-
Comentários
Surviving sepsis campaign: um esforço mundial para mudar a trajetória da sepse grave
Rev Bras Ter Intensiva. 2006;18(4):325-327
Abstract
ComentáriosSurviving sepsis campaign: um esforço mundial para mudar a trajetória da sepse grave
Rev Bras Ter Intensiva. 2006;18(4):325-327
-
Comentários
Brás Cubas, sepsis and the evidence: reflections on the surviving sepsis campaign
Rev Bras Ter Intensiva. 2006;18(4):328-330
Abstract
ComentáriosBrás Cubas, sepsis and the evidence: reflections on the surviving sepsis campaign
Rev Bras Ter Intensiva. 2006;18(4):328-330
-
Artigos originais
Nutrition support in an intensive care unit: delivery versus requirements
Rev Bras Ter Intensiva. 2006;18(4):331-337
Abstract
Artigos originaisNutrition support in an intensive care unit: delivery versus requirements
Rev Bras Ter Intensiva. 2006;18(4):331-337
DOI 10.1590/S0103-507X2006000400003
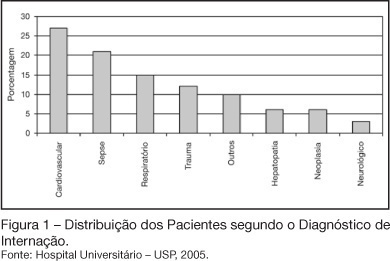
Views0See moreBACKGROUND AND OBJECTIVES: In critically ill patients nutritional deficiency is common. Considering this fact, the diary monitoring of energy delivered is extremely important. The objective of this study is to assess the adequacy of enteral nutrition (EN) in an Intensive Care Unit (ICU) and identify the reasons for interruptions in feeding. METHODS: Prospective study of adult patients admitted to ICU in period of 53 days. Patients receiving continuous enteral tube feeding (22 hours/day) exclusively and post-pyloric tube feeding position were followed. The feeding volume started at 25 mL/h and was increased until nutritional goal, guided by a feeding protocol. RESULTS: 33 patients between 18 and 85 years old were studied. 58% were male. The main admission diagnoses were cardiovascular diseases (27%) and septic shock (21%). The mean time to feeding was 25.3 hours after the patient admission and nutritional goal was achieved in a mean time of 32 hours. The total volume prescribed per day was sufficient to guarantee a mean of 26.1 kcal/kg of body weight and 1.04 g of protein/kg of body weight. Patients received a mean of 19.5 kcal/kg of body weight and 0.8 g of protein/kg of body weight, which correspond a 74% of adequacy. Interruptions of feeding for routine procedures related to patients accounted for 40.6% of the total reasons. CONCLUSIONS: The nutritional support is adequate considering the literature for these patients, who clinical instability causes gastrointestinal intolerance. The effective participation of the Nutrition Therapy Team can contribute positively on nutritional therapy.
