-
Artigos originais
Low-doses dobutamine and fluids in high-risk surgical patients: effects on tissue oxygenation, inflammatory response and morbidity
Rev Bras Ter Intensiva. 2007;19(1):5-13
Abstract
Artigos originaisLow-doses dobutamine and fluids in high-risk surgical patients: effects on tissue oxygenation, inflammatory response and morbidity
Rev Bras Ter Intensiva. 2007;19(1):5-13
DOI 10.1590/S0103-507X2007000100001
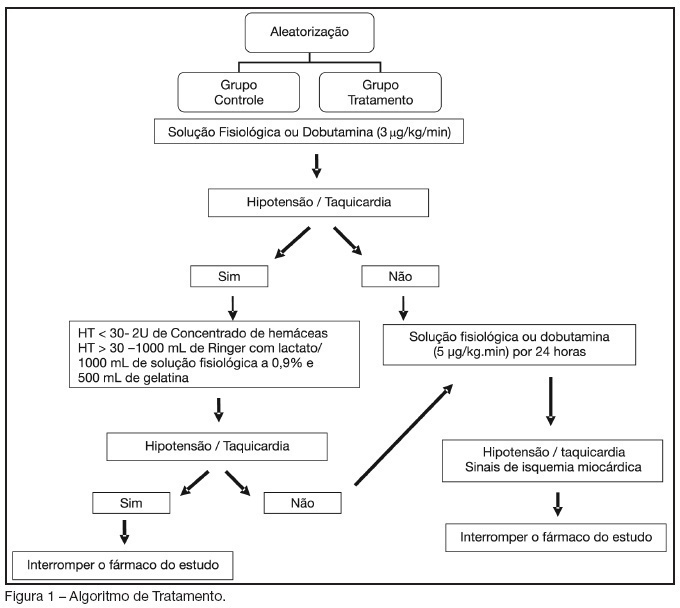
Views0See moreBACKGROUND AND OBJECTIVES: Dobutamine is an inotropic agent with predominant beta1- adrenergic properties frequently used to increase blood flow in critically ill patients. Dobutamine may have a role in increasing splanchnic perfusion, thereby protecting this area from further injury. We investigated the effects of low doses dobutamine (5 mug/kg/min) on tissue oxygenation, inflammatory response and postoperative complications in high-risk surgical patients. METHODS: Prospective, randomized, blinded and placebo-controlled study. One hundred surgical patients admitted in a step-down unit were evaluated and 82 patients were enrolled, 42 in the control group (saline) and 40 in the treatment group (5 mug/kg/h) during 24 hours. Similar therapeutic goals were applied to both groups. Fluids were given whenever tachycardia or hypotension developed after study drug infusion. RESULTS: The total volume of fluids given was significantly higher in treatment than in control group (7351 ± 2082 mL versus 6074 ± 2386 mL, respectively, p < 0.05). Central venous oxygen saturation (ScvO2), serum lactate and C-reactive protein were similar in both groups. Complications occurred in 35% and 50% of the patients in the treatment and control groups, respectively (RR 0, 70 IC 95% 0.41 - 1.17; NS). CONCLUSIONS: Low-doses dobutamine and fluids after surgical trauma has no effects on the prevalence of postoperative complications in high-risk surgical patients.
-
Artigos originais
Proteomics and sepsis: new perspectives for diagnosis
Rev Bras Ter Intensiva. 2007;19(1):14-22
Abstract
Artigos originaisProteomics and sepsis: new perspectives for diagnosis
Rev Bras Ter Intensiva. 2007;19(1):14-22
DOI 10.1590/S0103-507X2007000100002
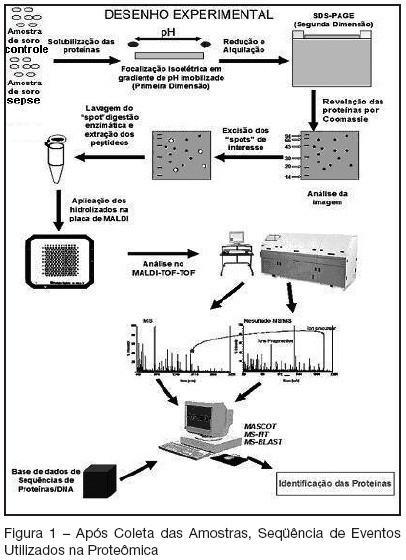
Views0See moreBACKGROUND AND OBJECTIVES: The diagnostic and treatment of sepsis continue to challenger all, and, more specific forms to approach are absolutely necessary. The objective of this study was to use proteomics techniques, two-dimensional electrophoresis and mass spectrometry, to verify the differential protein expression between serum of patients with sepsis and health controls. METHODS: Samples of serum the 30 patients with sepsis, caused for different types of microorganisms and serum of 30 health controls were obtained for analysis. Next, were submitted to 2D-SDS-PAGE, gels compared, selection of spots for excision and digestion with trypsin, being the peptides analyzed for MALDI TOF-TOF. The obtained spectrums were processed (Mascot-matrix science) for protein identification in NCBInr Data Bank. RESULTS: Image analyses showed several spots with differential expressions in the gels of the patients with sepsis in relation to the controls. The protein identification of some of these spots founded: Orosomucoid 1 precursor, Apolipoprotein A-IV, Apolipoprotein A-IV precursor, Haptoglobin protein precursor, Haptoglobin, Zinc finger protein, Serum amyloid A-1, Transthyretin, Nebulin, Complement C4, Alpha1-Antitrypsin, Unnamed protein product and others. CONCLUSIONS: Serum of the patients with different types of sepsis express characteristic protein profiles by 2D-SDS-PAGE compared with controls. The most expressed were from acute phase proteins and lipoproteins. It is possible in the future, with proteomics, create diagnostic panel of proteins, finding news biomarkers and targets for therapeutic interventions in sepsis. This is a first description, with proteomics, of the alterations in protein expression, in serum of the patients with sepsis.
