You searched for:"Cristiane Ritter"
We found (10) results for your search.-
Original Article
Biomarkers of neuropsychiatric dysfunction in intensive care unit survivors: a prospective cohort study
Crit Care Sci. 2023;35(2):147-155
Abstract
Original ArticleBiomarkers of neuropsychiatric dysfunction in intensive care unit survivors: a prospective cohort study
Crit Care Sci. 2023;35(2):147-155
DOI 10.5935/2965-2774.20230422-pt
Views8ABSTRACT
Objective:
To assess factors associated with long-term neuropsychiatric outcomes, including biomarkers measured after discharge from the intensive care unit.
Methods:
A prospective cohort study was performed with 65 intensive care unit survivors. The cognitive evaluation was performed through the Mini-Mental State Examination, the symptoms of anxiety and depression were evaluated using the Hospital Anxiety and Depression Scale, and posttraumatic stress disorder was evaluated using the Impact of Event Scale-6. Plasma levels of amyloid-beta (1-42) [Aβ (1-42)], Aβ (1-40), interleukin (IL)-10, IL-6, IL-33, IL-4, IL-5, tumor necrosis factor alpha, C-reactive protein, and brain-derived neurotrophic factor were measured at intensive care unit discharge.
Results:
Of the variables associated with intensive care, only delirium was independently related to the occurrence of long-term cognitive impairment. In addition, higher levels of IL-10 and IL-6 were associated with cognitive dysfunction. Only IL-6 was independently associated with depression. Mechanical ventilation, IL-33 levels, and C-reactive protein levels were independently associated with anxiety. No variables were independently associated with posttraumatic stress disorder.
Conclusion:
