-
Editorial
Open-access publications: a double-edged sword for critical care researchers in lowand middle-income countries
Crit Care Sci. 2023;35(4):342-344
Abstract
EditorialOpen-access publications: a double-edged sword for critical care researchers in lowand middle-income countries
Crit Care Sci. 2023;35(4):342-344
DOI 10.5935/2965-2774.20230263-pt
Views42Open access model and lowand middle-income countries Open access journals usually exempt researchers from low-income countries from publication fees, and this exemption seems to favor the publication of articles by researchers from sub-Saharan Africa.() However, producing high-quality scientific research in these settings is challenging and often funded by agencies such as the National Institutes of […]See more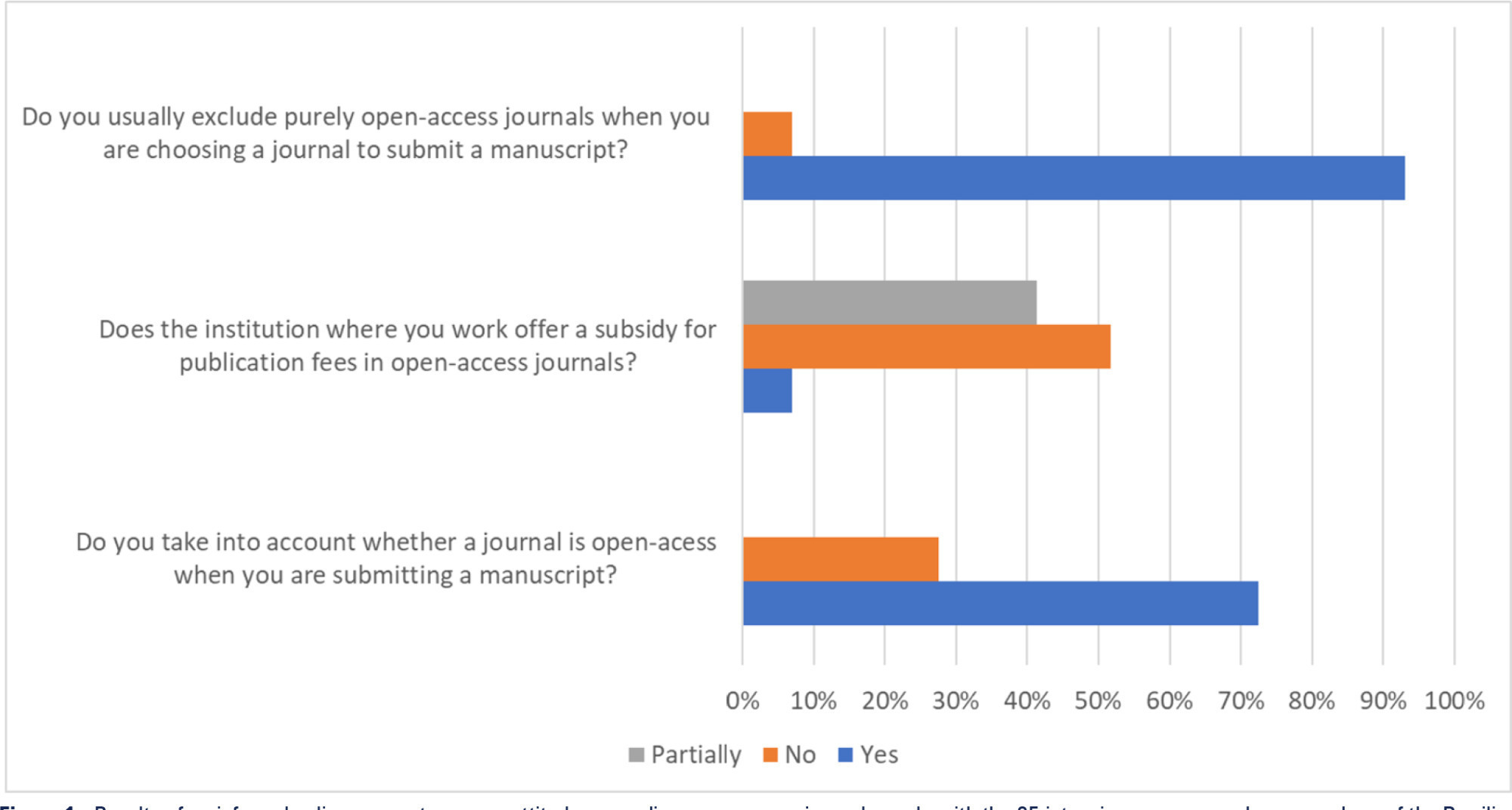
-
Special Article
Intensive glucose control in critically ill adults: a protocol for a systematic review and individual patient data meta-analysis
Crit Care Sci. 2023;35(4):345-354
Abstract
Special ArticleIntensive glucose control in critically ill adults: a protocol for a systematic review and individual patient data meta-analysis
Crit Care Sci. 2023;35(4):345-354
DOI 10.5935/2965-2774.20230162-pt
Views19ABSTRACT
Objective:
The optimal target for blood glucose concentration in critically ill patients is unclear. We will perform a systematic review and meta-analysis with aggregated and individual patient data from randomized controlled trials, comparing intensive glucose control with liberal glucose control in critically ill adults.
Data sources:
MEDLINE®, Embase, the Cochrane Central Register of Clinical Trials, and clinical trials registries (World Health Organization, clinical trials.gov). The authors of eligible trials will be invited to provide individual patient data. Published trial-level data from eligible trials that are not at high risk of bias will be included in an aggregated data meta-analysis if individual patient data are not available.
Methods:
Inclusion criteria: randomized controlled trials that recruited adult patients, targeting a blood glucose of ≤ 120mg/dL (≤ 6.6mmol/L) compared to a higher blood glucose concentration target using intravenous insulin in both groups. Excluded studies: those with an upper limit blood glucose target in the intervention group of > 120mg/dL (> 6.6mmol/L), or where intensive glucose control was only performed in the intraoperative period, and those where loss to follow-up exceeded 10% by hospital discharge.
Primary endpoint:
In-hospital mortality during index hospital admission. Secondary endpoints: mortality and survival at other timepoints, duration of invasive mechanical ventilation, vasoactive agents, and renal replacement therapy. A random effect Bayesian meta-analysis and hierarchical Bayesian models for individual patient data will be used.
Discussion:
This systematic review with aggregate and individual patient data will address the clinical question, ‘what is the best blood glucose target for critically ill patients overall?’
