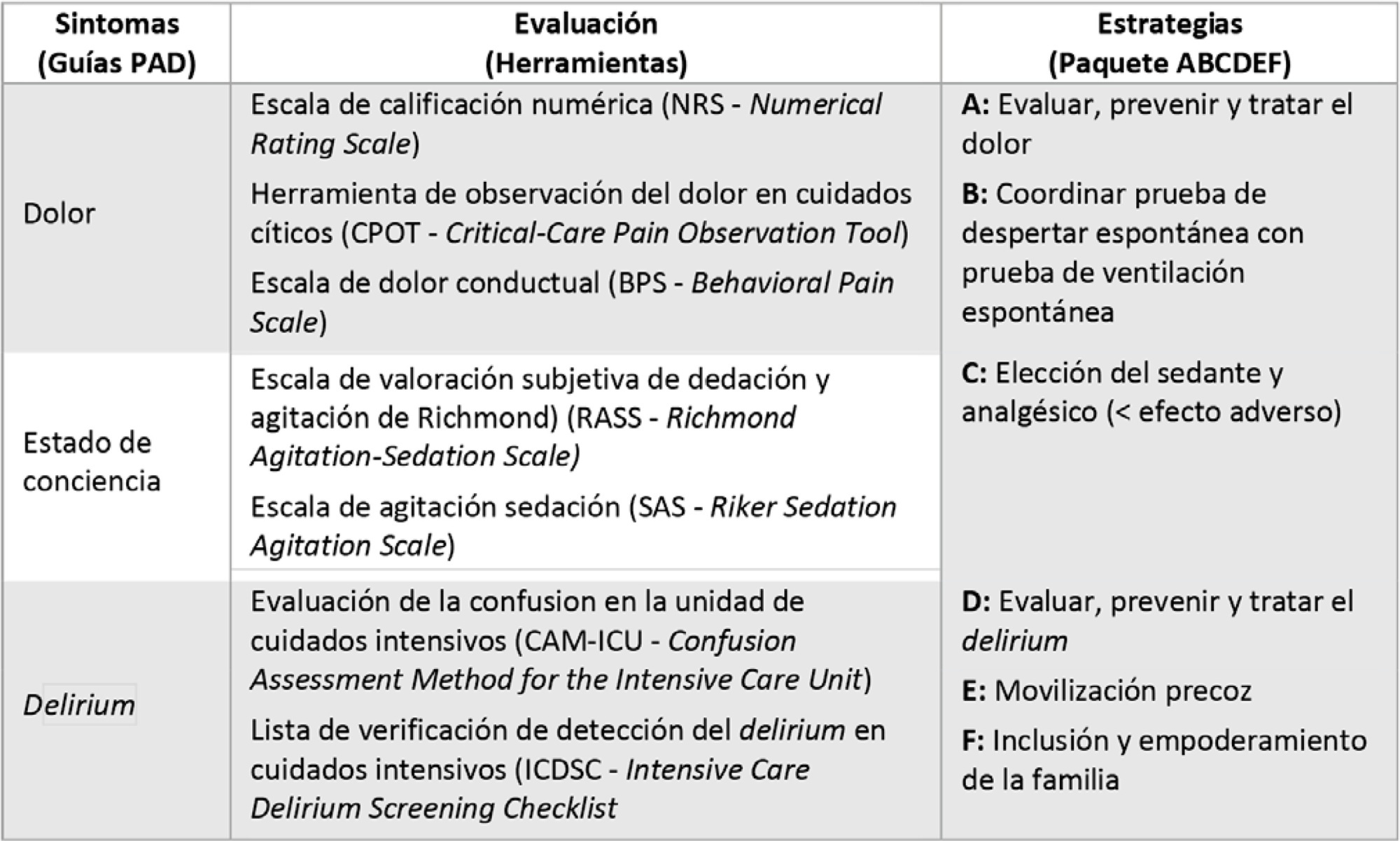
To propose agile strategies for a comprehensive approach to analgesia, sedation, delirium, early mobility and family engagement for patients with COVID-19-associated acute respiratory distress syndrome, considering the high risk of infection among health workers, the humanitarian treatment that we must provide to patients and the inclusion of patients’ families, in a context lacking specific therapeutic strategies against the virus globally available to date and a potential lack of health resources.
Methods:
A nonsystematic review of the scientific evidence in the main bibliographic databases was carried out, together with national and international clinical experience and judgment. Finally, a consensus of recommendations was made among the members of the Committee for Analgesia, Sedation and Delirium of the Sociedad Argentina de Terapia Intensiva.
Results:
Recommendations were agreed upon, and tools were developed to ensure a comprehensive approach to analgesia, sedation, delirium, early mobility and family engagement for adult patients with acute respiratory distress syndrome due to COVID-19.
Discussion:
Given the new order generated in intensive therapies due to the advancing COVID-19 pandemic, we propose to not leave aside the usual good practices but to adapt them to the particular context generated. Our consensus is supported by scientific evidence and national and international experience and will be an attractive consultation tool in intensive therapies.
-
Original Article
Changes in the management and clinical outcomes of critically ill patients without COVID-19 during the pandemic
Rev Bras Ter Intensiva. 2021;33(1):68-74
Abstract
Original ArticleChanges in the management and clinical outcomes of critically ill patients without COVID-19 during the pandemic
Rev Bras Ter Intensiva. 2021;33(1):68-74
DOI 10.5935/0103-507X.20210006
Views0Abstract
Objective:
To analyze whether changes in medical care due to the application of COVID-19 protocols affected clinical outcomes in patients without COVID-19 during the pandemic.
Methods:
This was a retrospective, observational cohort study carried out in a thirty-eight-bed surgical and medical intensive care unit of a high complexity private hospital. Patients with respiratory failure admitted to the intensive care unit during March and April 2020 and the same months in 2019 were selected. We compared interventions and outcomes of patients without COVID-19 during the pandemic with patients admitted in 2019. The main variables analyzed were intensive care unit respiratory management, number of chest tomography scans and bronchoalveolar lavages, intensive care unit complications, and status at hospital discharge.
Results:
In 2020, a significant reduction in the use of a high-flow nasal cannula was observed: 14 (42%) in 2019 compared to 1 (3%) in 2020. Additionally, in 2020, a significant increase was observed in the number of patients under mechanical ventilation admitted to the intensive care unit from the emergency department, 23 (69%) compared to 11 (31%) in 2019. Nevertheless, the number of patients with mechanical ventilation after 5 days of admission was similar in both years: 24 (69%) in 2019 and 26 (79%) in 2020.
Conclusion:
Intensive care unit protocols based on international recommendations for the COVID-19 pandemic have produced a change in non-COVID-19 patient management. We observed a reduction in the use of a high-flow nasal cannula and an increased number of tracheal intubations in the emergency department. However, no changes in the percentage of intubated patients in the intensive care unit, the number of mechanical ventilation days or the length of stay in intensive care unit.
Keywords:Coronavirus infectionsCOVID-19Critical careNoninvasive ventilationPandemicsRespiratory insufficiencySARS-CoV-2See more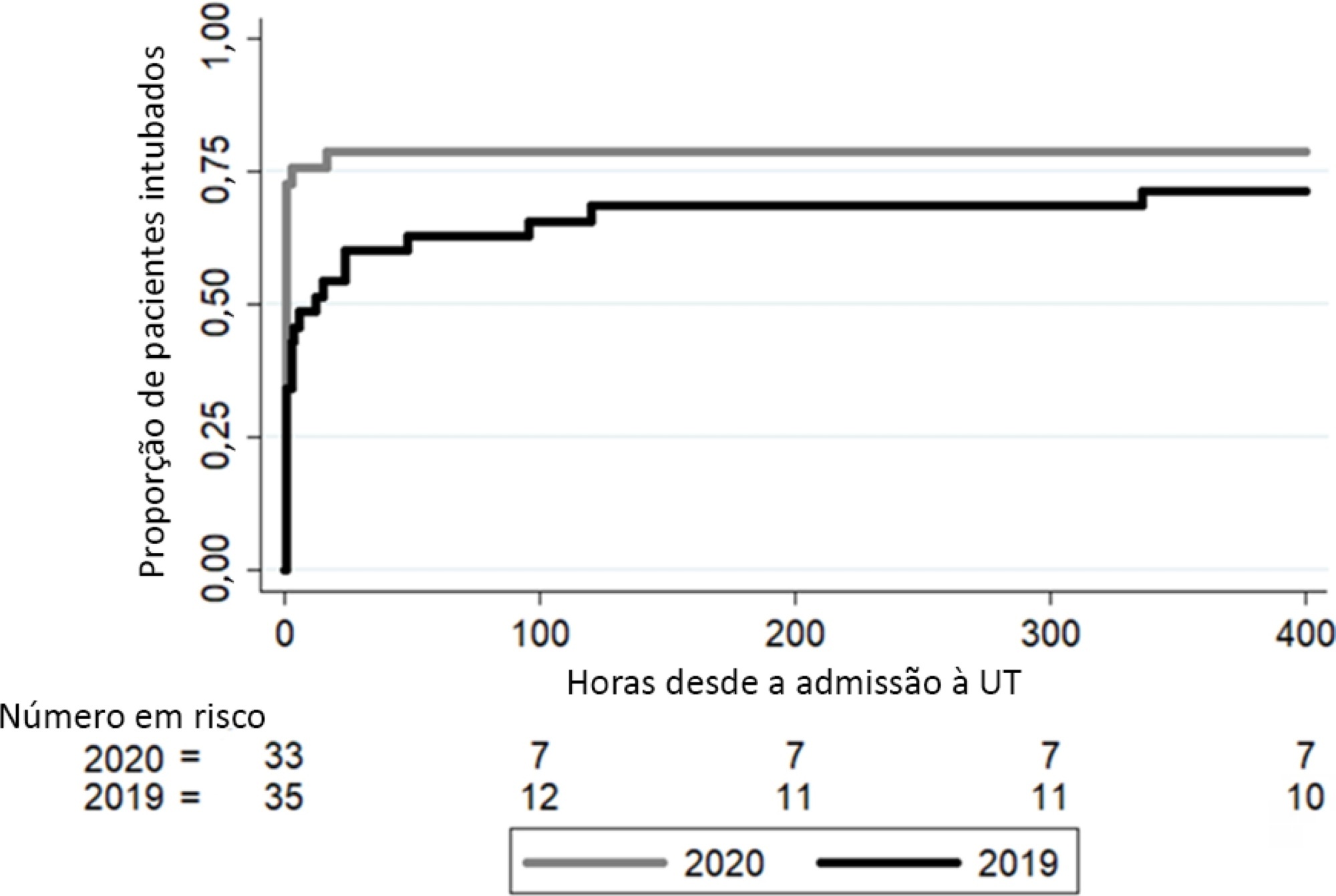
-
Original Article
Characterization of pulmonary impairment associated with COVID-19 in patients requiring mechanical ventilation
Rev Bras Ter Intensiva. 2021;33(1):75-81
Abstract
Original ArticleCharacterization of pulmonary impairment associated with COVID-19 in patients requiring mechanical ventilation
Rev Bras Ter Intensiva. 2021;33(1):75-81
DOI 10.5935/0103-507X.20210007
Views0ABSTRACT
Objective:
To detect early respiratory and hemodynamic instability to characterize pulmonary impairment in patients with severe COVID-19.
