-
Editorial
Constipation in critically ill patients: much more than we imagine
Rev Bras Ter Intensiva. 2013;25(2):73-74
Abstract
EditorialConstipation in critically ill patients: much more than we imagine
Rev Bras Ter Intensiva. 2013;25(2):73-74
-
Editorial
Increasing the awareness of delirium in critically ill patients
Rev Bras Ter Intensiva. 2013;25(2):75-76
Abstract
EditorialIncreasing the awareness of delirium in critically ill patients
Rev Bras Ter Intensiva. 2013;25(2):75-76
-
Special Article
How to prepare and submit abstracts for scientific meetings
Rev Bras Ter Intensiva. 2013;25(2):77-80
Abstract
Special ArticleHow to prepare and submit abstracts for scientific meetings
Rev Bras Ter Intensiva. 2013;25(2):77-80
DOI 10.5935/0103-507X.20130016
Views1See moreThe presentation of study results is a key step in scientific research, and submitting an abstract to a meeting is often the first form of public communication. Meeting abstracts have a defined structure that is similar to abstracts for scientific articles, with an introduction, the objective, methods, results and conclusions. However, abstracts for meetings are not presented as part of a full article and, therefore, must contain the necessary and most relevant data. In this article, we detail their structure and include tips to make them technically correct.

-
Special Article
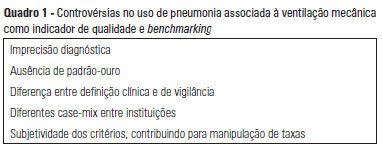
Defining ventilator-associated pneumonia: a (de)construction concept
Rev Bras Ter Intensiva. 2013;25(2):81-86
Abstract
Special ArticleDefining ventilator-associated pneumonia: a (de)construction concept
Rev Bras Ter Intensiva. 2013;25(2):81-86

-
Original Articles – Clinical Research
Incidence of constipation in an intensive care unit
Rev Bras Ter Intensiva. 2013;25(2):87-92
Abstract
Original Articles – Clinical ResearchIncidence of constipation in an intensive care unit
Rev Bras Ter Intensiva. 2013;25(2):87-92
DOI 10.5935/0103-507X.20130018
Views0See moreOBJECTIVES: To evaluate the incidence of constipation in critical patients on enteral nutrition in a hospital intensive care unit and to correlate this incidence with the variables found for critical patients. METHODS: The present investigation was a retrospective analytical study conducted in the intensive care unit of Hospital Regional da Asa Norte (DF) via the analysis of medical records of patients admitted during the period from January to December 2011. Data on the incidence of constipation and enteral nutritional support, gastrointestinal changes, stool frequency, ventilatory support, and outcomes were collected and analyzed. RESULTS: The initial sample consisted of 127 patients admitted to the unit during the period from January to December 2011. Eighty-four patients were excluded, and the final sample consisted of 43 patients. The incidence of constipation, defined as no bowel movement during the first 4 days of hospitalization, was 72% (n=31). The patients were divided into a control group and a constipated group. The group of constipated patients reached the caloric target, on average, at 6.5 days, and the control group reached the caloric target in 5.6 days (p=0.51). Constipation was not associated with the length of hospital stay, suspension of nutritional support, or outcome of hospitalization. There was an association between evacuation during hospitalization and a longer duration of hospitalization for a subgroup of patients who did not evacuate during the entire period (p=0.009). CONCLUSION: The incidence of constipation in the unit studied was 72%. Only the absence of evacuation during hospitalization was associated with longer hospital stays. Constipation was not associated with the length of hospital stay, suspension of nutritional support, or outcome of hospitalization.