-
Artigos originais
Noninvasive positive pressure ventilation in patients with acute respiratory failure after tracheal extubation
Rev Bras Ter Intensiva. 2006;18(4):338-343
Abstract
Artigos originaisNoninvasive positive pressure ventilation in patients with acute respiratory failure after tracheal extubation
Rev Bras Ter Intensiva. 2006;18(4):338-343
DOI 10.1590/S0103-507X2006000400004
Views0See moreBACKGROUND AND OBJECTIVES: Noninvasive positive pressure ventilation (NPPV) has been routinely used to assist the weaning of the mechanical ventilation. One of the applications most common is in patients who had acute respiratory failure after extubation, even the scientific evidences for this indication still controversy. The aims of this study were to evaluate the index of patients that evolve for respiratory failure after extubation and evaluated the effectiveness of NPPV to avoid the need for reintubation and to promote increase in success index of weaning. METHODS: We conducted a transversal and prospective study. It was applied to NPPV in the patients who presented respiratory failure after extubation, independent of its etiology. NPPV was applied in to pressure support ventilation, with Vte for 6 to 8 mL/kg, PEEP and FiO2 adjusted to reach SaO2 > 95%. The NPPV was accomplished of a continuous mould even interrupt the signs of respiratory failure presented initially. The success of weaning and the NPPV was defined when the clinical events were reverted by a period greater than 48 hours in spontaneous breathing, avoid thus reintubation. RESULTS: We included 103 patients. Noted that 32% (33) evolved with signals of respiratory failure after extubation and were submitted to NPPV. The time of NPPV was on mean 8 ± 5 hours, PSV of 12 ± 2 cmH2O, PEEP of 7 ± 2 cmH2O, FiO2 of 40% ± 20%, Vte of 462 ± 100 mL, RR of 26 ± 5 rpm. Among patients who accomplished NPPV (33), 76% (25) attended with success and them afterwards let the ICU. Of the patients assigned to NPPV, 24% (8) did not tolerate the procedure and were reintubated. CONCLUSIONS: We conclude that NPPV is safe and effective in averting the need for reintubation in patients with respiratory failure after extubation.
-
Artigos originais
Ventilator associated pneumonia: confection of a strategy of prophylaxis and management based on the analysis of epidemiology
Rev Bras Ter Intensiva. 2006;18(4):344-350
Abstract
Artigos originaisVentilator associated pneumonia: confection of a strategy of prophylaxis and management based on the analysis of epidemiology
Rev Bras Ter Intensiva. 2006;18(4):344-350
DOI 10.1590/S0103-507X2006000400005
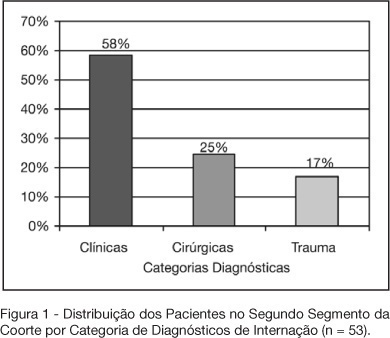
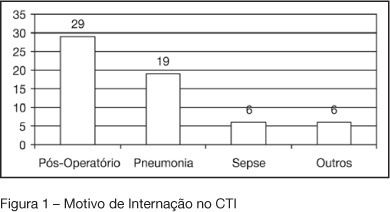
Views0See moreBACKGROUND AND OBJECTIVES: Variable magnitude of impact on the outcomes of the critically ill patients has been credited to ventilation-associated pneumonia, in terms of mortality, length of hospital stay and mechanic ventilation days. Three objectives have been defined in this study: mortality and incidence of ventilation-associated pneumonia before and after the implantation of a prophylaxis protocol (primary objectives); microbiologic mapping (secondary objective) as an instrument to optimize therapy. METHODS: A historical cohort was followed during the period of August 2001 to January 2004, fragmented in two segments, pre (until January 2003, n = 52) and post-implantation of the mentioned protocol, the analysis of mortality and microbiologic mapping been performed in the second segment (control group n = 39 and case group n = 14). RESULTS: The incidence rates from 2001 to 2003 were respectively 28.05‰ ± 12.92‰, 22.45‰ ± 10.18‰ and 10.75‰ ± 7.61‰. The decrease in this rate after the intervention did not reach statistical significance (p > 0.4). Mortality rates were 49% in the control group (CI 95 = 33% to 65%) and 43% in the case group (CI 95 = 14% to 72%), OR = 0.88 (CI 95 = 0.26 to 2.94), without statistical significance either (p = 0.65). Eight bronco-alveolar lavage were obtained (57%), 50% with multiple flora. Pseudomonas aeruginosa was isolated in six patients (75%), Acinetobacter sp in one case (12.5 %) and methicilin-resistent Staphylococcus aureus (MRSA) in one (12.5%). Other Gram negative bacilli producers of extended spectrum betalactamase (ESBL) were isolated in two cases (25%) and Stenotrophomonas maltophilia in another (12.5%). CONCLUSIONS: The incidence rate of ventilation-associated pneumonia revealed a tendency to considerable reduction after the utilization of the prophylaxis protocol, while the results suggest no impact on mortality rates. Further prospective evaluation of a greater sample is required, in order to get to definite conclusions regarding prognosis. The isolated germs were, in its majority, high risk pathogens to multiresistance to antibiotics, pointing the necessity of knowledge of local susceptibility profile, so that an adequate initial therapeutic strategy can be undertaken.