Keywords:Blood glucoseCritical illnessGlycemic controlinsulinIntraoperative periodMortalityPatient dischargeRegistriesSee more -
Original Article
Typical phenotypes of patients with acute respiratory failure with and without COVID-19 and their relationship with outcomes: a cohort study
Crit Care Sci. 2023;35(4):355-366
Abstract
Original ArticleTypical phenotypes of patients with acute respiratory failure with and without COVID-19 and their relationship with outcomes: a cohort study
Crit Care Sci. 2023;35(4):355-366
DOI 10.5935/2965-2774.20230015-pt
Views15See moreABSTRACT
Objective:
To compare, within a cohort of patients with acute respiratory failure, the phenotypes of patients with and without COVID-19 in the context of the pandemic and evaluate whether COVID-19 is an independent predictor of intensive care unit mortality.
Methods:
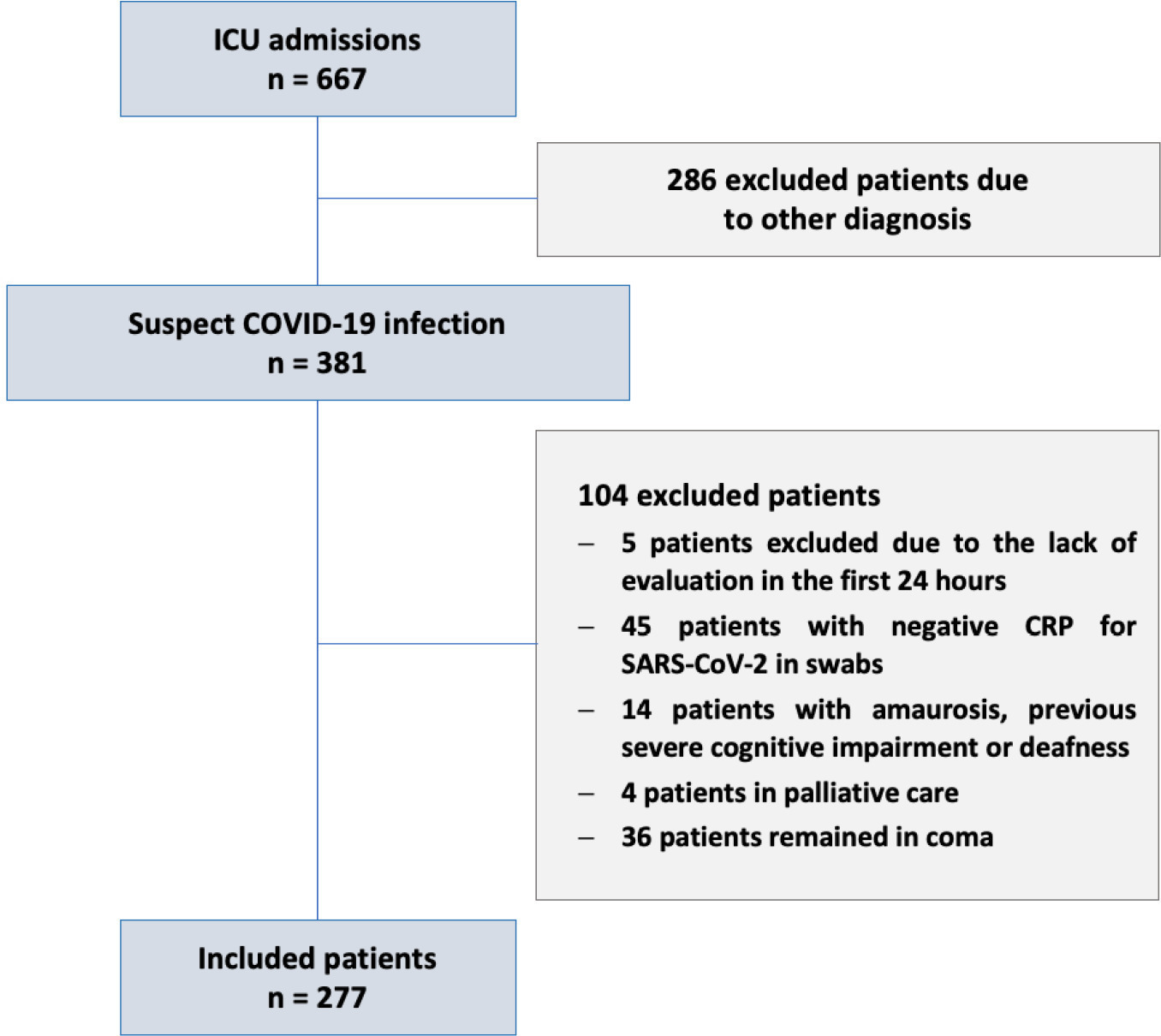
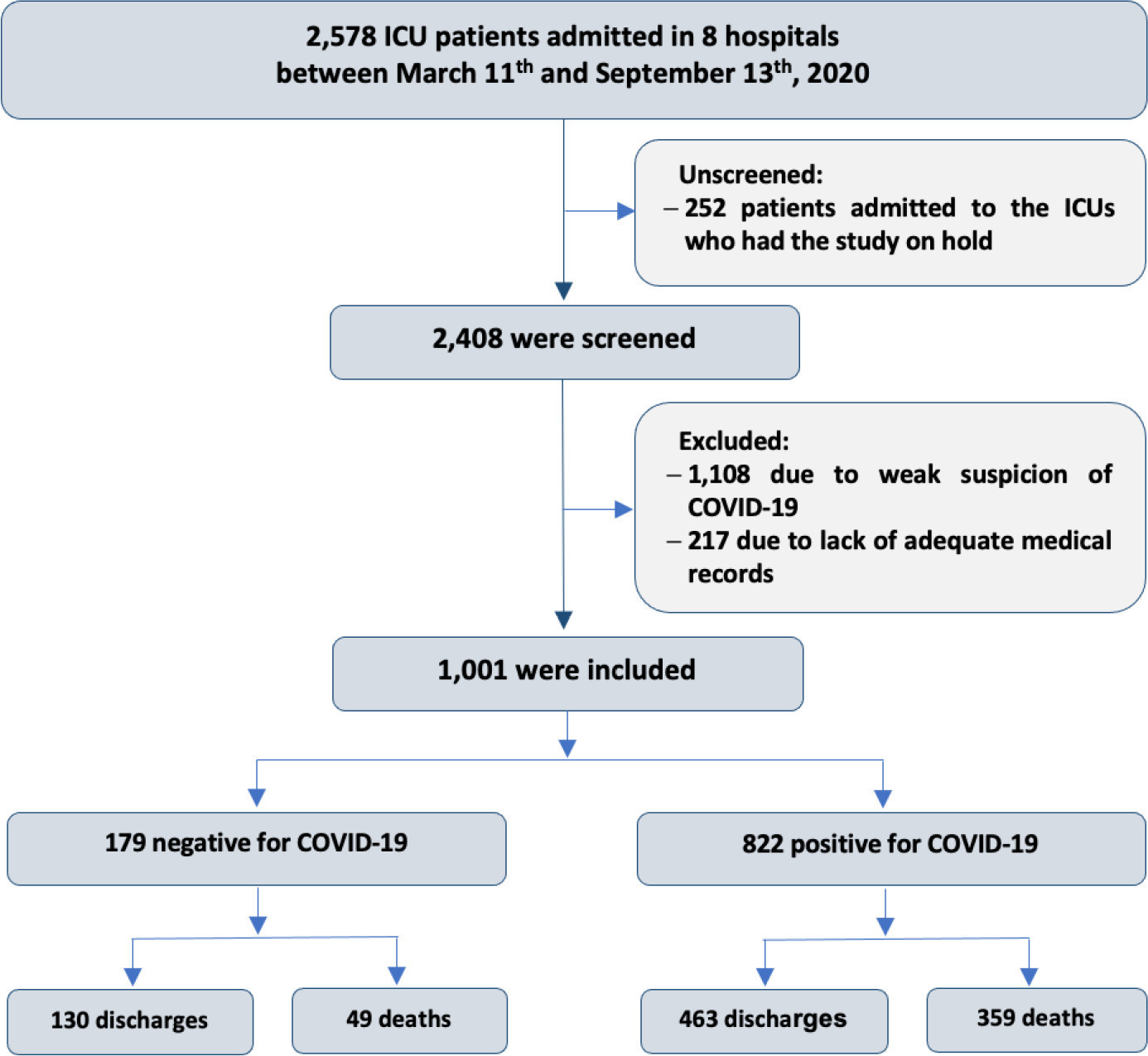
This historical cohort study evaluated 1001 acute respiratory failure patients with suspected COVID-19 admitted to the intensive care unit of 8 hospitals. Patients were classified as COVID-19 cases and non-COVID-19 cases according to real-time polymerase chain reaction results. Data on clinical and demographic characteristics were collected on intensive care unit admission, as well as daily clinical and laboratory data and intensive care unit outcomes.
