Abstract
Revista Brasileira de Terapia Intensiva. 2012;24(1):30-34
DOI 10.1590/S0103-507X2012000100005
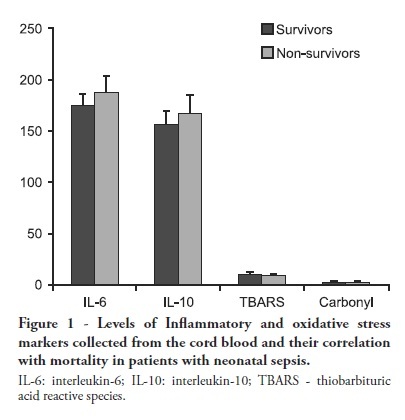
OBJECTIVES: Neonatal sepsis is a complex syndrome involving an uncontrolled systemic inflammatory response associated with an infection. It may result in the dysfunction or failure of one or more organs or even death. Given its high incidence in premature neonates, the identification of prognostic factors to optimize the early diagnosis and therapeutic interventions are highly desirable. This objective study determine the relationship between inflammatory markers and oxidative parameters as prognostic factors in early neonatal sepsis. METHODS: We conducted a prospective observational study by collecting data from 120 patients in the maternity unit of a university hospital. Preterm (<37 weeks of pregnancy) infants with at least one additional risk factor for neonatal sepsis were included. The levels of interleukin (IL)-6, IL-10, thiobarbituric acid reactive species (TBARS) and protein carbonyls and their association with sepsis severity were determined in the cord blood. RESULTS: Levels of IL-6 and TBARS, but not IL-10 and protein carbonyls, demonstrated a mild to moderate correlation with the SNAPPE-II severity score (r=0.435, p=0.02 and r = 0.385, p = 0.017, respectively). No correlations were found between these markers and mortality. CONCLUSION: TBARS and IL-6 have a mild to moderate correlation with SNAPPE-II, but none of the studied markers were able to predict mortality in our sample.
Abstract
Revista Brasileira de Terapia Intensiva. 2011;23(4):492-498
DOI 10.1590/S0103-507X2011000400015
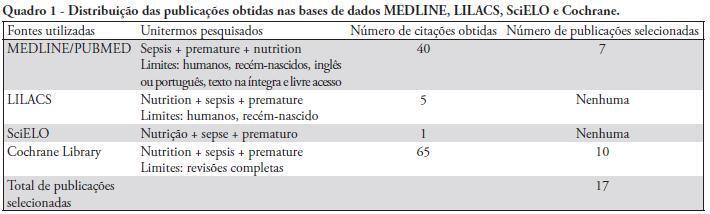
This article reviews the current understanding of enteral and parenteral nutrition therapy in preterm infants, with an emphasis on very low birth weight babies. The protective effects of nutrition therapy against neonatal sepsis and necrotizing enterocolitis are discussed. Different methods of feeding preterm infants are evaluated. Special attention is given to the problems of very low birth weight babies and the protective effects of nutrition to counteract complications, especially infection. The preferential use of breast milk for enteral nutrition, the management of protein and energy offers, the use of early and minimal enteral nutrition, the early introduction of parenteral nutrition (within the first 24 hours of life) and the use of immunonutrients that are appropriately supported by a sufficient number of studies can provide good adjuvant therapy guidelines to prevent neonatal sepsis and necrotizing enterocolitis. However, we conclude that additional multicenter, randomized controlled studies are necessary to clarify the protective role of nutrition in preterm infants. Appropriate nutrition is not only effective in treating and preventing infective complications, but it also promotes neurodevelopment and prevents future harmful consequences.
Abstract
Revista Brasileira de Terapia Intensiva. 2011;23(4):484-491
DOI 10.1590/S0103-507X2011000400014
Although tetanus is a preventable disease by vaccination, it continues to claim lives around the world. Whereas cases of accidental origin reflect insufficient population immunization, tetanus neonatorum reveals a double-nature fault-poor vaccination coverage of adults coupled with difficulties accessing appropriate prenatal care; this situation is aggravated by the extreme severity of tetanus in this age group in which the mortality rate can reach up to 80%. The early detection of tetanus in neonates is essential for immediately initiating the proper therapy. Therefore, although reaching an early diagnosis of tetanus is important, the most relevant aspect is related to the appropriate management and prophylaxis of this disease. Consequently, the aim of this article is to review neonatorum tetanus with an emphasis on its therapy and prevention.