Methods:
We retrospectively analyzed data collected from COVID-19 patients suffering from acute respiratory failure requiring intubation and mechanical ventilation. We used transpulmonary thermodilution assessment with a PiCCO™ device. We collected demographic, respiratory, hemodynamic and echocardiographic data within the first 48 hours after admission. Descriptive statistics were used to summarize the data.
Results:
Fifty-three patients with severe COVID-19 were admitted between March 22nd and April 7th. Twelve of them (22.6%) were monitored with a PiCCO™ device. Upon admission, the global-end diastolic volume indexed was normal (mean 738.8mL ± 209.2) and moderately increased at H48 (879mL ± 179), and the cardiac index was subnormal (2.84 ± 0.65). All patients showed extravascular lung water over 8mL/kg on admission (17.9 ± 8.9). We did not identify any argument for cardiogenic failure.
Conclusion:
In the case of severe COVID-19 pneumonia, hemodynamic and respiratory presentation is consistent with pulmonary edema without evidence of cardiogenic origin, favoring the diagnosis of acute respiratory distress syndrome.
Keywords:acute respiratory distress syndromeCoronavirus infectionsCOVID-19Pulmonary edemaSARS-CoV-2ThermodilutionSee more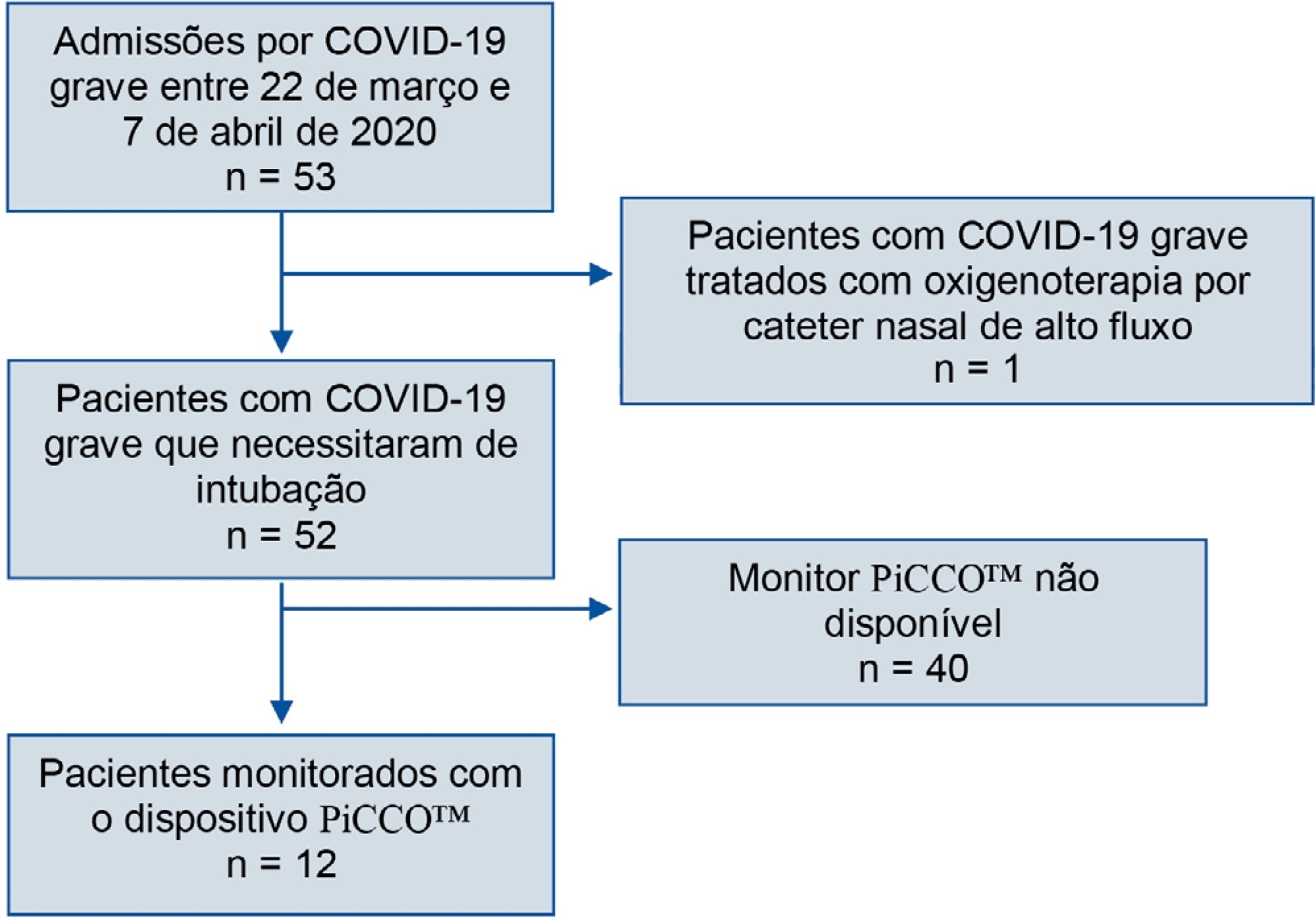
-
Original Article
Nursing workload associated with the frequency of multidisciplinary rounds: a cross-sectional study
Rev Bras Ter Intensiva. 2021;33(1):82-87
Abstract
Original ArticleNursing workload associated with the frequency of multidisciplinary rounds: a cross-sectional study
Rev Bras Ter Intensiva. 2021;33(1):82-87
DOI 10.5935/0103-507X.20210008
Views1See moreAbstract
Objective:
To assess the frequency of multidisciplinary rounds during ICU days, to evaluate the participation of diverse healthcare professionals, to identify the reasons why rounds were not performed on specific days, and whether bed occupancy rate and nurse workload were associated with the conduction of multidisciplinary rounds.
Methods:
We performed a cross-sectional study to assess the frequency of multidisciplinary rounds in four intensive care units in a cancer center. We also collected data on rates of professional participation, reasons for not performing rounds when they did not occur, and daily bed occupancy rates and assessed nurse workload by measuring the Nursing Activity Score.
