-
Original Articles
Evaluation of prognostic indicators for elderly patients admitted in intensive care units
Rev Bras Ter Intensiva. 2009;21(1):1-8
Abstract
Original ArticlesEvaluation of prognostic indicators for elderly patients admitted in intensive care units
Rev Bras Ter Intensiva. 2009;21(1):1-8
DOI 10.1590/S0103-507X2009000100001
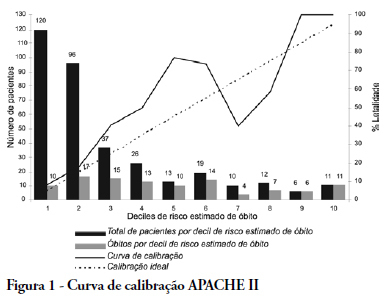
Views0See moreOBJECTIVE: The elderly constitute a population with their own features and frequent admissions in intensive care units. This study has the objective to evaluate the ability to predict the survival of these patients through the APACHE II, UNICAMP II, SAPS II and SAPS 3 indexes, global and Central America/South equations. METHODS: Elderly patients admitted from 01/01/2006 to 12/3/2006, defined as age > 60 years, were included in this study. Those who were readmitted were excluded. The rate of lethality standardized, calibration and discrimination for each index in the remaining patients were analysed. The outcome were death or hospital discharge. RESULTS: Three hundred eighty six elderly patients were included in this study, being 36 excluded by readmission, remaining 350 for analysis. The rate of lethality standardized came near to the unit in all indexes, except the SAPS II (TLP=1.5455) which underestimated the lethality. The calibration, via Hosmer-Lemeshow tests was inadequate (p < 0.05), except for the UNICAMP II (p > 0.5). On the calibration curve, the models have distanced themselves from the pattern line. All of them presented an excellent discrimination via receiver operating characteristics curves (> 0.8). CONCLUSIONS: In the studied population, the models presented an excellent discrimination and inadequate calibration. SAPS II underestimated the lethality.
-
Original Articles
Related prognostic factors in elderly patients with severe sepsis and septic shock
Rev Bras Ter Intensiva. 2009;21(1):9-17
Abstract
Original ArticlesRelated prognostic factors in elderly patients with severe sepsis and septic shock
Rev Bras Ter Intensiva. 2009;21(1):9-17
DOI 10.1590/S0103-507X2009000100002
Views0See moreOBJECTIVES: The objective of this study was to evaluate variables related to intra hospital mortality at 28 days, of aged persons with severe sepsis and septic shock in a clinical ICU. METHODS: One hundred and fifty-two patients aged > 65 years with severe sepsis and septic shock were followed for 28 days and the variables were collected on days 1, 3, 5, 7, 14 and 28 of stay. To compare categorical variables the Chi-square test was used and the Mann-Whitney or t test for continuous variables. All tests were double-tailed, alpha error of 0.05. RESULTS: Mean age was 82.0 ± 9.0 years and 64.5% were female. Mortality was of 47.4%. Related to death were the following: Acute Physiological and Chronic Heath Evaluation II score (p < 0.001), Sequential Organ Failure Assessment score on days 1, 3, 5, 7 (p < 0.001), length of stay in intensive care (p < 0.001), number of organ failures (p < 0.001), high serum lactate on day 3 (p = 0.05), positive troponin I (p < 0.01), echocardiographic variables (systolic diameter p = 0.005; diastolic diameter p = 0.05; shortening fraction p = 0.02), previous renal disease (p = 0.03), shock (p < 0.001), mechanical ventilation (p < 0.001) and Lawton scale (p = 0.04). CONCLUSIONS: Shock, elevated lactate, organ failure, especially respiratory were more prevalent in non-survivors. Heart dysfunction detected by echocardiographic variables and positive troponin I may play an important role in the mortality of aged patients with sepsis.