-
Original Articles – Clinical Research
Evaluation of functional independence after discharge from the intensive care unit
Rev Bras Ter Intensiva. 2013;25(2):93-98
Abstract
Original Articles – Clinical ResearchEvaluation of functional independence after discharge from the intensive care unit
Rev Bras Ter Intensiva. 2013;25(2):93-98
DOI 10.5935/0103-507X.20130019
Views1See moreOBJECTIVE: 1) To evaluate the functional independence measures immediately after discharge from an intensive care unit and to compare these values with the FIMs 30 days after that period. 2) To evaluate the possible associated risk factors. METHODS: The present investigation was a prospective cohort study that included individuals who were discharged from the intensive care unit and underwent physiotherapy in the unit. Functional independence was evaluated using the functional independence measure immediately upon discharge from the intensive care unit and 30 days thereafter via a phone call. The patients were admitted to the Hospital Santa Clara intensive care unit during the period from May 2011 to August 2011. RESULTS: During the predetermined period of data collection, 44 patients met the criteria for inclusion in the study. The mean age of the patients was 55.4±10.5 years. Twenty-seven of the subjects were female, and 15 patients were admitted due to pulmonary disease. The patients exhibited an functional independence measure of 84.1±24.2. When this measure was compared to the measure at 30 days after discharge, there was improvement across the functional independence variables except for that concerned with sphincter control. There were no significant differences when comparing the gender, age, clinical diagnosis, length of stay in the intensive care unit, duration of mechanical ventilation, and the presence of sepsis during this period. CONCLUSION: Functional independence, as evaluated by the functional independence measure scale, was improved at 30 days after discharge from the intensive care unit, but it was not possible to define the potentially related factors.
-
Original Articles – Clinical Research
The performance of a rapid response team in the management of code yellow events at a university hospital
Rev Bras Ter Intensiva. 2013;25(2):99-105
Abstract
Original Articles – Clinical ResearchThe performance of a rapid response team in the management of code yellow events at a university hospital
Rev Bras Ter Intensiva. 2013;25(2):99-105
DOI 10.5935/0103-507X.20130020
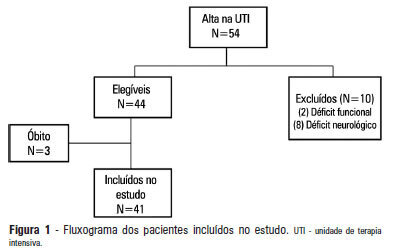
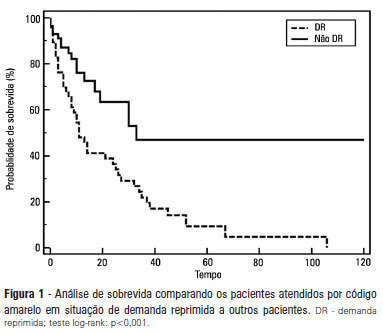
Views0See moreOBJECTIVE: To describe the epidemiological data of the clinical instability events in patients attended to by the rapid response team and to identify prognostic factors. METHODS: This was a longitudinal study, performed from January to July 2010, with an adult inpatient population in a hospital environment. The data collected regarding the code yellow service included the criteria of the clinical instability, the drug and non-drug therapies administered and the activities and procedures performed. The outcomes evaluated were the need for intensive care unit admission and the hospital mortality rates. A level of p=0.05 was considered to be significant. RESULTS: A total of 150 code yellow events that occurred in 104 patients were evaluated. The most common causes were related to acute respiratory insufficiency with hypoxia or a change in the respiratory rate and a concern of the team about the patient’s clinical condition. It was necessary to request a transfer to the intensive care unit in 80 of the 150 cases (53.3%). It was necessary to perform 42 procedures. The most frequent procedures were orotracheal intubation and the insertion of a central venous catheter. The patients who were in critical condition and had to wait for an intensive care unit bed had a higher risk of death compared to the other patients (hazard ratio: 3.12; 95% CI: 1.80-5.40; p<0.001). CONCLUSIONS: There are patients in critical condition that require expert intensive care in the regular ward unit hospital beds. The events that most frequently led to the code yellow activation were related to hemodynamic and respiratory support. The interventions performed indicate the need for a physician on the team. The situation of pent-up demand is associated with a higher mortality rate.
