You searched for:"Soraia Genebra Ibrahim"
We found (7) results for your search.-
Original Article
Brazilian version of the Critical Care Functional Rehabilitation Outcome Measure: translation, cross-cultural adaptation and evaluation of clinimetric properties
Rev Bras Ter Intensiva. 2022;34(2):272-278
Abstract
Original ArticleBrazilian version of the Critical Care Functional Rehabilitation Outcome Measure: translation, cross-cultural adaptation and evaluation of clinimetric properties
Rev Bras Ter Intensiva. 2022;34(2):272-278
DOI 10.5935/0103-507X.20220025-en
Views4ABSTRACT
Objective:
To translate, crossculturally adapt and evaluate the clinimetric properties of the Critical Care Functional Rehabilitation Outcome Measure for evaluating the functionality of patients admitted to intensive care units in Brazil.
Methods:
The process of translation and cross-cultural adaptation involved the following steps: initial translation, synthesis, back-translation, expert committee review and pretesting. The intra- and interrater reliability and agreement were analyzed between two physical therapists who evaluated the same group of patients (n = 35). The evaluations were performed by each therapist independently and blinded to the score assigned by the other professional. The qualitative analysis was performed by the review committee, and the experts adapted and synthesized the Portuguese translation of the Critical Care Functional Rehabilitation Outcome Measure.
Results:
There was agreement between the initial Brazilian translations of the Critical Care Functional Rehabilitation Outcome Measure scale. The conceptual, idiomatic, semantic and experimental equivalences between the original and translated versions were assessed, resulting in the final Brazilian version of the scale, called the Medida de Resultado da Reabilitação Funcional em Cuidados Intensivos. The evaluation of the clinimetric properties showed evidence of a high degree of agreement and reliability, as all had an intraclass correlation coefficient above 0.75. The overall intraclass correlation coefficient was 0.89.
Conclusion:
The translated version of the Critical Care Functional Rehabilitation Outcome Measure scale for assessing the functionality of patients admitted to an intensive care unit can be used reliably in Brazil following translation and cross-cultural adaptation to Brazilian Portuguese and presents evidence of excellent interrater reliability.
Keywords:Critical illnessExercise therapyHealth careInpatientsIntensive care unitsMobility limitationOutcome assessmentPhysical therapy modalitiesRecovery of functionSurveys and questionnairesSee more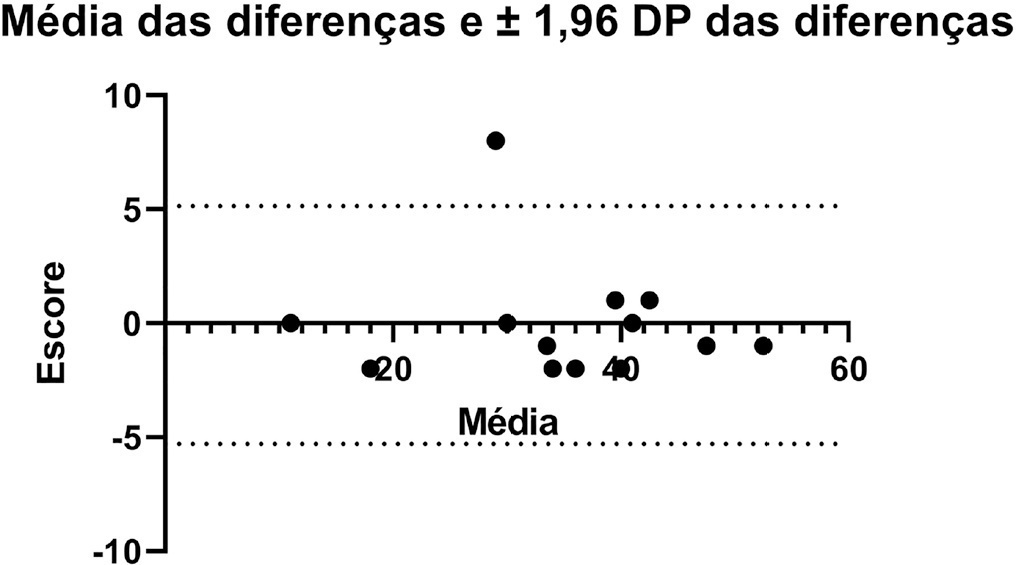
-
Review Article
Quality of life in survivors after a period of hospitalization in the intensive care unit: a systematic review
Rev Bras Ter Intensiva. 2018;30(4):496-507
Abstract
Review ArticleQuality of life in survivors after a period of hospitalization in the intensive care unit: a systematic review
Rev Bras Ter Intensiva. 2018;30(4):496-507
DOI 10.5935/0103-507X.20180071
Views0See moreABSTRACT
Objective:
To assess the long-term, health-related quality of life of intensive care unit survivors by systematic review.
