You searched for:"Sydney Agareno"
We found (7) results for your search.-
Original Articles Rev Bras Ter Intensiva. 2010;22(1):27-32
Abstract
Original ArticlesRev Bras Ter Intensiva. 2010;22(1):27-32
DOI 10.1590/S0103-507X2010000100006
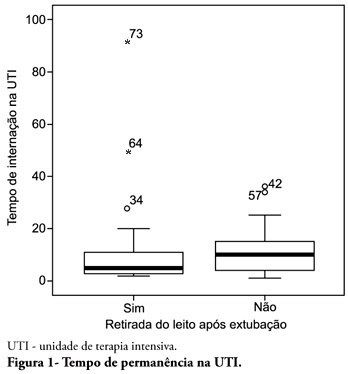
Views0See moreOBJECTIVE: To describe the withdrawal of the bed frequency in mechanic ventilation patients and its impact on mortality and length of stay in the intensive care unit. METHODS: This was a retrospective cohort study in mechanical ventilation patients. Clinical and epidemiological variables, withdrawal of bed related motor therapy, intensive care unit length of stay and mortality were evaluated. RESULTS: We studied 91 patients, mean age of 62.5± 18.8 years, predominantly female (52%) and mean intensive care unit length of stay of 07 days (95% CI, 8-13 days). Considering the withdrawal of the bed or not, no difference was observed between groups regarding length of stay in intensive care unit. Patients who were withdrawn of bed had a lower clinical severity. Their mortality rate was 29.7%. The not withdrawn of bed group had higher both actual and expected mortality. CONCLUSIONS: Patients withdrawn of bed following mechanical ventilation discontinuation showed lower mortality. It is suggested that early intensive care unit mobilization and withdrawal of bed should be stimulated.
-
Consenso Brasileiro de Monitorização e Suporte Hemodinâmico
Part II: basic hemodynamic monitoring and the use of pulmonary artery catheter
Rev Bras Ter Intensiva. 2006;18(1):63-77
Abstract
Consenso Brasileiro de Monitorização e Suporte HemodinâmicoPart II: basic hemodynamic monitoring and the use of pulmonary artery catheter
Rev Bras Ter Intensiva. 2006;18(1):63-77
DOI 10.1590/S0103-507X2006000100012
Views1See moreBACKGROUND AND OBJECTIVES: Monitoring of vital functions is one of the most important tools in the management of critically ill patients. Nowadays is possible to detect and analyze a great deal of physiologic data using a lot of invasive and non-invasive methods. The intensivist must be able to select and carry out the most appropriate monitoring technique according to the patient requirements and taking into account the benefit/risk ratio. Despite the fast development of non invasive monitoring techniques, invasive hemodynamic monitoring using Pulmonary Artery Catheter still is one of the basic procedures in Critical Care. The aim was to define recommendations about clinical utility of basic hemodynamic monitoring methods and the Use of Pulmonary Artery Catheter. METHODS: Modified Delphi methodology was used to create and quantify the consensus between the participants. AMIB indicated a coordinator who invited more six experts in the area of monitoring and hemodynamic support to constitute the Consensus Advisory Board. Twenty-five physicians and nurses selected from different regions of the country completed the expert panel, which reviewed the pertinent bibliography listed at the MEDLINE in the period from 1996 to 2004. RESULTS: Recommendations were made based on 55 questions about the use of central venous pressure, invasive arterial pressure, pulmonary artery catheter and its indications in different settings. CONCLUSIONS: Evaluation of central venous pressure and invasive arterial pressure, besides variables obtained by the PAC allow the understanding of cardiovascular physiology that is of great value to the care of critically ill patients. However, the correct use of these tools is fundamental to achieve the benefits due to its use.
