You searched for:"Edison Moraes Rodrigues Filho"
We found (9) results for your search.-
Original Article
Resuscitation fluid practices in Brazilian intensive care units: a secondary analysis of Fluid-TRIPS
Rev Bras Ter Intensiva. 2021;33(2):206-218
Abstract
Original ArticleResuscitation fluid practices in Brazilian intensive care units: a secondary analysis of Fluid-TRIPS
Rev Bras Ter Intensiva. 2021;33(2):206-218
DOI 10.5935/0103-507X.20210028
Views1See moreAbstract
Objective:
To describe fluid resuscitation practices in Brazilian intensive care units and to compare them with those of other countries participating in the Fluid-TRIPS.
Methods:
This was a prospective, international, cross-sectional, observational study in a convenience sample of intensive care units in 27 countries (including Brazil) using the Fluid-TRIPS database compiled in 2014. We described the patterns of fluid resuscitation use in Brazil compared with those in other countries and identified the factors associated with fluid choice.
Results:
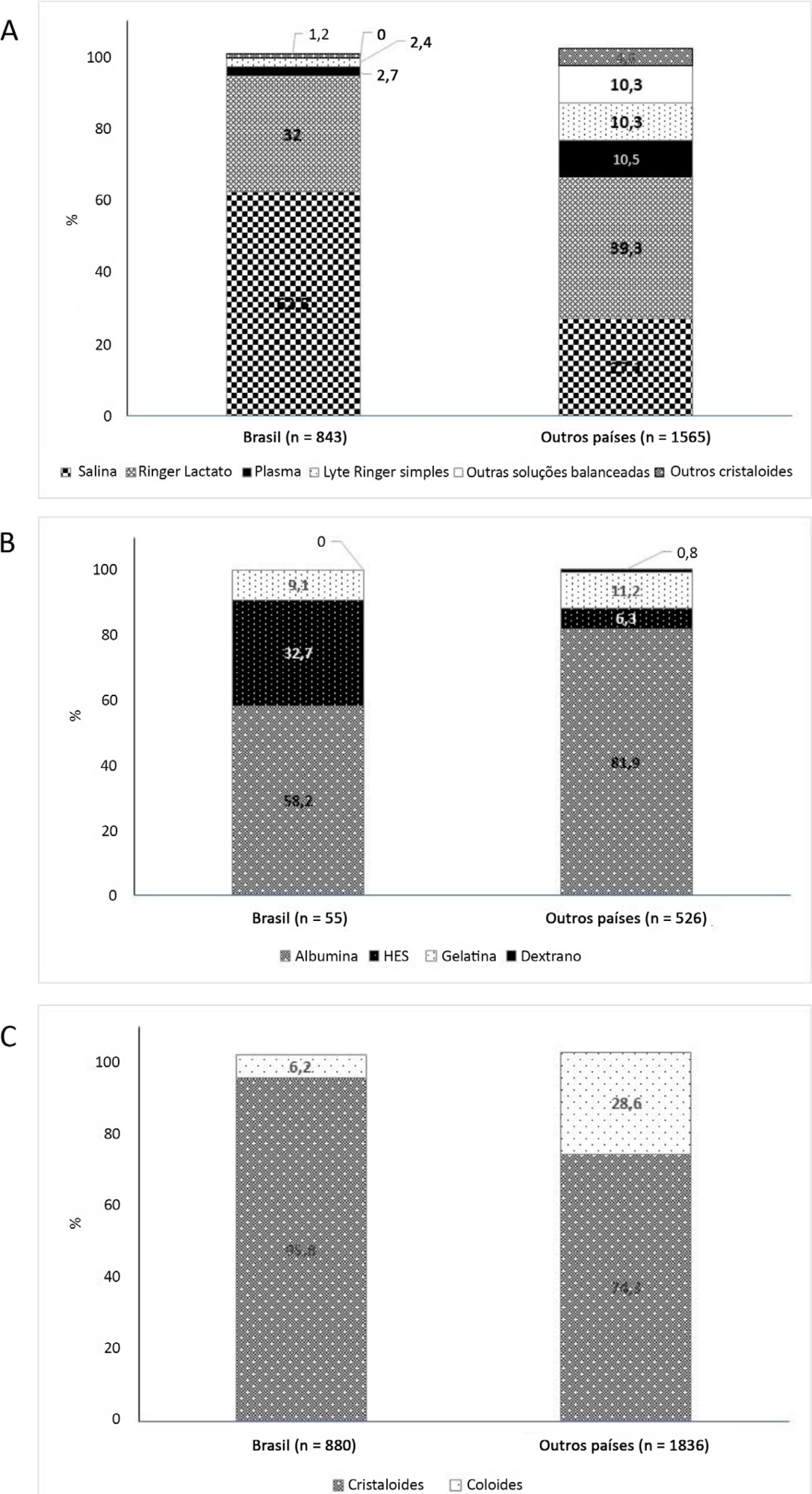
On the study day, 3,214 patients in Brazil and 3,493 patients in other countries were included, of whom 16.1% and 26.8% (p < 0.001) received fluids, respectively. The main indication for fluid resuscitation was impaired perfusion and/or low cardiac output (Brazil: 71.7% versus other countries: 56.4%, p < 0.001). In Brazil, the percentage of patients receiving crystalloid solutions was higher (97.7% versus 76.8%, p < 0.001), and 0.9% sodium chloride was the most commonly used crystalloid (62.5% versus 27.1%, p < 0.001). The multivariable analysis suggested that the albumin levels were associated with the use of both crystalloids and colloids, whereas the type of fluid prescriber was associated with crystalloid use only.
Conclusion:
Our results suggest that crystalloids are more frequently used than colloids for fluid resuscitation in Brazil, and this discrepancy in frequencies is higher than that in other countries. Sodium chloride (0.9%) was the crystalloid most commonly prescribed. Serum albumin levels and the type of fluid prescriber were the factors associated with the choice of crystalloids or colloids for fluid resuscitation.
-
Original Article
Brain death-induced cytokine release is not associated with primary graft dysfunction: a cohort study
Rev Bras Ter Intensiva. 2019;31(1):86-92
Abstract
Original ArticleBrain death-induced cytokine release is not associated with primary graft dysfunction: a cohort study
Rev Bras Ter Intensiva. 2019;31(1):86-92
DOI 10.5935/0103-507X.20190009
Views1See moreABSTRACT
Objective:
To examine the association between donor plasma cytokine levels and the development of primary graft dysfunction of organs transplanted from deceased donors.
Methods:
Seventeen deceased donors and the respective 47 transplant recipients were prospectively included in the study. Recipients were divided into two groups: group 1, patients who developed primary graft dysfunction; and group 2, patients who did not develop primary graft dysfunction. Donor plasma levels of TNF, IL-6, IL-1β, and IFN-γ assessed by ELISA were compared between groups.