-
Original Articles – Clinical Research
Translation, adaptation, and validation of the Sunderland Scale and the Cubbin & Jackson Revised Scale in Portuguese
Rev Bras Ter Intensiva. 2013;25(2):106-114
Abstract
Original Articles – Clinical ResearchTranslation, adaptation, and validation of the Sunderland Scale and the Cubbin & Jackson Revised Scale in Portuguese
Rev Bras Ter Intensiva. 2013;25(2):106-114
DOI 10.5935/0103-507X.20130021
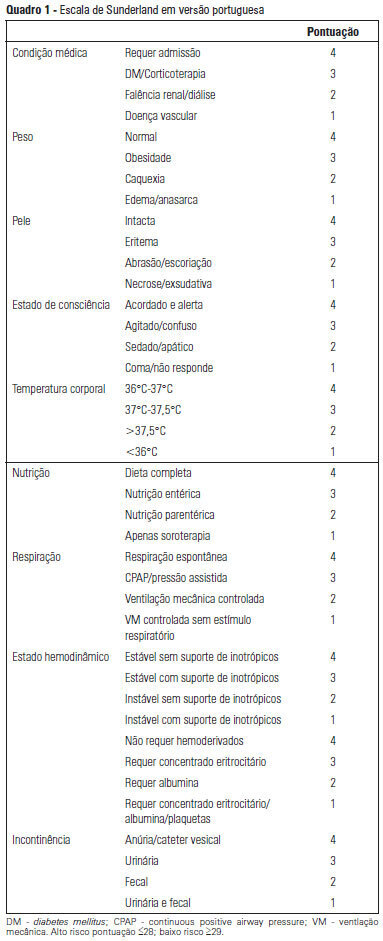
Views0See moreOBJECTIVE: To Translate into Portuguese and evaluate the measuring properties of the Sunderland Scale and the Cubbin & Jackson Revised Scale, which are instruments for evaluating the risk of developing pressure ulcers during intensive care. METHODS: This study included the process of translation and adaptation of the scales to the Portuguese language, as well as the validation of these tools. To assess the reliability, Cronbach alpha values of 0.702 to 0.708 were identified for the Sunderland Scale and the Cubbin & Jackson Revised Scale, respectively. The validation criteria (predictive) were performed comparatively with the Braden Scale (gold standard), and the main measurements evaluated were sensitivity, specificity, positive predictive value, negative predictive value, and area under the curve, which were calculated based on cutoff points. RESULTS: The Sunderland Scale exhibited 60% sensitivity, 86.7% specificity, 47.4% positive predictive value, 91.5% negative predictive value, and 0.86 for the area under the curve. The Cubbin & Jackson Revised Scale exhibited 73.3% sensitivity, 86.7% specificity, 52.4% positive predictive value, 94.2% negative predictive value, and 0.91 for the area under the curve. The Braden scale exhibited 100% sensitivity, 5.3% specificity, 17.4% positive predictive value, 100% negative predictive value, and 0.72 for the area under the curve. CONCLUSIONS: Both tools demonstrated reliability and validity for this sample. The Cubbin & Jackson Revised Scale yielded better predictive values for the development of pressure ulcers during intensive care.