-
Consenso Brasileiro de Monitorização e Suporte Hemodinâmico
Brazilian consensus of monitoring and hemodynamic support – part III: alternative methods for cardiac output monitoring and volemia estimation
Rev Bras Ter Intensiva. 2006;18(1):78-85
Abstract
Consenso Brasileiro de Monitorização e Suporte HemodinâmicoBrazilian consensus of monitoring and hemodynamic support – part III: alternative methods for cardiac output monitoring and volemia estimation
Rev Bras Ter Intensiva. 2006;18(1):78-85
DOI 10.1590/S0103-507X2006000100013
Views0See moreBACKGROUND AND OBJECTIVES: Cardiac output and preload as absolute data do not offer helpful information about the hemodynamic of critically ill patients. However, monitoring the response of these variables to volume challenge or inotropic drugs is a very useful tool in the critical care setting, particularly for patients with signs of tissue hypoperfusion. Although PAC remains the ” gold standard” to measure cardiac output and preload, new and alternative technologies were developed to evaluate these hemodynamic variables. METHODS: Modified Delphi methodology was used to create and quantify the consensus between the participants. AMIB indicated a coordinator who invited more six experts in the area of monitoring and hemodynamic support to constitute the Consensus Advisory Board. Twenty three physician and two nurses selected from different regions of the country completed the expert panel, which reviewed the pertinent bibliography listed at the MEDLINE in the period from 1996 to 2004. RESULTS: Recommendations regarding the use of arterial pulse pressure variation during mechanical ventilation, continuous arterial pulse contour and lithium dilution cardiac output measurements, esophageal Doppler waveform, thoracic electrical bioimpedance, echocardiography and partial CO2 rebreathing for monitoring cardiac output and preload were created. CONCLUSIONS: The new and less invasive techniques for the measurement of cardiac output, preload or fluid responsiveness are accurate and may be an alternative to PAC in critically ill patients.
-
Intensive care medicine on medical undergraduation: student’s perspective
Rev Bras Ter Intensiva. 2007;19(4):456-462
Abstract
Intensive care medicine on medical undergraduation: student’s perspective
Rev Bras Ter Intensiva. 2007;19(4):456-462
DOI 10.1590/S0103-507X2007000400009
Views1See moreBACKGROUND AND OBJECTIVES: There are deficiencies on Intensive Medicine (IM) teaching in most of medical undergraduate schools. Those deficiencies may imply damages on their clinical competence. The objective of this study was to analyze current status of IM teaching and the medical undergraduate student interest in this speciality. METHODS: A cross-sectional study was performed in 2005. We applied a self-reported questionnaire to enrolled students between the sixth and the last semesters of two medical schools from Salvador-Bahia. The questionnaire contained questions about students’ interest and knowledge on IM, and opinion on IM teaching in their schools. RESULTS: We studied 570 students. Most of them (57.5%) had never realized a clerkship in intensive care unit (ICU) despite classifying its usefulness as high (mean of 4.14 ± 1.05, in a scale from 1 to 5). IM interest was high or very high in 53.7% of sample. Almost all students (97%) thought that IM topics should be more explored at their curriculum. Only 42.1% reported to be able to assess a critical care patient and this assurance was higher among students with previous clerkship in ICU (p < 0.001). Shock, cardiopulmonary resuscitation and sepsis were the most interesting topics in ICU for students' opinion. CONCLUSIONS: This study revealed a high interest in IM among medical undergraduate students. However, most had never practice a clerkship in ICU, demonstrating to be an important factor on undergraduate student performance faced to a critical care patient.
-
Artigos originais
Therapeutic limitation conducts in intensive care unit patients
Rev Bras Ter Intensiva. 2007;19(2):137-143
Abstract
Artigos originaisTherapeutic limitation conducts in intensive care unit patients
Rev Bras Ter Intensiva. 2007;19(2):137-143
DOI 10.1590/S0103-507X2007000200001
Views1See moreBACKGROUND AND OBJECTIVES: There is a growing tendency of looking for “dying with dignity”, rather than to prolong death and suffering of terminal patients on intensive care units (ICU). This study aims to evaluate medical practices that suggest therapeutic limitation (TL) in patients who died in an adult ICU. METHODS: A retrospective exploratory study was carried out to evaluate medical records of patients who died in a general adult ICU of a private hospital in Salvador-BA, between January and August of 2003, after at least 24 hours from the admission. The patients were classified, in relation to their deaths, in: “not responding to cardiopulmonary resuscitation”, “brain death”, “decision not to resuscitate” (DNR) and “withhold or withdrawal life-support measures”. RESULTS: Sixty seven patients were included, corresponding to 90.4% of the deaths occurred in this ICU during the referred period. The most of them (56.7%) were women and the patients’ mean age was 66.58 ± 17.86 years. Suggestive measures of TL were found in 59.7% of the patients, being “withhold of life-support measures” the most important (35.8%), followed by DNR (17.9%) and “withdrawal of life-support measures” (6%). The procedures most commonly omitted were use of vasoactive drugs and dialysis, while antibiotics were the most discontinued. The use of TL measures was more frequent in clinical patients. CONCLUSIONS: The results of the present study suggest high frequencies of medical conducts suggestive of TL in a general ICU in Northeast of Brazil. Therapeutic methods that could cause discomfort or suffering to the patients, as nutrition, sedation and analgesia, were rarely omitted or discontinued.