Results:
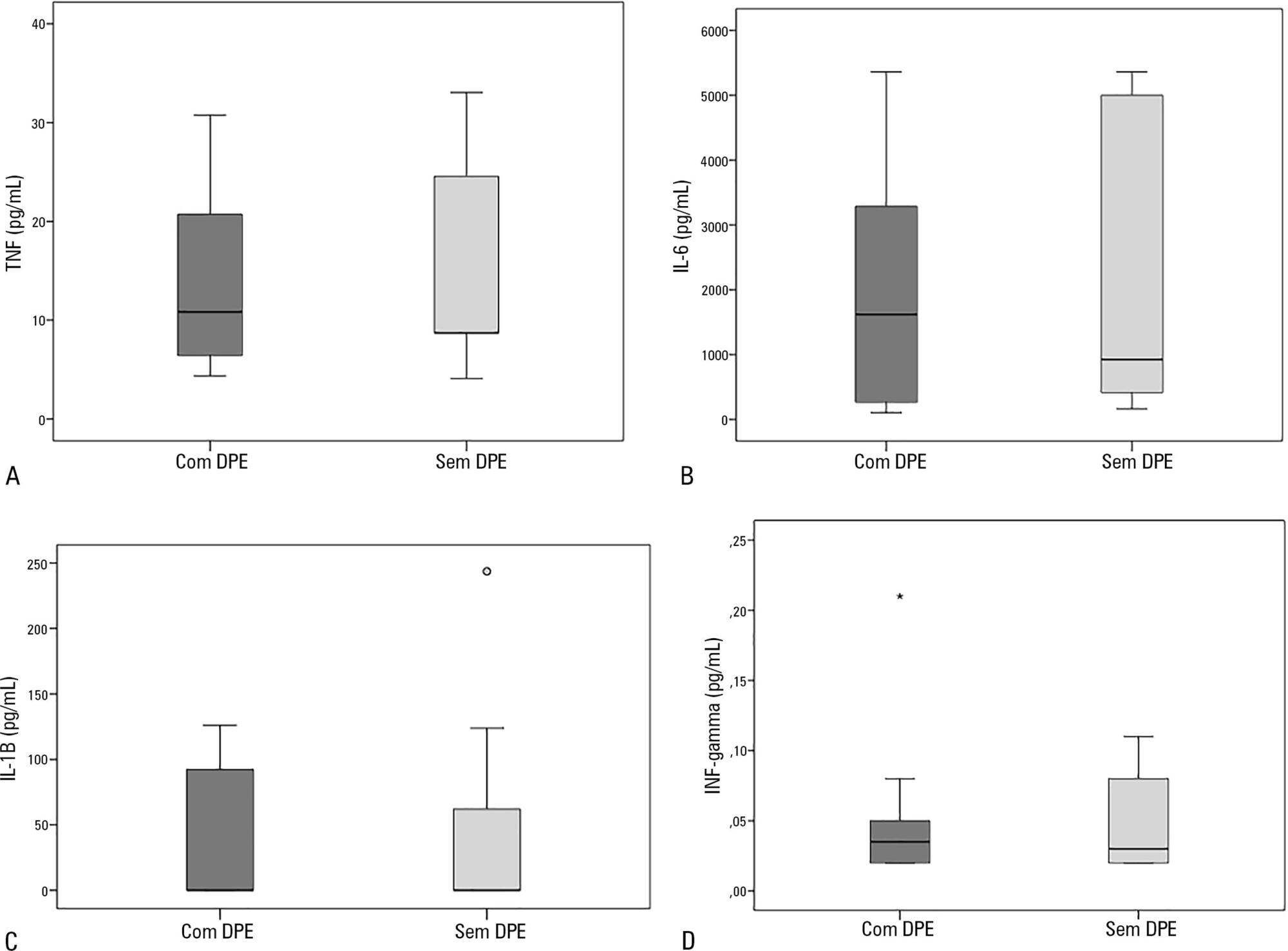
Sixty-nine organs were retrieved, and 48 transplants were performed. Donor plasma cytokine levels did not differ between groups (in pg/mL): TNF, group 1: 10.8 (4.3 – 30.8) versus group 2: 8.7 (4.1 – 33.1), p = 0.63; IL-6, group 1: 1617.8 (106.7 – 5361.7) versus group 2: 922.9 (161.7 – 5361.7), p = 0.56; IL-1β, group 1: 0.1 (0.1 – 126.1) versus group 2: 0.1 (0.1 – 243.6), p = 0.60; and IFN-γ, group 1: 0.03 (0.02 – 0.2) versus group 2: 0.03 (0.02 – 0.1), p = 0.93). Similar findings were obtained when kidney transplants were analyzed separately.
Conclusion:
In this sample of transplant recipients, deceased donor plasma cytokines TNF, IL-6, IL-1β, and IFN-γ were not associated with the development of primary graft dysfunction.
-
Original Article
Thrombin activatable fibrinolysis inhibitor as a bleeding predictor in liver transplantation: a pilot observational study
Rev Bras Ter Intensiva. 2016;28(2):161-166
Abstract
Original ArticleThrombin activatable fibrinolysis inhibitor as a bleeding predictor in liver transplantation: a pilot observational study
Rev Bras Ter Intensiva. 2016;28(2):161-166
DOI 10.5935/0103-507X.20160031
Views0See moreABSTRACT
Objective:
To correlate the levels of thrombin activatable fibrinolysis inhibitor in the immediate postoperative period and at 24 hours postoperatively with the volume of intraoperative bleeding.
