Abstract
Rev Bras Ter Intensiva. 2009;21(1):1-8
DOI 10.1590/S0103-507X2009000100001
OBJECTIVE: The elderly constitute a population with their own features and frequent admissions in intensive care units. This study has the objective to evaluate the ability to predict the survival of these patients through the APACHE II, UNICAMP II, SAPS II and SAPS 3 indexes, global and Central America/South equations. METHODS: Elderly patients admitted from 01/01/2006 to 12/3/2006, defined as age > 60 years, were included in this study. Those who were readmitted were excluded. The rate of lethality standardized, calibration and discrimination for each index in the remaining patients were analysed. The outcome were death or hospital discharge. RESULTS: Three hundred eighty six elderly patients were included in this study, being 36 excluded by readmission, remaining 350 for analysis. The rate of lethality standardized came near to the unit in all indexes, except the SAPS II (TLP=1.5455) which underestimated the lethality. The calibration, via Hosmer-Lemeshow tests was inadequate (p < 0.05), except for the UNICAMP II (p > 0.5). On the calibration curve, the models have distanced themselves from the pattern line. All of them presented an excellent discrimination via receiver operating characteristics curves (> 0.8). CONCLUSIONS: In the studied population, the models presented an excellent discrimination and inadequate calibration. SAPS II underestimated the lethality.
Abstract
Rev Bras Ter Intensiva. 2009;21(1):9-17
DOI 10.1590/S0103-507X2009000100002
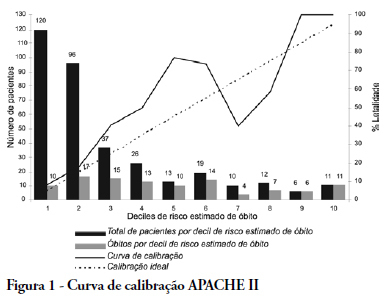
OBJECTIVES: The objective of this study was to evaluate variables related to intra hospital mortality at 28 days, of aged persons with severe sepsis and septic shock in a clinical ICU. METHODS: One hundred and fifty-two patients aged > 65 years with severe sepsis and septic shock were followed for 28 days and the variables were collected on days 1, 3, 5, 7, 14 and 28 of stay. To compare categorical variables the Chi-square test was used and the Mann-Whitney or t test for continuous variables. All tests were double-tailed, alpha error of 0.05. RESULTS: Mean age was 82.0 ± 9.0 years and 64.5% were female. Mortality was of 47.4%. Related to death were the following: Acute Physiological and Chronic Heath Evaluation II score (p < 0.001), Sequential Organ Failure Assessment score on days 1, 3, 5, 7 (p < 0.001), length of stay in intensive care (p < 0.001), number of organ failures (p < 0.001), high serum lactate on day 3 (p = 0.05), positive troponin I (p < 0.01), echocardiographic variables (systolic diameter p = 0.005; diastolic diameter p = 0.05; shortening fraction p = 0.02), previous renal disease (p = 0.03), shock (p < 0.001), mechanical ventilation (p < 0.001) and Lawton scale (p = 0.04). CONCLUSIONS: Shock, elevated lactate, organ failure, especially respiratory were more prevalent in non-survivors. Heart dysfunction detected by echocardiographic variables and positive troponin I may play an important role in the mortality of aged patients with sepsis.
Abstract
Rev Bras Ter Intensiva. 2009;21(1):18-24
DOI 10.1590/S0103-507X2009000100003
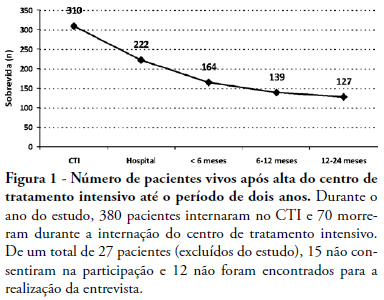
OBJECTIVES: To evaluate mortality and long term quality of life of patients who were discharged from the intensive care unit. METHODS: A prospective cohort, in which all the admitted patients in a intensive care unit (ICU) during 6 months were evaluated and interviewed by telephone after two years of discharge, aiming the completion of two quality of live scales: Karnofsky scale and activities of daily living (ADL) scale. RESULTS: From a total of 380 patients, 100 (26.5%) individuals were alive at the time of interview, 94% living in their homes and 90% without the need for family or specialized care. There was a significant reduction in quality of life of the survivors (Karnofsky pre-ICU = 90±10 vs. Karnofsky after two years = 79±11; p<0.05), although maintaining their functional capacity (ADL pre-ICU = 28±4 vs. ADL after two years = 25±8; p=0.09). This drop in the quality of life occurred mainly to patients who suffered stroke (Karnofsky pre-ICU = 88±7 vs. Karnofsky after two years = 60±15; p<0. 01). CONCLUSION: These preliminary data suggest that the performance of patients after two years of the intensive care discharge is preserved, since they retain the ability to perform self care, except in those with brain damage which shows an inferior quality of life.
