-
Editorial
Tackling healthcare-associated infections in Brazilian intensive care units: we need more than collaboration
Rev Bras Ter Intensiva. 2022;34(3):313-315
Abstract
EditorialTackling healthcare-associated infections in Brazilian intensive care units: we need more than collaboration
Rev Bras Ter Intensiva. 2022;34(3):313-315
DOI 10.5935/0103-507X.2022editorial-en
Views3Healthcare-associated infections (HAIs) and antimicrobial resistance (AMRs) demand a global effort for their containment.() Healthcare-associated infections have an estimated prevalence between 7 and 10% worldwide, whereas the incidence is greater than 15% in developing countries. This difference is more remarkable when comparing the incidence of HAIs in intensive care units (ICUs) with estimated values of […]See more -
Commentary
Subphenotyping of critical illness: where protocolized and personalized intensive care medicine meet
Rev Bras Ter Intensiva. 2022;34(3):316-318
Abstract
CommentarySubphenotyping of critical illness: where protocolized and personalized intensive care medicine meet
Rev Bras Ter Intensiva. 2022;34(3):316-318
DOI 10.5935/0103-507X.20220069-en
Views1INTRODUCTIONIn recent decades, successful quality improvement initiatives in critical care have been tested, and among the included principles were to “do no harm” (which means to prevent intensive care unit-acquired complications and to avoid overtreatment) and to provide early interventions for acute conditions (i.e., antibiotics for sepsis, as well as reperfusions for stroke and myocardial […]See more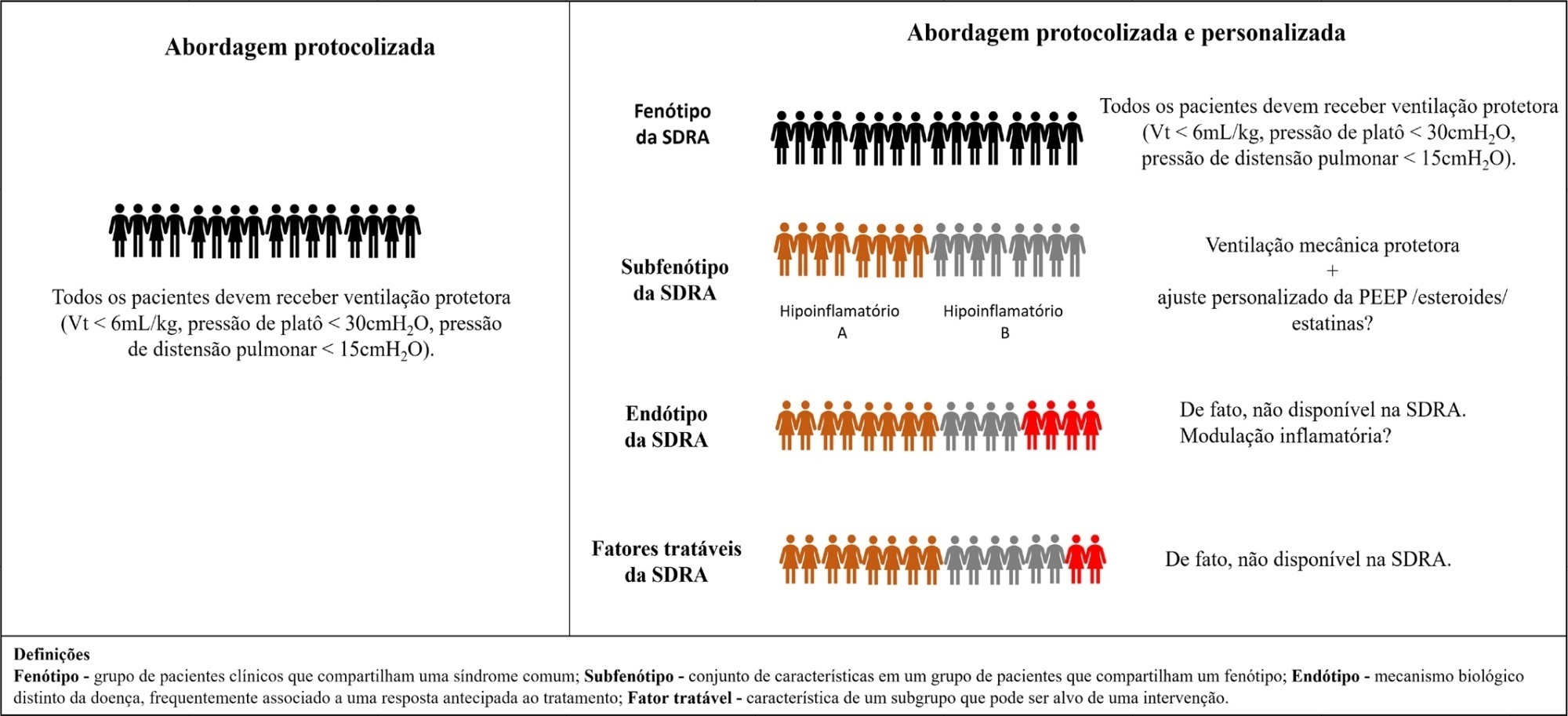
-
Special Article
Automated documentation of vital parameters in wards using portable stations – Effect on proper triggering of the rapid response team: a study protocol of a cluster randomized clinical trial
Rev Bras Ter Intensiva. 2022;34(3):319-326
Abstract
Special ArticleAutomated documentation of vital parameters in wards using portable stations – Effect on proper triggering of the rapid response team: a study protocol of a cluster randomized clinical trial
Rev Bras Ter Intensiva. 2022;34(3):319-326
DOI 10.5935/0103-507X.20220101-en
Views2ABSTRACT
Objective:
To evaluate the effectiveness of the Welch Allyn Connex® Spot Monitor/Hillrom Connecta™ solution in activating the rapid response team in a timely manner compared to manual activation.