-
Artigos originais
Risk factors associated to mortality on septic patients in an intensive care unit of a general private hospital from Pernambuco
Rev Bras Ter Intensiva. 2007;19(1):23-30
Abstract
Artigos originaisRisk factors associated to mortality on septic patients in an intensive care unit of a general private hospital from Pernambuco
Rev Bras Ter Intensiva. 2007;19(1):23-30
DOI 10.1590/S0103-507X2007000100003
Views0See moreBACKGROUND AND OBJECTIVES: Verify the association between clinical, epidemiological and laboratorial characteristics with mortality of septic patient in an Intensive Care Unit (ICU) from Pernambuco, northeast of Brazil, to improve the attention for patients with sepse which are in risk of developing organ dysfunction. METHODS: Case-control study, without intervention, that included adults’ patients admitted in ICU with sepsis or that developed it during ICU stay. RESULTS: It was included 199 patients. After logistic regression, the length of hospital stay more than 72 hours before admission in ICU, evidence of associated co-morbidities, more than three organ failures, and lactate more than 4 mmol/L were associated with mortality. The SOFA score with more than 12 points was associated with precocity mortality (< 72hours). CONCLUSIONS: The septic patients admitted ICU with less than 72h of hospital stay have a better prognosis, and those with a great number of organ failure, and co-morbidities have a superior mortality rate. Between laboratory results, only the high concentration of lactate is associated with mortality.
-
Artigos originais
Implementation, assessment and comparison of the T-Tube and pressure-support weaning protocols applied to the intensive care unit patients who had received mechanical ventilation for more than 48 hours
Rev Bras Ter Intensiva. 2007;19(1):31-37
Abstract
Artigos originaisImplementation, assessment and comparison of the T-Tube and pressure-support weaning protocols applied to the intensive care unit patients who had received mechanical ventilation for more than 48 hours
Rev Bras Ter Intensiva. 2007;19(1):31-37
DOI 10.1590/S0103-507X2007000100004
Views0BACKGROUND AND OBJECTIVES: Mechanical ventilation incurs significant morbidity and mortality, weaning intensive care unit patients is highly desirable, although it is usuallyconducted in an empirical manner. Thus, this article assessed a weaning protocol implementation and compared two different methods. METHODS: It was carried out a study involving 120 patients who had received mechanical ventilation for more than 48 hours. These patients were randomlyassigned to undergo one of two weaning techniques: pressure-supportventilation + PEEP (PSP) technique, which was applied to the patients in equal days, forming the PSP group (PSPG) and the T-tube method (TT), applied in odd days and forming the TT group (TTG). Standardized protocols were followedfor each technique RESULTS: The patients response to extubation revealed similar progress in both PSP and TT groups, but after the Chi-square statistical test, the benefits of using a weaning protocol was clear. One hundred nine (90.83%) of all patients, had a successful weaning and any noninvasive ventilation type was needed in a span time of 24 hours after extubation, and only eleven (9.17%), had an unsuccessful weaning. CONCLUSIONS: Although this study didn’t show any difference between the two methods applied, we could conclude that, the implementation of standardized weaning protocols can substantially decrease the patient’s reintubation rate, promoting a downward trend in mortality and morbidity for these patients and shortening their hospital and intensive care units length of stay.