-
Original Articles – Clinical Research
Effects of educational intervention on adherence to the technical recommendations for tracheobronchial aspiration in patients admitted to an intensive care unit
Rev Bras Ter Intensiva. 2013;25(2):115-122
Abstract
Original Articles – Clinical ResearchEffects of educational intervention on adherence to the technical recommendations for tracheobronchial aspiration in patients admitted to an intensive care unit
Rev Bras Ter Intensiva. 2013;25(2):115-122
DOI 10.5935/0103-507X.20130022
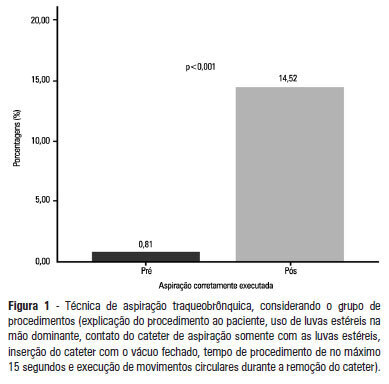
Views0See moreOBJECTIVE: To evaluate the effectiveness of an educational intervention on healthcare professionals’ adherence to the technical recommendations for tracheobronchial aspiration in intensive care unit patients. METHODS: A quasi-experimental study was performed to evaluate intensive care unit professionals’ adherence to the tracheobronchial aspiration technical recommendations in intensive care unit patients both before and after a theoretical and practical educational intervention. Comparisons were performed using the chi-square test, and the significance level was set to p<0.05. RESULTS: A total of 124 procedures, pre- and post-intervention, were observed. Increased adherence was observed in the following actions: the use of personal protective equipment (p=0.01); precaution when opening the catheter package (p<0.001); the use of a sterile glove on the dominant hand to remove the catheter (p=0.003); the contact of the sterile glove with the catheter only (p<0.001); the execution of circular movements during the catheter removal (p<0.001); wrapping the catheter in the sterile glove at the end of the procedure (p=0.003); the use of distilled water, opened at the start of the procedure, to wash the connection latex (p=0.002); the disposal of the leftover distilled water at the end of the procedure (p<0.001); and the performance of the aspiration technique procedures (p<0.001). CONCLUSION: There was a low adherence by health professionals to the preventive measures against hospital infection, indicating the need to implement educational strategies. The educational intervention used was shown to be effective in increasing adherence to the technical recommendations for tracheobronchial aspiration.
-
Original Articles – Clinical Research
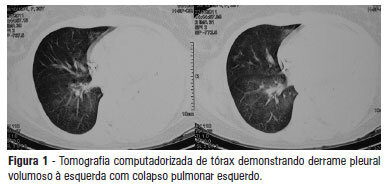
Acute kidney injury in critically ill patients with lung disease: kidney-lung crosstalk
Rev Bras Ter Intensiva. 2013;25(2):130-136
Abstract
Original Articles – Clinical ResearchAcute kidney injury in critically ill patients with lung disease: kidney-lung crosstalk
Rev Bras Ter Intensiva. 2013;25(2):130-136
DOI 10.5935/0103-507X.20130024
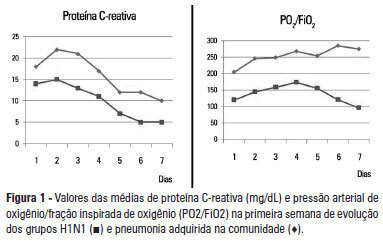
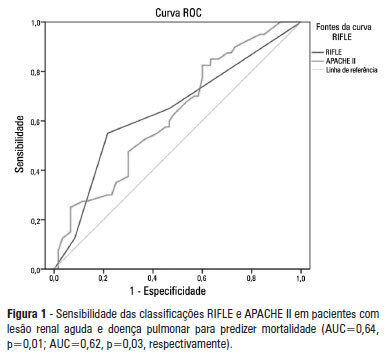
Views0See moreOBJECTIVE: To examine the factors associated with acute kidney injury and outcome in patients with lung disease. METHODS: A prospective study was conducted with 100 consecutive patients admitted to a respiratory intensive care unit in Fortaleza (CE), Brazil. The risk factors for acute kidney injury and mortality were investigated in a group of patients with lung diseases. RESULTS: The mean age of the study population was 57 years, and 50% were male. The incidence of acute kidney injury was higher in patients with PaO2/FiO2<200 mmHg (54% versus 23.7%; p=0.02). Death was observed in 40 cases and the rate of mortality of the acute kidney injury group was higher (62.8% versus 27.6%; p=0.01). The independent factor that was found to be associated with acute kidney injury was PaO2/FiO2<200 mmHg (p=0.01), and the independent risk factors for death were PEEP at admission (OR: 3.6; 95%CI: 1.3-9.6; p=0.009) and need for hemodialysis (OR: 7.9; 95%CI: 2.2-28.3; p=0.001). CONCLUSION: There was a higher mortality rate in the acute kidney injury group. Increased mortality was associated with mechanical ventilation, high PEEP, urea and need for dialysis. Further studies must be performed to better establish the relationship between kidney and lung injury and its impact on patient outcome.