Methods:
The search for, and selection and analysis of, observational studies that assessed the health-related quality of life of intensive care unit survivors in the electronic databases LILACS and MEDLINE® (accessed through PubMed) was performed using the indexed MESH terms “quality of life [MeSH Terms]” AND “critically illness [MeSH Terms]”. Studies on adult patients without specific prior diseases published in English in the last 5 years were included in this systematic review. The citations were independently selected by three reviewers. Data were standardly and independently retrieved by two reviewers, and the quality of the studies was assessed using the Newcastle-Ottawa scale.
Results:
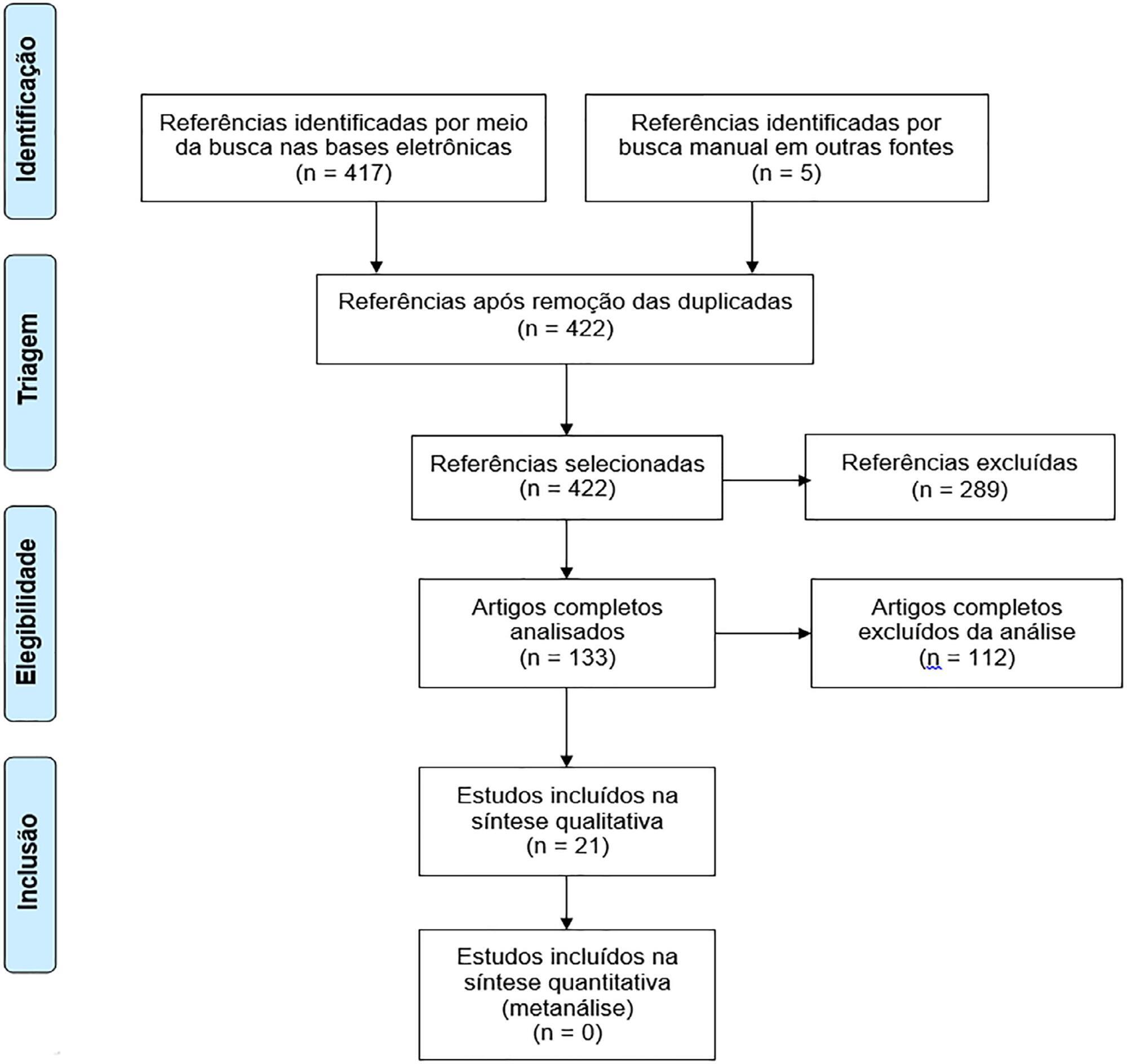
In total, 19 observational cohort and 2 case-control studies of 57,712 critically ill patients were included. The follow-up time of the studies ranged from 6 months to 6 years, and most studies had a 6-month or 1-year follow up. The health-related quality of life was assessed using two generic tools, the EuroQol and the Short Form Health Survey. The overall quality of the studies was low.
Conclusions:
Long-term, health-related quality of life is compromised among intensive care unit survivors compared with the corresponding general population. However, it is not significantly affected by the occurrence of sepsis, delirium, and acute kidney injury during intensive care unit admission when compared with that of critically ill patient control groups. High-quality studies are necessary to quantify the health-related quality of life among intensive care unit survivors.
-
Original Article