-
Original Articles
Mortality assessment and quality of life two years after discharge from the ICU: preliminary data from a prospective cohort
Rev Bras Ter Intensiva. 2009;21(1):18-24
Abstract
Original ArticlesMortality assessment and quality of life two years after discharge from the ICU: preliminary data from a prospective cohort
Rev Bras Ter Intensiva. 2009;21(1):18-24
DOI 10.1590/S0103-507X2009000100003
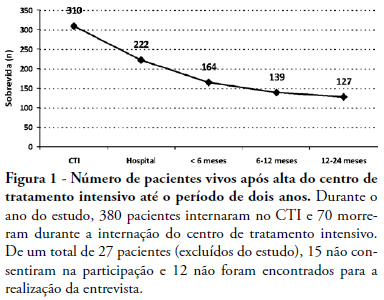
Views0See moreOBJECTIVES: To evaluate mortality and long term quality of life of patients who were discharged from the intensive care unit. METHODS: A prospective cohort, in which all the admitted patients in a intensive care unit (ICU) during 6 months were evaluated and interviewed by telephone after two years of discharge, aiming the completion of two quality of live scales: Karnofsky scale and activities of daily living (ADL) scale. RESULTS: From a total of 380 patients, 100 (26.5%) individuals were alive at the time of interview, 94% living in their homes and 90% without the need for family or specialized care. There was a significant reduction in quality of life of the survivors (Karnofsky pre-ICU = 90±10 vs. Karnofsky after two years = 79±11; p<0.05), although maintaining their functional capacity (ADL pre-ICU = 28±4 vs. ADL after two years = 25±8; p=0.09). This drop in the quality of life occurred mainly to patients who suffered stroke (Karnofsky pre-ICU = 88±7 vs. Karnofsky after two years = 60±15; p<0. 01). CONCLUSION: These preliminary data suggest that the performance of patients after two years of the intensive care discharge is preserved, since they retain the ability to perform self care, except in those with brain damage which shows an inferior quality of life.
-
Original Articles
Evaluation of the renal function in patients in the postoperative period of cardiac surgery: does AKIN classification predict acute kidney dysfunction?
Rev Bras Ter Intensiva. 2009;21(1):25-31
Abstract
Original ArticlesEvaluation of the renal function in patients in the postoperative period of cardiac surgery: does AKIN classification predict acute kidney dysfunction?
Rev Bras Ter Intensiva. 2009;21(1):25-31
DOI 10.1590/S0103-507X2009000100004
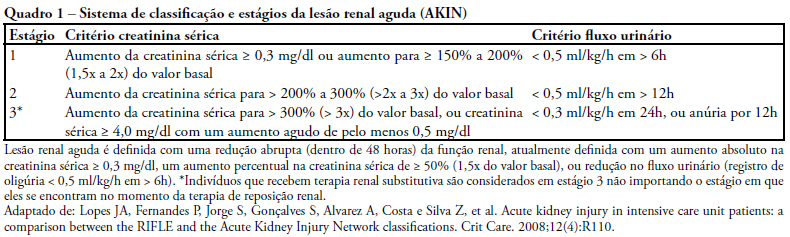
Views0See moreOBJECTIVES: To identify the frequency of the Acute Kidney Injury and to compare the application of the AKIN classification with the separate use of the serum creatinine in the postoperative period of cardiac surgery. METHODS: This study was prospectively developed in a teaching and specialized research hospital in cardiology of the public health system of the state of São Paulo. Forty-four patients submitted to the elective cardiac surgery since the immediate post-surgical period up to the 2nd post-surgical period were followed. RESULTS: It was possible to verify that from the forty-four patients, 75% were hypertensive, 27% were diabetic and mostly were male (64%), with an average age of 55+16 years old. It was observed that advanced age and the elevated body mass index shows a significant correlation to renal dysfunction (p<0, 05). According to the AKIN classification, the urinary flow criterion identified more renal dysfunction than creatinine criterion. It was verified that the renal dysfunction occurred more frequently in the postsurgery period and the majority (82%) from the 63,6% of the patients which were submitted to the revascularization of the myocardium surgery. CONCLUSION: The majority of patients (75%) evolved initially with renal dysfunction signaled it mainly by the urinary flow criterion from the AKIN classification, a higher number compared to the separated creatinine. This fact confirms that the serum creatinine association with the urinary flow has a higher discriminatory performance for the early identification of this syndrome comparatively with the routinely use of the isolated creatinine.

-
Original Articles
Analysis of family satisfaction in intensive care unit
Rev Bras Ter Intensiva. 2009;21(1):32-37
Abstract
Original ArticlesAnalysis of family satisfaction in intensive care unit
Rev Bras Ter Intensiva. 2009;21(1):32-37
DOI 10.1590/S0103-507X2009000100005
Views0OBJECTIVES: To know the needs and level of family members’ satisfaction is an essential part of the care provided to critically ill patients in intensive care units. The objective of this study was to identify the level of family members’ satisfaction in an intensive care unit. METHODS: A descriptive survey was carried out in the general adult intensive care unit of the Hospital Português (Salvador – BA) from November 2007 to January 2008. Jonhson’s 14-question modified version of the Critical Care Family Needs Inventory was used to evaluate satisfaction of family members. RESULTS: Fifty three family members were included, mean age was 44 years and 68% were female. The median of family members satisfaction level was 11 (IQI = 9-13). Critical Care Family Need Inventory, questions with higher percentiles of satisfaction were those stating that family members felt that the patient was receiving the best possible care (96%) and that the information provided was honest (96%). The questions with lower percentiles of satisfaction were those stating that family members believed that someone in the intensive care unit had shown interest in their feelings (45%) and that a healthcare professional had explained how the intensive care unit equipment was used (41%). CONCLUSIONS: Most family members positively evaluated the intensive care unit professionals in the questions related to communication, attitude and patient care. However, there was a lower level of satisfaction in the questions related to the intensive care unit professionals’ ability to comfort family members.