Cognitive dysfunction, as well as symptoms of depression, anxiety, and posttraumatic stress disorder, are present in patients who survive a critical illness, and some of these outcomes are associated with the levels of inflammatory biomarkers measured at discharge from the intensive care unit.
Keywords:AnxietyBiomarkersCognitive dysfunctionCritical care outcomesCritical illnessDeliriumDepressionIntensive care unitsPatient dischargeSee more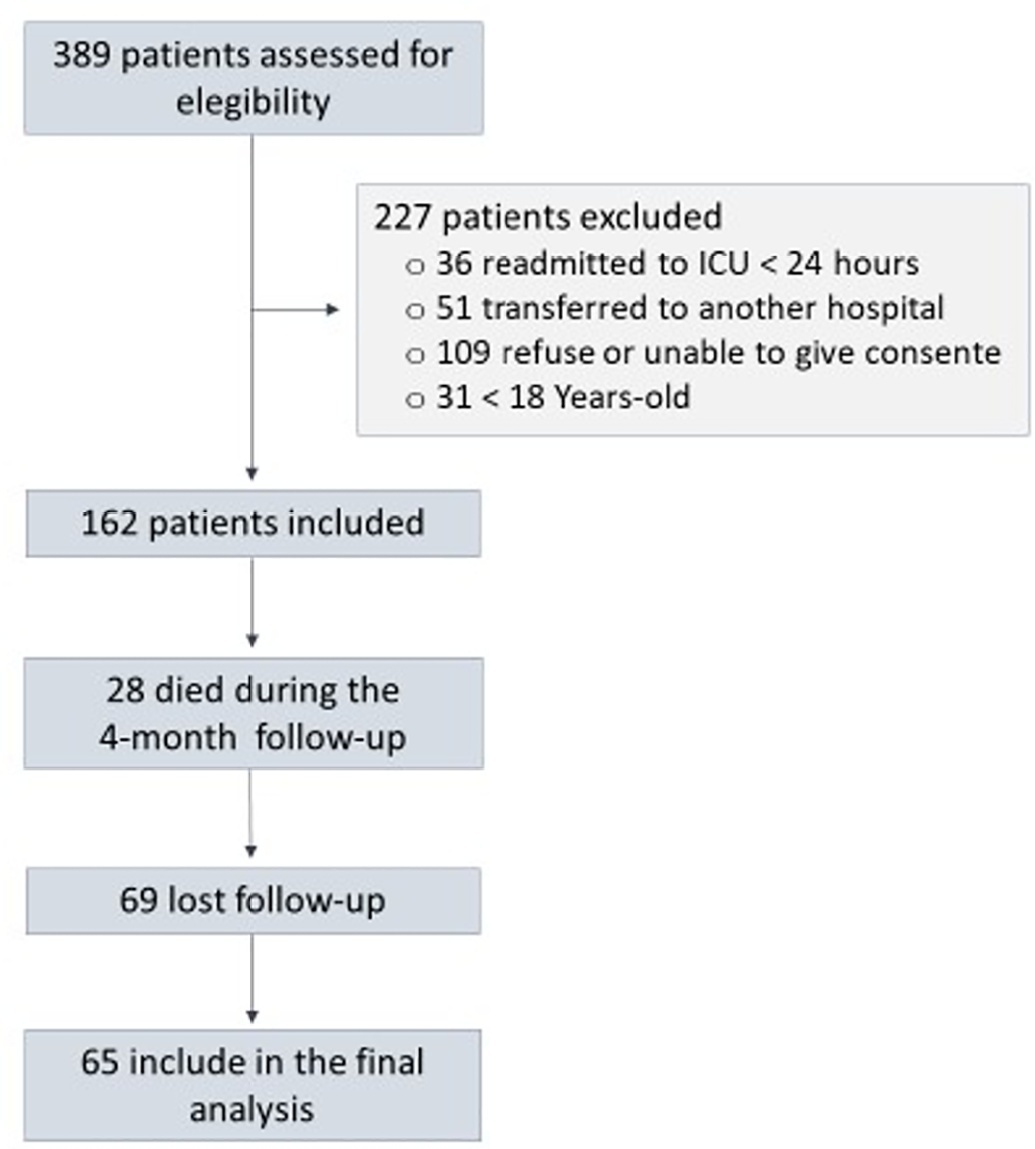
-
Original Article
Association of uteroglobin-related protein 1 with smoke inhalation injury severity
Rev Bras Ter Intensiva. 2021;33(2):276-281
Abstract
Original ArticleAssociation of uteroglobin-related protein 1 with smoke inhalation injury severity
Rev Bras Ter Intensiva. 2021;33(2):276-281
DOI 10.5935/0103-507X.20210035
Views1See moreABSTRACT
Objective:
To evaluate serum uteroglobin-related protein 1 expression early after smoke inhalation injuries and its association with the severity of inhalation injury in burned patients.
Methods:
Smoke or chemical inhalation injury is associated with morbidity and mortality. The consequences of inhalation result from an inflammatory response. Uteroglobin-related protein 1 is an anti-inflammatory protein and may improve lung inflammation. We hypothesized that uteroglobin-related protein 1 levels could reflect disease severity and predict outcome in patients with inhalation injury. Sixteen patients diagnosed with acute respiratory distress syndrome secondary to smoke inhalation injury were prospectively included in the study. Plasma was collected upon intensive care unit admission and within 24 hours of the inhalation injury. Bronchoscopies were carried out in all patients to assess the severity of inhalation injury within 72 hours. Uteroglobin-related protein 1 plasma levels were determined in duplicate with enzyme-linked immunosorbent assay.