Methods:
Twenty-one patients allocated immediately before (elective or emergency) liver transplantation were analyzed. Blood samples were collected for thrombin activatable fibrinolysis inhibitor analysis at three different time points: immediately before liver transplantation (preoperative thrombin activatable fibrinolysis inhibitor), immediately after the surgical procedure (immediate postoperative thrombin activatable fibrinolysis inhibitor), and 24 hours after surgery (thrombin activatable fibrinolysis inhibitor 24 hours after surgery). The primary outcome of the study was to correlate the preoperative and immediate postoperative levels of thrombin activatable fibrinolysis inhibitor with intraoperative blood loss.
Results:
There was a correlation between the preoperative thrombin activatable fibrinolysis inhibitor levels and bleeding volume (ρ = -0.469; p = 0.05) but no correlation between the immediate postoperative thrombin activatable fibrinolysis inhibitor and bleeding volume (ρ = -0.062; p = 0.79). No variable included in the linear regression analysis (prehemoglobin, prefibrinogen and preoperative thrombin activatable fibrinolysis inhibitor) was a bleeding predictor. There was a similar trend in the variation between the levels of thrombin activatable fibrinolysis inhibitor at the three different time points and fibrinogen levels. Patients who died within 6 months (14.3%) showed decreased preoperative and immediate postoperative levels of thrombin activatable fibrinolysis compared with survivors (preoperative: 1.3 ± 0.15 versus 2.55 ± 0.53, p = 0.06; immediate postoperative: 1.2 ± 0.15 versus 2.5 ± 0.42, p = 0.007).
Conclusion:
There was a moderate correlation between preoperative thrombin activatable fibrinolysis inhibitor and intraoperative bleeding in liver transplantation patients, although the predictive role of this variable independent of other variables remains uncertain. Preoperative and immediate postoperative thrombin activatable fibrinolysis inhibitor levels may have a role in the survival prognosis of this population; however, this possibility requires confirmation in further studies with larger sample sizes.
-
Original Articles
Inflammatory and perfusion markers as risk factors and predictors of critically ill patient readmission
Rev Bras Ter Intensiva. 2014;26(2):130-136
Abstract
Original ArticlesInflammatory and perfusion markers as risk factors and predictors of critically ill patient readmission
Rev Bras Ter Intensiva. 2014;26(2):130-136
DOI 10.5935/0103-507X.20140019
Views0Objective:
To assess the performance of central venous oxygen saturation, lactate, base deficit, and C-reactive protein levels and SOFA and SWIFT scores on the day of discharge from the intensive care unit as predictors of patient readmission to the intensive care unit.
Methods:
This prospective and observational study collected data from 1,360 patients who were admitted consecutively to a clinical-surgical intensive care unit from August 2011 to August 2012. The clinical characteristics and laboratory data of readmitted and non-readmitted patients after discharge from the intensive care unit were compared. Using a multivariate analysis, the risk factors independently associated with readmission were identified.
Results:
The C-reactive protein, central venous oxygen saturation, base deficit, and lactate levels and the SWIFT and SOFA scores did not correlate with the readmission of critically ill patients. Increased age and contact isolation because of multidrug-resistant organisms were identified as risk factors that were independently associated with readmission in this study group.
Conclusion:
Inflammatory and perfusion parameters were not associated with patient readmission. Increased age and contact isolation because of multidrug-resistant organisms were identified as predictors of readmission to the intensive care unit.