Keywords:FamilyHealth service evaluationIntensive care unitsPatient satisfactionProfessional-family relationsSupply of health careSee more -
Original Articles
Perceptions and actions of oral care performed by nursing teams in intensive care units
Rev Bras Ter Intensiva. 2009;21(1):38-44
Abstract
Original ArticlesPerceptions and actions of oral care performed by nursing teams in intensive care units
Rev Bras Ter Intensiva. 2009;21(1):38-44
DOI 10.1590/S0103-507X2009000100006
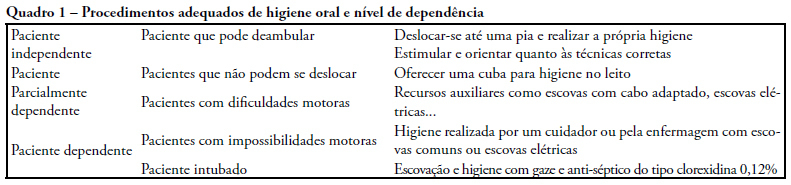
Views0See moreOBJECTIVES: A study was carried out, by means of a questionnaire for guided interviews seeking to establish a profile of perceptions and oral care given by ICU nursing team to patients in intensive care units. METHODS: The target population consisted of nursing practitioners divided in three education categories: nurses, nursing technicians and auxiliary nurses working at public and private hospital institutions providing for intensive care unit patients in Belem-PA. Dentistry experience has developed in this field reporting scientific findings and practical applications on prevention and reestablishment of the oral health in question. RESULTS: This survey disclosed results suggesting that oral hygiene care given to intensive care units patients is insufficient and inadequate requiring changes be made in the care now provided in the nosocomial environment by the nursing team. CONCLUSION: Presence of a dentist, knowledge of preventive dentistry, dissemination and use of oral hygiene specific resources are means suggested in an attempt to resolve difficulties found in oral health maintenance and treatment of oral diseases that affect the general health of hospitalized individuals. Interdisciplinary action for these individuals is advocated to achieve a better quality of life by preventing or minimizing oral pathologies.
-
Original Articles
Quality assessment of randomized clinical trial in intensive care
Rev Bras Ter Intensiva. 2009;21(1):45-50
Abstract
Original ArticlesQuality assessment of randomized clinical trial in intensive care
Rev Bras Ter Intensiva. 2009;21(1):45-50
DOI 10.1590/S0103-507X2009000100007
Views0See moreOBJECTIVE: A randomized clinical trial is a prospective study that compares the effect and value of interventions in human beings, of one or more groups vs. a control group. The objective of this study was to evaluate the quality of published randomized clinical trials in Intensive care in Brazil. METHODS: All randomized clinical trials in intensive care found by manual search in Revista Brasileira de Terapia Intensiva from January 2001 to March 2008 were assessed to evaluate their description by the quality scale. Descriptive statistics and a 95 % confidence interval were used for the primary outcome. Our primary outcome was the randomized clinical trial quality. RESULTS: Our search found 185 original articles, of which 14 were randomized clinical trials. Only one original article (7.1%) showed good quality. There was no statistical significance between the collected data and the data shown in the hypothesis of this search. CONCLUSION: It can be concluded that in the sample of assessed articles 7% of the randomized clinical trials in intensive care published in a single intensive care journal in Brazil, present good methodological quality.