Results:
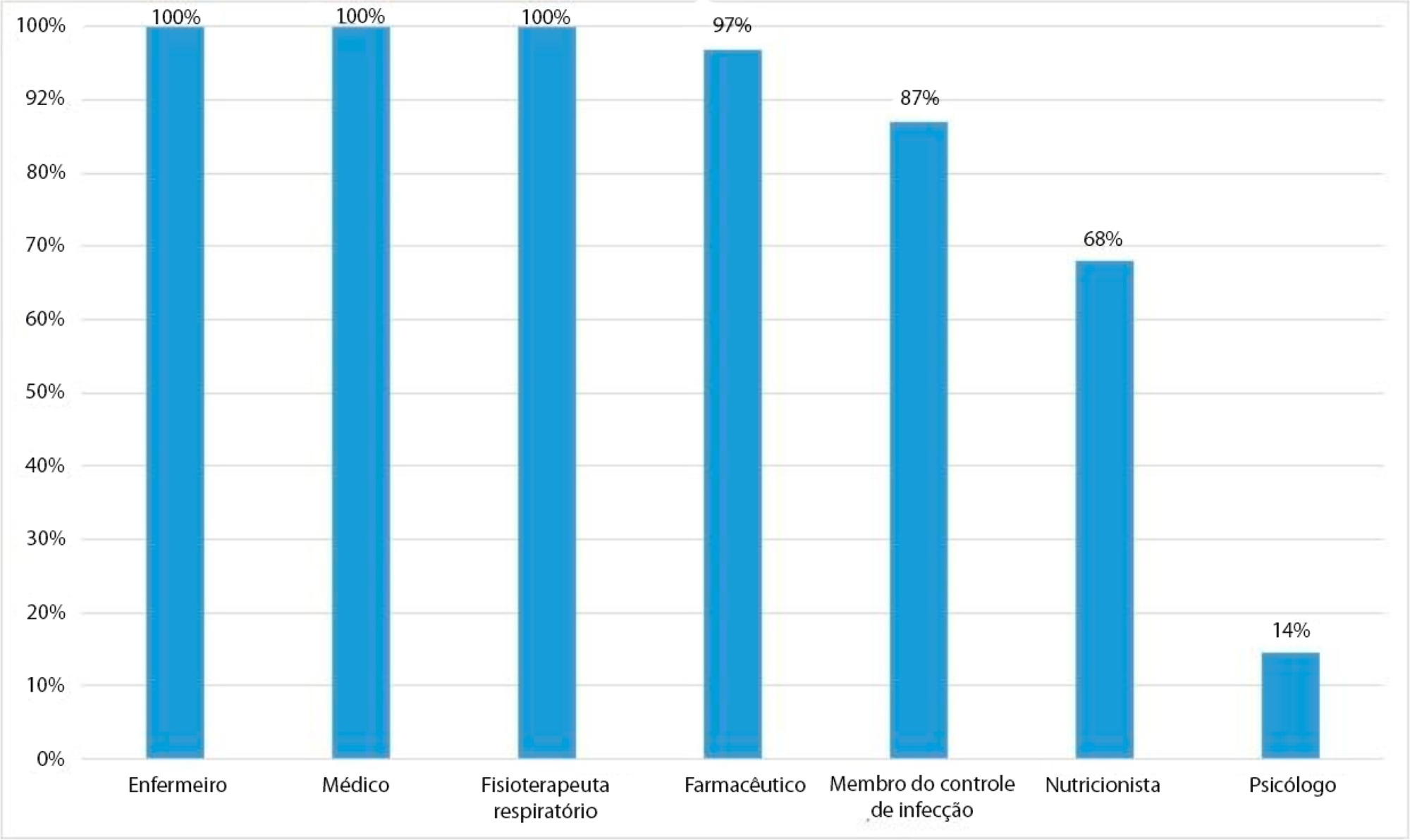
Rounds were conducted on 595 (65.8%) of 889 surveyed intensive care unit days. Nurses, physicians, respiratory therapists, pharmacists, and infection control practitioners participated most often. Rounds did not occur due to admission of new patients at the scheduled time (136; 44.7%) and involvement of nurses in activities unrelated to patients’ care (97; 31.9%). In multivariate analysis, higher Nursing Activity Scores were associated with greater odds of conducting multidisciplinary rounds (OR = 1.06; 95%CI 1.04 – 1.10; p < 0.01), whereas bed occupancy rates were not (OR = 0.99; 95%CI 0.97 - 1.00; p = 0.18).
Conclusion:
Multidisciplinary rounds were conducted on less than two-thirds of surveyed intensive care unit days. Many rounds were cancelled due to activities unrelated to patient care. Unexpectedly, increased workload was associated with higher odds of conducting rounds. Workload is a possible trigger to discuss daily goals to improve patient outcomes and to enhance the effectiveness of multidisciplinary teams.
-
Original Article
Is the p-value properly interpreted by critical care professionals? Online survey
Rev Bras Ter Intensiva. 2021;33(1):88-95
Abstract
Original ArticleIs the p-value properly interpreted by critical care professionals? Online survey
Rev Bras Ter Intensiva. 2021;33(1):88-95
DOI 10.5935/0103-507X.20210009
Views0ABSTRACT
Objective:
To determine the prevalence of and risk factors for insufficient knowledge related to p-values among critical care physicians and respiratory therapists in Argentina.
Methods:
This cross-sectional online survey contained 25 questions about respondents’ characteristics, self-perception and p-value knowledge (theory and practice). Descriptive and multivariable logistic regression analyses were conducted.
Results:
Three hundred seventy-six respondents were analyzed. Two hundred thirty-seven respondents (63.1%) did not know about p-values. According to the multivariable logistic regression analysis, a lack of training on scientific research methodology (adjusted OR 2.50; 95%CI 1.37 – 4.53; p = 0.003) and the amount of reading (< 6 scientific articles per year; adjusted OR 3.27; 95%CI 1.67 - 6.40; p = 0.001) were found to be independently associated with the respondents’ lack of p-value knowledge.
Conclusion:
The prevalence of insufficient knowledge regarding p-values among critical care physicians and respiratory therapists in Argentina was 63%. A lack of training on scientific research methodology and the amount of reading (< 6 scientific articles per year) were found to be independently associated with the respondents’ lack of p-value knowledge.
Keywords:Biomedical research/statistics & numerical dataBiostatisticsData interpretation, statisticalEvidence-based medicineHypothesis testingprevalenceSee more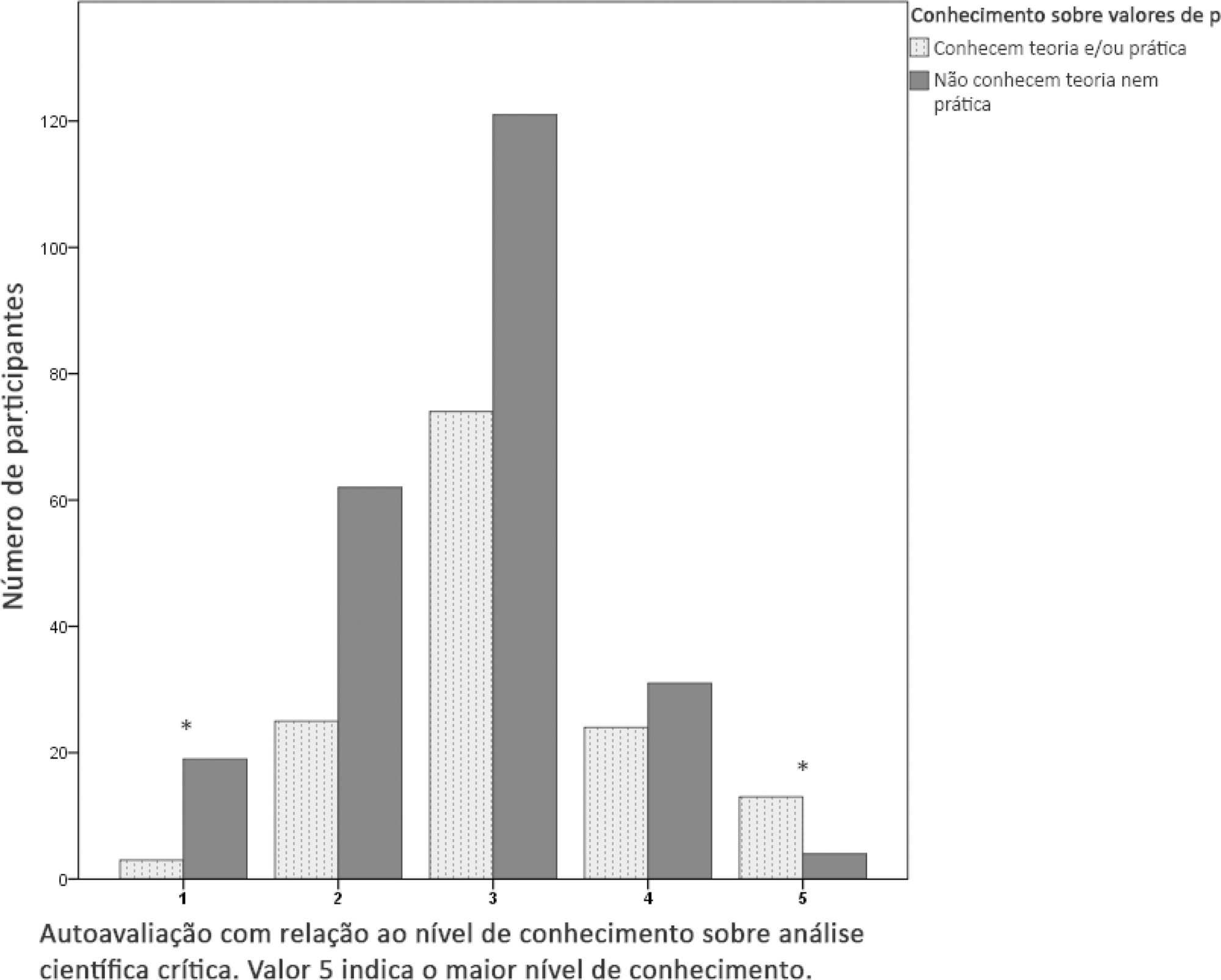
-
Original Article
Changes in cardiac arrest profiles after the implementation of a Rapid Response Team
Rev Bras Ter Intensiva. 2021;33(1):96-101
Abstract
Original ArticleChanges in cardiac arrest profiles after the implementation of a Rapid Response Team
Rev Bras Ter Intensiva. 2021;33(1):96-101
DOI 10.5935/0103-507X.20210010
Views1See moreABSTRACT
Objective:
To evaluate changes in the characteristics of in-hospital cardiac arrest after the implementation of a Rapid Response Team.
Methods:
This was a prospective observational study of in-hospital cardiac arrest that occurred from January 2013 to December 2017. The exclusion criterion was in-hospital cardiac arrest in the intensive care unit, emergency room or operating room. The Rapid Response Team was implemented in July 2014 in the study hospital. Patients were classified into two groups: a Pre-Rapid Response Team (in-hospital cardiac arrest before Rapid Response Team implementation) and a Post-Rapid Response Team (in-hospital cardiac arrest after Rapid Response Team implementation). Patients were followed until hospital discharge or death.