Abstract
Revista Brasileira de Terapia Intensiva. 2011;23(3):335-340
DOI 10.1590/S0103-507X2011000300012
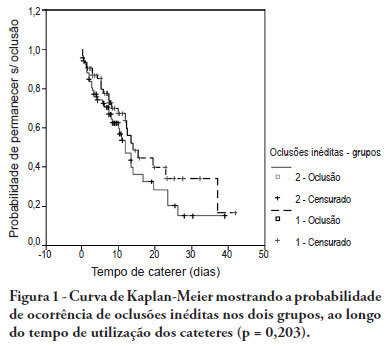
OBJECTIVE: To evaluate the effectiveness of intermittent 10 U/mL heparin flushes in reducing the occlusion of peripherally inserted central catheters in neonates. METHODS: In this randomized, open-label, prospective, controlled study, neonates were allocated either to receive 0.5 mL flushes of heparin (Group 1: n = 64) or saline (Group 2: n = 69) every 4 hours. Actions were taken to restore patency by using negative pressure (3-way stopcock method) in cases of occlusion. RESULTS: A total of 133 neonates were included. No significant intergroup difference was observed in the number of new occlusions (26 in Group 1, or 31/1,000 catheter-days; 36 in Group 2, or 36/1,000 catheter-days; P = 0.19). In Group 1, 5 catheters had 9 recurrent obstructions after successful clearance maneuvers. In Group 2, 19 catheters had 40 relapses (P < 0.0001), showing heparin's protective role against recurrence of obstruction (Relative Risk = 0.36). However, heparin failed to prevent catheter withdrawal due to permanent occlusion (3 catheters in Group 1 and 8 in Group 2; P = 0.24). CONCLUSION: Intermittent heparin is not effective for preventing the occlusion of peripherally inserted central catheters in neonates but reduces relapses when clearance maneuvers were successful
Abstract
Revista Brasileira de Terapia Intensiva. 2011;23(3):327-334
DOI 10.1590/S0103-507X2011000300011
PURPOSE: To evaluate the effectiveness of a noise control program in the Neonatal Intensive Care Unit of the Hospital Universitário Santa Maria (NICU-HUSM) in Santa Maria, Rio Grande do Sul, Brazil. METHODS: NICU-HUSM professionals were initially contacted through informal interviews during the morning, afternoon and night shifts. Leaflets were delivered and posters were installed to raise awareness of the harmful effects of noise on neonates and professionals and to suggest behavioral changes to reduce noise levels. The suggestions included avoiding loud talking, careful handling of the incubator doors and keeping mobile phones on silent mode. One month later, questionnaires were used to assess behavioral changes since the first contact. RESULTS: Most of the professionals rated the NICU-HUSM noise level as moderate. Overall, 71.4% of the respondents acknowledged that their behaviors were noisy. The entire sample reported believing that the unit noise levels could be reduced by speaking lower, reacting more quickly to alarms and handling furniture more carefully. The NICU professionals reported adopting these behaviors. CONCLUSION: This noise control program was considered successful because the professionals became aware of the level of noise and adopted behavioral changes to avoid generating unnecessary noise.

Abstract
Revista Brasileira de Terapia Intensiva. 2011;23(2):228-237
DOI 10.1590/S0103-507X2011000200017
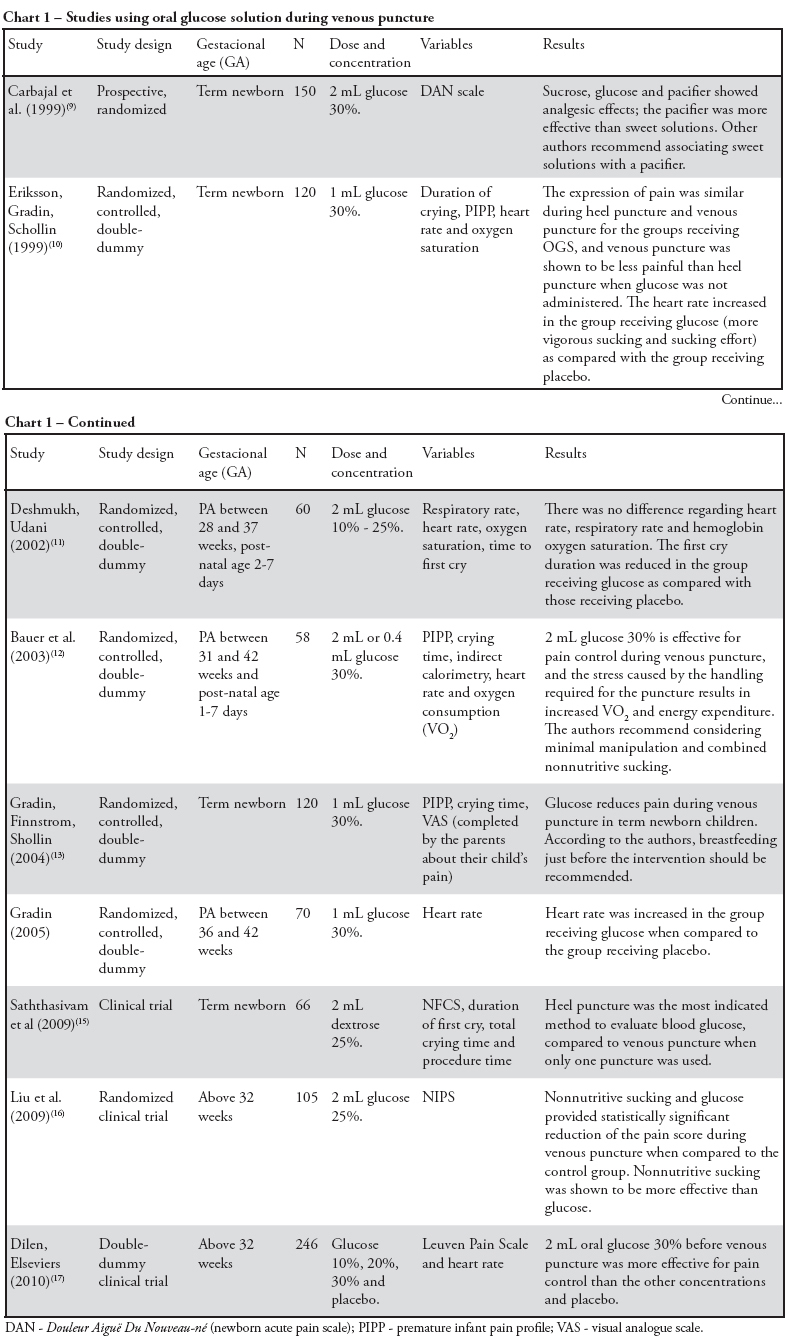
This article aims to review the main studies evaluating glucose as a therapeutic alternative during mildly to moderately painful procedures in neonatology, highlighting its benefits and limitations. During their stay in neonatal intensive care units, neonates are constantly subjected to a number of painful procedures without proper therapeutic management, although the medical literature emphatically recommends this type of management, highlighting the deleterious neurological consequences of pain. Most of these interventions are