-
Review Articles
Stem cell therapy in acute respiratory distress syndrome
Rev Bras Ter Intensiva. 2009;21(1):51-57
Abstract
Review ArticlesStem cell therapy in acute respiratory distress syndrome
Rev Bras Ter Intensiva. 2009;21(1):51-57
DOI 10.1590/S0103-507X2009000100008
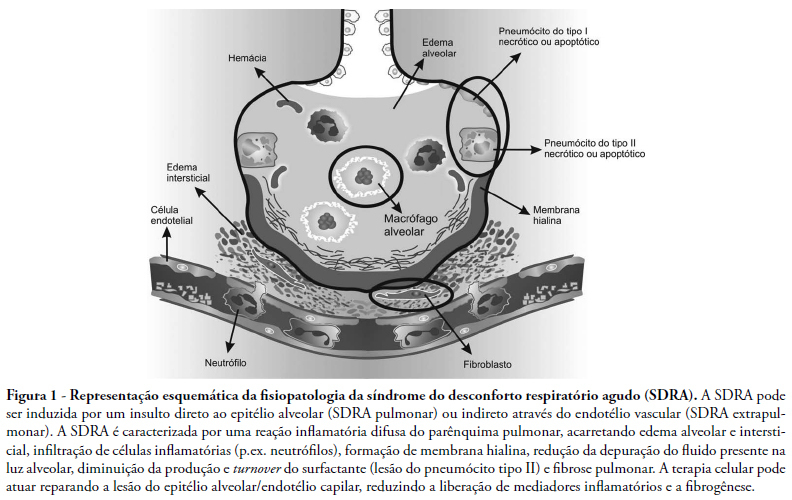
Views0See moreAcute respiratory distress syndrome is characterized by an acute pulmonary inflammatory process induced by the presence of a direct (pulmonary) insult that affects lung parenchyma, or an indirect (extrapulmonary) insult that results from an acute systemic inflammatory response. It is believed that an efficient therapy for the acute respiratory distress syndrome should attenuate inflammatory response and promote adequate repair of the lung injury. This article presents a brief review on the use of stem cells and their potential therapeutic effect on the acute respiratory distress syndrome. This systematic review was based upon clinical and experimental acute respiratory distress syndrome studies included in the MedLine and SciElO database during the last 10 years. Stem cell transplant lead to an improvement in lung injury and fibrotic process by inducing adequate tissue repair. This includes alveolar epithelial cell differentiation,and also reduces pulmonary and systemic inflammatory mediators and secretion of growth factors. Stem cells could be a potential therapy for acute respiratory distress syndrome promoting lung repair and attenuating the inflammatory response. However, mechanisms involving their anti-inflammatory and antifibrinogenic effects require better elucidation, limiting their immediate clinical use in acute respiratory distress syndrome.
-
Review Articles
Confusion assessment method to analyze delirium in intensive care unit: literature review
Rev Bras Ter Intensiva. 2009;21(1):58-64
Abstract
Review ArticlesConfusion assessment method to analyze delirium in intensive care unit: literature review
Rev Bras Ter Intensiva. 2009;21(1):58-64
DOI 10.1590/S0103-507X2009000100009
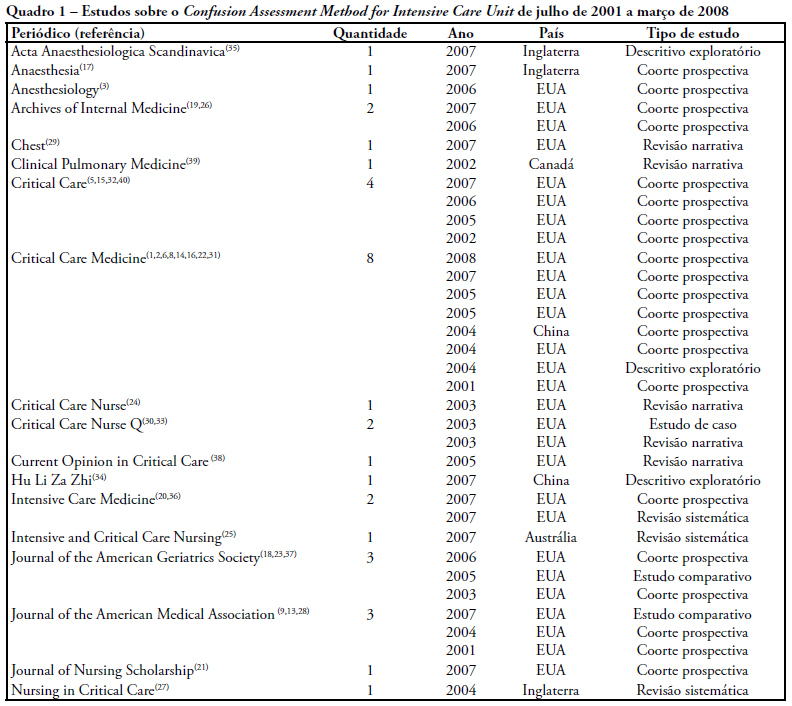
Views0See moreDelirium is frequently observed in intensive care unit patients and its occurrence is related to increased morbidity and mortality, length of stay, functional decline and high costs. The Confusion Assessment Method for Intensive Care Unit is a tool that facilitates early identification and occurrence of delirium among intubated patients. Objective: To verify the aspects of delirium studied by means of the Confusion Assessment Method for Intensive Care Unit. A literature review was conducted in the LILACS, MedLine, PubMed and CINAHL databases, from 2001, when the Confusion Assessment Method for Intensive Care Unit was validated, to 2008. Descriptors used for LILACS, MedLine and PubMed were delirium and intensive care unit, while for the CINAHL database, delirium and intensive care were used. From 293 articles, 35 were selected. The aspects analyzed disclosed, different types of delirium in different intensive care units. Variation in sensitivity was of 93% to 100% and variation in specificity, 89% to 100% of the Confusion Assessment Method for Intensive Care Unit, an important tool for detection, characterization and control of delirium and its impact. The aspects of delirium studied by means of the Confusion Assessment Method for Intensive Care Unit were: the performance index, identification, management, cost of treatment, morbidity and mortality due to delirium.