Keywords:implementationmechanical ventilation protocolpressure-support ventilationT-tube methodWeaningSee more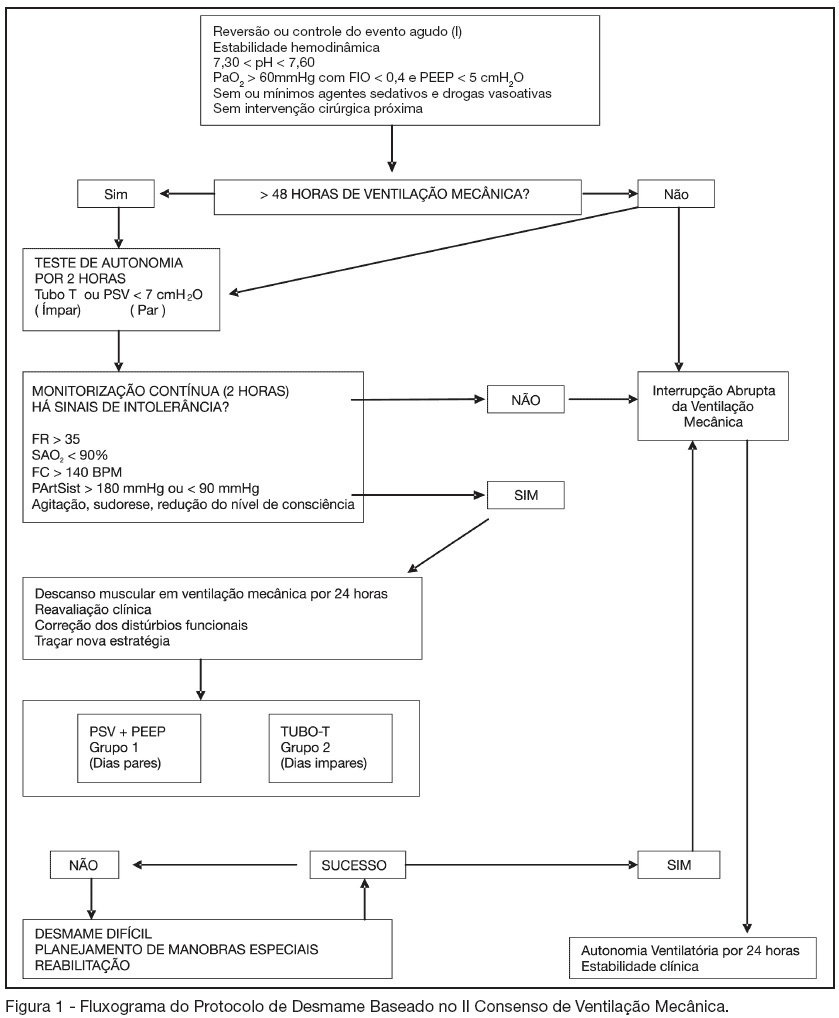
-
Artigos originais
Weaning from mechanical ventilation process at hospitals in Federal District
Rev Bras Ter Intensiva. 2007;19(1):38-43
Abstract
Artigos originaisWeaning from mechanical ventilation process at hospitals in Federal District
Rev Bras Ter Intensiva. 2007;19(1):38-43
DOI 10.1590/S0103-507X2007000100005
Views0See moreBACKGROUND AND OBJECTIVES: Concerning the mechanical ventilation, the weaning is a usual and significant intensive care process. Identifying, describing and demonstrating the techniques used by Respiratory Therapists in weaning and also obtaining its parameters in Intensive Care Units (ICU). METHODS: A survey related to the weaning process was done with active ICU Respiratory Therapists from (FD) in the year 2005. The survey consisted of 31 subjective and objective questions, some of them allowing multiple answers. RESULTS: Eighty surveys were carried out at twenty hospitals. 90% of participants were specialized staff with a mean of three year working experience in ICU. In 98.7% of the answers, doctors and respiratory therapists were responsible for operating the ventilators. In 61.3%, doctors and respiratory therapists were responsible for their use and, in 36.3%, the responsibility was solely on the respiratory therapist professionals. It was found that only twenty-four respiratory therapists (30%) follow the weaning protocol. Among the most practiced parameters from the weaning process are: respiratory frequency (98%), tidal volume (97.5%) and periferic oxygen saturation (92.5%). The least utilized are the maximum inspiratory pressure (18.8%) and the vital capacity (13.8%). CONCLUSIONS: Great differences were observed in the weaning methods, choice of parameters and the way they were collected. These variations suggest that there is a lack of routine and the need to implement simple protocols.