-
Artigos originais
Assessment of success in weaning from mechanical ventilation
Rev Bras Ter Intensiva. 2006;18(4):351-359
Abstract
Artigos originaisAssessment of success in weaning from mechanical ventilation
Rev Bras Ter Intensiva. 2006;18(4):351-359
DOI 10.1590/S0103-507X2006000400006
Views0See moreBACKGROUND AND OBJECTIVES: The weaning of patients under mechanical ventilation (MV) is one of the critical stages of respiratory assistance in intensive care. There are several criteria for taking patients out of respiratory prothesis. The aim of this work was to assess if there is a group of parameter which can predict the patients who will succeed in weaning from mechanical ventilation. METHODS: Sixty patients were studied in a prospective way within 24 months. All of them had been in MV for, time > 48 hours. The specific mechanical parameters were monitored for the weaning, clinical data, gasometrical values and laboratory results. The patients were divided into both succeeding and unsucceeding groups for comparable analysis. By the ROC curve, it was observed the best cut point for the numerical variables evaluated for the success of the weaning. RESULTS: In analysis of logistic regression performed to evaluate the simultaneous influence of all the factors: MV < 8 days, APACHE II (Acute Physiologic and Chronic Health Evaluation II) < 16 and Pimax (maximum respiratory pression) > (-) 20 cmH2O were statistically significant to predict the success to weaning, in this order of explainable capacity. CONCLUSIONS: We could conclude that the indexes evaluated were suitable for the determination of the success in the weaning of those patients in mechanical ventilation. APACHE II because of admition constitutes severity indicator and allows awareness from the patient. MV timing, optimizing the treatment in order to accelerate the process of weaning is conducts that aim not only for the weaning success but also interfere both in the evolution and period of hospital admition.
-
Artigos originais
Hyperlactatemia at ICU admission is a morbid-mortality determinant in high risk non-cardiac surgeries
Rev Bras Ter Intensiva. 2006;18(4):360-365
Abstract
Artigos originaisHyperlactatemia at ICU admission is a morbid-mortality determinant in high risk non-cardiac surgeries
Rev Bras Ter Intensiva. 2006;18(4):360-365
DOI 10.1590/S0103-507X2006000400007
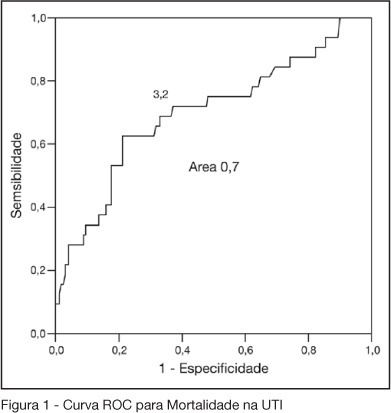
Views0See moreBACKGROUND AND OBJECTIVES: One of the greatest challenges found by the intensivists in their daily activities is tissue hipoperfusion control. Blood lactate is generally accepted as a marker of tissular hypoxia and several studies have demonstrated good correlation between blood lactate and prognosis during shock and resuscitation. The aim of this study was to evaluate the clinical utility of arterial blood lactate as a marker of morbidity and mortality in critically ill patients in the post-operative period of high risk non-cardiac surgeries. METHODS: Prospective and observational cohort study realized in an ICU of a tertiary hospital during a four month period. Demographic data of the patients submitted to high risk surgeries were collected, besides arterial lactate measures and number and type of complications in the post-operative period. To the statistic analysis was considered as significant a p < 0.05. The predictive ability of the indexes to differentiate survivors from non-survivors was tested using ROC curves. Lenght of ICU stay estimation where calculated by Kaplan Meier method. RESULTS: Were included 202 patients. 50.2% were female and their mean age was 66.5 ± 13.6 years. APACHE II score was 17.4 ± 3.0 and the median of MODS score was 4 (2-6). Median lenght of surgeries was 4h (3-6h). 70.7% of the surgeries were elective ones. ICU and hospital mortality were 15.6% and 33.7%, respectively. The best lactate value to discriminate mortality was 3.2 mmol/L, with sensitivity of 62.5%, specificity of 78.8% and an area under the curve of 0.7. 62.5% of patients with lactate > 3.2 did not survive versus 21.2% of survivors (OR = 2.95 IC95% 1.98- 4.38, p < 0.0001). ICU lenght of stay was greater when > 3.2 mmol/L (log rank 0.007) lactate. CONCLUSIONS: High risk patients submitted to non cardiac surgeries and admitted to the ICU with hiperlactatemia, defined as an arterial lactate > 3.2 mmol/L, are prone to a longer ICU lenght of stay and to die.