Results:
Although the groups did not differ in terms of APACHE II or SOFA scores at admission, the COVID-19 group had more initial symptoms of fever, myalgia and diarrhea, had a longer duration of symptoms, and had a higher prevalence of obesity. They also had a lower PaO2/FiO2 ratio, lower platelet levels than non-COVID-19 patients, and more metabolic changes, such as higher levels of blood glucose, C-reactive protein, and lactic dehydrogenase. Patients with non-COVID-19 acute respiratory failure had a higher prevalence of chronic obstructive pulmonary disease/asthma and cardiopathy. Patients with COVID-19 stayed in the hospital longer and had more complications, such as acute kidney failure, severe acute respiratory distress syndrome and severe infection. The all-cause mortality rate was also higher in this group (43.7% in the COVID-19 group versus 27.4% in the non-COVID-19 group). The diagnosis of COVID-19 was a predictor of intensive care unit mortality (odds ratio, 2.77; 95%CI, 1.89 – 4.07; p < 0.001), regardless of age or Charlson Comorbidity Index score.
Conclusion:
In a prospective cohort of patients admitted with acute respiratory failure, patients with COVID-19 had a clearly different phenotype and a higher mortality than non-COVID-19 patients. This may help to outline more accurate screening and appropriate and timely treatment for these patients.
-
Original Article
Impact of vertical positioning on lung aeration among mechanically ventilated intensive care unit patients: a randomized crossover clinical trial
Crit Care Sci. 2023;35(4):367-376
Abstract
Original ArticleImpact of vertical positioning on lung aeration among mechanically ventilated intensive care unit patients: a randomized crossover clinical trial
Crit Care Sci. 2023;35(4):367-376
DOI 10.5935/2965-2774.20230069-pt
Views12ABSTRACT
Objective:
To assess the impact of different vertical positions on lung aeration in patients receiving invasive mechanical ventilation.
Methods:
An open-label randomized crossover clinical trial was conducted between January and July 2020. Adults receiving invasive mechanical ventilation for > 24 hours and < 7 days with hemodynamic, respiratory and neurological stability were randomly assigned at a 1:1 ratio to the sitting position followed by passive orthostasis condition or the passive orthostasis followed by the sitting position condition. The primary outcome was lung aeration assessed using the lung ultrasound score (score ranges from 0 [better] to 36 [worse]).
Results:
A total of 186 subjects were screened; of these subjects, 19 were enrolled (57.8% male; mean age, 73.2 years). All participants were assigned to receive at least one verticalization protocol. Passive orthostasis resulted in mean lung ultrasound scores that did not differ significantly from the sitting position (11.0 versus 13.7; mean difference, -2.7; [95%CI -6.1 to 0.71; p = 0.11). Adverse events occurred in three subjects in the passive orthostasis group and in one in the sitting position group (p = 0.99).
Conclusion:
This analysis did not find significant differences in lung aeration between the sitting and passive orthostasis groups. A randomized crossover clinical trial assessing the impact of vertical positioning on lung aeration in patients receiving invasive mechanical ventilation is feasible. Unfortunately, the study was interrupted due to the need to treat COVID-19 patients.