-
Artigos originais
Traumatic brain injury and acute respiratory distress syndrome: how to ventilate? Evaluation of clinical practice
Rev Bras Ter Intensiva. 2007;19(1):44-52
Abstract
Artigos originaisTraumatic brain injury and acute respiratory distress syndrome: how to ventilate? Evaluation of clinical practice
Rev Bras Ter Intensiva. 2007;19(1):44-52
DOI 10.1590/S0103-507X2007000100006
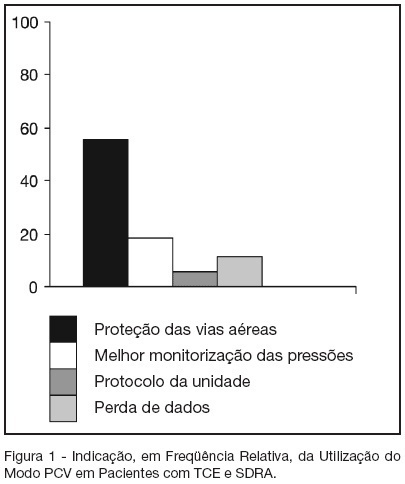
Views0See moreBACKGROUND AND OBJECTIVES: The traumatic brain injury (TBI) is a healthy-world problem, some of his patients develop respiratory failure, requiring intubation and mechanical ventilation, and the most common complications are the acute respiratory distress syndrome (ARDS). In this way, this study has the objective describe the daily clinical practice of respiratory care in this patients submit mechanical ventilation. METHODS: The methods and ventilatories parameters used to ventilate the patients with TBI and ARDS has been evaluated by a sample of physiotherapists from the city of Salvador, BA, from a descriptive study. The data were collected by face-to-face interviews in the period of October 2005 to March 2006. For in such way a half structuralized questionnaire was elaborated contends changeable social-demographic, about the hospital profile and the applied ventilatory strategy in patients with TBI that come to develop ARDS. RESULTS: The sample was composed by 70 physiotherapists, 41 (58.6%) was female, with mean of age of 31.2 ± 6.4 (24-49) years-old and graduated time 7.7 ± 6.4 (1-27) years, which 37 (52.9%) works on public hospital; 67 (95.7%) has any specialization. Sixty four physiotherapists affirm the usage of the pressure controlled ventilation mode. The peak pressure and the plateau pressure wanted to ventilate the patients with TBI and ARDS were in mean 35.6 ± 5,3 (25-50) and 28,4 ± 5,8 (15-35) cmH2O respectively. Forty eighty (68.6%) of the interviewed wants a PaCO2 in 30-35 mmHg. Thirty one (44.3%) of the interviewed finds the ideal PEEP through the best SpO2 with minor FiO2. CONCLUSIONS: It’s incontestable that the ventilatory strategy of a patient with severe TBI that become to develop ALI or ARDS is an authentic challenge; a predilection for PCV mode is observed due to the already known protective ventilation strategy.
-
Artigos originais
Analysis of stressors for the patient in Intensive Care Unit
Rev Bras Ter Intensiva. 2007;19(1):53-59
Abstract
Artigos originaisAnalysis of stressors for the patient in Intensive Care Unit
Rev Bras Ter Intensiva. 2007;19(1):53-59
DOI 10.1590/S0103-507X2007000100007
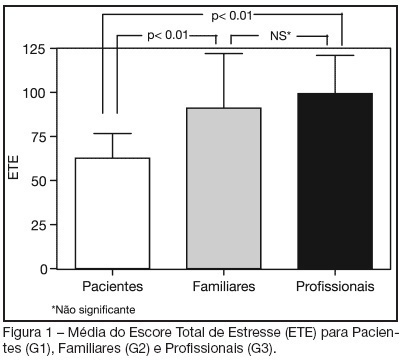
Views0See moreBACKGROUND AND OBJECTIVES: The hospital environment, especially in Intensive Care Units (ICU), due to the complexity of the assistance, as well as the physical structure, the noise, the equipments and people’s movement, is considered as stress generator for the patients. The aim of this study was to identify and stratify the stressful factors for patients at an ICU, in the perspective of the own patient, relatives and health care professionals. METHODS: A cross-sectional study was carried out between June and November 2004 in a general ICU of a private hospital. The sample was composed of three groups: patients (G1), relatives (G2) and a member of the ICU health care team responsible for the included patient (G3). In order to identify and stratify the stressful factors, we used the Intensive Care Unit Environmental Stressor Scale (ICUESS). For each individual, a total stress score (TSS) was calculated from the sum of all the answers of the scale. RESULTS: Thirty individuals were included in each group. The mean age of the three groups was: 57.30 ± 17.61 years for G1; 41.43 ± 12.19 for G2; and 40.82 ± 20.20 for G3. The mean TSS was 62.63 ± 14.01 for the patients; 91.10 ± 30.91 for the relatives; and 99.30 ± 21.60 for the health care professionals. The patients’ mean TSS was statistically lower than mean TSS of relatives and professionals (p < 0.01). The most stressful factors for the patients were: seeing family and friends only a few minutes a day; having tubes in their nose and/or mouth; and having no control on oneself. CONCLUSIONS: The perception of the main stressful factors was different among the three groups. The identification of these factors is important to the implementation of changes that can make the humanization of the ICU environment easier.