Lung hyperinflation by mechanical ventilation versus isolated tracheal aspiration in the bronchial hygiene of patients undergoing mechanical ventilation
Rev Bras Ter Intensiva. 2016;28(1):27-32
Abstract
Original ArticleLung hyperinflation by mechanical ventilation versus isolated tracheal aspiration in the bronchial hygiene of patients undergoing mechanical ventilation
Rev Bras Ter Intensiva. 2016;28(1):27-32
DOI 10.5935/0103-507X.20160010
Views0See moreABSTRACT
Objective:
To determine the efficacy of lung hyperinflation maneuvers via a mechanical ventilator compared to isolated tracheal aspiration for removing secretions, normalizing hemodynamics and improving lung mechanics in patients on mechanical ventilation.
Methods:
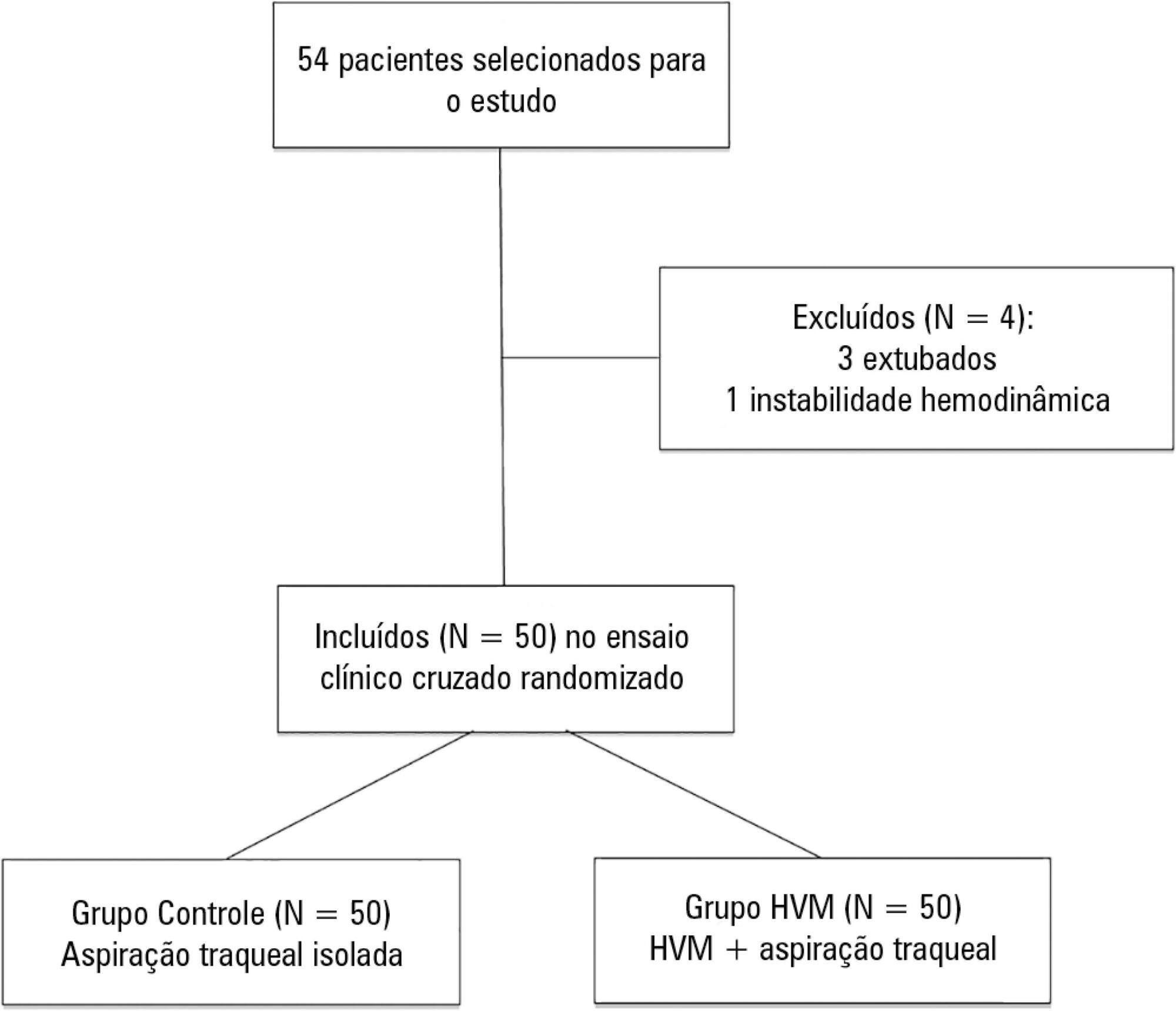
This was a randomized crossover clinical trial including patients admitted to the intensive care unit and on mechanical ventilation for more than 48 hours. Patients were randomized to receive either isolated tracheal aspiration (Control Group) or lung hyperinflation by mechanical ventilator (MVH Group). Hemodynamic and mechanical respiratory parameters were measured along with the amount of aspirated secretions.
Results:
A total of 50 patients were included. The mean age of the patients was 44.7 ± 21.6 years, and 31 were male. Compared to the Control Group, the MVH Group showed greater aspirated secretion amount (3.9g versus 6.4g, p = 0.0001), variation in mean dynamic compliance (-1.3 ± 2.3 versus -2.9 ± 2.3; p = 0.008), and expired tidal volume (-0.7 ± 0.0 versus -54.1 ± 38.8, p = 0.0001) as well as a significant decrease in peak inspiratory pressure (0.2 ± 0.1 versus 2.5 ± 0.1; p = 0.001).
Conclusion:
In the studied sample, the MVH technique led to a greater amount of aspirated secretions, significant increases in dynamic compliance and expired tidal volume and a significant reduction in peak inspiratory pressure.
-
AUTHORS’ RESPONSE
Rev Bras Ter Intensiva. 2015;27(3):293-295
Abstract
AUTHORS’ RESPONSE
Rev Bras Ter Intensiva. 2015;27(3):293-295
DOI 10.5935/0103-507X.20150049
Views0Thank you for your compliments and the opportunity to discuss not only the practices of early mobilization and out-of-bed extubation but also the incorporation of these practices into the care of critically ill patients in our country.First, we note that the benefits of early mobilization (the mobilization of patients who have received mechanical ventilation for […]See more -
Review Articles
Alveolar recruitment maneuver and perioperative ventilatory support in obese patients undergoing abdominal surgery
Rev Bras Ter Intensiva. 2013;25(4):312-318
Abstract
Review ArticlesAlveolar recruitment maneuver and perioperative ventilatory support in obese patients undergoing abdominal surgery
Rev Bras Ter Intensiva. 2013;25(4):312-318
DOI 10.5935/0103-507X.20130053
Views0The development of abdominal surgery represents an alternative therapy for the morbidly obese; however, patients undergoing this surgical procedure often experience postoperative pulmonary complications. The use of alveolar recruitment maneuvers and/or perioperative ventilatory strategies is a possible alternative to reduce these complications, focusing on the reduction of postoperative pulmonary complications. In this review, the benefits of perioperative ventilatory strategies and the implementation of alveolar recruitment maneuvers in obese patients undergoing abdominal surgery are described.