Results:
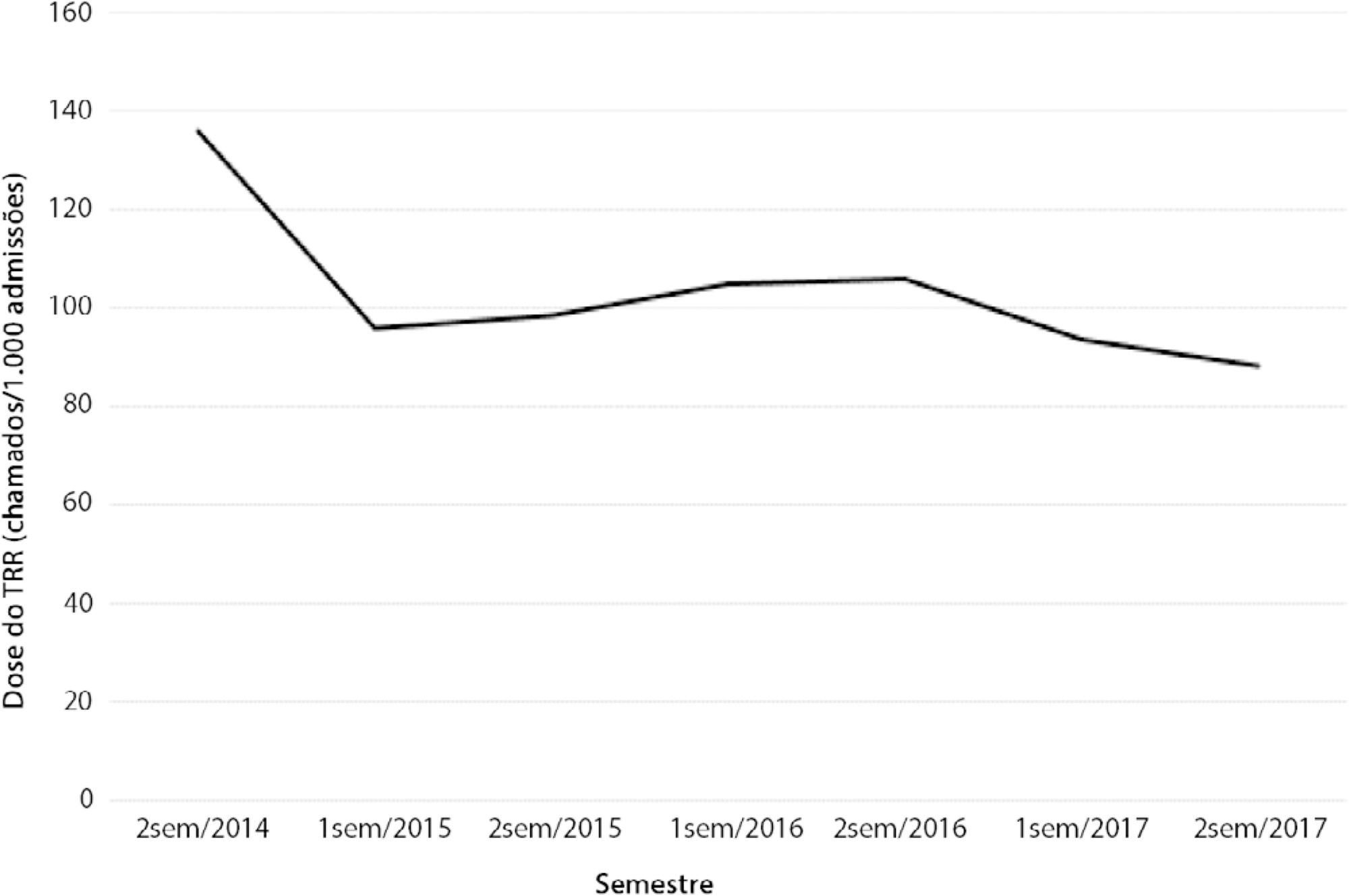
We had a total of 308 cardiac arrests (64.6 ± 15.2 years, 60.3% men, 13.9% with initial shockable rhythm). There was a decrease from 4.2 to 2.5 in-hospital cardiac arrest/1000 admissions after implementation of the Rapid Response Team, and we had approximately 124 calls/1000 admissions. Pre-Rapid Response Team cardiac arrest was associated with more hypoxia (29.4 versus 14.3%; p = 0.006) and an altered respiratory rate (14.7 versus 4.2%; p = 0.004) compared with post-Rapid Response Team cardiac arrest. Cardiac arrest due to hypoxia was more common before Rapid Response Team implementation (61.2 versus 38.1%, p < 0.001). In multivariate analysis, return of spontaneous circulation was associated with shockable rhythm (OR 2.97; IC95% 1.04 - 8.43) and witnessed cardiac arrest (OR 2.52; IC95% 1.39 - 4.59) but not with Rapid Response Team implementation (OR 1.40; IC95% 0.70 - 2.81) or premonitory signs (OR 0.71; IC95% 0.39 - 1.28). In multivariate analysis, in-hospital mortality was associated with non-shockable rhythm (OR 5.34; IC95% 2.28 - 12.53) and age (OR 1.03; IC95% 1.01 - 1.05) but not with Rapid Response Team implementation (OR 0.89; IC95% 0.40 - 2.02).
Conclusion:
Even though Rapid Response Team implementation is associated with a reduction in in-hospital cardiac arrest, it was not associated with the mortality of in-hospital cardiac arrest victims. A significant decrease in cardiac arrests due to respiratory causes was noted after Rapid Response Team implementation.
-
Original Article
Cross-cultural adaptation of the Richmond Agitation-Sedation Scale to Brazilian Portuguese for the evaluation of sedation in pediatric intensive care
Rev Bras Ter Intensiva. 2021;33(1):102-110
Abstract
Original ArticleCross-cultural adaptation of the Richmond Agitation-Sedation Scale to Brazilian Portuguese for the evaluation of sedation in pediatric intensive care
Rev Bras Ter Intensiva. 2021;33(1):102-110
DOI 10.5935/0103-507X.20210011
Views0ABSTRACT
Objective:
To perform a cross-cultural adaptation of the Richmond Agitation-Sedation Scale (RASS) to Brazilian Portuguese for the evaluation of sedation in pediatric intensive care.
Methods:
Cross-cultural adaptation process including the conceptual, item, semantic and operational equivalence stages according to current recommendations.
Results:
Pretests, divided into two stages, included 30 professionals from the pediatric intensive care unit of a university hospital, who administered the translated RASS to patients aged 29 days to 18 years. The pretests showed a content validity index above 0.90 for all items: 0.97 in the first stage of pretests and 0.99 in the second.
Conclusion:
The cross-cultural adaptation of RASS to Brazilian Portuguese resulted in a version with excellent comprehensibility and acceptability in a pediatric intensive care setting. Reliability and validity studies should be performed to evaluate the psychometric properties of the Brazilian Portuguese version of the RASS.
Keywords:Conscious sedationCross-cultural comparisonDeep sedationIntensive care units, pediatricTranslatingSee more -
Original Article
Hypothermia related to continuous renal replacement therapy: incidence and associated factors
Rev Bras Ter Intensiva. 2021;33(1):111-118
Abstract
Original ArticleHypothermia related to continuous renal replacement therapy: incidence and associated factors
Rev Bras Ter Intensiva. 2021;33(1):111-118
DOI 10.5935/0103-507X.20210012
Views0See moreABSTRACT
Objective:
To evaluate the incidence of hypothermia in patients undergoing continuous renal replacement therapy in the intensive care unit. As secondary objectives, we determined associated factors and compared the occurrence of hypothermia between two modalities of continuous renal replacement therapy.
Methods:
A prospective cohort study was conducted with adult patients who were admitted to a clinical-surgical intensive care unit and underwent continuous renal replacement therapy in a high-complexity public university hospital in southern Brazil from April 2017 to July 2018. Hypothermia was defined as a body temperature ≤ 35ºC. The patients included in the study were followed for the first 48 hours of continuous renal replacement therapy. The researchers collected data from medical records and continuous renal replacement therapy records.