Results:
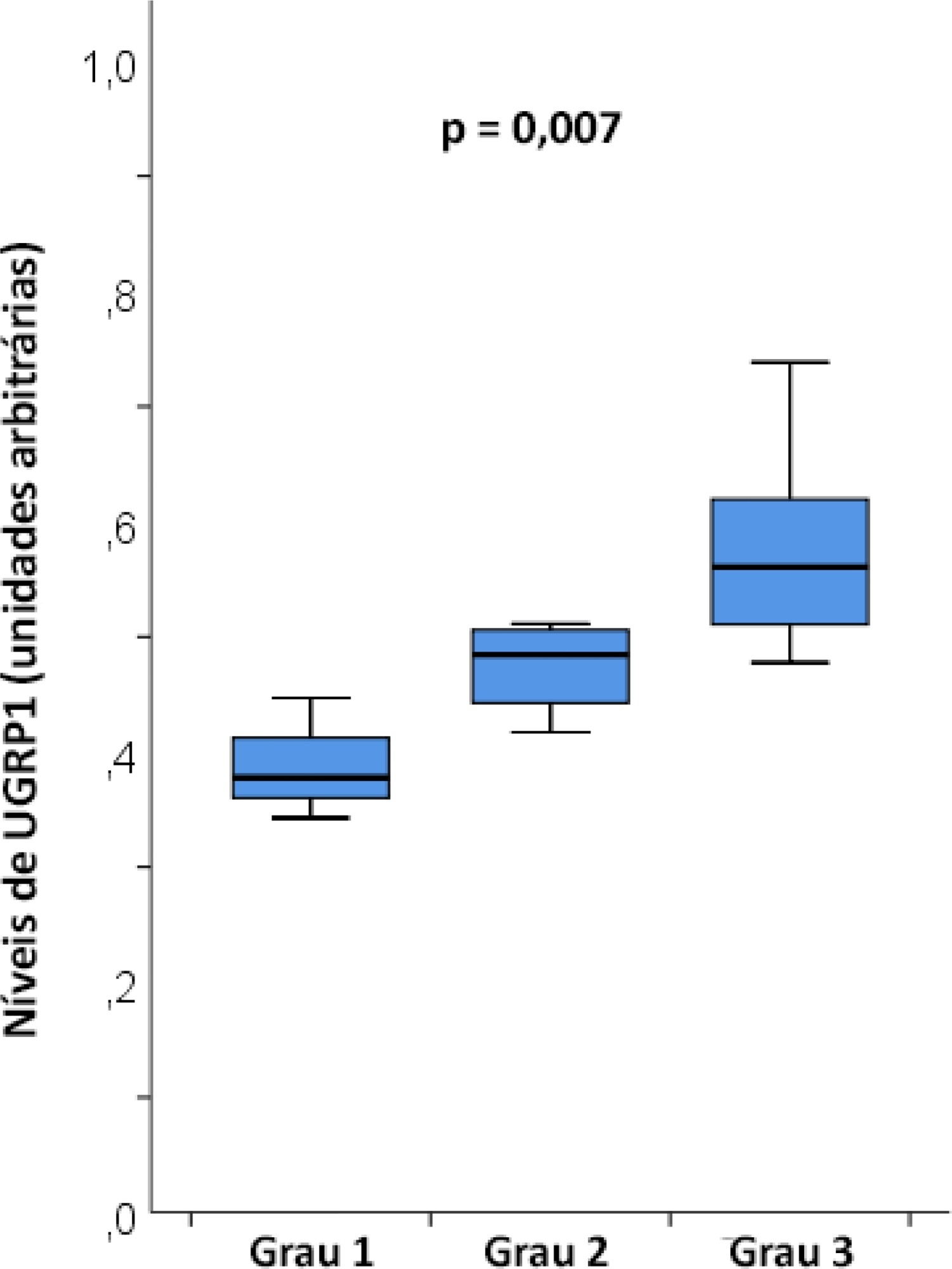
The mean age was 23 ± 5 years, and the inhalation injury distribution was as follows: three of grade 1, four of grade 2, and nine of grade 3. The level of uteroglobin-related protein 1 was related to inhalation severity (grade 1: 0.389 ± 0.053 arbitrary units versus grade 2: 0.474 ± 0.0423 arbitrary units versus grade 3: 0.580 ± 0.094 arbitrary units; p = 0.007).
Conclusion:
Plasma levels of uteroglobin-related protein 1 are associated with the degree of lung inhalation injury.
-
Original Article
Stratification to predict the response to antioxidant
Rev Bras Ter Intensiva. 2020;32(1):108-114
Abstract
Original ArticleStratification to predict the response to antioxidant
Rev Bras Ter Intensiva. 2020;32(1):108-114
DOI 10.5935/0103-507X.20200016
Views1See moreABSTRACT
Objective:
To examine the effectiveness of stratification to identify and target antioxidant therapy for animal models of lethal sepsis and in patients who develop sustained hypotension.