-
Review Articles
Therapeutical hypothermia after cardiopulmonary resuscitation: evidences and practical issues
Rev Bras Ter Intensiva. 2009;21(1):65-71
Abstract
Review ArticlesTherapeutical hypothermia after cardiopulmonary resuscitation: evidences and practical issues
Rev Bras Ter Intensiva. 2009;21(1):65-71
DOI 10.1590/S0103-507X2009000100010
Views0See moreCardiac arrest survivors frequently suffer from ischemic brain injury associated with poor neurological outcome and death. Therapeutic hypothermia improves outcomes in comatose survivors after resuscitation from out-of-hospital cardiac arrest. Considering its formal recommendation as a therapy, post-return of spontaneous circulation after cardiac arrest, the objective of this study was to review the clinical aspects of therapeutic hypothermia. Non-systematic review of articles using the keywords “cardiac arrest, cardiopulmonary resuscitation, cooling, hypothermia, post resuscitation syndrome” in the Med-Line database was performed. References of these articles were also reviewed. Unconscious adult patients with spontaneous circulation after out-of-hospital ventricular fibrillation or pulseless ventricular tachycardia should be cooled. Moreover, for any other rhythm or in the intra-hospital scenario, such cooling may also be beneficial. There are different ways of promoting hypothermia. The cooling system should be adjusted as soon as possible to the target temperature. Mild therapeutic hypothermia should be administered under close control, using neuromuscular blocking drugs to avoid shivering. The rewarming process should be slow, and reach 36º C, usually in no less then 8 hours. When temperature increases to more than 35º C, sedation, analgesia, and paralysis could be discontinued. The expected complications of hypothermia may be pneumonia, sepsis, cardiac arrhythmias, and coagulopathy. In spite of potential complications which require rigorous control, only six patients need to be treated to save one life.

-
Review Articles
Management of mechanical ventilation in brain injury: hyperventilation and positive end-expiratory pressure
Rev Bras Ter Intensiva. 2009;21(1):72-79
Abstract
Review ArticlesManagement of mechanical ventilation in brain injury: hyperventilation and positive end-expiratory pressure
Rev Bras Ter Intensiva. 2009;21(1):72-79
DOI 10.1590/S0103-507X2009000100011
Views0The study intended to make a critical review on use of pulmonary hyperventilation maneuvers and the different positive end-expiratory pressures applied to traumatic brain injury patients. As a reference were used publications in English, Spanish and Portuguese, contained in the following databases: MedLine, SciELO and LILACS, from 2000 to 2007, we included all studies about the use of pulmonary hyperventilation maneuvers and the different positive end-expiratory levels used for adult patients with brain injury at acute or chronic stage. Thirty one trials were selected, 13 about pulmonary hyperventilation, as prophylaxis, prolonged or optimized and 9 shows the levels of positive end-expiratory pressures used, ranging from 0 to 15 cmH2O. The prophylactic hyperventilation maneuver in the first 24 hours can lead to an increase of cerebral ischemia; the prolonged hyperventilation must be avoided if intracranial pressure did not increase; however optimized hyperventilation seems to be the most promising technique for control of the intracranial pressure and cerebral perfusion pressure; the rise of the positive end-expiratory pressure, up to 15cmH2O, can be applied in a conscientious form aiming to increase arterial oxygen saturation in lung injury.