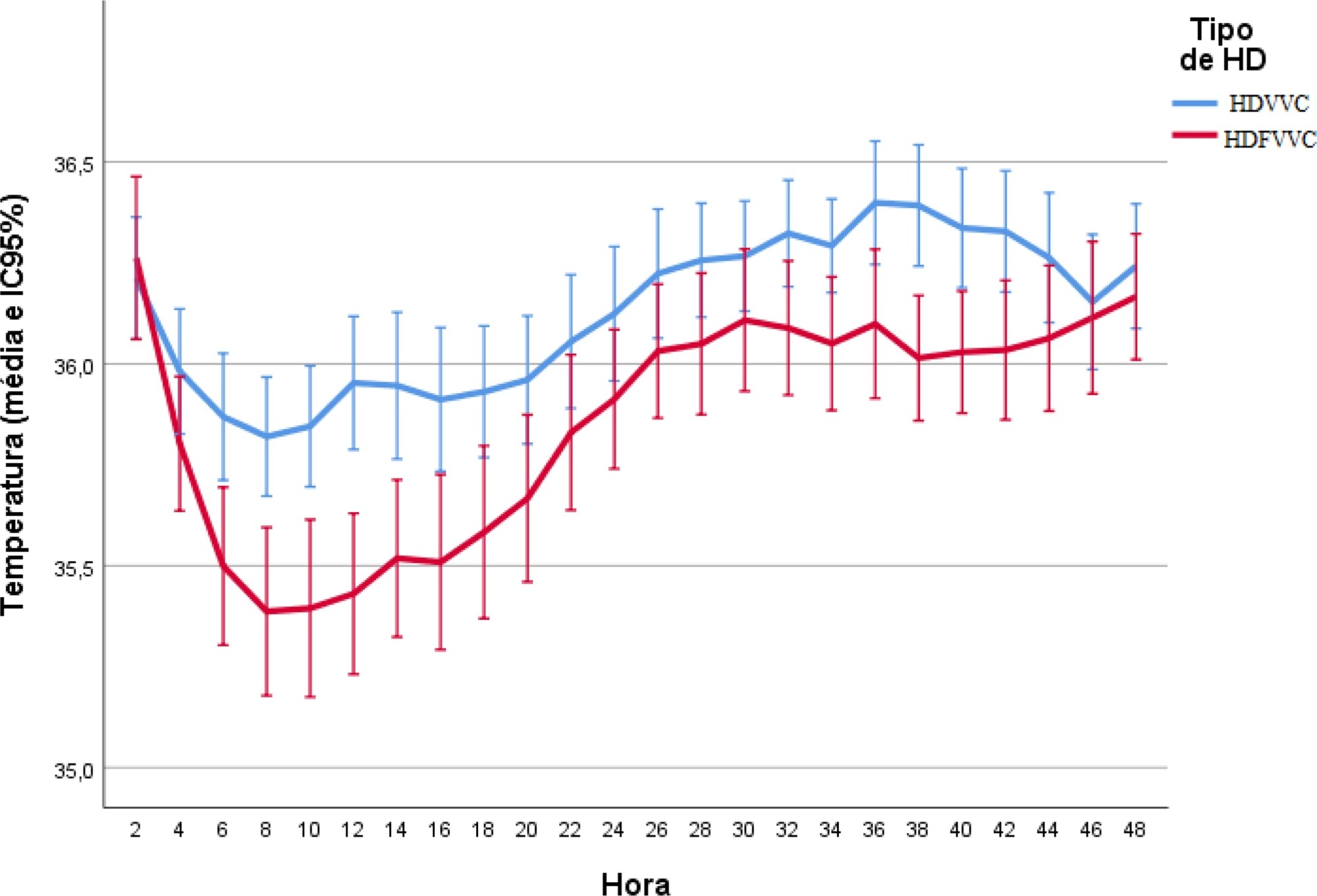
Results:
A total of 186 patients were equally distributed between two types of continuous renal replacement therapy: hemodialysis and hemodiafiltration. The incidence of hypothermia was 52.7% and was higher in patients admitted for shock (relative risk of 2.11; 95%CI 1.21 – 3.69; p = 0.009) and in those who underwent hemodiafiltration with heating in the return line (relative risk of 1.50; 95%CI 1.13 – 1.99; p = 0.005).
Conclusion:
Hypothermia in critically ill patients with continuous renal replacement therapy is frequent, and the intensive care team should be attentive, especially when there are associated risk factors.
-
Original Article
Performance of PRISM III and PIM 2 scores in a cancer pediatric intensive care unit
Rev Bras Ter Intensiva. 2021;33(1):119-124
Abstract
Original ArticlePerformance of PRISM III and PIM 2 scores in a cancer pediatric intensive care unit
Rev Bras Ter Intensiva. 2021;33(1):119-124
DOI 10.5935/0103-507X.20210013
Views0ABSTRACT
Objective:
To assess the performance of Pediatric Risk of Mortality (PRISM) III and Pediatric Index of Mortality (PIM) 2 scores in the pediatric intensive care unit.
Methods:
A retrospective cohort study. Data were retrospectively collected from medical records of all patients admitted to the pediatric intensive care unit of a cancer hospital from January 2017 to June 2018.
Results:
The mean PRISM III score was 15, and PIM 2, 24%. From the 338 studied patients, 62 (18.34%) died. The PRISM III estimated mortality was 79.52 patients (23.52%) and for PIM 2 80.19 patients (23.72%), corresponding to a standardized mortality ratio (95% confidence interval: 0.78 for PRISM II and 0.77 for PIM 2). The Hosmer-Lemeshow chi-square test was 11.56, 8df, 0.975 for PRISM II and 0.48, 8df, p = 0.999 for PIM 2. The area under the Receiver Operating Characteristic curve was 0.71 for PRISM III and 0.76 for PIM 2.
Conclusion:
Both scores overestimated mortality and have shown a regular ability to discriminate between survivors and non-survivors. Models should be developed to quantify the severity of cancer pediatric patients in Pediatric Intensive Care Units and to predict the mortality risk accounting for their peculiarities.
Keywords:Child mortalityIntensive care units, pediatricPediatric oncologyPIM 2PRISMPrognosisRisk assessmentSee more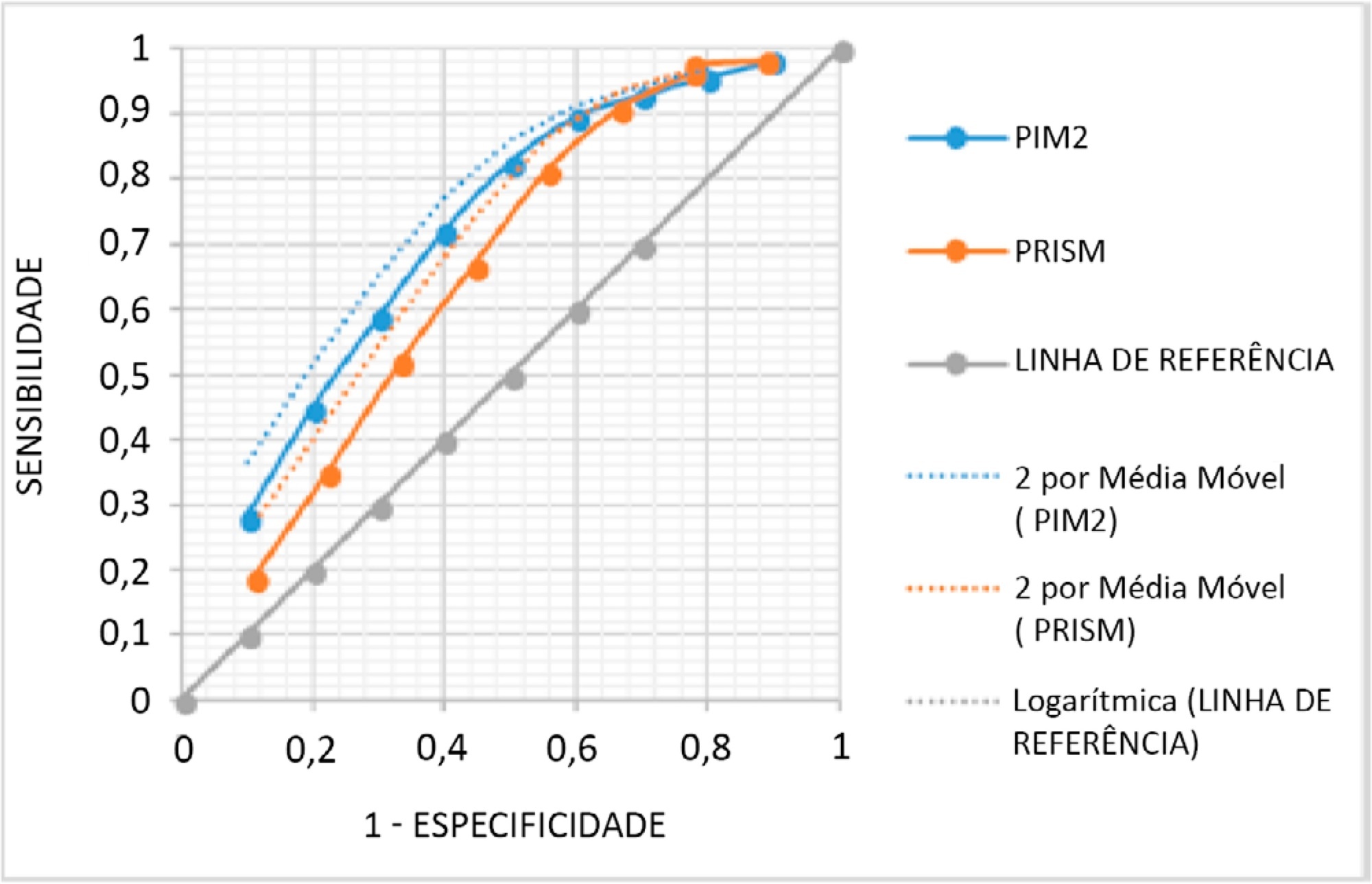
-
Original Article
Delayed intensive care unit admission from the emergency department: impact on patient outcomes. A retrospective study
Rev Bras Ter Intensiva. 2021;33(1):125-137
Abstract
Original ArticleDelayed intensive care unit admission from the emergency department: impact on patient outcomes. A retrospective study
Rev Bras Ter Intensiva. 2021;33(1):125-137
DOI 10.5935/0103-507X.20210014
Views1Abstract
Objective:
To study the impact of delayed admission by more than 4 hours on the outcomes of critically ill patients.
Methods:
This was a retrospective observational study in which adult patients admitted directly from the emergency department to the intensive care unit were divided into two groups: Timely Admission if they were admitted within 4 hours and Delayed Admission if admission was delayed for more than 4 hours. Intensive care unit length of stay and hospital/intensive care unit mortality were compared between the groups. Propensity score matching was performed to correct for imbalances. Logistic regression analysis was used to explore delayed admission as an independent risk factor for intensive care unit mortality.