Keywords:AerationIntensive care unitslungRespiration, artificialSitting positionStanding positionUltrasonographySee more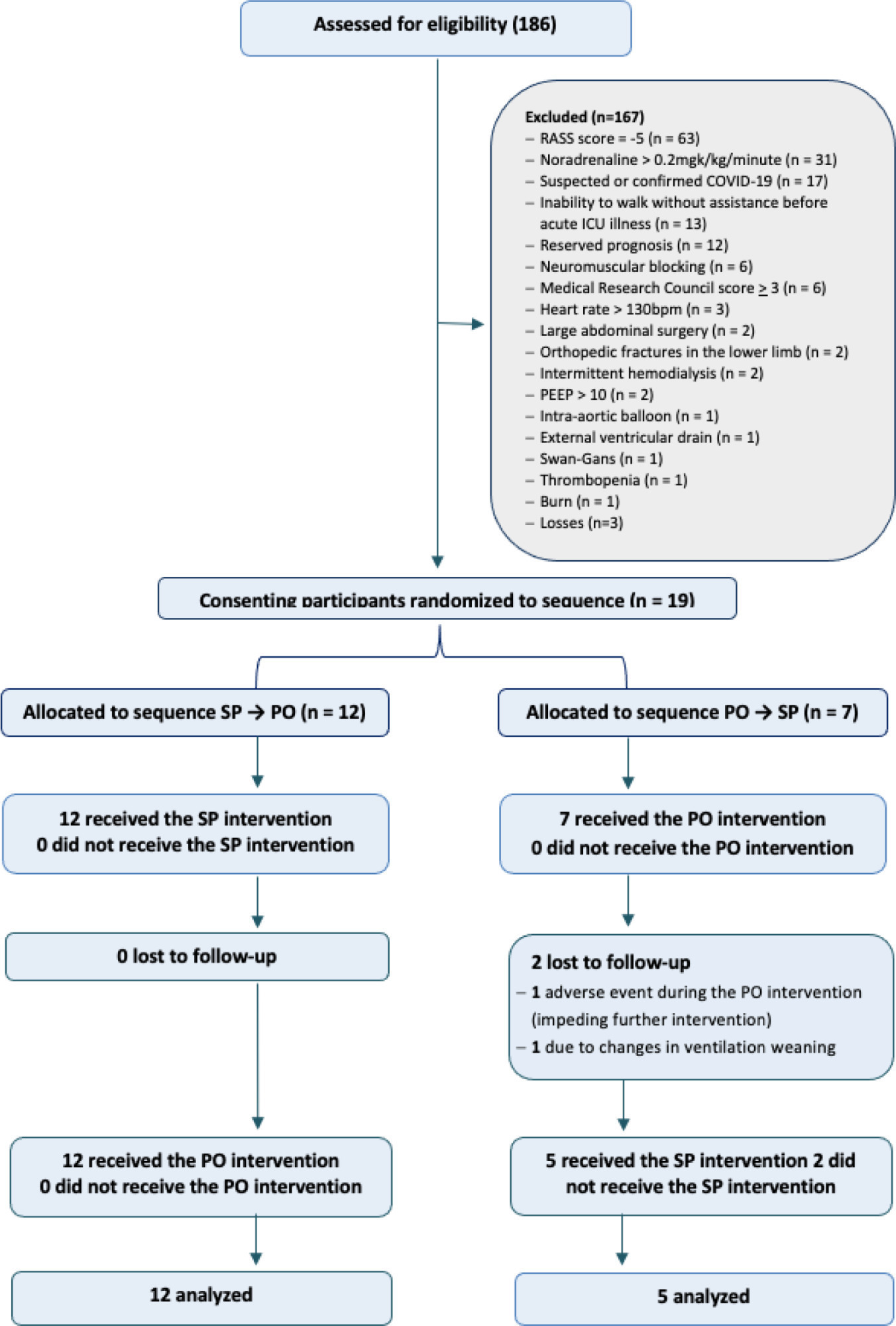
-
Original Article
Adverse events in the postoperative period of cardiac surgery in a pediatric intensive care unit: the contribution of the VIS score and the RACHS-1
Crit Care Sci. 2023;35(4):377-385
Abstract
Original ArticleAdverse events in the postoperative period of cardiac surgery in a pediatric intensive care unit: the contribution of the VIS score and the RACHS-1
Crit Care Sci. 2023;35(4):377-385
DOI 10.5935/2965-2774.20230215-pt
Views9ABSTRACT
Objective:
To evaluate the occurrence of adverse events in the postoperative period of cardiac surgery in a pediatric intensive care unit and to find any patient characteristics that can predict such events.
Methods:
This was a historical cohort study of patients recovering in the pediatric intensive care unit for the first 7 days after cardiac surgery between April and December 2019, by reviewing the medical records. The following were reviewed: demographic, clinical, and laboratory characteristics; patient severity scores; and selected adverse events, grouped into device-related, surgical, and nonsurgical.
Results:
A total of 238 medical records were included. At least one adverse event occurred in 110 postoperative patients (46.2%). The total number of adverse events was 193 (81%). Vascular catheters were the most common cause, followed by cardiac arrest, bleeding, and surgical reexploration. In the univariate analysis, the vasoactive-inotropic score (VIS), Risk Adjustment in Congenital Heart Surgery (RACHS-1) score, age, Pediatric Index of Mortality (PIM-2), cardiopulmonary bypass and aortic clamping duration were significantly associated with adverse events. In the multivariate analysis, VIS ≥ 20 (OR 2.90; p = 0.004) and RACHS-1 ≥ 3 (OR 2.11; p = 0.019) were significant predictors, while age and delayed sternal closure showed only trends toward significance. To predict the occurrence of adverse events from VIS and RACHS-1, the area under the curve was 0.73 (95%CI 0.66 – 0.79).
Conclusion:
Adverse events were quite frequent in children after cardiac surgery, especially those related to devices. The VIS and RACHS-1, used together, predicted the occurrence of adverse events well in this pediatric sample.
Keywords:Cardiac surgical procedures/adverse effectsCardiovascular agentsIntensive care units, pediatricPatient safetyPostoperative periodSafety managementSee more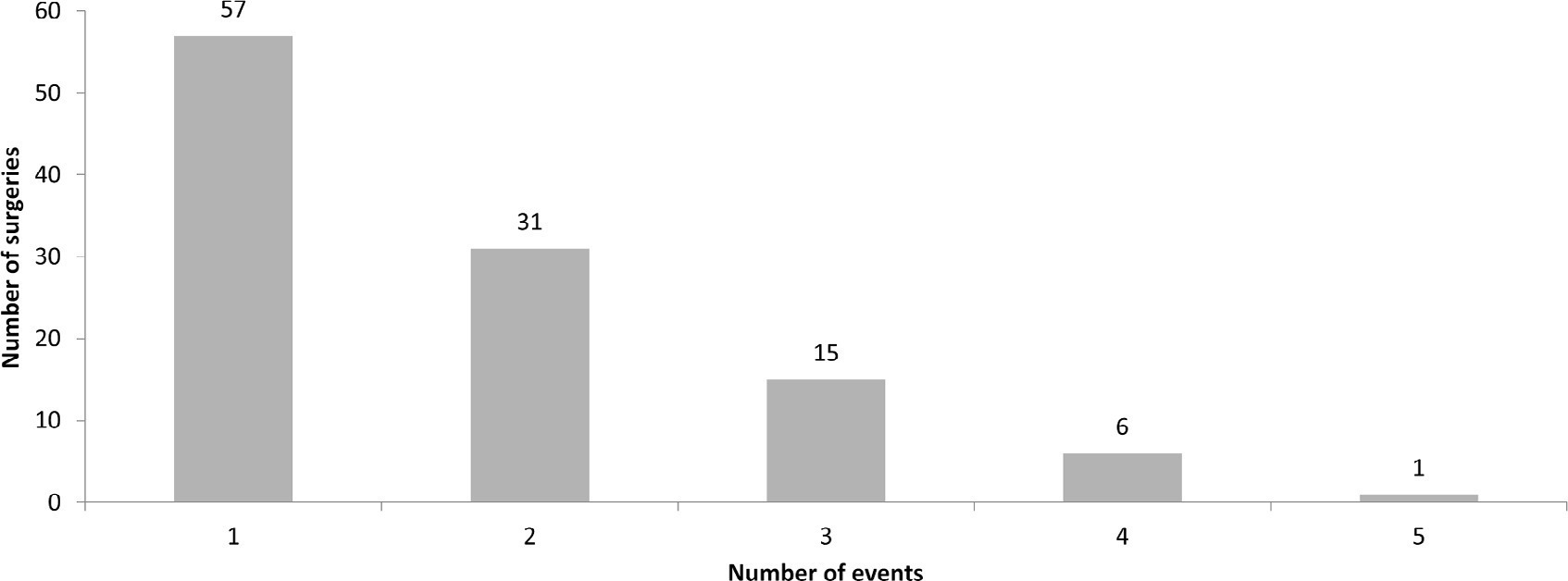
-
Original Article
Effects of atelectatic areas on the surrounding lung tissue during mechanical ventilation in an experimental model of acute lung injury induced by lipopolysaccharide
Crit Care Sci. 2023;35(4):386-393
Abstract
Original ArticleEffects of atelectatic areas on the surrounding lung tissue during mechanical ventilation in an experimental model of acute lung injury induced by lipopolysaccharide
Crit Care Sci. 2023;35(4):386-393
DOI 10.5935/2965-2774.20230190-pt
Views4ABSTRACT
Objective:
To assess the effect of atelectasis during mechanical ventilation on the periatelectatic and normal lung regions in a model of atelectasis in rats with acute lung injury induced by lipopolysaccharide.