frequently necessary in neonatal intensive care units to maintain clinical stability in these children; the use of systemic analgesia, however, is not considered to be a good option. The administration of oral glucose solution is apparently effective and safe for pain control during procedures causing mild-to-moderate pain in neonate intensive care units, with rare adverse effects; however, its mode of action has not yet been described clearly in the literature. The administration of oral glucose solution is well described for use in venous punctures; it is apparently effective also for heel punctures, especially when associated with nonnutritive sucking, with most studies showing favorable results.
Abstract
Revista Brasileira de Terapia Intensiva. 2010;22(3):280-290
DOI 10.1590/S0103-507X2010000300011
The nonspecific presentation of neonatal sepsis and systemic inflammatory response syndrome preceding septic shock delay the early diagnosis of septic shock and increase its mortality rate. Early diagnosis involves suspecting septic shock in every newborn with tachycardia, respiratory distress, difficult feeding, altered tonus and skin coloration, tachypnea and reduced perfusion, specially in case of maternal peripartum infection, chorioamnionitis or long-term membranes rupture. This article aims to review current knowledge on neonatal period peculiarities, fetal circulation dynamics, and the pregnancy age variable. Newborn septic shock is not just a small adult shock. In the newborn, the septic shock is predominantly cold and characterized by reduced cardiac output and increased systemic vascular resistance (vasoconstriction). Time is fundamental for septic shock reversion. The indexed-databases literature review provides subside for the newborn management.

Abstract
Revista Brasileira de Terapia Intensiva. 2009;21(2):183-189
DOI 10.1590/S0103-507X2009000200011
OBJECTIVES: This research aimed to evaluate the repercussions of specific chest physiotherapy procedures in mean airway resistance and in dynamic compliance in preterm infants in mechanical ventilation. METHODS: Eighteen preterm infants in conventional mechanical ventilation were submitted to one session of chest physiotherapy (manual chest compression during expiration + intermittent aspiration of intratracheal cannula). Mean airway resistance and dynamic compliance measurements were taken prior to, 10, 40 and 70 minutes after intervention using a pneumotachograph with graphic display (Newport Navigator GM-250®), coupled to a flow transducer (Varfley-Bicore®). For analysis of results the infants were divided into 2 groups; less than 5 days (group mechanical ventilation <5) and 5 days or more (group mechanical ventilation >5) on mechanical ventilation. Values were analyzed by Friedman Test, with Dunn's Multiple Comparisons Test (p<0,05 significant). RESULTS: In group mechanical ventilation <5 a significant reduction of mean airway resistance was observed at the 10th minute after intervention (p<0,05). There were no significant alterations in dynamic compliance. The group mechanical ventilation >5 mean airway resistance had a significant reduction at the 10th (p<0,001), 40th (p<0,05) and 70th (p<0,05) minute after intervention. The dynamic compliance improved significantly only at the 10th minute (p<0,05). CONCLUSIONS: The airway clearance techniques used in preterm neonates under conventional mechanical ventilation >5 improved mean airway resistance and dynamic compliance, with best results for the mean airway resistance.