Results:
During the study period, 1,887 patients were admitted directly from the emergency department to the intensive care unit, with 42% being delayed admissions. Delayed patients had significantly longer intensive care unit lengths of stay and higher intensive care unit and hospital mortality. These results were persistent after propensity score matching of the groups. Delayed admission was an independent risk factor for intensive care unit mortality (OR = 2.6; 95%CI 1.9 – 3.5; p < 0.001). The association of delay and intensive care unit mortality emerged after a delay of 2 hours and was highest after a delay of 4 hours.
Conclusion:
Delayed admission to the intensive care unit from the emergency department is an independent risk factor for intensive care unit mortality, with the strongest association being after a delay of 4 hours.
Keywords:Emergency service, hospitalHospital mortalityIntensive care unitsLength of stayrisk factorsSee more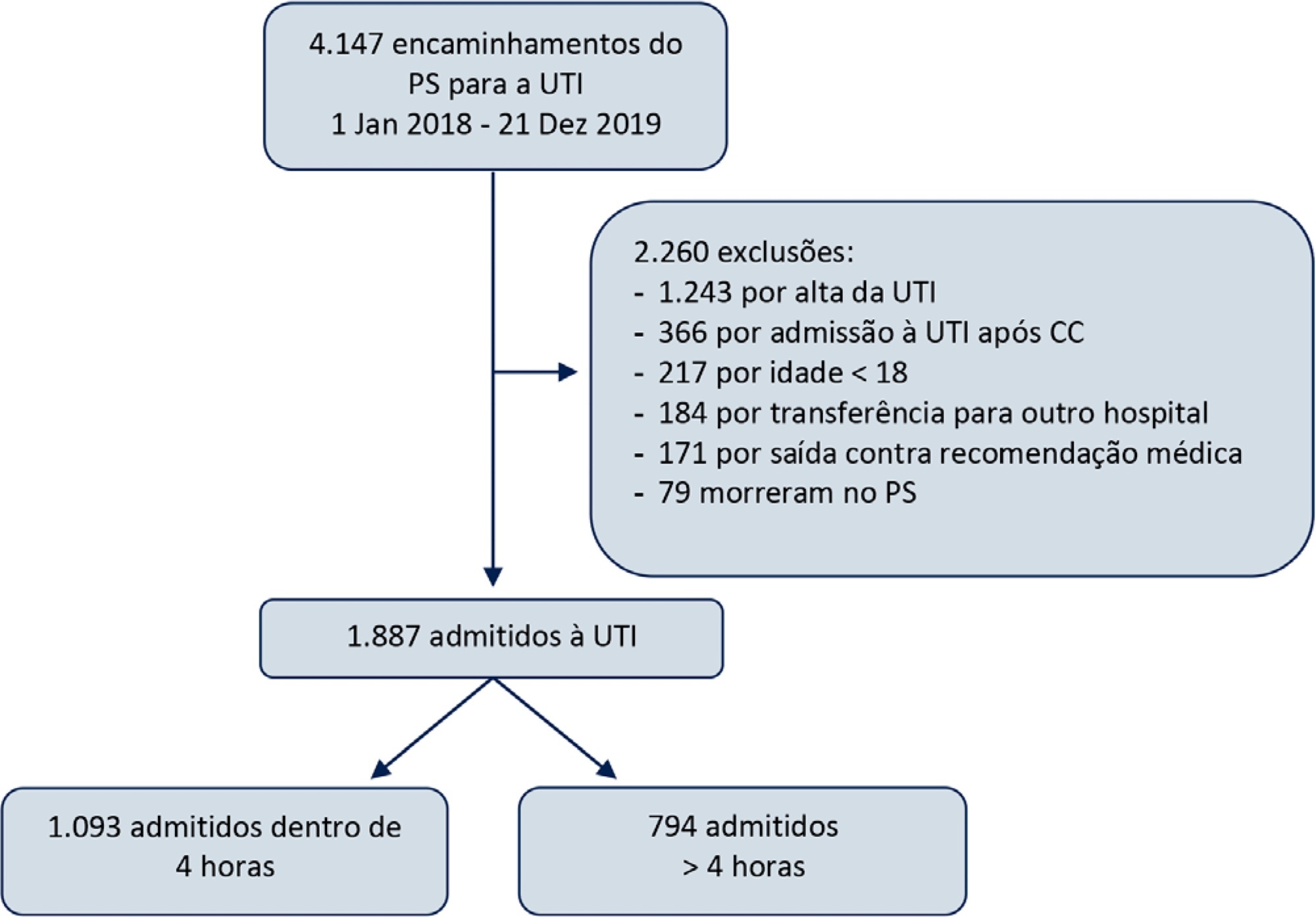
-
Original Article
GlucoSTRESS – A project to optimize glycemic control in a level C (III) Portuguese intensive care unit
Rev Bras Ter Intensiva. 2021;33(1):138-145
Abstract
Original ArticleGlucoSTRESS – A project to optimize glycemic control in a level C (III) Portuguese intensive care unit
Rev Bras Ter Intensiva. 2021;33(1):138-145
DOI 10.5935/0103-507X.20210015
Views0See moreABSTRACT
Objective:
To double the percentage of time within the 100 – 180mg/dL blood glucose range in the first three months following a phased implementation of a formal education program, and then, of an insulin therapy protocol, without entailing an increased incidence of hypoglycemia.
Methods:
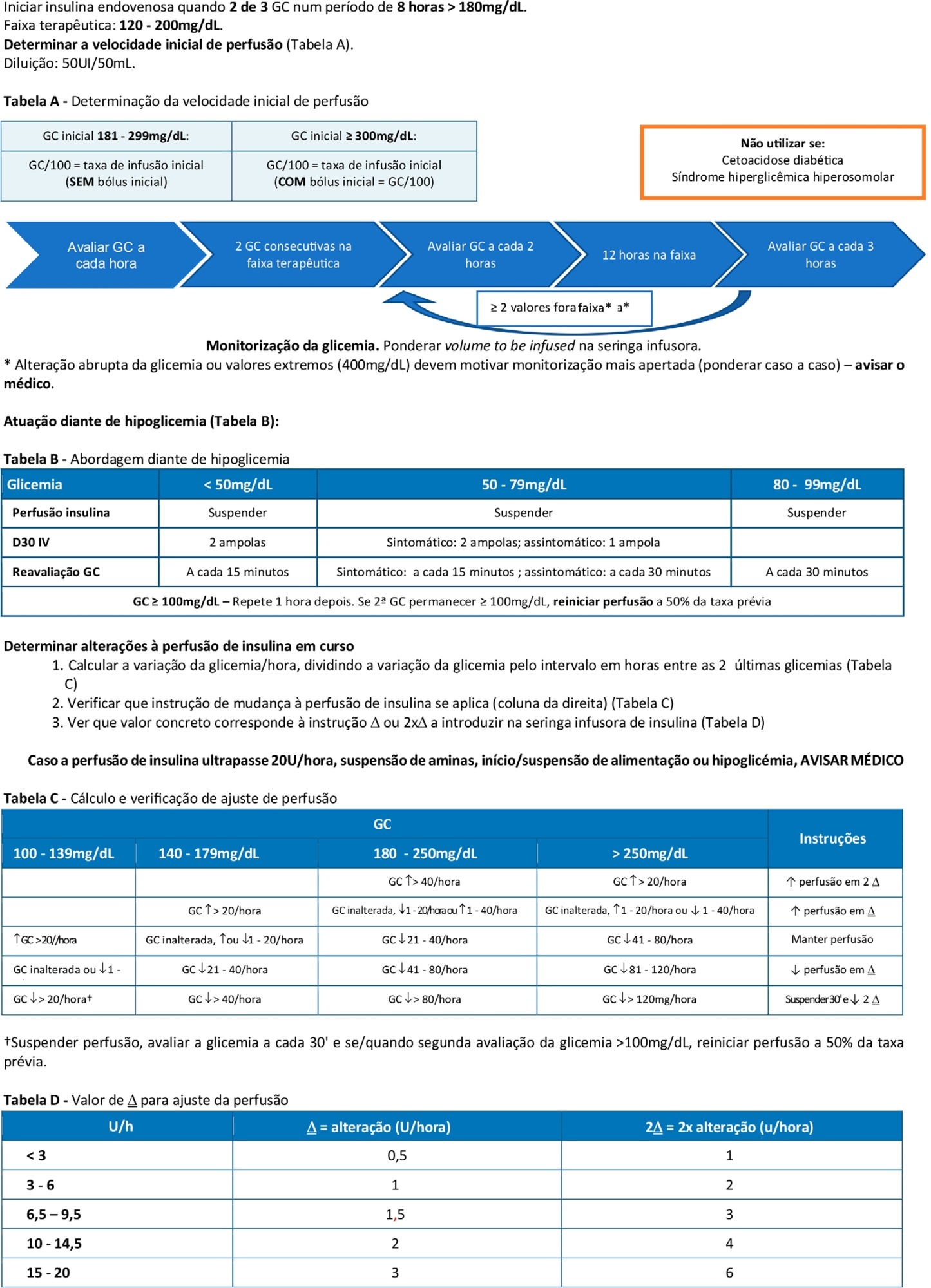
The pre-intervention glycemic control was assessed retrospectively. Next, were carried out the implementation of a formal education program, distribution of manual algorithms for intravenous insulin therapy – optimized by the users, based on the modified Yale protocol – and informal training of the nursing staff. The use of electronic blood glucose control systems was supported, and the results were recorded prospectively.
Results:
The first phase of the program (formal education) lead to improvement of the time within the euglycemic interval (28% to 37%). In the second phase, euglycemia was achieved 66% of the time, and the incidence of hypoglycemia was decreased. The percentage of patients on intravenous insulin infusion at 48 hours from admission increased from 6% to 35%.