Abstract
Rev Bras Ter Intensiva. 2009;21(1):25-31
DOI 10.1590/S0103-507X2009000100004
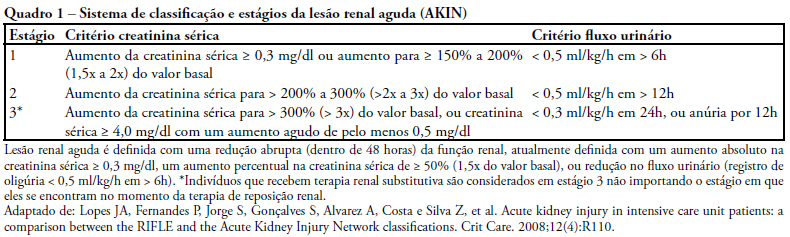
OBJECTIVES: To identify the frequency of the Acute Kidney Injury and to compare the application of the AKIN classification with the separate use of the serum creatinine in the postoperative period of cardiac surgery. METHODS: This study was prospectively developed in a teaching and specialized research hospital in cardiology of the public health system of the state of São Paulo. Forty-four patients submitted to the elective cardiac surgery since the immediate post-surgical period up to the 2nd post-surgical period were followed. RESULTS: It was possible to verify that from the forty-four patients, 75% were hypertensive, 27% were diabetic and mostly were male (64%), with an average age of 55+16 years old. It was observed that advanced age and the elevated body mass index shows a significant correlation to renal dysfunction (p<0, 05). According to the AKIN classification, the urinary flow criterion identified more renal dysfunction than creatinine criterion. It was verified that the renal dysfunction occurred more frequently in the postsurgery period and the majority (82%) from the 63,6% of the patients which were submitted to the revascularization of the myocardium surgery. CONCLUSION: The majority of patients (75%) evolved initially with renal dysfunction signaled it mainly by the urinary flow criterion from the AKIN classification, a higher number compared to the separated creatinine. This fact confirms that the serum creatinine association with the urinary flow has a higher discriminatory performance for the early identification of this syndrome comparatively with the routinely use of the isolated creatinine.

Abstract
Rev Bras Ter Intensiva. 2009;21(1):32-37
DOI 10.1590/S0103-507X2009000100005
OBJECTIVES: To know the needs and level of family members' satisfaction is an essential part of the care provided to critically ill patients in intensive care units. The objective of this study was to identify the level of family members' satisfaction in an intensive care unit. METHODS: A descriptive survey was carried out in the general adult intensive care unit of the Hospital Português (Salvador - BA) from November 2007 to January 2008. Jonhson's 14-question modified version of the Critical Care Family Needs Inventory was used to evaluate satisfaction of family members. RESULTS: Fifty three family members were included, mean age was 44 years and 68% were female. The median of family members satisfaction level was 11 (IQI = 9-13). Critical Care Family Need Inventory, questions with higher percentiles of satisfaction were those stating that family members felt that the patient was receiving the best possible care (96%) and that the information provided was honest (96%). The questions with lower percentiles of satisfaction were those stating that family members believed that someone in the intensive care unit had shown interest in their feelings (45%) and that a healthcare professional had explained how the intensive care unit equipment was used (41%). CONCLUSIONS: Most family members positively evaluated the intensive care unit professionals in the questions related to communication, attitude and patient care. However, there was a lower level of satisfaction in the questions related to the intensive care unit professionals' ability to comfort family members.