Methods:
Twenty-four rats were randomized into the following four groups, each with 6 animals: the Saline-Control Group, Lipopolysaccharide Control Group, Saline-Atelectasis Group, and Lipopolysaccharide Atelectasis Group. Acute lung injury was induced by intraperitoneal injection of lipopolysaccharide. After 24 hours, atelectasis was induced by bronchial blocking. The animals underwent mechanical ventilation for two hours with protective parameters, and respiratory mechanics were monitored during this period. Thereafter, histologic analyses of two regions of interest, periatelectatic areas and the normally-aerated lung contralateral to the atelectatic areas, were performed.
Results:
The lung injury score was significantly higher in the Lipopolysaccharide Control Group (0.41 ± 0.13) than in the Saline Control Group (0.15 ± 0.51), p < 0.05. Periatelectatic regions showed higher lung injury scores than normally-aerated regions in both the Saline-Atelectasis (0.44 ± 0.06 x 0.27 ± 0.74 p < 0.05) and Lipopolysaccharide Atelectasis (0.56 ± 0.09 x 0.35 ± 0.04 p < 0.05) Groups. The lung injury score in the periatelectatic regions was higher in the Lipopolysaccharide Atelectasis Group (0.56 ± 0.09) than in the periatelectatic region of the Saline-Atelectasis Group (0.44 ± 0.06), p < 0.05.
Conclusion:
Atelectasis may cause injury to the surrounding tissue after a period of mechanical ventilation with protective parameters. Its effect was more significant in previously injured lungs.
Keywords:acute respiratory distress syndromeLipopolysaccharidesModels, animalPulmonary atelectasisRespiration, artificialSepsisVentilator-induced lung injurySee more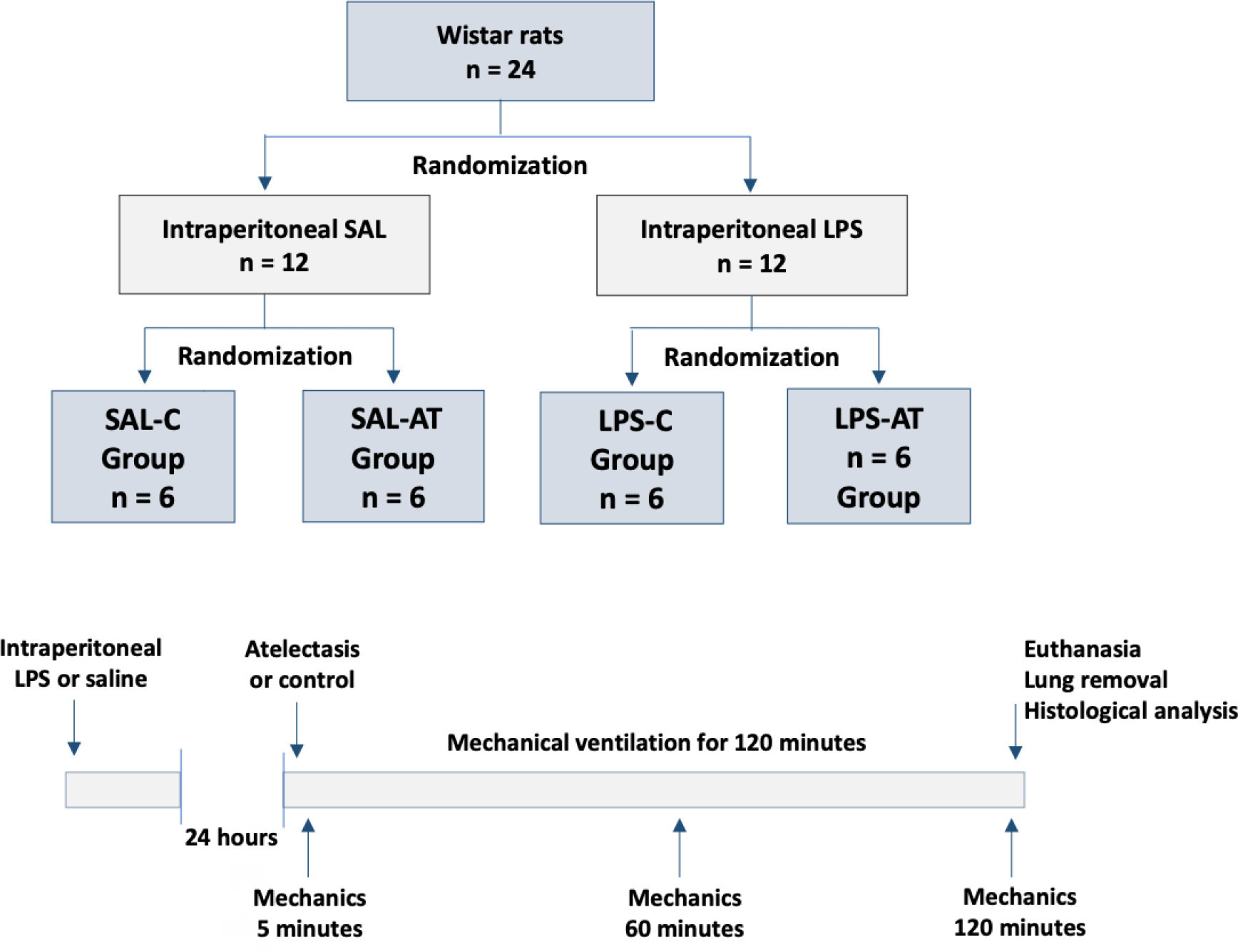
-
Original Article
Intensivist-led ultrasound-guided percutaneous tracheostomy: a phase IV cohort study
Crit Care Sci. 2023;35(4):402-410
Abstract
Original ArticleIntensivist-led ultrasound-guided percutaneous tracheostomy: a phase IV cohort study
Crit Care Sci. 2023;35(4):402-410
DOI 10.5935/2965-2774.20230174-pt
Views29See moreABSTRACT
Objective:
To describe, with a larger number of patients in a real-world scenario following routine implementation, intensivist-led ultrasound-guided percutaneous dilational tracheostomy and the possible risks and complications of the procedure not identified in clinical trials.