-
Artigos originais
Assessment of the diagnostic and treatment in cardiac arrest between doctors with five years after graduation
Rev Bras Ter Intensiva. 2006;18(4):374-379
Abstract
Artigos originaisAssessment of the diagnostic and treatment in cardiac arrest between doctors with five years after graduation
Rev Bras Ter Intensiva. 2006;18(4):374-379
DOI 10.1590/S0103-507X2006000400009
Views0See moreBACKGROUND AND OBJECTIVES: New resuscitation guidelines contain significant changes intended to improve resuscitation practice and survival from cardiac arrest. The objective of this study was to evaluate the theoretical knowledge about cardiac arrest (CA) and cardiac and pulmonary resuscitation (CPR) among doctors after five years of the graduation. METHODS: The questionnaire survey was conducted in an Emergency Hospital in the State of Alagoas. The population was composed of doctors with five years after your graduation. The data was collected with a questionnaire with questions about the theme. The results were analyzed based on bibliographies about CA and CPR. RESULTS: Thirty-nine professionals answered the questionnaire. The CA diagnostic was correct in 76.9% and increased to 82.7 when the case report was included. Questions about sodium bicarbonate and vasopressin were correctly answered by 30.8% and 15.4% of the participants. CONCLUSIONS: The greatest difficulty reported in this study was on the CA arrest Most of the participants of the survey are not aware of the correct indications of vasopressin and sodium bicarbonate in the CPR. According to this study, a continuing medical education program on CPR for physicians with more than five years of graduations warranted.
-
Artigos originais
Laboratory exams necessity for patients admitted to an university hospital intensive care unity
Rev Bras Ter Intensiva. 2006;18(4):385-389
Abstract
Artigos originaisLaboratory exams necessity for patients admitted to an university hospital intensive care unity
Rev Bras Ter Intensiva. 2006;18(4):385-389
DOI 10.1590/S0103-507X2006000400011
Views0See moreBACKGROUND AND OBJECTIVES: The progressive increasing diagnostic resources had influenced the quality and quantity of laboratory exams. It is not clear if the amount of exams performed influence the morbidity and mortality in the ICU patients. The purpose of this study was to appraise the frequency of the most ordering tests in the ICU of HU-UFSC and to check if there was connection between them and the age, the destiny until the ICU discharge and the estimate severity of their diseases. METHODS: Prospective cohort study with qualitative approach. The blood samples of admitted patients were analyzed, from July to December 2005. Clinical and demographic features were collected and the most frequently blood-samples were quantified per day. In the sequence the daily rate of exams were calculated during all the admission period. The patients were analyzed according to three criterions: age, destiny until the ICU discharge and estimate severity according to APACHE II index. Data were analyzed using Fisher Exact, Chi-square and ANOVA tests. RESULTS: One hundred and thirteen patients were enrolled to this study. The average test-ordering was 11.50 per day. These numbers didn’t have statistical difference when they were compared between survivor and non-survivor patients, and between those whose the death estimated tax was bigger or smaller than 50 per cent. CONCLUSIONS: The test-ordering didn’t show clinical and prognostic relation to its request. There were no statistic relation between the patient’s age, ICU discharge and the estimate severity.