Keywords:Brain traumaHyperventilationIntracranial hypertensionIntracranial pressurePositive pressure respirationSee more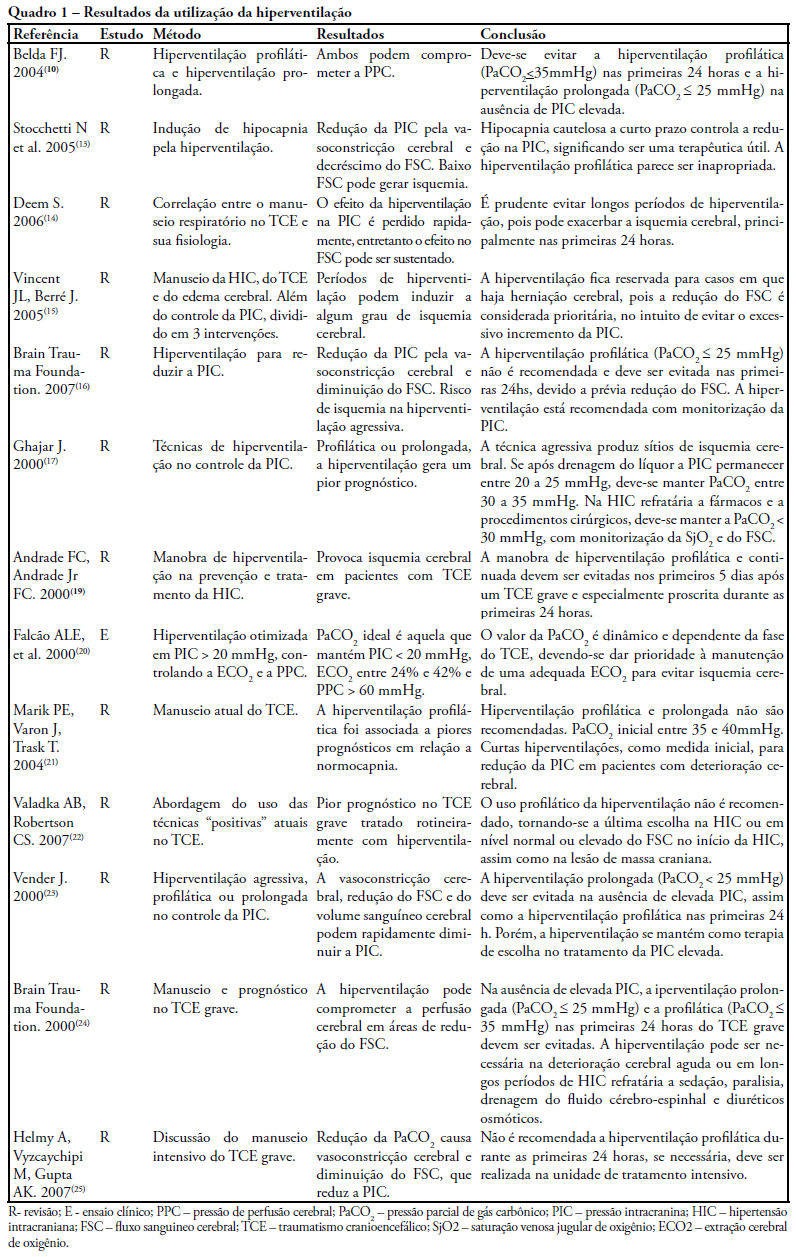
-
Review Articles
Impact of the open and closed tracheal suctioning system on the incidence of mechanical ventilation associated pneumonia: literature review
Rev Bras Ter Intensiva. 2009;21(1):80-88
Abstract
Review ArticlesImpact of the open and closed tracheal suctioning system on the incidence of mechanical ventilation associated pneumonia: literature review
Rev Bras Ter Intensiva. 2009;21(1):80-88
DOI 10.1590/S0103-507X2009000100012
Views0Pneumonia is the most common nosocominal infection in intensive care units and mechanical ventilation is a significant factor associated to its development. The objective of this study was to describe the impact of the open and closed tracheal suction systems on the incidence of ventilation-associated pneumonia. A search in the Pubmed database was performed to identify randomized controlled trials, published from 1990 to November 2008. Nine studies were included. Of the studies reviewed, seven did not disclose any significant advantages of using the closed system when compared to th e open, whereas two reported that use of the closed system increased colonization rates but not incidence of ventilation-associated pneumonia and one observed that use of the closed system did not increase colonization of the respiratory tract but reduced the spread of infection resulting in decreased sepsis rates. Only two studies found a reduction in the incidence of ventilation-associated pneumonia with use of the closed system, and one revealed a 3.5 times greater risk of developing this infection with the open system. Results suggest that the impact of the open and closed tracheal suction system is similar on development of ventilation-associated pneumonia, choice of the suction system should therefore be based on other parameters. While the closed system increases risk of colonization of the respiratory tract, but has the advantages of continuing mechanical ventilation and lessening hemodynamic impairment.