Methods:
The Hillrom study is a single-center, open-label, superiority, cluster-randomized, parallel-group (1:1 allocation ratio) clinical trial that will be conducted in a tertiary hospital. Two sets of three wards with 28 beds will be included (one as the intervention cluster and the other as the control). The wards will be randomly assigned to use the Welch Allyn Connex® Spot Monitor/Hillrom Connecta™ automated solution (intervention cluster) or to maintain the usual routine (control cluster) regarding rapid response team activation. The primary outcome will be the absolute number of episodes of rapid response team triggering in an appropriate time; as secondary outcomes, clinical features (mortality, cardiac arrest, need for intensive care unit admission and duration of hospitalization) will be assessed according to clusters in an exploratory way. A sample size of 216 rapid response team activations was estimated to identify a possible difference between the groups. The protocol has been approved by the institutional Research Ethics Committee.
Expected results:
The Welch Allyn Connex® Spot Monitor/Hillrom Connecta™ automated solution is expected to be more effective in triggering the nurse call system to activate the rapid response team in a timely and adequate manner compared to manual triggering (usual practice).
ClinicalTrials.gov:
NCT04648579
Keywords:computerizedHealth information interoperabilityHospital rapid response teamMedical records systemsNursing stationsVital signsSee more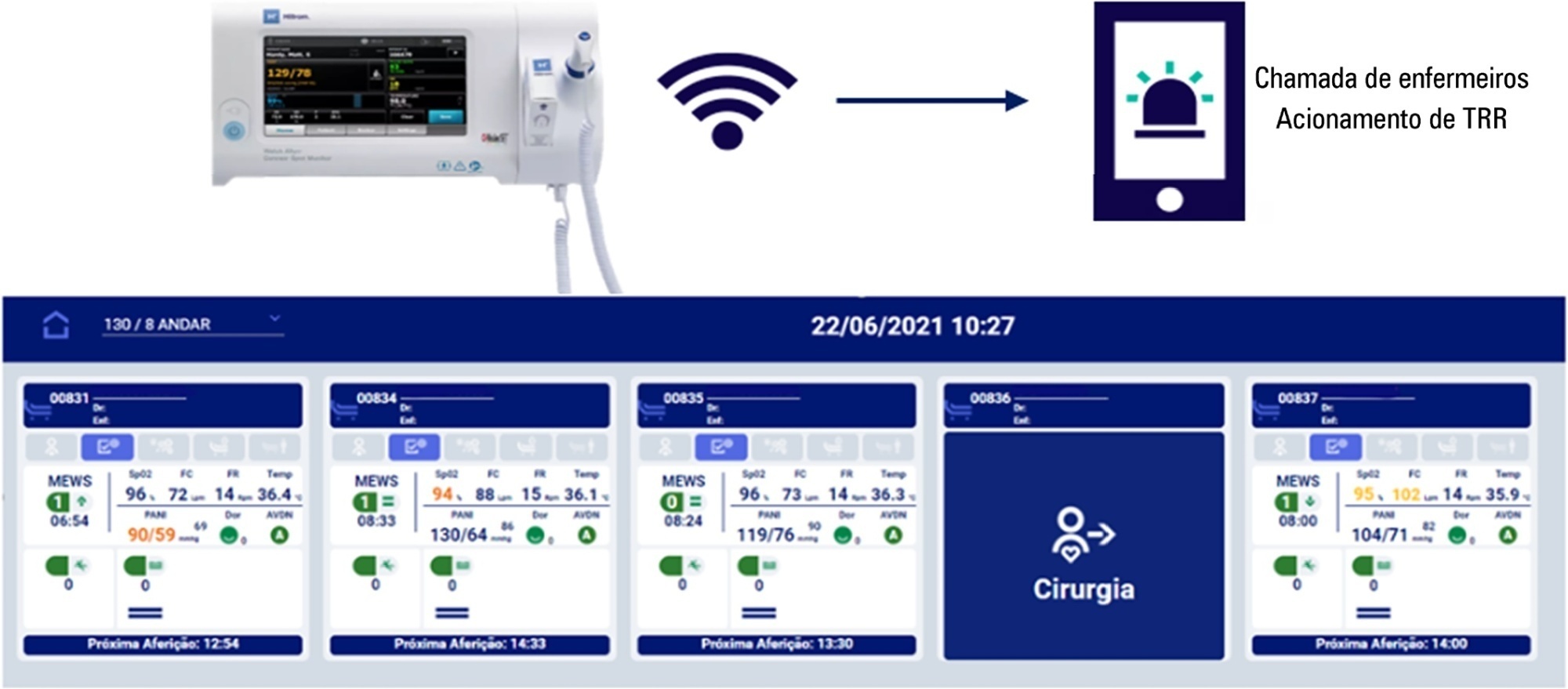
-
Original Article
Success factors of a collaborative project to reduce healthcare-associated infections in intensive care units in Northeastern Brazil
Rev Bras Ter Intensiva. 2022;34(3):327-334
Abstract
Original ArticleSuccess factors of a collaborative project to reduce healthcare-associated infections in intensive care units in Northeastern Brazil
Rev Bras Ter Intensiva. 2022;34(3):327-334
DOI 10.5935/0103-507X.20220070-en
Views1ABSTRACT
Objective:
To describe the implementation and results of the collaborative PROADI-SUS project by the Brazilian Ministry of Health to reduce healthcare-associated infections: ventilator-associated pneumonia, primary central line-associated bloodstream infection and catheter-associated urinary tract infections.
Methods:
This was a prospective observational study that investigated the implementation stages and outcomes during 18 months in five intensive care units in the city of Recife. Reductions in healthcare-associated infections in each unit were calculated using previous medians compared to those of the study period.
Results:
The goal of reducing the three healthcare-associated infections, i.e., 30% in 18 months, was achieved in at least one of the healthcare-associated infections and was also achieved for two healthcare-associated infections in two hospitals and three healthcare-associated infections in just one hospital; the latter reached the target of 36 months. Implementing the bundles and monitoring the results by the professionals were considered essential actions by the local management teams. In addition, the acquisition of supplies and their availability alongside the beds, signage, checklists, staff awareness, adaptation, team building, training and celebration of achievements were assessed as being relevant for reducing healthcare-associated infections.