Keywords:C-reactive proteinLactatePatient readmissionPatient readmission/economicsPatient safetyrisk factorsSee more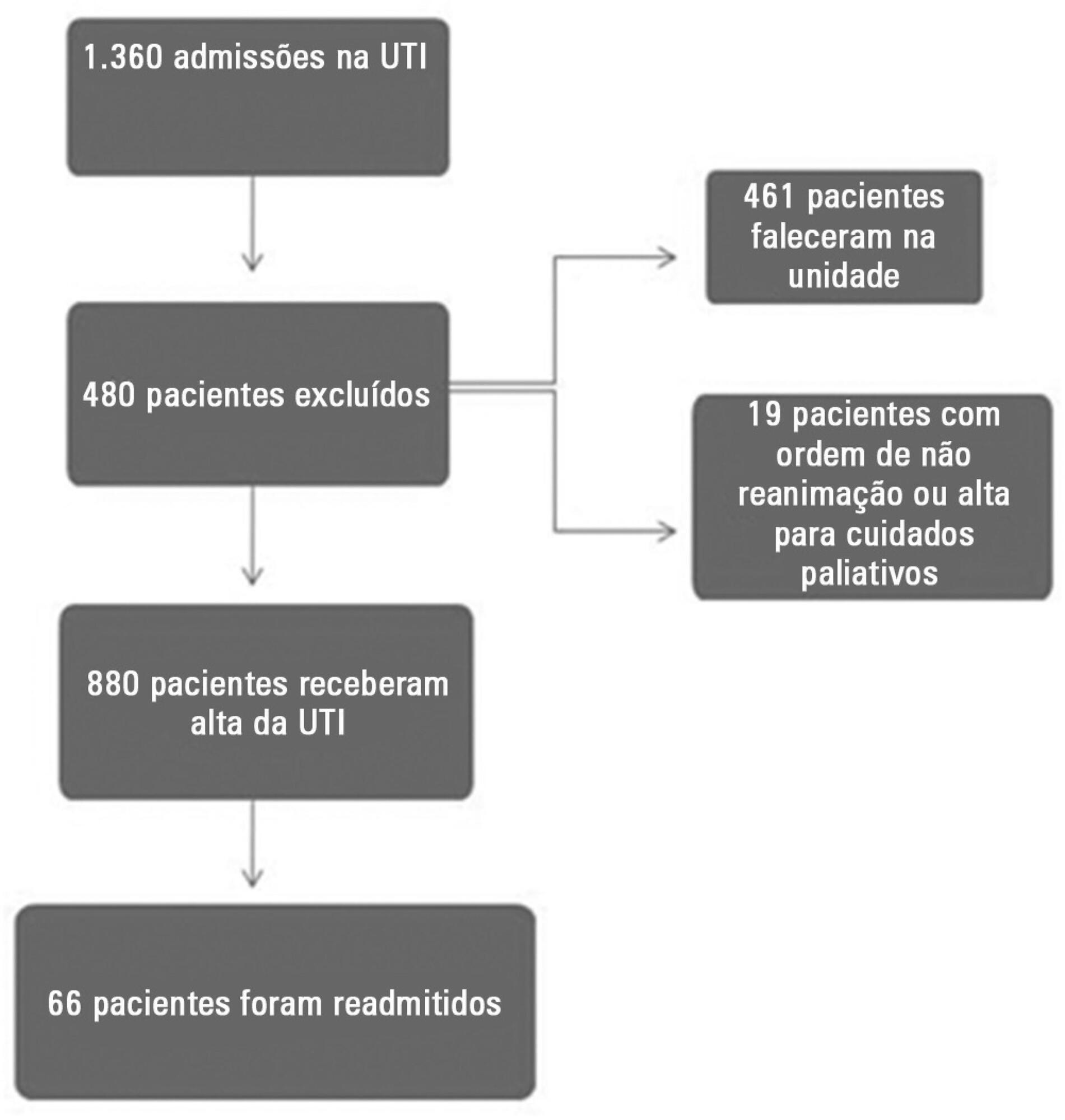
-
Review Article
Prognostic value of circulating DNA levels in critically ill and trauma patients
Rev Bras Ter Intensiva. 2014;26(3):305-312
Abstract
Review ArticlePrognostic value of circulating DNA levels in critically ill and trauma patients
Rev Bras Ter Intensiva. 2014;26(3):305-312
DOI 10.5935/0103-507X.20140043
Views0See moreThe number of studies investigating circulating nucleic acids as potential biomarkers has increased in recent years. The detection of such biomarkers is a minimally invasive alternative for the diagnosis and prognosis of various clinical conditions. The value of circulating DNA levels as a predictive biomarker has been demonstrated in patients suffering from numerous acute pathologies that have a high risk of intensive care needs and in-hospital deaths. The mechanism by which circulating DNA levels increase in patients with these conditions remains unclear. In this review, we focused on the potential use of this biomarker for prognosis prediction in critically ill and trauma patients. The literature review was performed by searching MedLine using PubMed in the English language.