Keywords:Intensive care unitsPneumonia bacterialPneumonia, ventilator-associatedRespiration, artificialSuctionSee more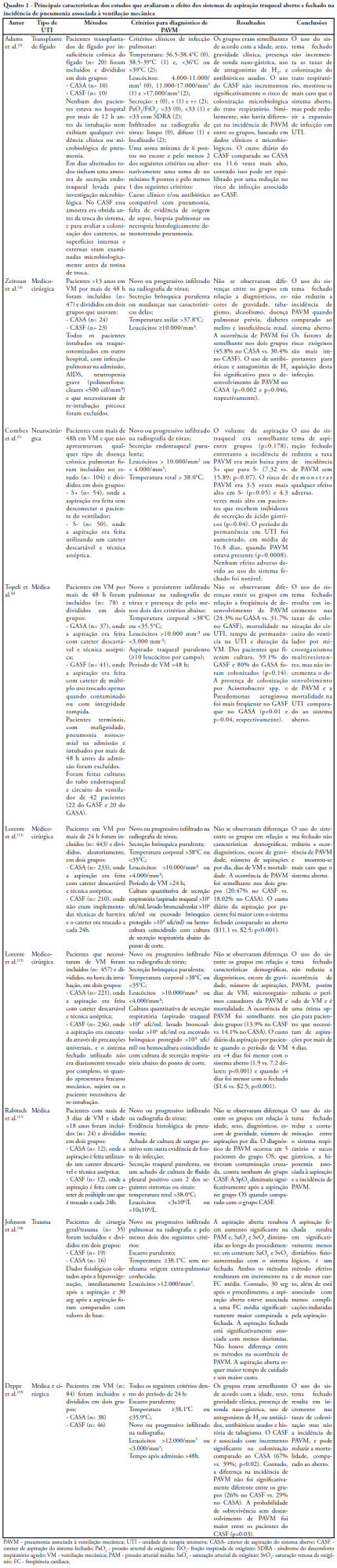
-
Review Articles
Prevention and treatment of postoperative nausea and vomiting
Rev Bras Ter Intensiva. 2009;21(1):89-95
Abstract
Review ArticlesPrevention and treatment of postoperative nausea and vomiting
Rev Bras Ter Intensiva. 2009;21(1):89-95
DOI 10.1590/S0103-507X2009000100013
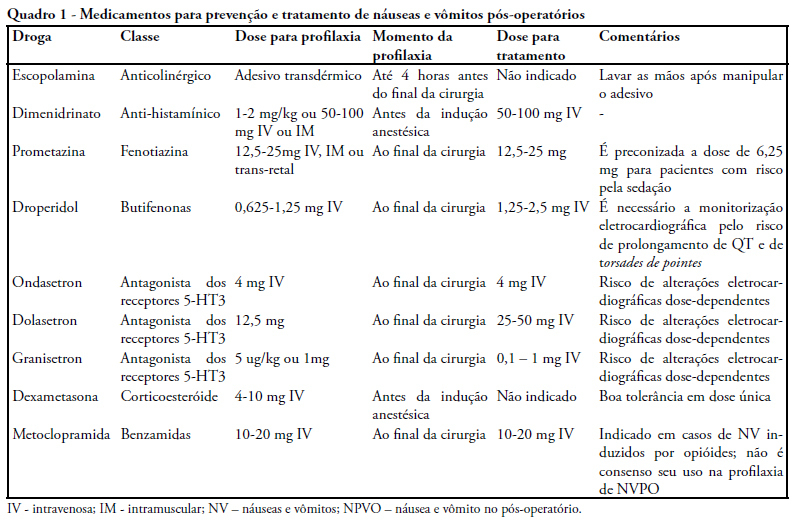
Views0See morePostoperative nausea and vomiting are common and can be prevented. Complications of this condition cause higher rates of morbidity and mortality. A review of literature was carried out on MEDLINE, with focus on controlled clinical trials. Pathophysiology is complex, with many afferent and efferent pathways, and its comprehension facilitate the choice of medication. Risk factors are presented, with a stratified score of chance to develop postoperative nausea and vomiting. An algorithm for identification of higher risk patients was elaborated and classified the level of prevention/treatment recommended to avoid excessive use of drugs and their side effects. Postoperative nausea and vomiting must be prevented, because of the involved complications and discomfort for patients. A systematic approach with analysis of preoperative risk factors and prescription of medication can be effective for prevention.