Conclusion:
The collaborative approach reduced healthcare-associated infections, despite partial adherence to the bundles. The hypothesis is that success is related to the project methodology and motivated multidisciplinary teams, especially nursing teams.
Keywords:Health evaluationHealthcare-associated pneumoniaImplementation scienceInfectionsIntensive care unitsOutcome and process assessment (Health Care)Outcome assessment, health carePatient safetyProgram developmentQuality improvementRespiration, artificialSee more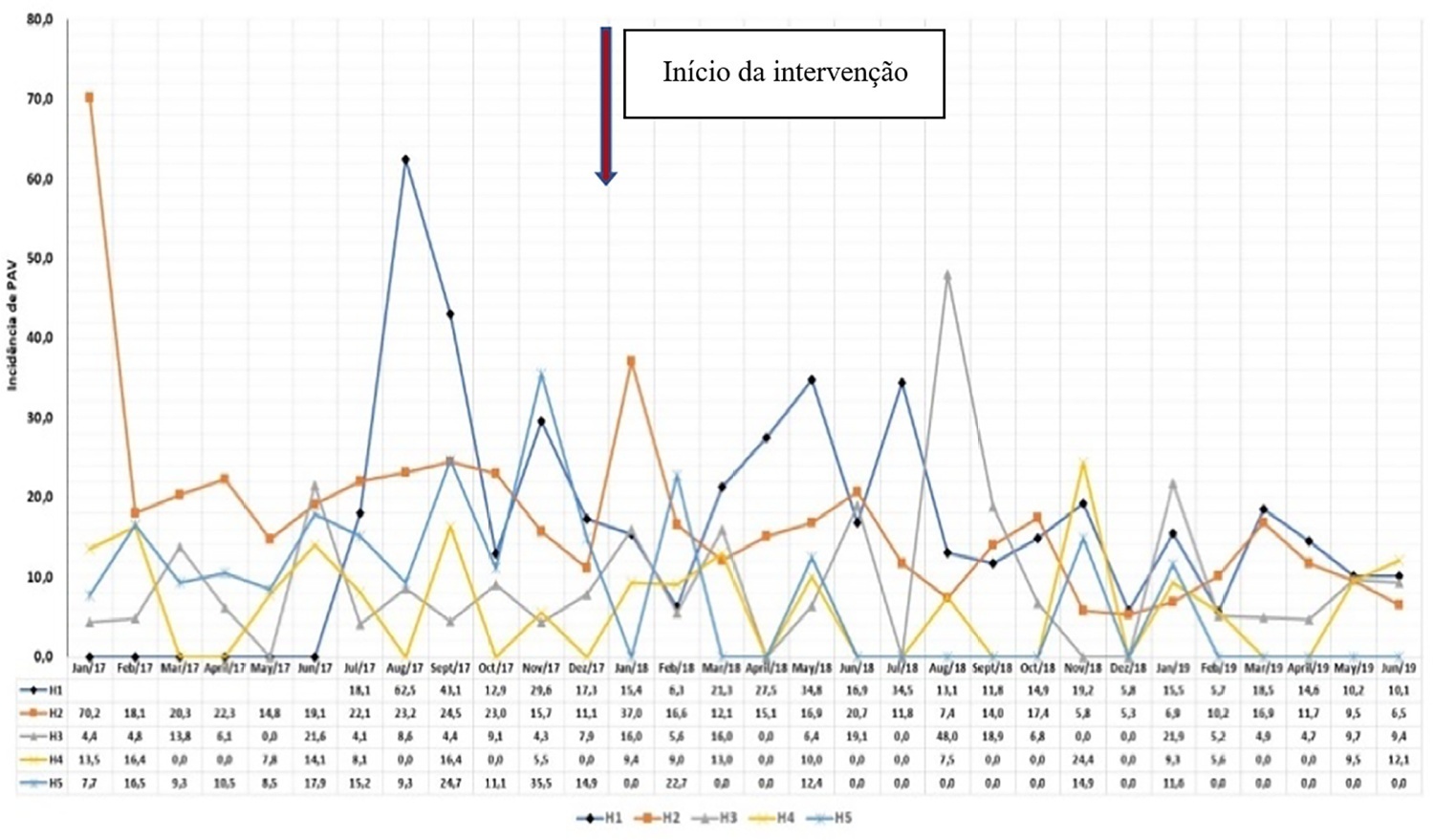
-
Original Article
Clinical outcomes and lung mechanics characteristics between COVID-19 and non-COVID-19-associated acute respiratory distress syndrome: a propensity score analysis of two major randomized trials
Rev Bras Ter Intensiva. 2022;34(3):335-341
Abstract
Original ArticleClinical outcomes and lung mechanics characteristics between COVID-19 and non-COVID-19-associated acute respiratory distress syndrome: a propensity score analysis of two major randomized trials
Rev Bras Ter Intensiva. 2022;34(3):335-341
DOI 10.5935/0103-507X.20220040-en
Views3ABSTRACT
Objective:
To compare the lung mechanics and outcomes between COVID-19-associated acute respiratory distress syndrome and non-COVID-19-associated acute respiratory distress syndrome.
Methods:
We combined data from two randomized trials in acute respiratory distress syndrome, one including only COVID-19 patients and the other including only patients without COVID-19, to determine whether COVID-19-associated acute respiratory distress syndrome is associated with higher 28-day mortality than non-COVID-19 acute respiratory distress syndrome and to examine the differences in lung mechanics between these two types of acute respiratory distress syndrome.