-
Review Articles
Delirium in intensive care: an under-diagnosed reality
Rev Bras Ter Intensiva. 2013;25(2):137-147
Abstract
Review ArticlesDelirium in intensive care: an under-diagnosed reality
Rev Bras Ter Intensiva. 2013;25(2):137-147
DOI 10.5935/0103-507X.20130025
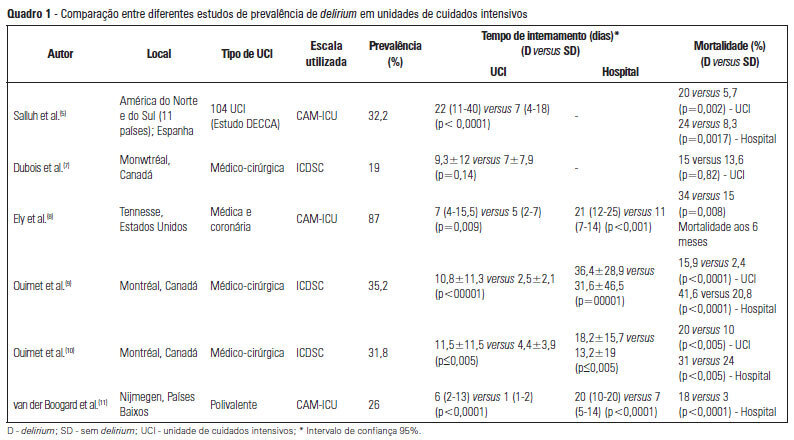
Views0See moreDelirium occurs in up to 80% of patients admitted to intensive care units. Although under-diagnosed, delirium is associated with a significant increase in morbidity and mortality in critical patients. Here, we review the main risk factors, clinical manifestations and preventative and therapeutic approaches (pharmacological and non-pharmacological) for this illness.
-
Review Articles
Delirium rating scales in critically ill patients: a systematic literature review
Rev Bras Ter Intensiva. 2013;25(2):148-154
Abstract
Review ArticlesDelirium rating scales in critically ill patients: a systematic literature review
Rev Bras Ter Intensiva. 2013;25(2):148-154
DOI 10.5935/0103-507X.20130026
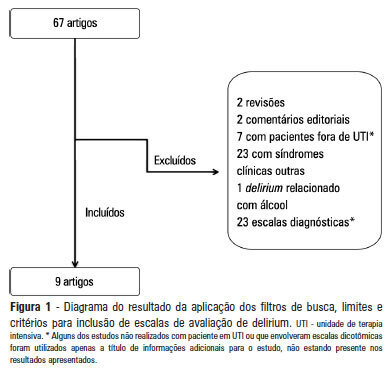
Views0See moreOBJECTIVE: To identify scales that can establish a quantitative assessment of delirium symptoms in critically ill patients through a systematic review. METHODS: Studies that evaluated delirium stratification scales in patients hospitalized in intensive care units were selected in a search performed in the MedLine database. Validation studies of these scales and their target patient populations were analyzed, and we identified the examiner and the signs and symptoms evaluated. In addition, the duration of the application and the sensitivity and specificity of each scale were assessed. RESULTS: Six scales were identified: the Delirium Detection Score, the Cognitive Test of Delirium, the Memorial Delirium Assessment Scale, the Intensive Care Delirium Screening Checklist, The Neelon and Champagne Confusion Scale and the Delirium Rating Scale-Revised-98. CONCLUSION: The scales identified allow the stratification and monitoring of critically ill patients with delirium. Among the six scales, the most studied and best suited for use in the intensive care units was the Intensive Care Delirium Screening
-
Review Articles
Perceptions and practices regarding delirium, sedation and analgesia in critically ill patients: a narrative review
Rev Bras Ter Intensiva. 2013;25(2):155-161
Abstract
Review ArticlesPerceptions and practices regarding delirium, sedation and analgesia in critically ill patients: a narrative review
Rev Bras Ter Intensiva. 2013;25(2):155-161
DOI 10.5935/0103-507X.20130027
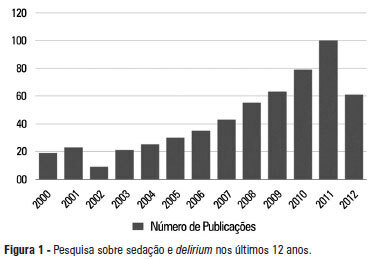