Keywords:AnesthesiaObesity/surgeryPostoperative complicationsPostoperative periodPulmonary alveoli/physiopathologyRespiration, artificialRespiratory mechanicsSee more -
Original Articles – Clinical Research
Use of a noninvasive ventilation device following tracheotomy: an alternative to facilitate ICU discharge?
Rev Bras Ter Intensiva. 2012;24(2):167-172
Abstract
Original Articles – Clinical ResearchUse of a noninvasive ventilation device following tracheotomy: an alternative to facilitate ICU discharge?
Rev Bras Ter Intensiva. 2012;24(2):167-172
DOI 10.1590/S0103-507X2012000200012
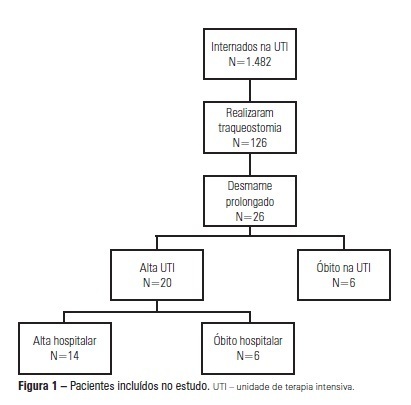
Views0See moreOBJECTIVE: We aimed to assess the use of noninvasive ventilation devices in patients with prolonged weaning following tracheotomy. METHODS: We performed a retrospective observational study using data collected from the clinical records of tracheotomized patients diagnosed with prolonged weaning. The participants were hospitalized in the adult intensive care unit of Moinhos de Vento Hospital, Porto Alegre (RS) between December 2007 and December 2008. RESULTS: In the data collection period, 1,482 patients were admitted to the intensive care unit. In total, 126 patients underwent tracheotomies, and 26 of these patients met the inclusion criteria for participating in the study. The average age of the patients in our sample was 73 ± 12 years. In our sample, 57.7% of the participants were female, and 80.8% were admitted as a result of acute hypoxemic respiratory failure. After the tracheotomy, the patients remained under mechanical ventilation for an average of 29.8 days. After the initiation of the experimental protocol, the tracheotomized patients remained under ventilation for an average of 53.5 days on a portable noninvasive device connected to the tracheotomy. There were three possible outcomes for the patients. They were discharged, were weaned from the noninvasive ventilation, or died in the intensive care unit or hospital ward. In total, 76.9% (20/26) of the patients were discharged from the intensive care unit, and 53.8% (14/26) of the patients were discharged from the hospital. CONCLUSION: The use of noninvasive portable ventilators connected to the tracheotomy may represent an alternative for discontinuing ventilationand discharging tracheotomized patients with prolonged ventilatory weaning from intensive care unit.
-
Letters to the Editor
Influence of peripheral muscle strength on the decannulation success rate
Rev Bras Ter Intensiva. 2011;23(3):380-381
Abstract
Letters to the EditorInfluence of peripheral muscle strength on the decannulation success rate
Rev Bras Ter Intensiva. 2011;23(3):380-381
Search
Search in:
KEY WORDS
Case reports Child Coronavirus infections COVID-19 Critical care Critical illness Extracorporeal membrane oxygenation Infant, newborn Intensive care Intensive care units Intensive care units, pediatric mechanical ventilation Mortality Physical therapy modalities Prognosis Respiration, artificial Respiratory insufficiency risk factors SARS-CoV-2 Sepsis