Methods:
This was a phase IV cohort study of patients admitted to three intensive care units of a quaternary academic hospital who underwent intensivist-led ultrasound-guided percutaneous tracheostomy in Brazil from September 2017 to December 2021.
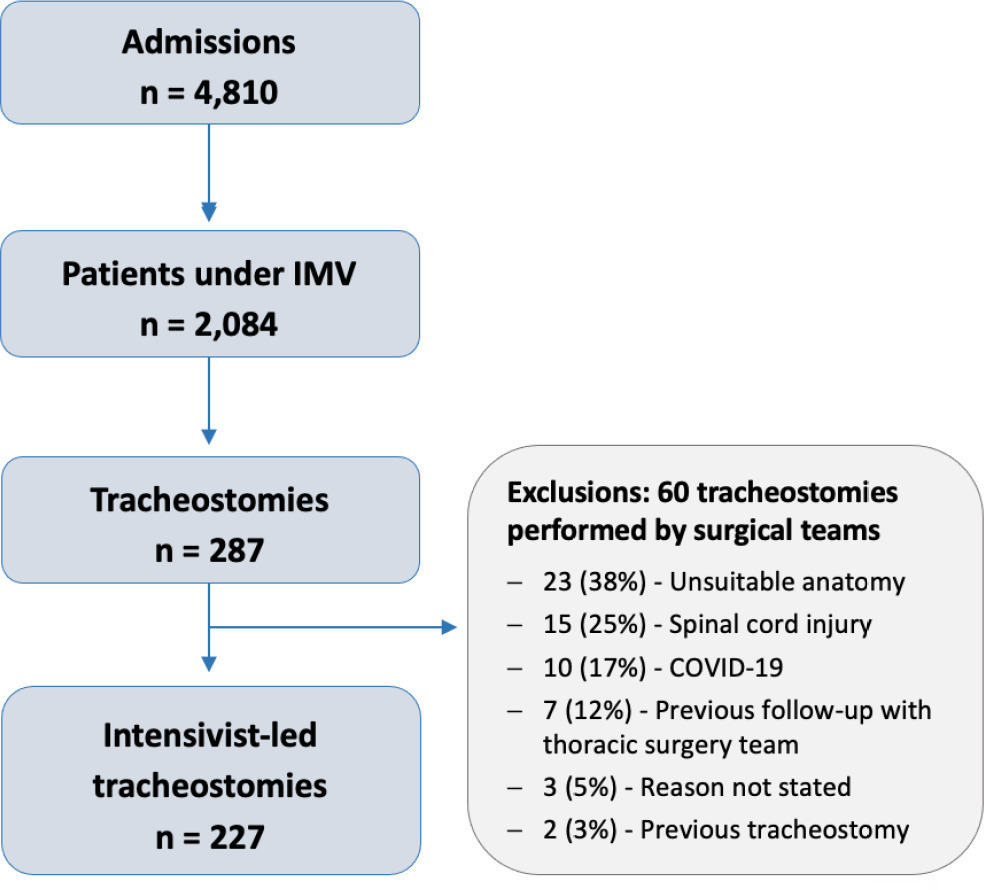
Results:
There were 4,810 intensive care unit admissions during the study period; 2,084 patients received mechanical ventilation, and 287 underwent tracheostomy, 227 of which were performed at bedside by the intensive care team. The main reason for intensive care unit admission was trauma, and for perform a tracheostomy it was a neurological impairment or an inability to protect the airways. The median time from intubation to tracheostomy was 14 days. Intensive care residents performed 76% of the procedures. At least one complication occurred in 29.5% of the procedures, the most common being hemodynamic instability and extubation during the procedure, with only 3 serious complications. The intensive care unit mortality was 29.1%, and the hospital mortality was 43.6%.
Conclusion:
Intensivist-led ultrasound-guided percutaneous tracheostomy is feasible out of a clinical trial context with outcomes and complications comparable to those in the literature. Intensivists can acquire this competence during their training but should be aware of potential complications to enhance procedural safety.
-
Letter to the Editor
Outcomes of critically ill pregnant COVID-19 patients: a cohort study
Crit Care Sci. 2023;35(4):411-412
Abstract
Letter to the EditorOutcomes of critically ill pregnant COVID-19 patients: a cohort study
Crit Care Sci. 2023;35(4):411-412
DOI 10.5935/2965-2774.20230222-pt
Views8To the editor,Information related to coronavirus disease 2019 (COVID-19), caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), in pregnant women is scarce and limited. Increased oxygen consumption, a reduction in chest wall compliance, and decreased functional residual capacity can exacerbate respiratory distress and may lead to the development of acute respiratory distress syndrome (ARDS).() […]See more -