Views0See moreA significant number of landmark studies have been published in the last decade that increase the current knowledge on sedation for critically ill patients. Therefore, many practices that were considered standard of care are now outdated. Oversedation has been shown to be hazardous, and light sedation and no-sedation protocols are associated with better patient outcomes. Delirium is increasingly recognized as a major form of acute brain dysfunction that is associated with higher mortality, longer duration of mechanical ventilation and longer lengths of stay in the intensive care unit and hospital. Despite all the available evidence, translating research into bedside care is a daunting task. International surveys have shown that practices such as sedation interruption and titration are performed only in the minority of cases. Implementing best practices is a major challenge that must also be addressed in the new guidelines. In this review, we summarize the findings of sedation and delirium research over the last years. We also discuss the gap between evidence and clinical practice and highlight ways to implement best practices at the bedside.
-
Review Articles
Drug-nutrient interactions in the intensive care unit: literature review and current recommendations
Rev Bras Ter Intensiva. 2013;25(2):162-167
Abstract
Review ArticlesDrug-nutrient interactions in the intensive care unit: literature review and current recommendations
Rev Bras Ter Intensiva. 2013;25(2):162-167
DOI 10.5935/0103-507X.20130028
Views0OBJECTIVE: To describe the interactions between drugs and nutrients and their frequency in the intensive care unit and to assess the professional team’s awareness regarding this subject. METHODS: The keywords “drug interactions” and “nutrition therapy” were searched in the PubMed (specifically MeSH) electronic database. The studies were systematically reviewed for descriptions of the types of interactions between drugs and nutrients, including their frequency and consequences. RESULTS: Sixty-seven articles were found. Among these, 20 articles were appropriate for the methodology adopted and accomplished the objectives of the study. Of these 20 articles, 14 articles described interactions between drugs and enteral nutrition, three described interactions between drugs and parenteral nutrition, and three described the importance and care required to avoid such interactions. CONCLUSIONS: The literature about drug and nutrient interactions is limited and suggests the inability of health care teams to recognize the potential for these interactions. Possibly, the elaboration of a protocol to evaluate drug-nutrient interactions will increase the safety and efficacy of therapeutics.
Keywords:Critical careDrug interactionsIntensive careNutrientsnutrition therapyPharmaceutical preparationsSee more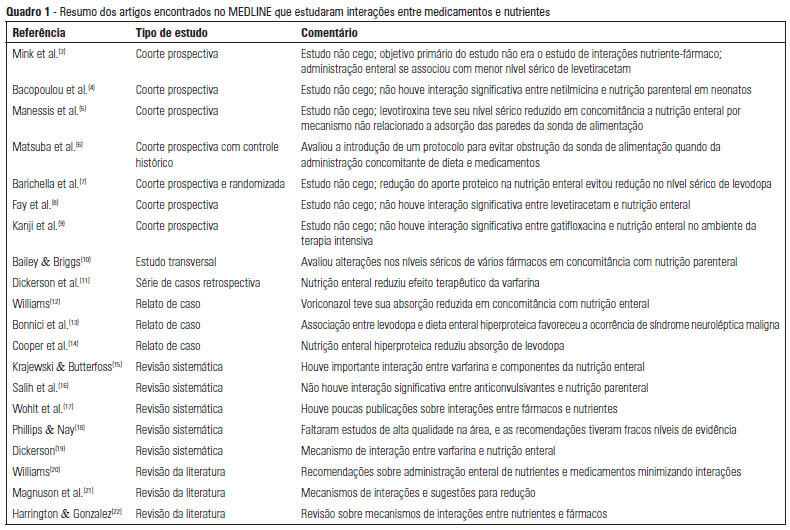
-
Review Articles
Use of femoral vein catheters for the assessment of perfusion parameters
Rev Bras Ter Intensiva. 2013;25(2):168-174
Abstract
Review ArticlesUse of femoral vein catheters for the assessment of perfusion parameters
Rev Bras Ter Intensiva. 2013;25(2):168-174
DOI 10.5935/0103-507X.20130029