Results:
A total of 299 patients with COVID-19-associated acute respiratory distress syndrome and 1,010 patients with non-COVID-19-associated acute respiratory distress syndrome were included in the main analysis. The results showed that non-COVID-19 patients used higher positive end-expiratory pressure (12.5cmH2O; SD 3.2 versus 11.7cmH2O SD 2.8; p < 0.001), were ventilated with lower tidal volumes (5.8mL/kg; SD 1.0 versus 6.5mL/kg; SD 1.2; p < 0.001) and had lower static respiratory compliance adjusted for ideal body weight (0.5mL/cmH2O/kg; SD 0.3 versus 0.6mL/cmH2O/kg; SD 0.3; p = 0.01). There was no difference between groups in 28-day mortality (52.3% versus 58.9%; p = 0.52) or mechanical ventilation duration in the first 28 days among survivors (13 [IQR 5 – 22] versus 12 [IQR 6 – 26], p = 0.46).
Conclusion:
This analysis showed that patients with non-COVID-19-associated acute respiratory distress syndrome have different lung mechanics but similar outcomes to COVID-19-associated acute respiratory distress syndrome patients. After propensity score matching, there was no difference in lung mechanics or outcomes between groups.
Keywords:Coronavirus infectionsCOVID-19Critical careCritical care outcomesRespiratory distress syndromeRespiratory mechanicsSee more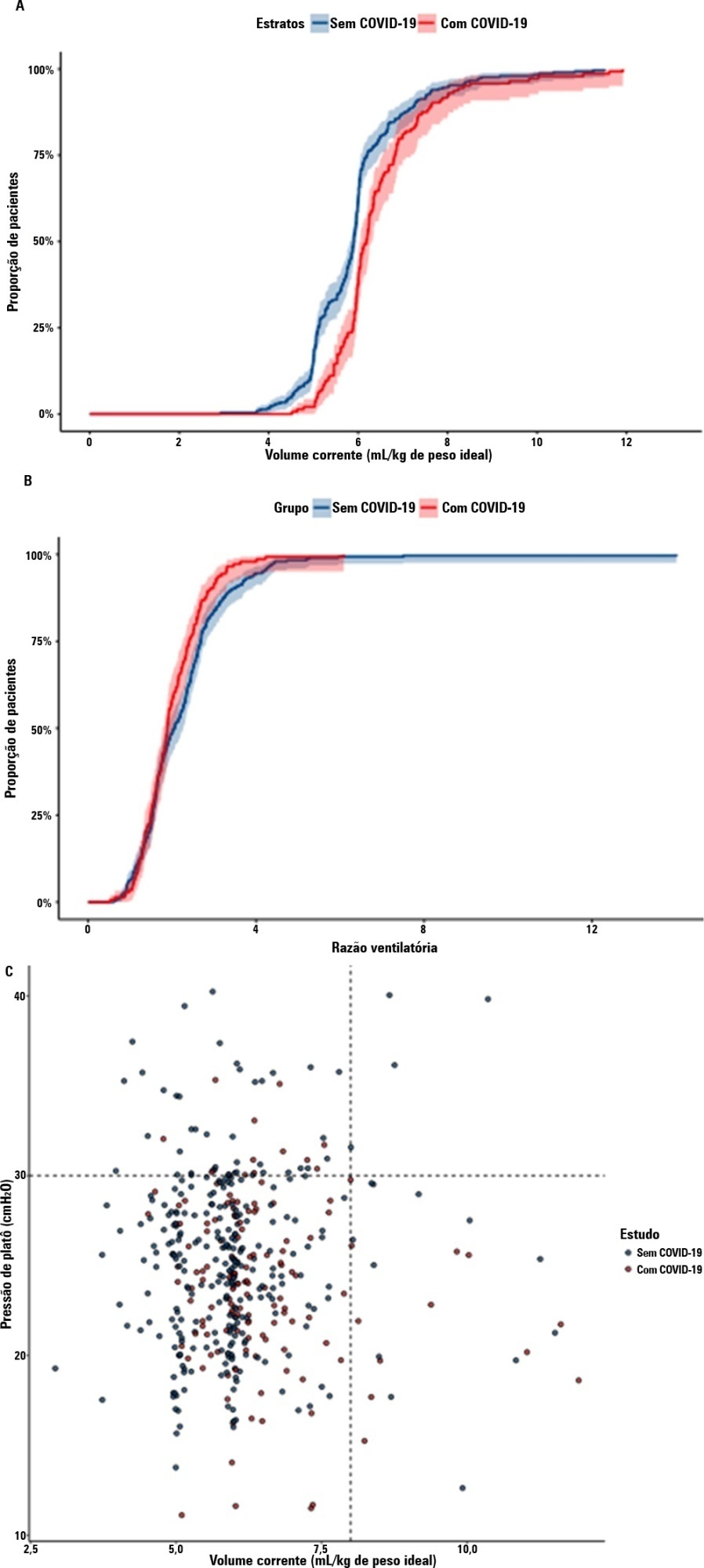
-
Original Article
Critical COVID-19 and neurological dysfunction – a direct comparative analysis between SARS-CoV-2 and other infectious pathogens
Rev Bras Ter Intensiva. 2022;34(3):342-350
Abstract
Original ArticleCritical COVID-19 and neurological dysfunction – a direct comparative analysis between SARS-CoV-2 and other infectious pathogens
Rev Bras Ter Intensiva. 2022;34(3):342-350
DOI 10.5935/0103-507X.20220229-en
Views11ABSTRACT
Objective:
To evaluate whether critical SARS-CoV-2 infection is more frequently associated with signs of corticospinal tract dysfunction and other neurological signs, symptoms, and syndromes, than other infectious pathogens.
Methods:
This was a prospective cohort study with consecutive inclusion of patients admitted to intensive care units due to primary infectious acute respiratory distress syndrome requiring invasive mechanical ventilation > 48 hours. Eligible patients were randomly assigned to three investigators for clinical evaluation, which encompassed the examination of signs of corticospinal tract dysfunction. Clinical data, including other neurological complications and possible predictors, were independently obtained from clinical records.
Results:
We consecutively included 54 patients with acute respiratory distress syndrome, 27 due to SARS-CoV-2 and 27 due to other infectious pathogens. The groups were comparable in most characteristics. COVID-19 patients presented a significantly higher risk of neurological complications (RR = 1.98; 95%CI 1.23 – 3.26). Signs of corticospinal tract dysfunction tended to be more prevalent in COVID-19 patients (RR = 1.62; 95%CI 0.72 – 3.44).