Letter to the Editor
Capillary leak syndrome during continuous renal replacement therapy after renal hilum ligation in a hypercapnic landrace pig
Crit Care Sci. 2023;35(4):413-415
Abstract
Letter to the EditorCapillary leak syndrome during continuous renal replacement therapy after renal hilum ligation in a hypercapnic landrace pig
Crit Care Sci. 2023;35(4):413-415
DOI 10.5935/2965-2774.20230139-pt
Views11Literature on dialysis in pigs is scarce, and there is no description of capillary leak syndrome during dialysis in pigs. Our aim in this paper is to bring attention to the possible occurrence of this syndrome, at least in the described specific condition.In an ongoing experimental line of research, we are investigating the impact of […]See more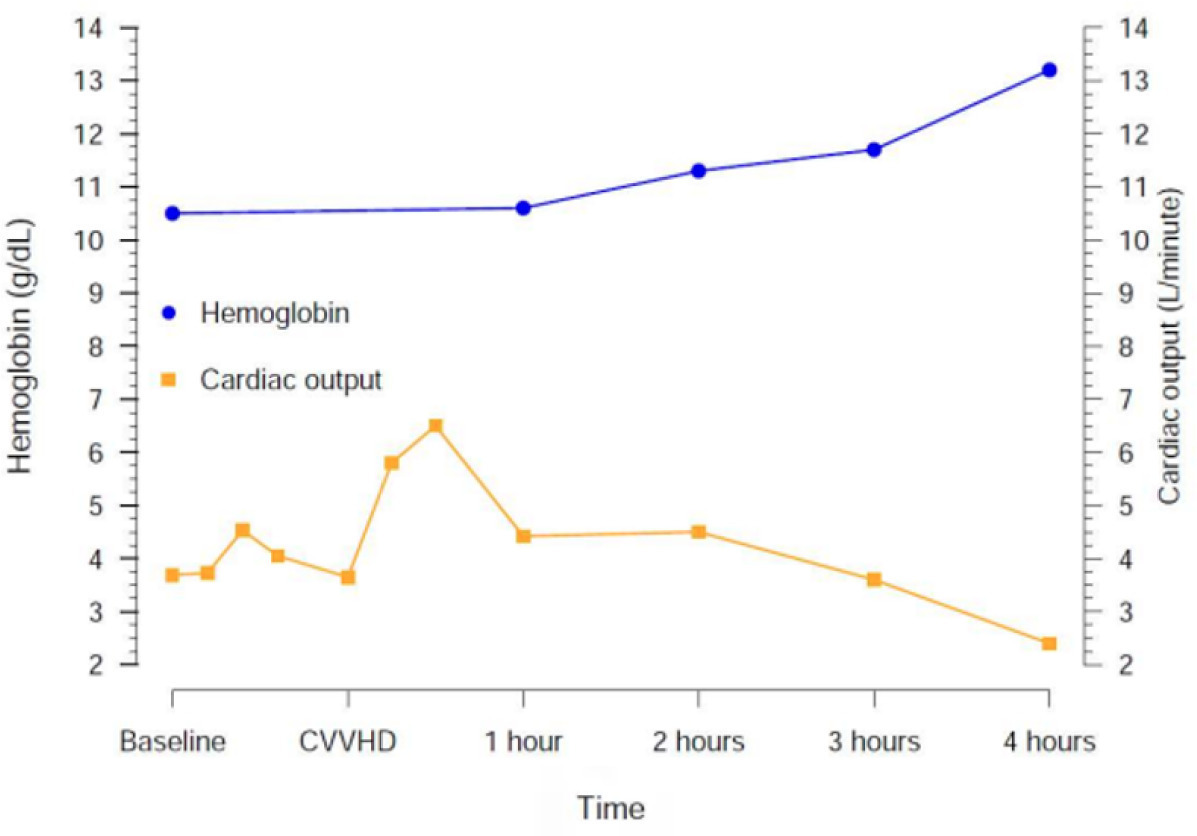
-
Letter to the Editor
Death by community-based methicillin-resistant Staphylococcus aureus: case report
Crit Care Sci. 2023;35(4):416-420
Abstract
Letter to the EditorDeath by community-based methicillin-resistant Staphylococcus aureus: case report
Crit Care Sci. 2023;35(4):416-420
DOI 10.5935/2965-2774.20230078-pt
Views19INTRODUCTIONCommunity methicillin-resistant Staphylococcus aureus (CA-MRSA) has by definition a minimum inhibitory concentration for oxacillin ≥ 4mcg/mL, giving it intrinsic resistance to all beta-lactams, including cephalosporins, which is associated with the presence of the mecA gene. It also has bacteriological and epidemiological characteristics distinct from hospital-acquired MRSA, including its resistance profile to other antimicrobials, its genotypic […]See more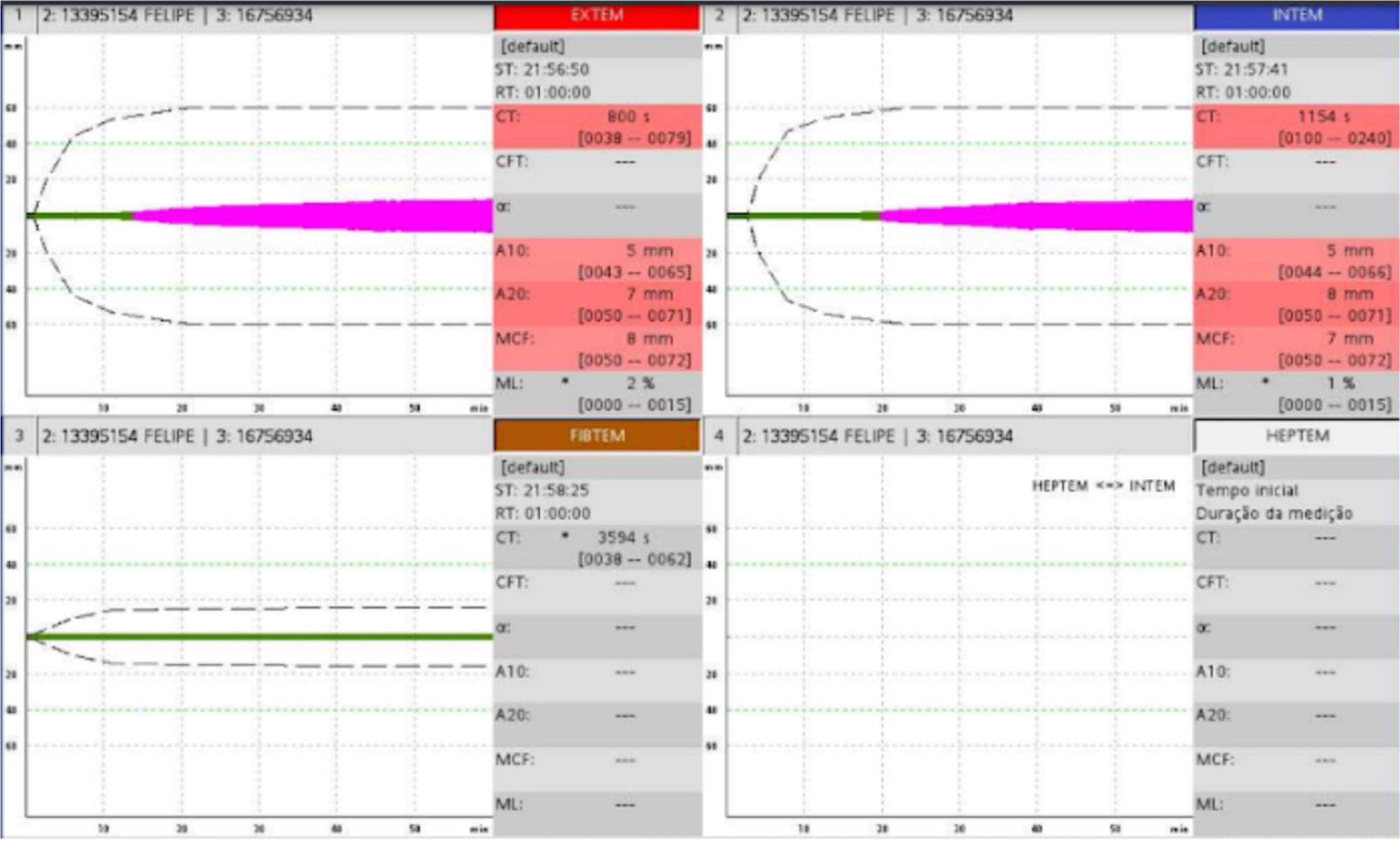
-
Letter to the Editor
Should the citrate used in continuous renal replacement therapy be taken into account as a source of calories?