Abstract
Rev Bras Ter Intensiva. 2009;21(1):38-44
DOI 10.1590/S0103-507X2009000100006
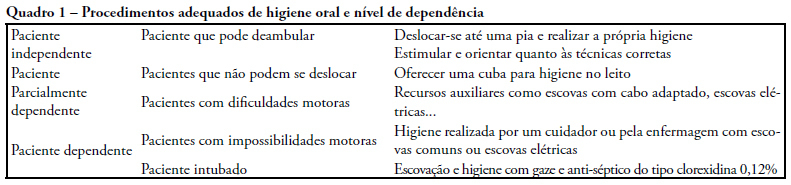
OBJECTIVES: A study was carried out, by means of a questionnaire for guided interviews seeking to establish a profile of perceptions and oral care given by ICU nursing team to patients in intensive care units. METHODS: The target population consisted of nursing practitioners divided in three education categories: nurses, nursing technicians and auxiliary nurses working at public and private hospital institutions providing for intensive care unit patients in Belem-PA. Dentistry experience has developed in this field reporting scientific findings and practical applications on prevention and reestablishment of the oral health in question. RESULTS: This survey disclosed results suggesting that oral hygiene care given to intensive care units patients is insufficient and inadequate requiring changes be made in the care now provided in the nosocomial environment by the nursing team. CONCLUSION: Presence of a dentist, knowledge of preventive dentistry, dissemination and use of oral hygiene specific resources are means suggested in an attempt to resolve difficulties found in oral health maintenance and treatment of oral diseases that affect the general health of hospitalized individuals. Interdisciplinary action for these individuals is advocated to achieve a better quality of life by preventing or minimizing oral pathologies.
Abstract
Rev Bras Ter Intensiva. 2009;21(1):45-50
DOI 10.1590/S0103-507X2009000100007
OBJECTIVE: A randomized clinical trial is a prospective study that compares the effect and value of interventions in human beings, of one or more groups vs. a control group. The objective of this study was to evaluate the quality of published randomized clinical trials in Intensive care in Brazil. METHODS: All randomized clinical trials in intensive care found by manual search in Revista Brasileira de Terapia Intensiva from January 2001 to March 2008 were assessed to evaluate their description by the quality scale. Descriptive statistics and a 95 % confidence interval were used for the primary outcome. Our primary outcome was the randomized clinical trial quality. RESULTS: Our search found 185 original articles, of which 14 were randomized clinical trials. Only one original article (7.1%) showed good quality. There was no statistical significance between the collected data and the data shown in the hypothesis of this search. CONCLUSION: It can be concluded that in the sample of assessed articles 7% of the randomized clinical trials in intensive care published in a single intensive care journal in Brazil, present good methodological quality.

Abstract
Rev Bras Ter Intensiva. 2008;20(4):376-384
DOI 10.1590/S0103-507X2008000400010
OBJECTIVES: Due to the dramatic medical breakthroughs and an increasingly ageing population, the proportion of patients who are at risk of dying following surgery is increasing over time. The aim of this study was to evaluate the outcomes and the epidemiology of non-cardiac surgical patients admitted to the intensive care unit. METHODS: A multicenter, prospective, observational, cohort study was carried out in 21 intensive care units. A total of 885 adult surgical patients admitted to a participating intensive care unit from April to June 2006 were evaluated and 587 patients were enrolled. Exclusion criteria were trauma, cardiac, neurological, gynecologic, obstetric and palliative surgeries. The main outcome measures were postoperative complications and intensive care unit and 90-day mortality rates. RESULTS: Major and urgent surgeries were performed in 66.4% and 31.7% of the patients, respectively. The intensive care unit mortality rate was 15%, and 38% of the patients had postoperative complications. The most common complication was infection or sepsis (24.7%). Myocardial ischemia was diagnosed in only 1.9% of the patients. A total of 94 % of the patients who died after surgery had co-morbidities at the time of surgery (3.4 ± 2.2). Multiple organ failure was the main cause of death (53%). CONCLUSION: Sepsis is the predominant cause of morbidity in patients undergoing non-cardiac surgery. In this patient population, multiple organ failure prevailed as the most frequent cause of death in the hospital.