-
Artigo Original de Pediatria
Red blood cell transfusion in children admitted in a pediatric intensive care unit
Rev Bras Ter Intensiva. 2006;18(4):390-395
Abstract
Artigo Original de PediatriaRed blood cell transfusion in children admitted in a pediatric intensive care unit
Rev Bras Ter Intensiva. 2006;18(4):390-395
DOI 10.1590/S0103-507X2006000400012
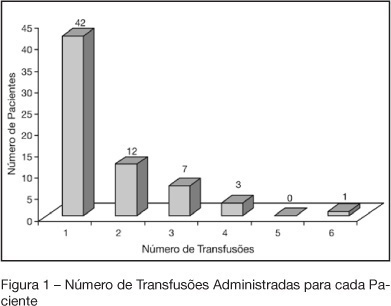
Views0See moreBACKGROUND AND OBJECTIVES: Indications of red blood cell transfusion in critically ill children are not very well determined. This study aims to describe red blood cells transfusion practice at the PICU of UNESP-Botucatu Medical School. METHODS: Retrospective observational study of all patients who received transfusion during 2003. RESULTS: Seventy five patients received transfusion and 105 indications were recorded. 53.3% of the patients were less than one year of age. Increased respiratory rate (75.2%), paleness (65.7%), and hypotension (51.4%) were the alterations more frequently recorded, before transfusion. Also, metabolic acidosis (68.08%) e and hipoxemia (63.8%) were very frequently observed. From 93 hemoglobin (Hb) values recorded, 54 (58.1%) varied from 7 to 10 g/dL and from 90 records of hematocrit (Ht) 66 (73.3%) varied from 21% to 30%. The main indications of the transfusion were anemia, in 75 children (71.4%), and active bleeding in 26 (24.7%). The mean value of Hb before transfusion was 7.82 ± 2.82 g/dL. Seven transfusions were indicated for patients with Hb levels higher than 10 g/dL (postoperative heart surgery and septic patients). CONCLUSIONS: red blood cells transfusion is carefully prescribed at the PICU by using restrictive indications (Hb between 7 and 10 g/dL). Not always is possible to find out records of the Hb levels immediately before transfusion. Hence, a protocol to better prescribe red blood cell transfusion at the PICU was adopted.
-
Artigos de Revisão
Serum neuron-specific enolase as a prognostic marker after a cardiac arrest
Rev Bras Ter Intensiva. 2006;18(4):396-401
Abstract
Artigos de RevisãoSerum neuron-specific enolase as a prognostic marker after a cardiac arrest
Rev Bras Ter Intensiva. 2006;18(4):396-401
DOI 10.1590/S0103-507X2006000400013
Views0See moreBACKGROUND AND OBJECTIVES: Cardiac arrest is a state of severe cerebral perfusion deficit. Patients recovering from a cardiopulmonary resuscitation are at great risk of subsequent death or incapacitating neurologic injury, including persistent vegetative state. The early definition of prognosis for these patients has ethical and economic implications. The main purpose of this manuscript was to review the prognostic value of serum Neuron-Specific Enolase (NSE) in predicting outcomes in patients early after a cardiac arrest. CONTENTS: Severe neurologic disability is the most feared complication after a cardiac arrest. Many studies are trying to find prognostic markers that can be associated with outcomes in patients surviving a cardiac arrest. Biochemical markers of neuronal injury seem to be promising in this scenario. Therefore, NSE levels have been studied in patients after a cardiac arrest and high enzyme levels suggest more extensive brain damage and are associated with unfavorable clinical outcomes. CONCLUSIONS: Outcome after a cardiac arrest is mostly determined by the degree of hypoxic brain damage and early determinations of serum NSE level can be a valuable ancillary method for assessing outcome in these patients.