-
Review Articles
High-frequency oscillatory ventilation in pediatrics and neonatology
Rev Bras Ter Intensiva. 2009;21(1):96-103
Abstract
Review ArticlesHigh-frequency oscillatory ventilation in pediatrics and neonatology
Rev Bras Ter Intensiva. 2009;21(1):96-103
DOI 10.1590/S0103-507X2009000100014
Views0This article intends to review literature on high frequency oscillatory ventilation and describe its main clinical applications for children and neonates. Articles from the last 15 years were selected using MedLine and SciElo databases. The following key words were used: high frequency oscillatory ventilation, mechanical ventilation, acute respiratory distress syndrome, children, and new-born. The review describes high frequency oscillatory ventilation in children with acute respiratory distress syndrome, air leak syndrome, and obstructive lung disease. Respiratory distress syndrome, bronchopulmonary dysplasia, intracranial hemorrhage, periventricular leukomalacia, and air leak syndrome were reviewed in neonates. Transition from conventional mechanical ventilation to high frequency ventilation and its adjustments relating to oxygenation, CO2 elimination, chest radiography, suctioning, sedatives and use of neuromuscular blocking agents were described. Weaning and complications were also reported. For children, high frequency oscillatory ventilation is a therapeutic option, particularly in acute respiratory distress syndrome, and should be used as early as possible. It may be also useful in the air leak syndrome and obstructive pulmonary disease. Evidence that, in neonates, high frequency oscillatory ventilation is superior to conventional mechanical ventilation is lacking. However there is evidence that better results are only achieved with this ventilatory mode to manage the air leak syndrome.
Keywords:acute respiratory distress syndromeChildHigh frequency oscillatory ventilationInfant, newbornmechanical ventilationSee more -
Case Reports
Alveolar recruitment in pulmonary contusion: case report and literature review
Rev Bras Ter Intensiva. 2009;21(1):104-108
Abstract
Case ReportsAlveolar recruitment in pulmonary contusion: case report and literature review
Rev Bras Ter Intensiva. 2009;21(1):104-108
DOI 10.1590/S0103-507X2009000100015
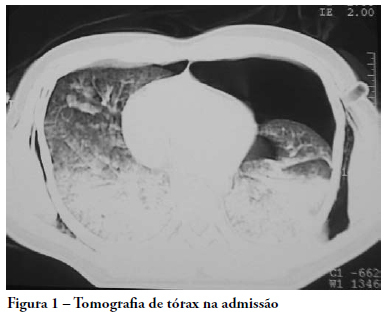
Views0See moreTreatment of pulmonary contusion when adequately established is very simple in most cases. Pathophysiological changes occur as a result of the effects produced by loss of chest wall integrity, accumulation of fluid in the pleural cavity, obstruction of the airways and lung dysfunction. The alveolar recruitment maneuver is the reopening of collapsed lung areas by increasing inspiratory pressure in the airway. The primary objective of this case report was to evaluate the effectiveness of the alveolar recruitment maneuver in a patient with pulmonary contusion. A 33 year old male patient, with a clinical condition of bilateral chest trauma and traumatic brain injury, evolved with reduction of the level of consciousness, acute respiratory failure, hypovolemic shock and hemoptysis. The patient underwent thoracentesis, bilateral thoracic drainage and was also submitted to invasive mechanical ventilation. After 48 hours of invasive mechanical ventilation, in accordance with protective strategy an alveolar recruitment maneuver mode, pressure-controlled ventilation, pressure controlled 10 cmH2O, respiratory rate 10 rpm, inspiratory time 3.0, positive end-expiratory pressure 30 cmH2O and FI0(2) 100%, for two minutes. After the alveolar recruitment maneuver, the patient presented clinical pulmonary improvement, but there was a variation of 185 to 322 of Pa0(2)/FiO2 (arterial partial pressure of oxygen/ fraction of inspired oxygen). He was discharged from the intensive care unit 22 days after admission. The alveolar recruitment maneuver in this patient showed significant results in the treatment of pulmonary contusion, improving blood oxygenation, preventing alveolar collapse and reversing atelectasis.
-
Letters to the Editor
Postoperative complications of coronary artery bypass graft in elderly patients
Rev Bras Ter Intensiva. 2009;21(1):109-110
Abstract
Letters to the EditorPostoperative complications of coronary artery bypass graft in elderly patients
Rev Bras Ter Intensiva. 2009;21(1):109-110
DOI 10.1590/S0103-507X2009000100016
Views0LETTER TO THE EDITOR Postoperative complications of coronary artery bypass graft in elderly patients[…]See more -
Letters to the Editor
Postoperative complications of coronary artery bypass graft in elderly patients: reply of the letter to the editor
Rev Bras Ter Intensiva. 2009;21(1):111-112
Abstract
Letters to the EditorPostoperative complications of coronary artery bypass graft in elderly patients: reply of the letter to the editor
Rev Bras Ter Intensiva. 2009;21(1):111-112
DOI 10.1590/S0103-507X2009000100017
Views0LETTER TO THE EDITOR Postoperative complications of coronary artery bypass graft in elderly patients. Reply of the letter to the editor […]See more