Views0The use of central venous oxygen saturation (SvcO2) and arterial lactate in the diagnosis of severe tissue hypoperfusion is well established, and the optimization of these parameters is currently under investigation, particularly in patients with severe sepsis/septic shock. However, the only place for deep venous puncture or the first choice for puncture is often the femoral vein. Although venous saturation obtained from blood sampling from this catheter, instead of SvcO2, has already been used in the diagnosis of severe tissue hypoperfusion, little is known about the accuracy of the results. The venous lactate in place of arterial puncture has also been used to guide therapeutic decisions. We conducted this literature review to seek evidence on the correlation and concordance of parameters obtained by collecting femoral venous blood gases in relation to SvcO2 and arterial lactate. Few studies in the literature have evaluated the use of femoral venous oxygen saturation (SvfO2) or venous lactate. The results obtained thus far demonstrate no adequate agreement between SvfO2 and SvcO2, which limits the clinical use of SvfO2. However, the apparent strong correlation between arterial and peripheral and central venous lactate values suggests that venous lactate obtained from the femoral vein could eventually be used instead of arterial lactate, although there is insufficient evidence on which to base this procedure at this time.
Keywords:Catheterization, centralCentral venous pressureFemoral veinHemodynamicsOxygenPerfusionSepsisSee more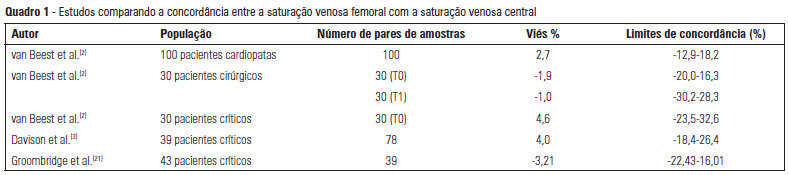
-
Case Report
Spontaneous acute subdural hematoma and intracerebral hemorrhage in a patient with thrombotic microangiopathy during pregnancy
Rev Bras Ter Intensiva. 2013;25(2):175-180
Abstract
Case ReportSpontaneous acute subdural hematoma and intracerebral hemorrhage in a patient with thrombotic microangiopathy during pregnancy
Rev Bras Ter Intensiva. 2013;25(2):175-180
DOI 10.5935/0103-507X.20130030
Views0Preeclampsia, HELLP syndrome (hemolysis, elevated liver enzymes, and low-platelet count), and acute fatty liver of pregnancy are the main causes of thrombotic microangiopathy and evere liver dysfunction during pregnancy and represent different manifestations of the same pathological continuum. The case of a 35-week pregnant woman who was admitted to an intensive care unit immediately after a Cesarean section due to fetal death and the presence of nausea, vomiting, and jaundice is reported. Postpartum preeclampsia and acute fatty liver of pregnancy were diagnosed. The patient developed an acute subdural hematoma and an intracerebral hemorrhage, which were subjected to neurosurgical treatment. The patient died from refractory hemolytic anemia and spontaneous bleeding of multiple organs. Preeclampsia HELLP syndrome, and acute fatty liver of pregnancy might overlap and be associated with potentially fatal complications, including intracranial hemorrhage, as in the present case. Early detection and diagnosis are crucial to ensure management and treatment success.
Keywords:Acute subdural hematomaCase reportsCerebral hemorrhageFatty liverHELLP syndromeHemolytic anemiapregnancySee more