Methods:
Rats were subjected to sepsis induced by cecal ligation and puncture. Animals were divided into two groups: those with high and low plasma levels of interleukin-6. Following stratification, N-acetylcysteine plus deferoxamine or saline was administered to animals starting 3 and 12 hours after surgery. N-Acetylcysteine plus deferoxamine or placebo was administered within 12 hours of meeting the inclusion criteria in hypotensive patients.
Results:
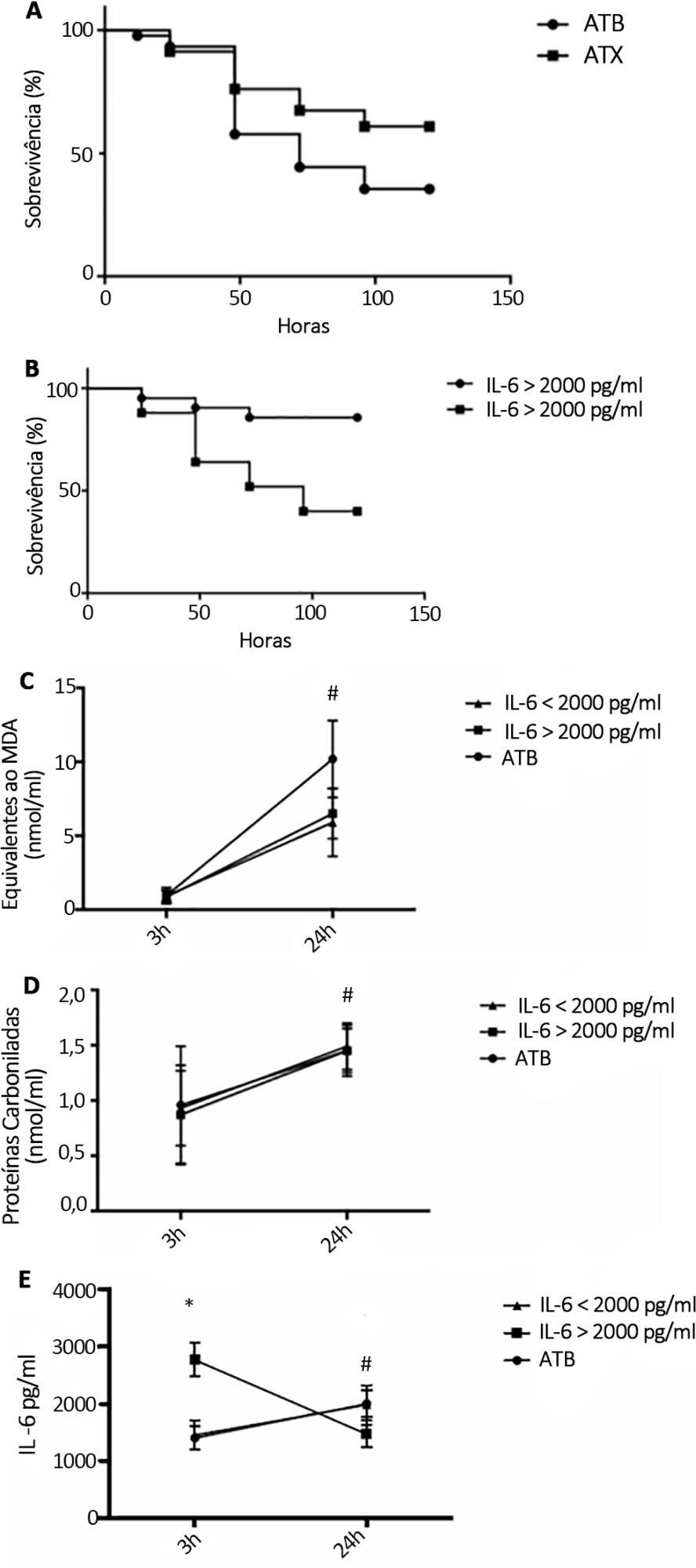
N-Acetylcysteine plus deferoxamine increased survival in the cecal ligation and puncture model when administered 3 and 12 hours after sepsis induction. When dividing animals that received antioxidants using plasma interleukin-6 levels, the protective effect was observed only in those animals with high IL-6 levels. The antioxidant effect of N-acetylcysteine + deferoxamine was similar in the two groups, but a significant decrease in plasma interleukin-6 levels was observed in the high-interleukin-6-level group. Compared with patients treated with antioxidants in the low-interleukin-6 subgroup, those in the high-interleukin-6 subgroup had a lower incidence of acute kidney injury but were not different in terms of acute kidney injury severity or intensive care unit mortality.