Conclusion:
The phased implementation of a formal education program, fostering the use of electronic insulin therapy protocols and dynamic manuals, received good adherence and has shown to be safe and effective for blood glucose control in critically ill patients, with a concomitant decrease in hypoglycemia.
-
Review Article
Neuropalliative care: new perspectives of intensive care
Rev Bras Ter Intensiva. 2021;33(1):146-153
Abstract
Review ArticleNeuropalliative care: new perspectives of intensive care
Rev Bras Ter Intensiva. 2021;33(1):146-153
DOI 10.5935/0103-507X.20210016
Views2See moreABSTRACT
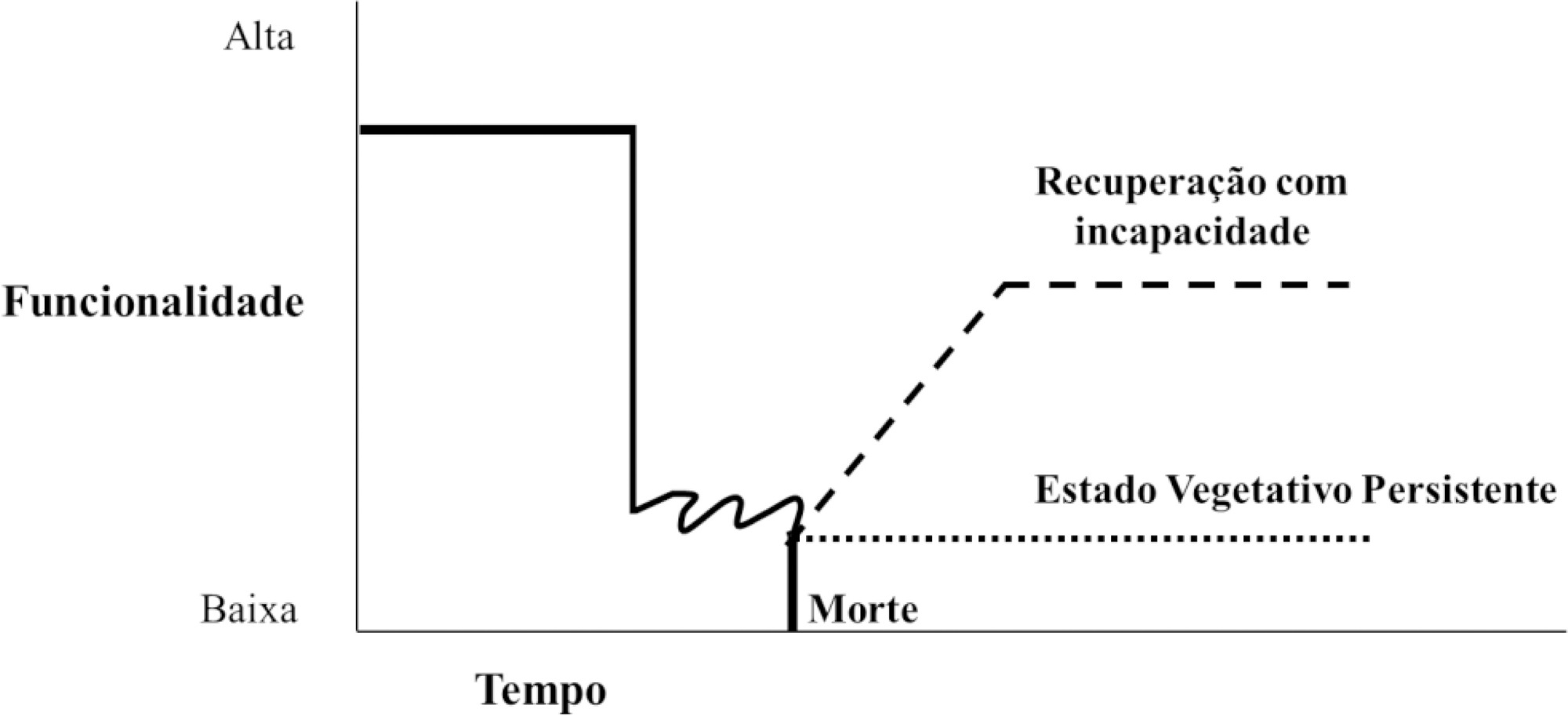
Neurological diseases are estimated to affect 1 billion people worldwide and are the cause of one in 10 deaths. In Brazil, they are responsible for approximately 14% of clinical admissions to intensive care units, 9% of elective neurosurgeries and 14% of emergency neurosurgeries. Many of these conditions are incurable, result in reduced life expectancy and quality of life and increased dependence, and are associated with symptoms that are likely to cause suffering, which justifies the integration of palliative care into usual care. In addition, factors unique to acute neurological injuries, such as their catastrophic clinical presentation, complex and uncertain prognosis, associated communication difficulties and issues related to quality of life, require a specific approach, which has recently been termed “neuropalliative care”. Although the topic is relevant and current, it is still little discussed, and much of what is known about palliative care in this context is extrapolated from approaches used under other conditions. Therefore, the objective of this study was to conduct a narrative literature review to identify the challenges of applying the palliative care approach in the care of neurocritically ill patients, with a focus on three groups: neurocritically ill patients, families and intensive care teams. This review identified that in intensive care, the main demands for palliative care are for prognostic definitions and care planning. Training in primary palliative care and improving communication were also needs identified by intensivists and families, respectively. In contrast with what has been found under other conditions, the management of symptoms was not indicated as a complex issue, although it is still relevant.
-
Review Article
Impact of red blood cell transfusion on oxygen transport and metabolism in patients with sepsis and septic shock: a systematic review and meta-analysis
Rev Bras Ter Intensiva. 2021;33(1):154-166
Abstract
Review ArticleImpact of red blood cell transfusion on oxygen transport and metabolism in patients with sepsis and septic shock: a systematic review and meta-analysis
Rev Bras Ter Intensiva. 2021;33(1):154-166
DOI 10.5935/0103-507X.20210017
Views0ABSTRACT
Red blood cell transfusion is thought to improve cell respiration during septic shock. Nevertheless, its acute impact on oxygen transport and metabolism in this condition remains highly debatable. The objective of this study was to evaluate the impact of red blood cell transfusion on microcirculation and oxygen metabolism in patients with sepsis and septic shock. We conducted a search in the MEDLINE®, Elsevier and Scopus databases. We included studies conducted in adult humans with sepsis and septic shock. A systematic review and meta-analysis were performed using the DerSimonian and Laird random-effects model. A p value < 0.05 was considered significant. Nineteen manuscripts with 428 patients were included in the analysis. Red blood cell transfusions were associated with an increase in the pooled mean venous oxygen saturation of 3.7% (p < 0.001), a decrease in oxygen extraction ratio of -6.98 (p < 0.001) and had no significant effect on the cardiac index (0.02L/minute; p = 0,96). Similar results were obtained in studies including simultaneous measurements of venous oxygen saturation, oxygen extraction ratio, and cardiac index. Red blood cell transfusions led to a significant increase in the proportion of perfused small vessels (2.85%; p = 0.553), while tissue oxygenation parameters revealed a significant increase in the tissue hemoglobin index (1.66; p = 0.018). Individual studies reported significant improvements in tissue oxygenation and sublingual microcirculatory parameters in patients with deranged microcirculation at baseline. Red blood cell transfusions seemed to improve systemic oxygen metabolism with apparent independence from cardiac index variations. Some beneficial effects have been observed for tissue oxygenation and microcirculation parameters, particularly in patients with more severe alterations at baseline. More studies are necessary to evaluate their clinical impact and to individualize transfusion decisions.