-
Artigos de Revisão
Statins on sepsis: a new therapeutic gun in intensive care medicine?
Rev Bras Ter Intensiva. 2006;18(4):402-406
Abstract
Artigos de RevisãoStatins on sepsis: a new therapeutic gun in intensive care medicine?
Rev Bras Ter Intensiva. 2006;18(4):402-406
DOI 10.1590/S0103-507X2006000400014
Views0See moreBACKGROUND AND OBJECTIVES: Sepsis is a syndrome with an important inflammatory component in its pathophysiology. Some drugs that act on the activation of inflammatory cascade have been tested in septic patients. Statins, beyond hypolipemic effects, have anti-inflammatory capacities, known as pleiotropic effects. That action may be of value on sepsis treatment. Review of publications who discuss the use of statins. This article has the objective to review the mainly papers about statins and sepses. METHODS: Original published articles were searched using Medline database crossing the keys words “sepsis and statins” between 1990 and 2006 RESULTS: Experimental and retrospective studies has been investigated the use of statins in septic patients, until this moment, most of then show benefits on morbidity and mortality. However, there is not prospective, randomized, placebo controlled trials. Or metanalyses, witch denotes lack strong and robust that could be indicated this action. So, since the benefit is still unable, it is necessary randomized clinical trials witch can prove this theory. CONCLUSIONS: Several experimental and retrospective studies have investigated the use of statins in septic patients, but despite literature demonstrating a promising role for its use in these patients, these studies are experimental or retrospective. Therefore, we must wait larger, prospective, randomized trials before we may be able to understand its role and possibly recommend these drugs in the treatment of septic patients.
-
Artigo de Revisão de Pediatria
Inhaled nitric oxide for children with acute respiratory distress syndrome
Rev Bras Ter Intensiva. 2006;18(4):407-411
Abstract
Artigo de Revisão de PediatriaInhaled nitric oxide for children with acute respiratory distress syndrome
Rev Bras Ter Intensiva. 2006;18(4):407-411
DOI 10.1590/S0103-507X2006000400015
Views0See moreBACKGROUND AND OBJECTIVE: The objective of this study was to review the literature on inhaled nitric oxide to children with acute respiratory distress syndrome. CONTENTS: A review of literature and selection of the most important publications on inhaled nitric oxide, using the MedLine and Cochrane Systematic Review Databases. This review was organized as follows: introduction; metabolism and biological effects; clinical applications; dosage, gas administration and weaning process; warnings and side-effects. Inhaled nitric oxide use was described in acute respiratory distress syndrome. CONCLUSIONS: Inhaled nitric oxide as the first vasodilator to produce selective pulmonary vasodilation has beneficial effects on gas exchange and ventilation, improving outcome in children with severe hypoxia. It is safe when administered in intensive care units under strict surveillance and monitoring. Further studies should be concentrated on early treatment, when acute respiratory distress syndrome is potentially reversible.