Conclusion:
Targeting antioxidant therapy to a high inflammatory phenotype would select a responsive population.
-
Original Articles
Baseline acetylcholinesterase activity and serotonin plasma levels are not associated with delirium in critically ill patients
Rev Bras Ter Intensiva. 2015;27(2):170-177
Abstract
Original ArticlesBaseline acetylcholinesterase activity and serotonin plasma levels are not associated with delirium in critically ill patients
Rev Bras Ter Intensiva. 2015;27(2):170-177
DOI 10.5935/0103-507X.20150029
Views0See moreABSTRACT
Objective:
The aim of this study was to investigate whether plasma serotonin levels or acetylcholinesterase activities determined upon intensive care unit admission could predict the occurrence of acute brain dysfunction in intensive care unit patients.
Methods:
A prospective cohort study was conducted with a sample of 77 non-consecutive patients observed between May 2009 and September 2010. Delirium was determined using the Confusion Assessment Method for the Intensive Care Unit tool, and the acetylcholinesterase and serotonin measurements were determined from blood samples collected up to a maximum of 24 h after the admission of the patient to the intensive care unit.
Results:
In the present study, 38 (49.6%) patients developed delirium during their intensive care unit stays. Neither serum acetylcholinesterase activity nor serotonin level was independently associated with delirium. No significant correlations of acetylcholinesterase activity or serotonin level with delirium/coma-free days were observed, but in the patients who developed delirium, there was a strong negative correlation between the acetylcholinesterase level and the number of delirium/coma-free days, indicating that higher acetylcholinesterase levels are associated with fewer days alive without delirium or coma. No associations were found between the biomarkers and mortality.
Conclusions:
Neither serum acetylcholinesterase activity nor serotonin level was associated with delirium or acute brain dysfunction in critically ill patients. Sepsis did not modify these relationships.
-
Original Article – Basic Research
N-acetylcysteine and deferrioxamine protects against acute renal failure induced by ischemia/reperfusion in rats
Rev Bras Ter Intensiva. 2012;24(3):219-223
Abstract
Original Article – Basic ResearchN-acetylcysteine and deferrioxamine protects against acute renal failure induced by ischemia/reperfusion in rats
Rev Bras Ter Intensiva. 2012;24(3):219-223
DOI 10.1590/S0103-507X2012000300003
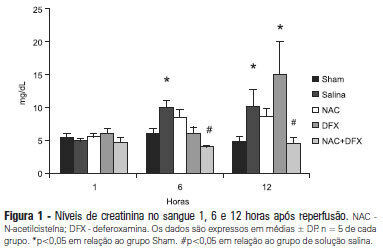
Views0See moreOBJECTIVE: Antioxidants are widely used in animal models to prevent renal injury after ischemia/reperfusion, but it is unknown if the benefits of antioxidants are additive. In this study, we aimed to investigate the protective effects of N-acetylcysteine plus deferoxamine in an animal model of kidney ischemia/reperfusion injury. METHODS: Bilateral kidney ischemia was mastintained for 45 minutes. N-acetylcysteine, deferoxamine or both were administered into the aorta above the renal arteries immediately prior to induction of ischemia. Five rats from each group were sacrificed 1, 6 or 12 hours after reperfusion for the determination of blood creatinine, kidney oxidative damage parameters and myeloperoxidase activity. RESULTS: The combination of N-acetylcysteine and deferoxamine, but not their isolated use, prevented the increase in creatinine after ischemia/reperfusion. This prevention was followed by a consistent decrease in myeloperoxidase activity and oxidative damage parameters both in the kidney cortex and medulla. CONCLUSION: Treatment with N-acetylcysteine and deferoxamine was superior to the isolated use of either compound in an animal model of kidney ischemia/reperfusion.