-
Artigos originais
Evaluation the quality and satisfaction of life of patients, before admission in Intensive Care Unit and after hospital discharge
Rev Bras Ter Intensiva. 2007;19(1):60-66
Abstract
Artigos originaisEvaluation the quality and satisfaction of life of patients, before admission in Intensive Care Unit and after hospital discharge
Rev Bras Ter Intensiva. 2007;19(1):60-66
DOI 10.1590/S0103-507X2007000100008
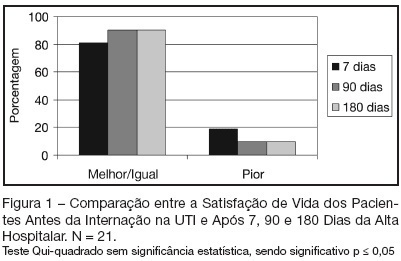
Views0See moreBACKGROUND AND OBJETIVES: To evaluate the quality and satisfaction of life (QSL) of patients before admission in ICU, and after hospital discharge. To verify the influence of the patient’s demographic/clinic/therapeutic factors in the QSL. METHODS: Prospective cohort study with quali-quantitative approach. All patients admitted in ICU/HU/UFSC from April-July 2005, who’s stayed more than 24 hours were included. Initially, the data of QSL before ICU admission, patient’s demographics/clinics/therapeutics features were recorded. Afterwards, by telephone, 7, 90 and 180 days after hospital discharge, the patients answered the questionnaires about QSL. In the sequence, all patients were subdivided into 2 main groups: unchanged or better, and worse QSL. Data were analyzed using t Student and Chi-square tests (p-value < 0.05). RESULTS: Sixty eight patients were enrolled into the study. Completed questionnaires were obtained from 21 of them. A comparison of 7, 90 and 180 days after hospital discharge showed that QSL of patients was unchanged or better at 90 and 180 days. The majority of patients expressed more satisfaction in that moment. Unchanged or better QSL was associated with advanced age. However, there were no statistical significant differences in sex, schooling, APACHE II score, length of stay, mechanical ventilation and used drugs. Sixty percent returned to their previous work. CONCLUSIONS: There was a tendency for patients who felt themselves satisfied after hospital discharge to have their QSL improved as time went bye. Better QSL was associated with advanced age. Even when patients reported worse QSL they returned to their previous work.
-
Artigos originais
Safety and efficacy of sodium enoxaparin in anti-thrombotic prophylaxis and treatment
Rev Bras Ter Intensiva. 2007;19(1):67-73
Abstract
Artigos originaisSafety and efficacy of sodium enoxaparin in anti-thrombotic prophylaxis and treatment
Rev Bras Ter Intensiva. 2007;19(1):67-73
DOI 10.1590/S0103-507X2007000100009
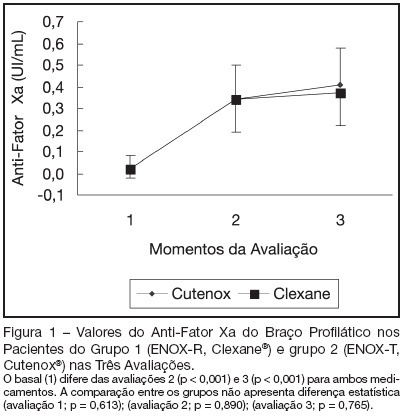
Views0See moreBACKGROUND AND OBJECTIVES: Use of low molecular weight heparins (LMWH), either prophylactic or therapeutic, is of most importance in several syndromes and diseases in daily clinical practice. Our objective in this clinical trial was to evaluate safety and efficacy of test sodium enoxaparin (ENOX-T) compared to the reference drug (ENOX-R). METHODS: We conducted a prospective, randomized, comparative, unicentric and open-labeled trial including patients with either prophylactic or therapeutic anti-thrombotic indications. A total of 100 patients were enrolled in two branches: prophylactic (n=50) and therapeutic (n=50) and two groups for each branch (group 1: ENOX-R and group 2: ENOX-T). We analyzed clinical and laboratory data in each segment. Anti-factor Xa was measured in three different moments: baseline (1st evaluation); 1st or 2nd day (2nd evaluation) and 5th to 7th day (3rd evaluation). Doppler-sonography of inferior limbs was performed on all patients in prophylactic group on 2nd or 3rd evaluation. RESULTS: The data showed that both branches (prophylactic and therapeutic) were homogenous in regard of sex, age, body mass index (BMI), serum creatinine and APACHE II severity score at admission. Anti-factor Xa results, in both prophylactic and therapeutic branches, showed expected efficacy to both drugs, without any clinical or statistical difference between them. Adverse events incurred in both groups in a similar way, without any clinical or statistical difference between them. In prophylactic branch, Doppler-sonography of inferior limbs added useful information on drugs efficacy. CONCLUSIONS: We conclude that test sodium enoxaparin (ENOX-T) was effective and safe in our patient’s cohort and equivalent to reference drug (ENOX-R).