-
Artigos de Revisão
Importance of dental work in patients under intensive care unit
Rev Bras Ter Intensiva. 2006;18(4):412-417
Abstract
Artigos de RevisãoImportance of dental work in patients under intensive care unit
Rev Bras Ter Intensiva. 2006;18(4):412-417
DOI 10.1590/S0103-507X2006000400016
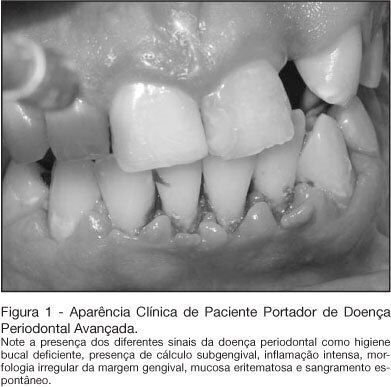
Views0See moreBACKGROUND AND OBJECTIVES: In the intensive care unit, the nosocomial respiratory infection is responsible for high rates of morbidity, mortality and expressive increase in hospitals costs. Its establishment feels more commonly by the aspiration of the content present within the mouth and the pharynx. Thus we intended to review the literature on the participation of the oral condition in the establishment of the nosocomial respiratory infection. CONTENTS: Deficient oral hygiene is common in patients under intensive care, which provides the colonization of oral biofilm for pathogenic microorganisms, especially for respiratory pathogens. The studies clearly show that the amount of oral biofilm in patients under intensive care increases according to period hospitalization meanwhile there also is an increase in respiratory pathogens. That colonizes the oral biofilm. This biofilm is an important resource of pathogens in patients under intensive care. CONCLUSIONS: In spite of well-established hypotheses that narrow down the relationships between lung infections and the oral condition, the studies are not still completely defined. However, due to strong possibilities that these hypotheses are true, it is necessary to have and maintain the oral health, in addition to more integration of dentistry and of Medicine, seeking patients’ global treatment, the prevention of diseases, and more humanization at the intensive care unit.
-
Relatos de Caso
Activated C protein in the treatment of a newborn with sepsis, shock and multiple organ dysfunction systems: case report and literature review
Rev Bras Ter Intensiva. 2006;18(4):418-422
Abstract
Relatos de CasoActivated C protein in the treatment of a newborn with sepsis, shock and multiple organ dysfunction systems: case report and literature review
Rev Bras Ter Intensiva. 2006;18(4):418-422
DOI 10.1590/S0103-507X2006000400017
Views0See moreBACKGROUND AND OBJECTIVES: Severe sepsis represents the systemic inflammatory response resulting from an infection, associated with one of the following: cardiovascular organ dysfunction, acute respiratory distress syndrome or two or more organ dysfunctions. Although the mortality rate from sepsis in children has steadily decreased in the last decades, the mortality rate in newborns remains high (20% to 40%) despite the development in intensive care. The authors describe a newborn who suffered from sepsis, shock and multiple organ dysfunction syndromes (MODS) that recovered after the administration of activated C protein. CASE REPORT: A premature newborn underwent cesarean section because of a premature rupture of membranes and acute fetal distress. The newborn developed acute respiratory distress due to intrauterine pneumonia and was taken to the Neonatal Intensive Care Unit. The patient was given mechanical ventilation, exogenous pulmonary surfactant and antibiotics early in the treatment. Nevertheless, he developed persistent pulmonary hypertension and shock. The control of the infection was difficult, despite the adjustment of the antibiotics, resulting in the development of MODS. On the 28th day, activated C protein was given to the patient. The administration of the drug was successful and the patient recovered from the organ dysfunction without bleeding. CONCLUSIONS: The activated C protein can’t be recommended as a routine in the treatment of newborns with severe sepsis. However, in this case, it contributed to the recovery of the organ dysfunctions presented by the patient.