-
Artigos originais
Evaluation of medical students knowledge on brain death
Rev Bras Ter Intensiva. 2007;19(2):144-150
Abstract
Artigos originaisEvaluation of medical students knowledge on brain death
Rev Bras Ter Intensiva. 2007;19(2):144-150
DOI 10.1590/S0103-507X2007000200002
Views0See moreBACKGROUND AND OBJECTIVES: Because brain death (BD) is a new concept and little divulged, it’s not well accepted in general population, including doctors and Medical students. This study aims to evaluate the knowledge of a sample of Medical students on the Brazilian BD diagnosis protocol. METHODS: Descriptive cross-sectional survey that evaluated students from two medical schools in Salvador-BA. We used a questionnaire composed by questions about technical and ethical knowledge contained in the Federal Council of Medicine’s Resolution nº 1480/97 that establishes the criteria for BD diagnosis. RESULTS: We evaluated 115 Medical students. In 14 questions about the knowledge of BD criteria, the mean of right answers were 6.7 ± 1.8, which were higher among the students that had attended some presentation on BD. Most of the students (87.4%) knew how to identify the candidates to the BD diagnosis protocol. However, only 5.2% and 16.1% of the students answered right, respectively, the clinical and complementary tests that should be accomplished during the diagnosis protocol. Facing a no-donor patient with confirmed diagnosis of BD, 66.4% referred that artificial life support should be suspended. Only 15% of the interviewed students had already evaluated a patient with BD, being this percentage higher among those who had already frequented ICU (38.2% versus 5.1%; p < 0.001). CONCLUSIONS: The results of this study showed a limited knowledge of the evaluated students on BD diagnosis criteria, mainly in relation to the practical approach of this condition.
-
Artigos originais
Analysis of stressors for the patient in Intensive Care Unit
Rev Bras Ter Intensiva. 2007;19(1):53-59
Abstract
Artigos originaisAnalysis of stressors for the patient in Intensive Care Unit
Rev Bras Ter Intensiva. 2007;19(1):53-59
DOI 10.1590/S0103-507X2007000100007
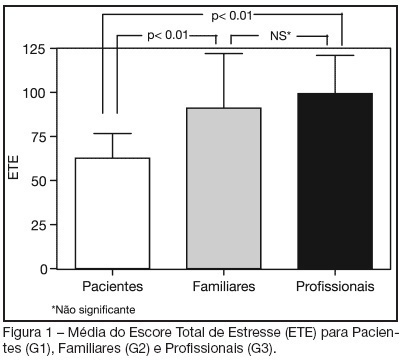
Views0See moreBACKGROUND AND OBJECTIVES: The hospital environment, especially in Intensive Care Units (ICU), due to the complexity of the assistance, as well as the physical structure, the noise, the equipments and people’s movement, is considered as stress generator for the patients. The aim of this study was to identify and stratify the stressful factors for patients at an ICU, in the perspective of the own patient, relatives and health care professionals. METHODS: A cross-sectional study was carried out between June and November 2004 in a general ICU of a private hospital. The sample was composed of three groups: patients (G1), relatives (G2) and a member of the ICU health care team responsible for the included patient (G3). In order to identify and stratify the stressful factors, we used the Intensive Care Unit Environmental Stressor Scale (ICUESS). For each individual, a total stress score (TSS) was calculated from the sum of all the answers of the scale. RESULTS: Thirty individuals were included in each group. The mean age of the three groups was: 57.30 ± 17.61 years for G1; 41.43 ± 12.19 for G2; and 40.82 ± 20.20 for G3. The mean TSS was 62.63 ± 14.01 for the patients; 91.10 ± 30.91 for the relatives; and 99.30 ± 21.60 for the health care professionals. The patients’ mean TSS was statistically lower than mean TSS of relatives and professionals (p < 0.01). The most stressful factors for the patients were: seeing family and friends only a few minutes a day; having tubes in their nose and/or mouth; and having no control on oneself. CONCLUSIONS: The perception of the main stressful factors was different among the three groups. The identification of these factors is important to the implementation of changes that can make the humanization of the ICU environment easier.
Search
Search in:
KEY WORDS
Case reports Child Coronavirus infections COVID-19 Critical care Critical illness Extracorporeal membrane oxygenation Infant, newborn Intensive care Intensive care units Intensive care units, pediatric mechanical ventilation Mortality Physical therapy modalities Prognosis Respiration, artificial Respiratory insufficiency risk factors SARS-CoV-2 Sepsis