-
Artigos de Revisão
Brain death, multiorgan donor and lung transplantation
Rev Bras Ter Intensiva. 2007;19(1):74-84
Abstract
Artigos de RevisãoBrain death, multiorgan donor and lung transplantation
Rev Bras Ter Intensiva. 2007;19(1):74-84
DOI 10.1590/S0103-507X2007000100010
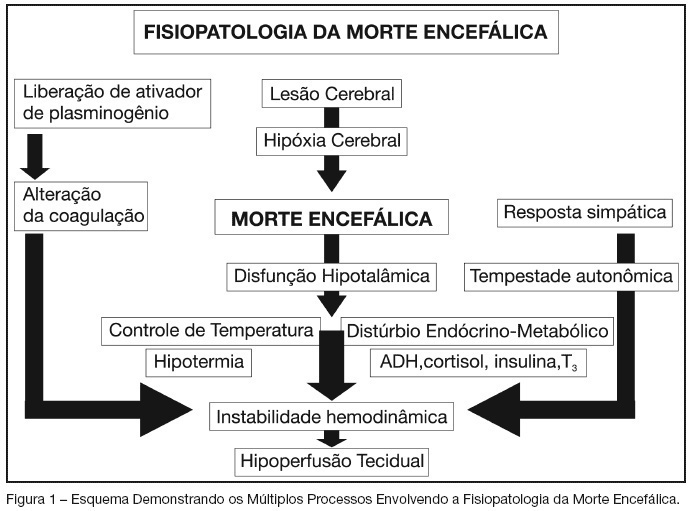
Views0See moreBACKGROUND AND OBJECTIVES: Organ transplantation is now an accepted option for end stage organ disease in well selected patients. This position is a result of great advances in the field of immunology, critical care medicine and pharmacology. However, organ transplantation is now suffering from its own success as the number of patients in waiting lists is dramatically increasing the same is not happening with organ availability results in increasing number of mortalities while waiting for transplantation. Transplant community responses to this situation consist of reviewing the criteria for organ acceptability and developing new strategies to get organs as the called non-heart beating organ donors. CONTENTS: However the physiopathology of brain death and its consequences are now better understood helping in such patients’ management. The purpose of this review is to help to identify the most important clinical and therapeutic aspects related to its physiopathology as depletion of vasoactives substances and its importance in the management of cardio and respiratory systems. We also discuss endocrine and hidroelectrolytes disturbances. Organ specific data are also focused in order to offer a whole view of donor management. CONCLUSIONS: It is important to observe that new technologies will be available in the near future to diminish the low rate between organ availability and organ waiting patients. In conclusion, with the raising numbers in transplant waiting lists and scarce resources of organs make us believe that we have to improve the management of multi organ donors and the preservation technology in order to reduce the mortality in such waiting lists.
-
Artigos de Revisão
Nutritional therapy in Intensive Care Unit
Rev Bras Ter Intensiva. 2007;19(1):90-97
Abstract
Artigos de RevisãoNutritional therapy in Intensive Care Unit
Rev Bras Ter Intensiva. 2007;19(1):90-97
DOI 10.1590/S0103-507X2007000100012
Views0BACKGROUND AND OBJECTIVES: The purpose of this review is to approach the main necessary aspects for the accomplishment of safety and efficient nutritional therapy to the critically ill patient. CONTENTS: Bibliographical survey with didactic books and scientific articles was made in Portuguese, English and Spanish with results of the last 20 years. Nutritional support is an integrant part in the care of patients in intensive care units. The success of the nutritional therapy involves the stages of nutritional assessment, determines the route of diet infusion and the calories and nutrients needs. CONCLUSIONS: The use of nutrients with immune function (immunonutrients) is each more frequents, however, its use is not well established for critical illness. More clinical studies are necessary to establish the best form to nourish the critical ill patient.
Keywords:critical ill patiententeral nutritionimmunonutritionnutritional therapyparenteral nutritionSee more -
Artigos de Revisão
Severe traumatic braininjury in children and adolescents
Rev Bras Ter Intensiva. 2007;19(1):98-106
Abstract
Artigos de RevisãoSevere traumatic braininjury in children and adolescents
Rev Bras Ter Intensiva. 2007;19(1):98-106
DOI 10.1590/S0103-507X2007000100013
Views0See moreBACKGROUND AND OBJECTIVES: Present a critical review of traumatic brain injury (TBI) in children and adolescents, focusing on severe TBI, the mortality and the factors related with poor outcome. CONTENTS: It was made a systematic review in MEDLINE, SciElo e Lilacs, with the key words: traumatic brain injury, craniocerebral trauma, children and mortality. The most important articles related in the Guidelines of Brain Trauma Foundation (2000 e 2003) were selected too. TBI is one of the most important causes of mortality and morbidity in children and adolescents, and morbidity in children and adolescents. The mortality variation was between 10% and 55%, depending of the patients select criteria, trauma severity and units where the studies were made. The children mortality was, in general, lower than that found in adults and the most important factors related with an increased mortality were: Glasgow Coma Score, hypotension, cerebral swelling and lower cerebral perfusion press. Severe TBI endpoint treatment is to correct the secondary brain lesions related factors. CONCLUSIONS: The factors related with better outcomes in children with severe TBI are still obscures, despite the large number of studies, large numbers of studies. Many of these factors can be avoided or correct by aggressive fluid resuscitation, surgery treatment, monitoration and adequate intensive care.