Crit Care Sci. 2023;35(4):421-422
Abstract
Letter to the EditorShould the citrate used in continuous renal replacement therapy be taken into account as a source of calories?
Crit Care Sci. 2023;35(4):421-422
DOI 10.5935/2965-2774.20230202-pt
Views11To the editorAcute kidney injury is a prevalent organ dysfunction in intensive care units (ICUs) and often affects critically ill patients. Currently, approximately 13.5% of patients require renal replacement therapy (RRT).() Critically ill patients are at a high risk of experiencing hemorrhagic events, and therefore, sodium citrate is the preferred method of anticoagulation in continuous […]See more -
Letter to the Editor
In-hospital extracorporeal cardiopulmonary resuscitation: preliminary results in a second-level hospital
Crit Care Sci. 2023;35(4):423-426
Abstract
Letter to the EditorIn-hospital extracorporeal cardiopulmonary resuscitation: preliminary results in a second-level hospital
Crit Care Sci. 2023;35(4):423-426
DOI 10.5935/2965-2774.20230161-pt
Views38INTRODUCTIONCardiac arrest (CA) is a major health problem associated with serious personal and social consequences. In Spain, 50,000 CA cases are estimated to occur per year, half of which are expected to occur in health care facilities.() The shortand long-term prognoses of these patients are associated with the early initiation of basic and advanced life […]See more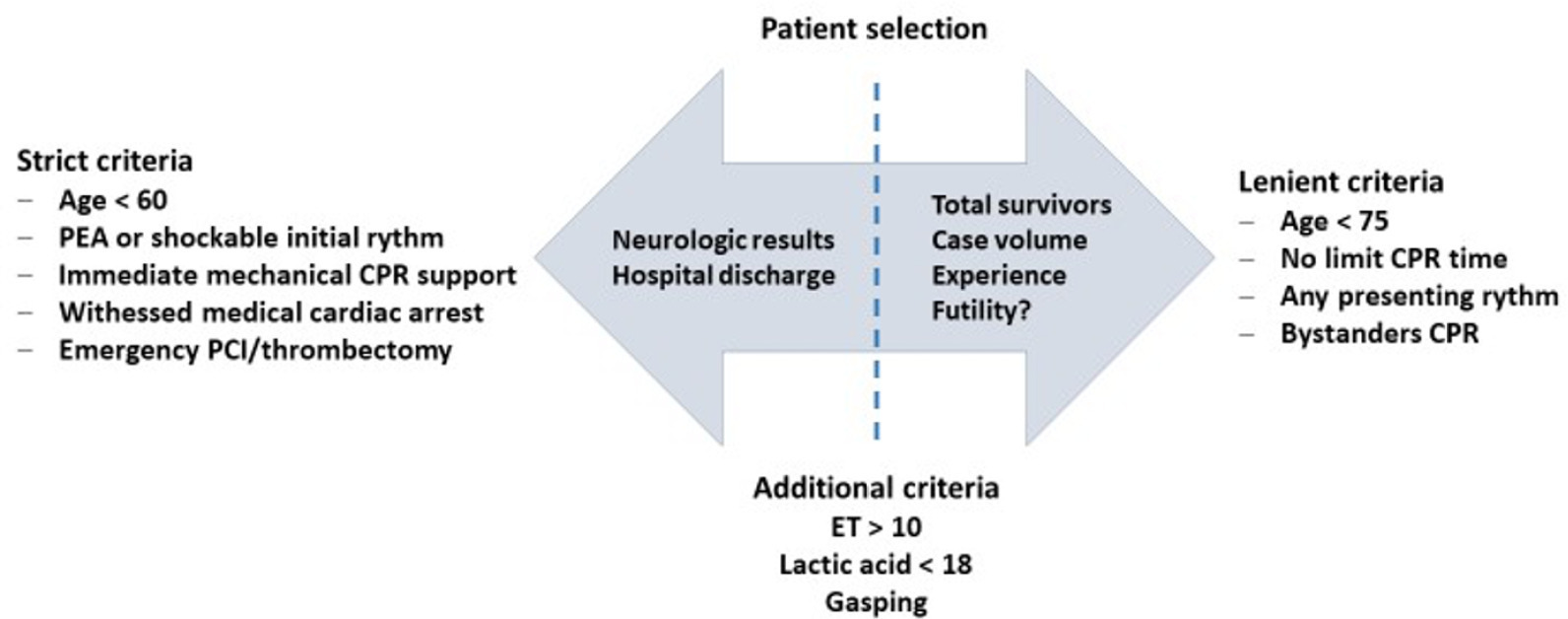
-
Letter to the Editor
To: Posterior reversible encephalopathy syndrome in a child with severe multisystem inflammatory syndrome due to COVID-19
Crit Care Sci. 2023;35(4):427-428
Abstract
Letter to the EditorTo: Posterior reversible encephalopathy syndrome in a child with severe multisystem inflammatory syndrome due to COVID-19
Crit Care Sci. 2023;35(4):427-428
DOI 10.5935/2965-2774.20230283-pt
Views144To the editorWe read with interest the article by Dominguez-Rojas et al. about a severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) polymerase chain reaction (PCR)-negative 9-year-old male who underwent laparotomy for suspected acute abdomen (vomiting, abdominal pain, diarrhea), which was noninformative.() On postoperative day one, the patient experienced respiratory insufficiency attributed to pneumonia with pleural […]See more -
Letter to the Editor
To: Posterior reversible encephalopathy syndrome in a child with severe multisystem inflammatory syndrome due to COVID-19
Crit Care Sci. 2023;35(4):429-430
Abstract
Letter to the EditorTo: Posterior reversible encephalopathy syndrome in a child with severe multisystem inflammatory syndrome due to COVID-19
Crit Care Sci. 2023;35(4):429-430
DOI 10.5935/2965-2774.20230322-pt
Views57To the editorWe eagerly read the article by Dominguez-Rojas et al. about a 9-year-old male with a 3-day history of a gastrointestinal infection who underwent explorative abdominal surgery for acute abdomen, which was noninformative.() Postoperatively, the patient developed pneumonia requiring mechanical ventilation.() After extubation, the patient was diagnosed with multisystem inflammatory syndrome in children (MIS-C) […]See more