-
Relatos de Caso
Adverse systemic reactions in intensive care medicine after isolated limb perfusion with melphalan and hyperthermia: case report
Rev Bras Ter Intensiva. 2006;18(4):423-426
Abstract
Relatos de CasoAdverse systemic reactions in intensive care medicine after isolated limb perfusion with melphalan and hyperthermia: case report
Rev Bras Ter Intensiva. 2006;18(4):423-426
DOI 10.1590/S0103-507X2006000400018
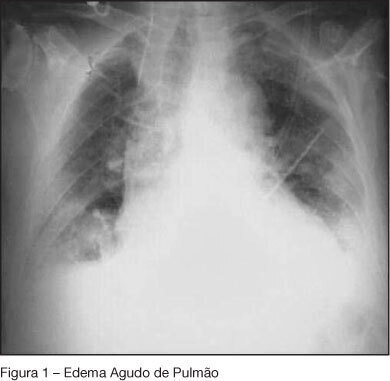
Views0See moreBACKGROUND AND OBJECTIVES: The presence of adverse reactions, inherent to all treatments, justifies the necessity of deep knowledge, by the medical team of the prevention and treatment of occasional organic dysfunctions, reducing its impact. The purpose of this paper is to report a case comprising the several systemic adverse reactions after perfusion of limb with melphalan and hyperthermia. CASE REPORT: A white female, 64-years old patient with diagnosis of melanoma in the medial malleoli region of the left lower limb. Six months after surgical removal of wound, an isolated perfusion of limb was carried out with melphalan and hyperthermia in order to curb the possible metastatic process in evolution. At admission in the ICU, the patient presented systemic inflammatory response syndrome (SIRS) with refractary hemodynamic instability to volemic expansion. During internation the patient evolved to acute lung edema and myocardial dysfunction, all reverted successfully. CONCLUSIONS: The potential presence of adverse reactions, inherent to all treatments, justify the necessity of knowledge by the intensive care team in the prevention and treatment of occasional organic dysfunctions, reducing the impact of morbidity and mortality.
-
Relatos de Caso
Cardiovascular complications related to cocaine use: case report
Rev Bras Ter Intensiva. 2006;18(4):427-432
Abstract
Relatos de CasoCardiovascular complications related to cocaine use: case report
Rev Bras Ter Intensiva. 2006;18(4):427-432
DOI 10.1590/S0103-507X2006000400019
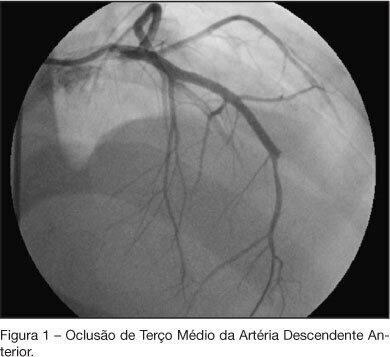
Views0See moreBACKGROUND AND OBJECTIVES: Cocaine is the most commonly used illicit drug and its acute and chronic effects are related to a variety of physiological changes, mainly in the cardiovascular system. This study is a case report of a patient with cardiomyopathy related to cocaine use. CASE REPORT: A 19 year old men, who has been using cocaine and crack since 15 years old, was admitted to the emergency department (ED) in February 2006 with progressive dyspnea during minimal efforts and bloody expectoration. During the physical exam it was observed legs edema, jugular stasis and dyspnea at rest. The echocardiogram demonstrated left ventricular hypocinesia, a 17 mm ventricular thrombus and a 12% ejection fraction. A bleeding from the left upper lobe was identified during a pulmonary bronchoscopy which was treated with arterial embolization. After 48h of the procedure, the patient was asymptomatic and an antithrombotic treatment with warfarin and enoxaparin was started. No obstruction was found at the cineangiography and the patient was discharged after clinical improvement. The patient was admitted again to the intensive care unit in July with intense chest pain and dyspnea at rest. A new cineangiography was performed and it was observed occlusion in the anterior descendent coronary artery. CONCLUSIONS: The cocaine acute effects are commonly seen at the ED but the chronic effects, as the cardiovascular manifestations, can take longer to be correlated as a side effect of cocaine use. Its prolonged use is related to left ventricular systolic dysfunction due to hypertrophy or myocardial dilation, atherosclerosis, arrhythmias, myocyte apoptosis and sympathetic damage.