-
Artigos de Revisão
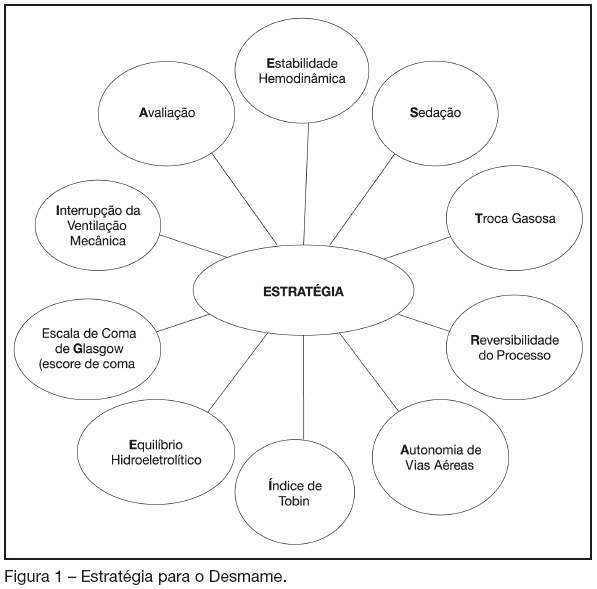
Weaning from mechanical ventilation: let’s perform a strategy
Rev Bras Ter Intensiva. 2007;19(1):107-112
Abstract
Artigos de RevisãoWeaning from mechanical ventilation: let’s perform a strategy
Rev Bras Ter Intensiva. 2007;19(1):107-112
DOI 10.1590/S0103-507X2007000100014
Views0See moreBACKGROUND AND OBJECTIVES: Weaning patients from mechanical ventilation is still a challenge in Intensive Care Units (ICU) and is related to complications and mortality. Daily rounds at the bedside, which are part of good care, can identify patients able to undergo to spontaneous breathing trials. The authors suggest one mnemonic technique with the term “ESTRATEGIA” (strategy) considering some key aspects, as a checklist, which can be applied by any person of the multidisciplinary team, during the bedside rounds, in order to shorten the weaning time. CONTENTS: To introduce the word Strategy as a mnemonic method based on the studies related to weaning from mechanical ventilation and its applicability as a checklist in any intensive care unit by the multidisciplinary team where each letter reminds some key aspects related to the subject. CONCLUSIONS: The applicability of a mnemonic mechanism as a checklist for weaning patients from mechanical ventilation easily practiced during the daily round to identify those who are able to undergo to spontaneous breathing trials.
-
Relatos de Caso
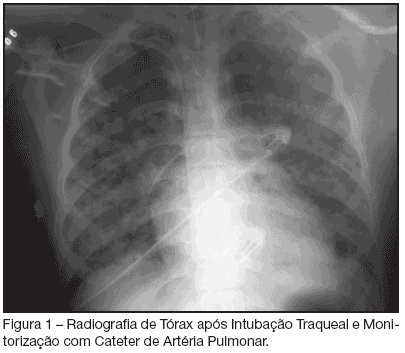
Varicella pneumonia complicated with acute respiratory distress syndrome: two cases report
Rev Bras Ter Intensiva. 2007;19(1):113-117
Abstract
Relatos de CasoVaricella pneumonia complicated with acute respiratory distress syndrome: two cases report
Rev Bras Ter Intensiva. 2007;19(1):113-117
DOI 10.1590/S0103-507X2007000100015
Views0See moreBACKGROUNG AND OBJECTIVES: Varicella is an exantematic disease caused by varicella-zoster virus. Varicella pneumonia complicated with acute respiratory distress syndrome (ARDS) is very rare in adults and is associated with high morbimortality. We report two cases of ARDS secondary to varicella-zoster virus pneumonia. CASES REPORT: We report two cases of ARDS and multiple organ dysfunction syndrome (MODS) secondary to varicella-zoster virus pneumonia. A 15-year-old man with human immunodeficiency virus (HIV) infection and a 29-year-old immunocompetent female were admitted in the ICU with primary varicella infection and pneumonia. Both cases progressed towards ARDS, severe thrombocytopenia and acidosis. In addition cardiovascular and renal failure occurred in the first and second patients, respectively. Treatment consisted of immediate administration of intravenous acyclovir and a lung-protective ventilation strategy. CONCLUSIONS: Both cases of varicella-zoster pneumonia, complicated with ARDS and MODS, had a favourable outcome.