Conclusion:
Our study is the first comparative analysis between SARS-CoV-2 and other infectious pathogens, in an intensive care unit setting, assessing neurological dysfunction. We report a significantly higher risk of neurological dysfunction among COVID-19 patients. As such, we suggest systematic screening for neurological complications in severe COVID-19 patients.
Keywords:Coronavirus infectionsCOVID-19Intensive careNeurological manifestationsPyramidal tractRespiratory distress syndromeSARS-CoV-2See more -
Original Article
Robust, maintainable, emergency invasive mechanical ventilator
Rev Bras Ter Intensiva. 2022;34(3):351-359
Abstract
Original ArticleRobust, maintainable, emergency invasive mechanical ventilator
Rev Bras Ter Intensiva. 2022;34(3):351-359
DOI 10.5935/0103-507X.20220383-en
Views1ABSTRACT
Objective:
To develop a simple, robust, safe and efficient invasive mechanical ventilator that can be used in remote areas of the world or war zones where the practical utility of more sophisticated equipment is limited by considerations of maintainability, availability of parts, transportation and/or cost.
Methods:
The device implements the pressure-controlled continuous mandatory ventilation mode, complemented by a simple assist-control mode. Continuous positive airway pressure is also possible. The consumption of compressed gases is minimized by avoiding a continuous flow of oxygen or air. Respiratory rates and inspiration/expiration time ratios are electronically determined, and an apnea/power loss alarm is provided.
Results:
The pressure profiles were measured for a range of conditions and found to be adjustable within a ± 2.5cmH2O error margin and stable well within this range over a 41-hour period. Respiratory cycle timing parameters were precise within a few percentage points over the same period. The device was tested for durability for an equivalent period of four months. Chemical and biological tests failed to identify any contamination of the gas by volatile organic compounds or microorganisms. A ventilation test on a large animal, in comparison with a well established ventilator, showed that the animal could be adequately ventilated over a period of 60 minutes, without any noticeable negative aftereffects during the subsequent 24-hour period.
Conclusion:
This ventilator design may be viable, after further animal tests and formal approval by the competent authorities, for clinical application in the abovementioned atypical circumstances.
Keywords:AnimalsContinuous positive airway pressureGasesmechanicalOxygenPulmonary VentilationRespiratory rateventilatorsVolatile organic compoundsSee more
-
Original Article
The Respiratory Rate-Oxygenation Index predicts failure of post-extubation high-flow nasal cannula therapy in intensive care unit patients: a retrospective cohort study
Rev Bras Ter Intensiva. 2022;34(3):360-366
Abstract
Original ArticleThe Respiratory Rate-Oxygenation Index predicts failure of post-extubation high-flow nasal cannula therapy in intensive care unit patients: a retrospective cohort study
Rev Bras Ter Intensiva. 2022;34(3):360-366
DOI 10.5935/0103-507X.20220477-en
Views2ABSTRACT
Objective:
To investigate the applicability of the Respiratory Rate-Oxygenation Index to identify the risk of high-flow nasal cannula failure in post-extubation pneumonia patients.
Methods:
This was a 2-year retrospective observational study conducted in a reference hospital in Bogotá, Colombia. All patients in whom post-extubation high-flow nasal cannula therapy was used as a bridge to extubation were included in the study. The Respiratory Rate-Oxygenation Index was calculated to assess the risk of post-extubation high-flow nasal cannula failure.
Results:
A total of 162 patients were included in the study. Of these, 23.5% developed high-flow nasal cannula failure. The Respiratory Rate-Oxygenation Index was significantly lower in patients who had high-flow nasal cannula failure [median (IQR): 10.0 (7.7 – 14.4) versus 12.6 (10.1 – 15.6); p = 0.006]. Respiratory Rate-Oxygenation Index > 4.88 showed a crude OR of 0.23 (95%CI 0.17 – 0.30) and an adjusted OR of 0.89 (95%CI 0.81 – 0.98) stratified by severity and comorbidity. After logistic regression analysis, the Respiratory Rate-Oxygenation Index had an adjusted OR of 0.90 (95%CI 0.82 – 0.98; p = 0.026). The area under the Receiver Operating Characteristic curve for extubation failure was 0.64 (95%CI 0.53 – 0.75; p = 0.06). The Respiratory Rate-Oxygenation Index did not show differences between patients who survived and those who died during the intensive care unit stay.
Conclusion:
The Respiratory Rate-Oxygenation Index is an accessible tool to identify patients at risk of failing high-flow nasal cannula post-extubation treatment. Prospective studies are needed to broaden the utility in this scenario.