-
Original Articles
Lack of association between interleukin-1 gene polymorphism and prognosis in severe traumatic brain injury patients
Rev Bras Ter Intensiva. 2009;21(4):343-348
Abstract
Original ArticlesLack of association between interleukin-1 gene polymorphism and prognosis in severe traumatic brain injury patients
Rev Bras Ter Intensiva. 2009;21(4):343-348
DOI 10.1590/S0103-507X2009000400002
Views0See moreOBJECTIVE: Traumatic brain injury is the major cause of death among individuals between 1-45 years-old. The outcome of traumatic brain injury may be related to brain susceptibility to the injury and genetic factors. Genes that may affect traumatic brain injury outcome are being investigated, however there is still few data concerning the association between genetic polymorphisms and traumatic brain injury outcome. The interleukin-1 beta gene (IL-1B) is one of the most studied genes, because levels of this cytokine are raised after traumatic brain injury and this can affect worsen the prognosis. The aim of this study was to test whether the -31C/T polymorphism, located at the promoter region of the IL-1B gene, is associated with primary short-term outcome (death or intensive care unit discharge) in severe traumatic brain injury patients. METHODS: Were studied 69 patients admitted with severe traumatic brain injury in three hospitals of the metropolitan region of Porto Alegre. The polymorphism was analyzed by polymerase chain reaction, followed by restriction digestion. RESULTS: Severe traumatic brain injury was associated with a 45% mortality rate. No significant differences were observed in the allele and genotype frequencies between patients stratified by traumatic brain injury outcome. CONCLUSION: Our findings suggest that -31C/T IL-1B gene polymorphism have no significant impact on the outcome of patients after acute severe traumatic brain injury.
-
Care of the potential organ donor
Rev Bras Ter Intensiva. 2007;19(2):197-204
Abstract
Care of the potential organ donor
Rev Bras Ter Intensiva. 2007;19(2):197-204
DOI 10.1590/S0103-507X2007000200010
Views0See moreBACKGROUND AND OBJECTIVES: Organ transplantation has long been considered the treatment of choice for many end-stage organ diseases. As soon as transplantation turned to be a viable therapy, organ shortage became the major limitation for the procedures. Nowadays, there is an increasing imbalance between organ supply and demand. Apparently, the most promising way to increase organ supply is optimizing the care for the brain death organ donor. The objective of this manuscript was to review the pathophysiological aspects and therapeutic strategies for the optimized care of the potential organ donor. CONTENTS: Brain death causes a massive catecholamine release, inducing a variety of deleterious effects that can threat organ perfusion. Studies have documented a sudden decrease in cortisol, insulin, thyroid and pituitary hormones. In this scenario of hemodynamic and metabolic instability, a special attention to the multiple organ donor support is required. CONCLUSIONS: An extensive knowledge of the complex brain death pathophysiology is extremely important for the implementation of rational aggressive management protocols of the potential organ donor, aiming to increase the number of harvested organs and the number of organs harvested per donor.
Search
Search in:
KEY WORDS
Case reports Child Coronavirus infections COVID-19 Critical care Critical illness Extracorporeal membrane oxygenation Infant, newborn Intensive care Intensive care units Intensive care units, pediatric mechanical ventilation Mortality Physical therapy modalities Prognosis Respiration, artificial Respiratory insufficiency risk factors SARS-CoV-2 Sepsis