Keywords:Erythrocyte transfusionMicrocirculationOxygen consumptionOxygenationSepsisShock, septicSpectroscopy, near-infraredSee more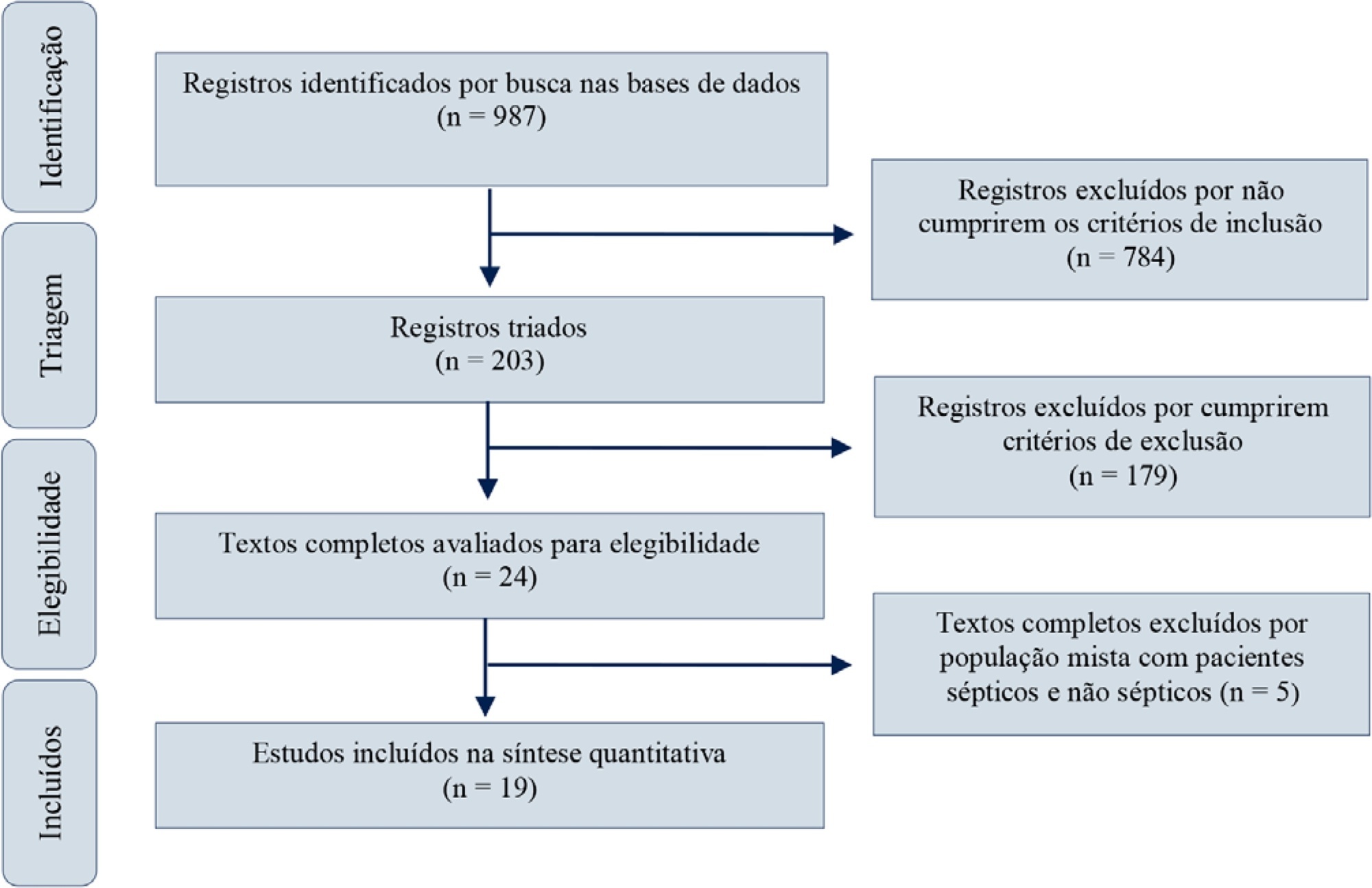
-
Case Report
Cardiopulmonary rehabilitation in post-COVID-19 patients: case series
Rev Bras Ter Intensiva. 2021;33(1):167-171
Abstract
Case ReportCardiopulmonary rehabilitation in post-COVID-19 patients: case series
Rev Bras Ter Intensiva. 2021;33(1):167-171
DOI 10.5935/0103-507X.20210018
Views0ABSTRACT
The natural history of the disease, and the treatment of post-COVID-19 patients, are still being built. Symptoms are persistent, even in mild cases, and the infection consequences include fatigue, dyspnea, tachycardia, muscle loss, and reduced functional capacity. Regarding cardiopulmonary rehabilitation, there seems to be an improvement in functional capacity, quality of life, and prognosis with the 6-Minute Walk Test used as a prognostic and therapeutic evaluator. Therefore, this case series report aims to present our experience with four cases of different severity levels, involved in a post-COVID-19 cardiopulmonary rehabilitation program. These patients were assessed with the 6-Minute Walk Test, peripheral muscle strength, and double product at rest, to assess the results after a three-month rehabilitation protocol of at least 300 minutes per week. The four patients had their distance covered during the walk test increased between 16% and 94%. Peripheral muscle strength was improved by 20% to six times the baseline values, and double product at rest was reduced by 8% to 42%. The cardiopulmonary rehabilitation program had a positive impact on these cases, improving functional capacity despite the different severity levels in these post-COVID-19 cases.
Keywords:Coronavirus infectionsCOVID-19DyspneaFatigueMuscle strengthphysical therapyRehabilitationWalk testSee more -
Case Report
Taxus baccata intoxication: the sun after the electrical storm
Rev Bras Ter Intensiva. 2021;33(1):172-175
Abstract
Case ReportTaxus baccata intoxication: the sun after the electrical storm
Rev Bras Ter Intensiva. 2021;33(1):172-175
DOI 10.5935/0103-507X.20210019
Views0ABSTRACT
European yew (Taxus baccata) is a tree with alternate branchlets, green needles and reddish-brown bark. A high-dose ingestion of Taxus baccata for suicidal purposes usually results in death. The systemic toxicity is mainly cardiac. The authors describe the case of a young patient who ingested a high dose of yew needles and presented to the emergency department with a serious intoxication, which manifested as a chaotic malignant arrhythmia that was successfully treated after exhaustive supportive care.
Keywords:DeathEmergency medical servicesNeedlesPoisoningTaxus baccata/toxicityVentricular fibrillationSee more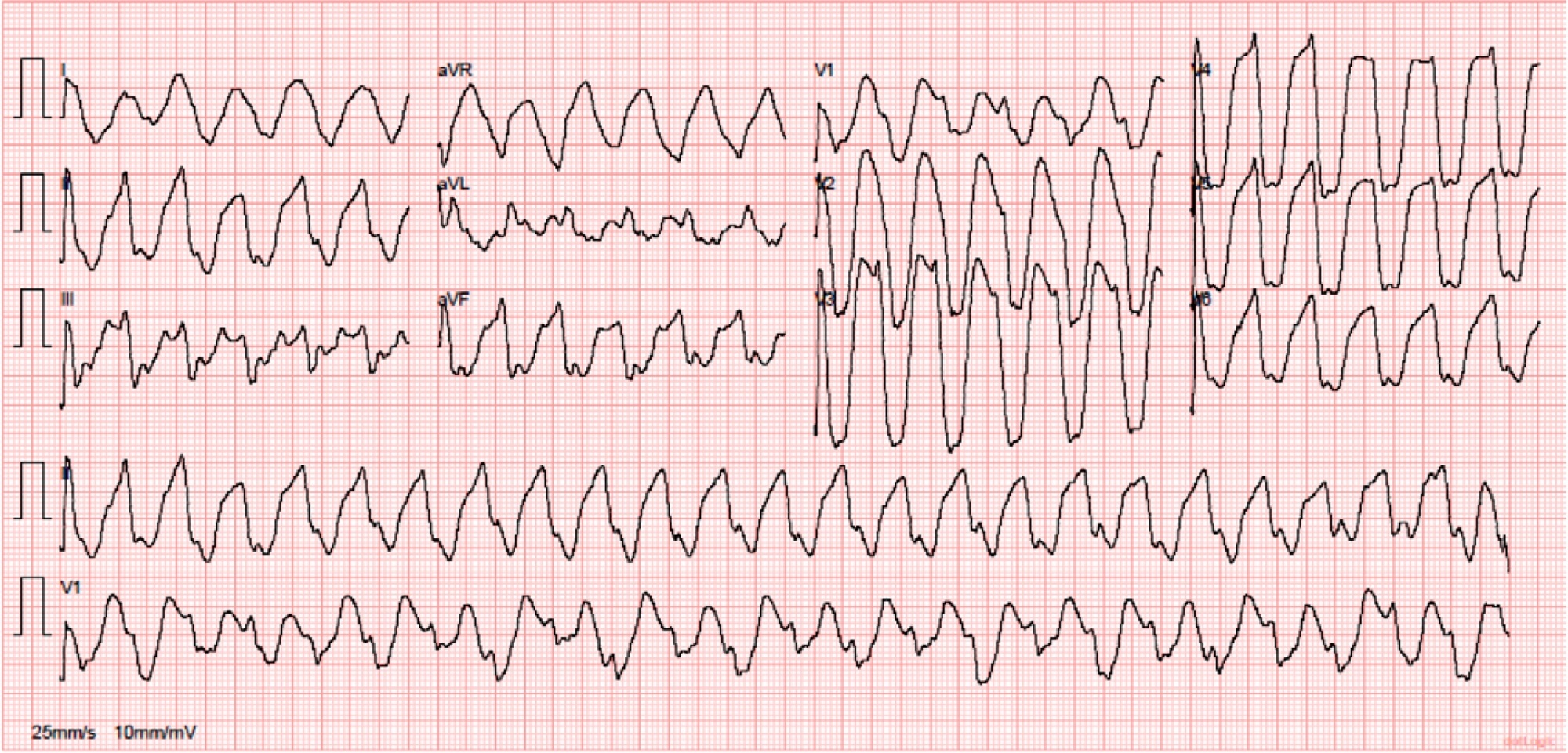
-
Letter to the Editor
Is there room for children to visit adult intensive care units?
Rev Bras Ter Intensiva. 2021;33(1):176-178
Abstract
Letter to the EditorIs there room for children to visit adult intensive care units?
Rev Bras Ter Intensiva. 2021;33(1):176-178
DOI 10.5935/0103-507X.20210020
Views0TO THE EDITOR “ My husband has been in the ICU for more than 60 days and I fear that the time for his departure is coming. I was informed of the rule that the visit is allowed from 12 years old, but our daughter is 11. She will be 12 in 2 weeks, but […]See more
-
Letter to the Editor
To: Patient functionality and walking speed after discharge from the intensive care unit
Rev Bras Ter Intensiva. 2021;33(1):179-180
Abstract
Letter to the EditorTo: Patient functionality and walking speed after discharge from the intensive care unit
Rev Bras Ter Intensiva. 2021;33(1):179-180
DOI 10.5935/0103-507X.20210021
Views0TO THE EDITOR The subject approached by Silva and Santos’ work ‘Patient functionality and walking speed after discharge from the intensive care unit’() is highly important, considering the need for the functional and physical capabilities assessment in patients after discharge from an intensive care unit (ICU); this is aimed to provide quality indicators to guide […]See more