Keywords:Airway extubationCannulaCritical careIntensive care unitsOxygenationPneumoniaRespiratory rateSee more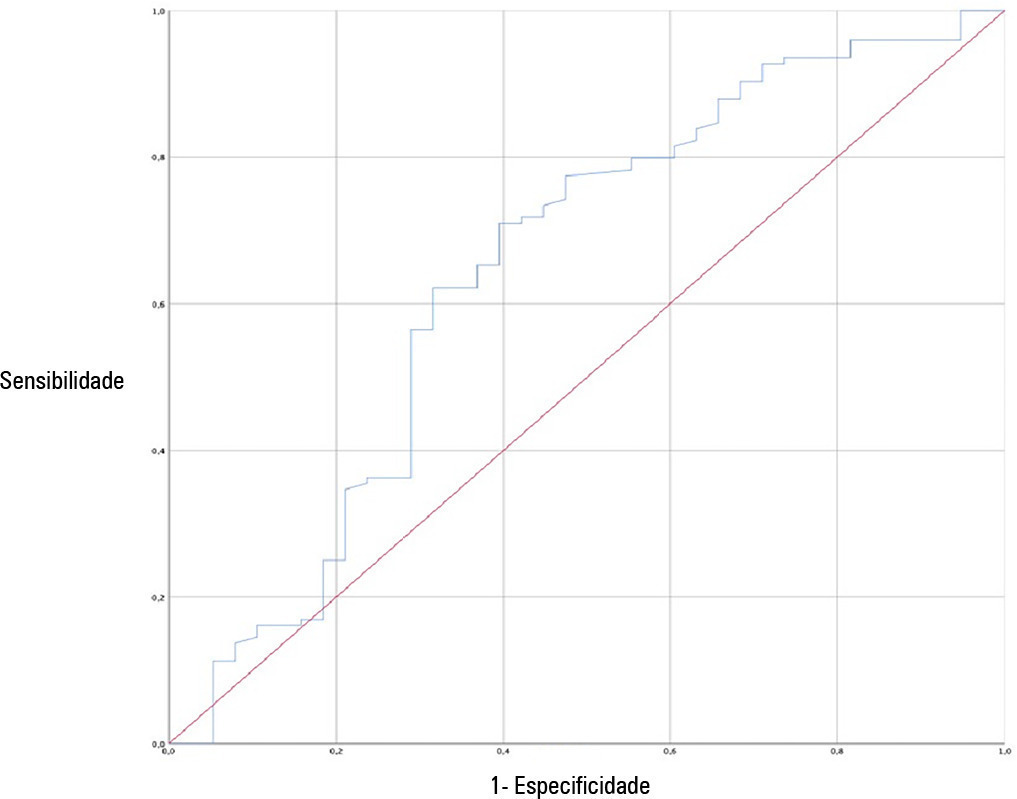
-
Original Article
The prognostic value of peripheral ischemic microvascular reserve in sepsis is not related to calcitonin gene-related peptide or substance P
Rev Bras Ter Intensiva. 2022;34(3):367-373
Abstract
Original ArticleThe prognostic value of peripheral ischemic microvascular reserve in sepsis is not related to calcitonin gene-related peptide or substance P
Rev Bras Ter Intensiva. 2022;34(3):367-373
DOI 10.5935/0103-507X.20220102-en
Views1See moreABSTRACT
Objective:
To evaluate the mechanisms attributed to the prognostic value of peripheral ischemic microvascular reserve in patients with sepsis.
Methods:
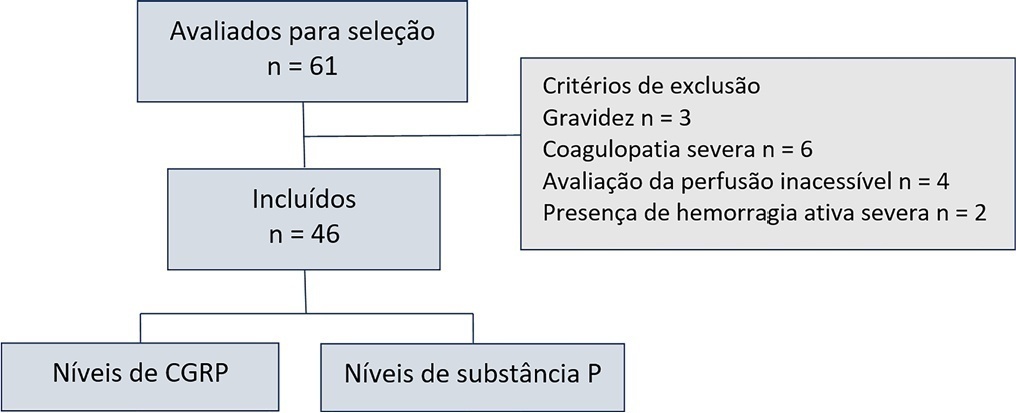
This observational cohort study enrolled 46 consecutive septic patients in the intensive care unit between November 2020 and October 2021. After fluid resuscitation, the peripheral ischemic microvascular reserve was evaluated using the association of postocclusion reactive hyperemia with the peripheral perfusion index. Additionally, peripheral venous blood samples were used to evaluate the neuropeptide calcitonin gene-related peptide and substance P levels in the upper limb before and immediately after postocclusion reactive hyperemia
Results:
There was no statistically significant correlation (p > 0.05) between basal values (pg/mL) or variations from neuropeptide levels (%) and the peripheral ischemic microvascular reserve (%).
Conclusion:
Although calcitonin gene-related peptide and substance P may have a prognostic role in sepsis, these neuropeptides do not appear to contribute to peripheral ischemic microvascular reserve.
-
Original Article
Comparison between the perceptions of family members and health professionals regarding a flexible visitation model in an adult intensive care unit: a cross-sectional study
Rev Bras Ter Intensiva. 2022;34(3):374-379
Abstract
Original ArticleComparison between the perceptions of family members and health professionals regarding a flexible visitation model in an adult intensive care unit: a cross-sectional study
Rev Bras Ter Intensiva. 2022;34(3):374-379
DOI 10.5935/0103-507X.20220114-en
Views3ABSTRACT
Objective:
To compare the perceptions of patients’ relatives with the perceptions of health professionals regarding a flexible visitation model in intensive care units.
Methods:
Cross-sectional study. This study was carried out with patients’ relatives and members of the care team of a clinical-surgical intensive care unit with a flexible visitation model (12 hours/day) from September to December 2018. The evaluation of the flexible visitation policy was carried out through an open visitation instrument composed of 22 questions divided into three domains (evaluation of family stress, provision of information, and interference in the work of the team).
Results:
Ninety-five accompanying relatives and 95 members of the care team were analyzed. The perceptions of relatives regarding the decrease in anxiety and stress with flexible visitation was higher than the perceptions of the team (91.6% versus 58.9%, p < 0.001), and the family also had a more positive perception regarding the provision of information (86.3% versus 64.2%, p < 0.001). The care team believed that the presence of the relative made it difficult to provide care to the patient and caused work interruptions (46.3% versus 6.3%, p < 0.001).