-
Relatos de Caso
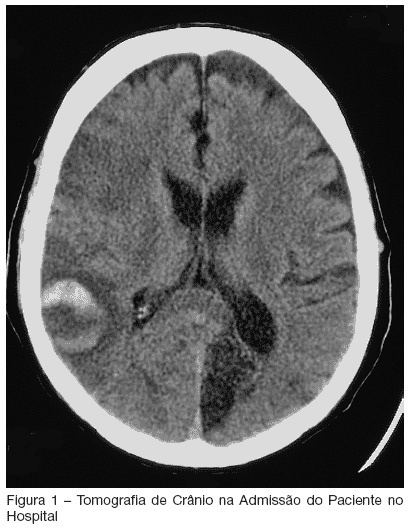
Aspirative pneumonia associated to swallowing dysfunction: case report
Rev Bras Ter Intensiva. 2007;19(1):118-122
Abstract
Relatos de CasoAspirative pneumonia associated to swallowing dysfunction: case report
Rev Bras Ter Intensiva. 2007;19(1):118-122
DOI 10.1590/S0103-507X2007000100016
Views0See moreBACKGROUND AND OBJECTIVES: Critically ill patients represent a population with multiple risk factors for aspiration. Features such as decreased level of consciousness, mechanical ventilation, and comorbities as stroke, correlate with this increased threat in intensive care unit (ICU) patients. Recognition of deglutition dysfunction may identify patients at high risk of aspiration, and thereby help to avoid pulmonary complications such as recurrent pneumonia. The goal of our report is show a severe case of recurrent aspirative pneumonia after acute stroke and intubation, alerting to appropriate diagnosis and treatment of this condition. CASE REPORT: A male patient, 57 year old, was admitted to the hospital because of acute stroke. Ten days later, the patient began to have fever and severe shortness of breath. He was admitted to the ICU necessitating of intratracheal intubation. Four days after intubation he was extubated, however, he had a new aspirative pneumonia in ICU, newly treated. An evaluation of swallowing demonstrated a severe deglutition dysfunction with a high risk of aspiration. The patient was transferred, but aspirative pneumonia was diagnosed eight days after his ICU discharge and he was readmitted, stayed for a long time in ICU and presenting severe morbidity. CONCLUSIONS: ICU patients who are at risk for swallowing dysfunction and aspiration should be identified to prevent their associated morbidity and mortality.
-
Relatos de Caso
Negative pressure pulmonary edema after tracheal extubation: case report
Rev Bras Ter Intensiva. 2007;19(1):123-127
Abstract
Relatos de CasoNegative pressure pulmonary edema after tracheal extubation: case report
Rev Bras Ter Intensiva. 2007;19(1):123-127
DOI 10.1590/S0103-507X2007000100017
Views0See moreBACKGROUND AND OBJECTIVES: Negative pressure pulmonary edema after acute upper airway obstruction is a well-described event, thought infrequently diagnosed and reported. This report aimed at presenting a case of postextubation negative pressure pulmonary edema refractory to use of diuretics and with successful therapeutic after using positive pressure noninvasive mechanic ventilation. CASE REPORT: A 22-year-old-woman underwent an operation to opened colecistectomy. The preoperative exams were abnormality us. Immediately after the extubation the patient presented with dyspnea and lungs stertors. The treatment for the acute pulmonary edema started with oxygen therapy under Venturi mask, lifting up chest and diuretic. The patient was transferred to Intensive Care Unit due to the lack of success with the treatment. A noninvasive ventilation (NIV) was started with support pressure of 15 cmH2O and PEEP of 5 cmH2O with resolution of symptoms. The patient was maintained under observation for 24 hours after the event with good conditions and received discharge to room without symptoms. CONCLUSIONS: Negative pressure pulmonary edema (NPPE) is a difficult diagnosed event and it must be always considered when patient develop with symptoms and signals of respiratory insufficiency postextubation. In our case was possible to treat with positive pressure non-invasive mechanical ventilation, but in case of the NIV failure the tracheal intubation and the invasive mechanical ventilatory support be initiated to improve the oxygen levels of the patient.
-
Relatos de Caso
Strongyloides Stercoralis hyperinfection syndrome: case report
Rev Bras Ter Intensiva. 2007;19(1):128-131
Abstract
Relatos de CasoStrongyloides Stercoralis hyperinfection syndrome: case report
Rev Bras Ter Intensiva. 2007;19(1):128-131
DOI 10.1590/S0103-507X2007000100018
Views0See moreBACKGROUND AND OBJECTIVES: Strongyloides Stercoralis is a common cause of gastrointestinal infection. This nematode can produce an overwhelming hyperinfection syndrome, especially in the immunocompromised patient. Typically, patients present with pulmonary symptoms, but subsequently they can acquire Gram-negative sepsis. The objective of this report is to describe a lethal case and call attention to the importance of early diagnosis and treatment. CASE REPORT: Male patient, 60 year-old with diagnosis of timoma, treated with surgery, radiotherapy and chemotherapy in the past. He presented to the emergency room complaining of diarrhea and dyspnea, and then transferred to the ICU after development of hypoxemic acute respiratory failure and refractory septic shock, and despite treatment the patient died. A bronchial sample of sputum showed Strongyloides stercoralis worms. CONCLUSIONS: Strongyloides stercoralis infection symptoms are usually mild, but in the setting of impaired host immunity, a disseminated and severe illness may occur. Clinicians must be aware for patients from endemic areas. Diagnosis may be established through sputum and stool examination for Strongyloides stercoralis worms.
-
Agradecimentos
Rev Bras Ter Intensiva. 2007;19(1):132-132
Abstract
Agradecimentos
Rev Bras Ter Intensiva. 2007;19(1):132-132
DOI 10.1590/S0103-507X2007000100019
Views0Agradecimentos Agradeço a todos que colaboraram com a RBTI revisando artigos e fazendo sugestões ao longo de 2006 para a melhora da nossa revista.[…]See more