Conclusion:
Family members and staff-intensive care unit teams have different perceptions about flexible visits in the intensive care unit. However, a positive view regarding the perception of decreased anxiety and stress among the family members and greater information and contributions to patient recovery predominates.
Keywords:Critical careFamilyIntensive care units/organization & administrationPatient care teamPerceptionVisitors to patientsSee more -
Original Article
Incidence and risk factors for postintensive care syndrome in a cohort of critically ill patients
Rev Bras Ter Intensiva. 2022;34(3):380-385
Abstract
Original ArticleIncidence and risk factors for postintensive care syndrome in a cohort of critically ill patients
Rev Bras Ter Intensiva. 2022;34(3):380-385
DOI 10.5935/0103-507X.20220224-en
Views3See moreABSTRACT
Objective:
To determine the incidence of postintensive care syndrome in a cohort of critically ill patients admitted to the intensive care unit and to identify risk factors related to its development in the physical, cognitive and mental health areas.
Methods:
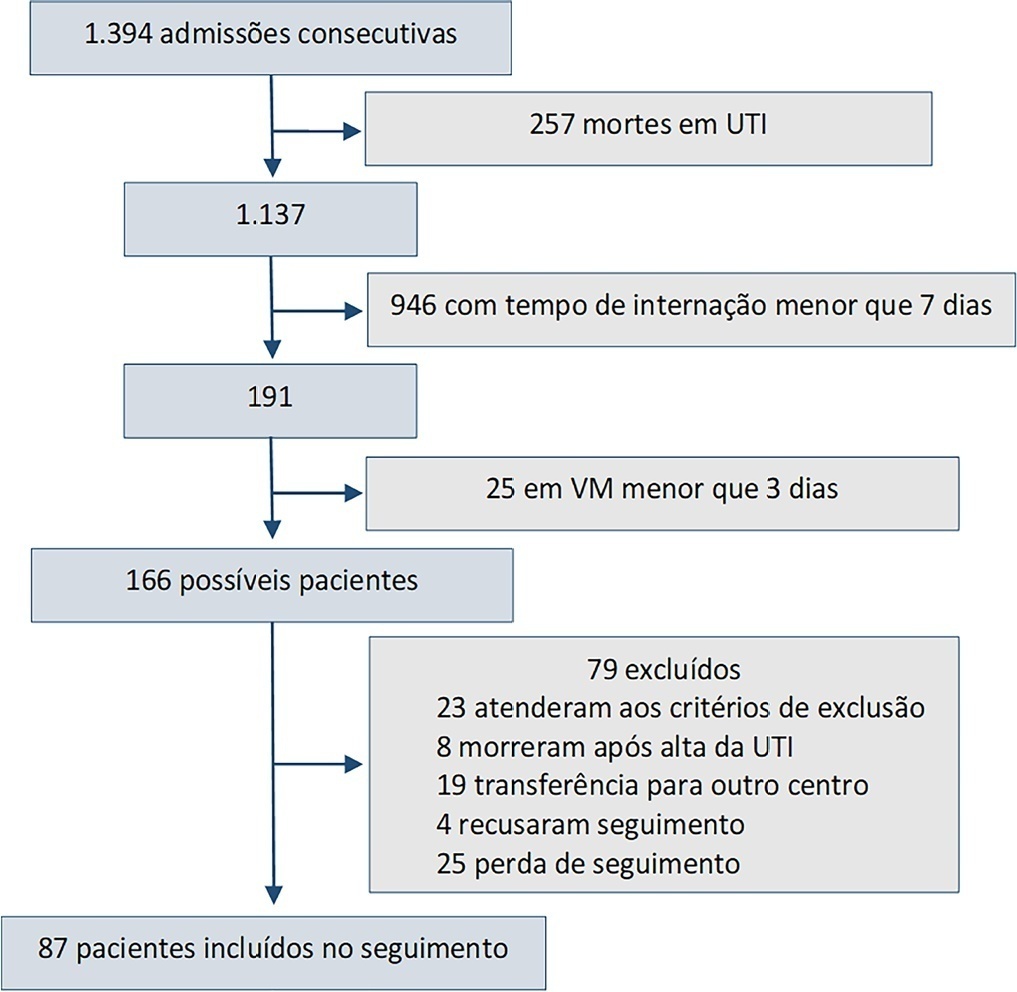
This was a prospective observational cohort study developed in the intensive care unit of a university hospital. Patients with intensive care unit stays equal to or longer than one week and the need for mechanical ventilation for more than 3 days, shock or delirium were included in the study. Demographic variables, reasons for admission, diagnoses, sedation, type of mechanical ventilation used, complications and length of stay were recorded. A univariate analysis was performed to identify risk factors related to postintensive care syndrome. The scales used for the assessment of the different spheres were Barthel, Pfeiffer, Hospital Anxiety and Depression Scale and Impact of Event Scale-6. The main variables of interest were postintensive care syndrome incidence overall and by domains. Risk factors were examined in each of the health domains (physical, cognitive and mental health).
Results:
Eighty-seven patients were included. The mean Acute Physiology and Chronic Health Evaluation II score was 16.5. The mean number of intensive care unit days was 17. The incidence of global postintensive care syndrome was 56.3% (n = 49, 95%CI 45.8 – 66.2%). The incidence of postintensive care syndrome in each of the spheres was 32.1% (physical), 11.5% (cognitive), and 36.6% (mental health).
Conclusions:
The incidence of postintensive care syndrome is 56.3%. The mental health sphere is the most frequently involved. The risk factors are different depending on the area considered.
-
Original Article
Patient safety culture and incidents recorded during nursing shift changes in intensive care units
Rev Bras Ter Intensiva. 2022;34(3):386-392
Abstract
Original ArticlePatient safety culture and incidents recorded during nursing shift changes in intensive care units
Rev Bras Ter Intensiva. 2022;34(3):386-392
DOI 10.5935/0103-507X.20220446-en
Views1ABSTRACT
Objective:
To analyze the association of patient safety culture perceived by nursing professionals with incidents recorded during nursing shifts in intensive care units.
Methods:
This was a cross-sectional study that investigated patient safety culture measured by the Hospital Survey on Patient Safety Culture instrument. Descriptive statistics, chi-square tests, Student’s t-test and multiple linear regression models were analyzed considering a significance level of 5%.
Results:
The study reported a mean of 3.1 (standard deviation of 0.4) for the culture of patient safety in the perception of nursing professionals and 480 incidents with and without damage recorded during the nursing shifts. The variables patient safety culture with a difference between means of 0.543 (95%CI 0.022 – 1.065; p < 0.05) and nursing assistants with a difference between means of -0.133 (95%CI -0.192 - -0.074; p < 0.05) were associated with the incidents recorded during the nursing shifts. Further, nursing assistants had a lower tendency to record incidents than did the nurses.
Conclusion:
The strengthening of the patient safety culture and the aspects tangential to the nursing professionals represent a possible target for interventions to encourage the recording of incidents during the nursing shift shifts and improve patient safety.
Keywords:CommunicationIntensive care unitsNursing assistantsOrganizational culturePatient safetyPerceptionSafety managementSee more -
Letter to the Editor
The hemoglobin level impact on arterial oxygen saturation during venous-venous-extracorporeal membrane oxygenation support of acute respiratory distress syndrome patients: a mathematical marginal approach
Rev Bras Ter Intensiva. 2022;34(3):393-395
Abstract
Letter to the EditorThe hemoglobin level impact on arterial oxygen saturation during venous-venous-extracorporeal membrane oxygenation support of acute respiratory distress syndrome patients: a mathematical marginal approach
Rev Bras Ter Intensiva. 2022;34(3):393-395
DOI 10.5935/0103-507X.20220465-en
Views1TO THE EDITORHemoglobin (Hb) levels in the range of 7 – 14g/dL have been targeted in extracorporeal membrane oxygenation (ECMO)-supported acute respiratory distress syndrome (ARDS) patients. There is an association between low Hb levels and prolonged duration of mechanical ventilation and bleeding episodes. In contrast, higher Hb levels are associated with lower ECMO blood flow, […]See more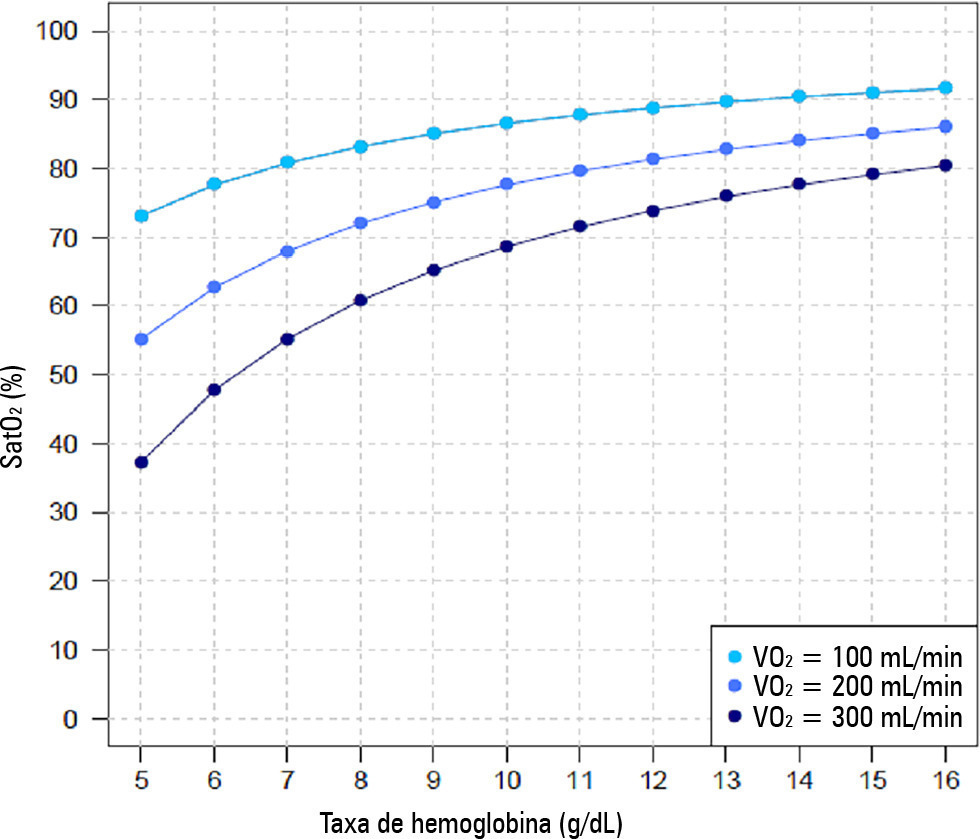
-
Letter to the Editor
To: Epistaxis as a complication of high-flow nasal cannula therapy in adults
Rev Bras Ter Intensiva. 2022;34(3):396-397
Abstract
Letter to the EditorTo: Epistaxis as a complication of high-flow nasal cannula therapy in adults
Rev Bras Ter Intensiva. 2022;34(3):396-397
DOI 10.5935/0103-507X.20220047-en
Views0TO THE EDITORWe have read with great interest this original article by Veiga et al. titled “Epistaxis as a complication of high-flow nasal cannula therapy in adults”.() Although epistaxis is an infrequent complication, it is very interesting as epistaxis has important clinical repercussions. The authors consider that the high flow rate in use (65L/minute) and […]See more -
Erratum
Erratum
Rev Bras Ter Intensiva. 2022;34(3):399-399
Abstract
ErratumErratum
Rev Bras Ter Intensiva. 2022;34(3):399-399
DOI 10.5935/0103-507X.20220020-er-en
Views0In the article Sedation, analgesia, and delirium management in Portugal: a survey and point prevalence study, with DOI number: 10.5935/0103-507X.20220020-en, published in the journal Revista Brasileira de Terapia Intensiva, 34(2):227-36, on page 235, after “Author contributions”:Read:[…]See more