-
Editorial
Searching for the Holy Grail: where do we go with the current biomarkers for sepsis?
Rev Bras Ter Intensiva. 2012;24(2):117-118
Abstract
EditorialSearching for the Holy Grail: where do we go with the current biomarkers for sepsis?
Rev Bras Ter Intensiva. 2012;24(2):117-118
DOI 10.1590/S0103-507X2012000200004
Views0EDITORIAL Searching for the Holy Grail: where do we go with the current biomarkers for sepsis? […]See more -
Original Articles – Basic Research
Inflammatory and oxidative cord blood parameters as predictors of neonatal sepsis severity
Rev Bras Ter Intensiva. 2012;24(1):30-34
Abstract
Original Articles – Basic ResearchInflammatory and oxidative cord blood parameters as predictors of neonatal sepsis severity
Rev Bras Ter Intensiva. 2012;24(1):30-34
DOI 10.1590/S0103-507X2012000100005
Views0OBJECTIVES: Neonatal sepsis is a complex syndrome involving an uncontrolled systemic inflammatory response associated with an infection. It may result in the dysfunction or failure of one or more organs or even death. Given its high incidence in premature neonates, the identification of prognostic factors to optimize the early diagnosis and therapeutic interventions are highly desirable. This objective study determine the relationship between inflammatory markers and oxidative parameters as prognostic factors in early neonatal sepsis. METHODS: We conducted a prospective observational study by collecting data from 120 patients in the maternity unit of a university hospital. Preterm (<37 weeks of pregnancy) infants with at least one additional risk factor for neonatal sepsis were included. The levels of interleukin (IL)-6, IL-10, thiobarbituric acid reactive species (TBARS) and protein carbonyls and their association with sepsis severity were determined in the cord blood. RESULTS: Levels of IL-6 and TBARS, but not IL-10 and protein carbonyls, demonstrated a mild to moderate correlation with the SNAPPE-II severity score (r=0.435, p=0.02 and r = 0.385, p = 0.017, respectively). No correlations were found between these markers and mortality. CONCLUSION: TBARS and IL-6 have a mild to moderate correlation with SNAPPE-II, but none of the studied markers were able to predict mortality in our sample.
Keywords:Fetal bloodInfant, newbornIntensive care units, neonatalInterleukin-10Interleukin-6Oxidative stressSepsisSee more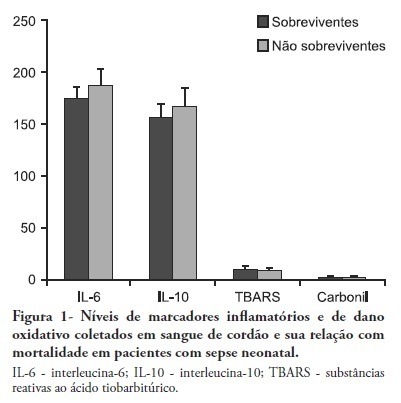
-
Original Articles – Clinical Research
The incidence of delirium in patients pretreated with statins who remain in an intensive care unit after cardiac surgery
Rev Bras Ter Intensiva. 2012;24(1):52-57
Abstract
Original Articles – Clinical ResearchThe incidence of delirium in patients pretreated with statins who remain in an intensive care unit after cardiac surgery
Rev Bras Ter Intensiva. 2012;24(1):52-57
DOI 10.1590/S0103-507X2012000100008
Views0OBJECTIVE: To determine the association between the preoperative administration of statins and postoperative delirium in a prospective cohort of patients undergoing cardiac surgery. METHODS: All adult patients who were admitted to the intensive care unit following cardiac surgery between January and June 2011 were included. Delirium was screened during the postoperative period using the Confusion Assessment Method for Intensive Care Unit (CAM-ICU) and Intensive Care Delirium Screening Checklist (ICDSC). RESULTS: A total of 169 patients underwent elective cardiac surgery, and 40.2% of the patients were treated preoperatively with statins. Delirium was identified using the CAM-ICU in 14.9% of patients not taking preoperative statins in comparison with 11.8% of the patients taking statins (p = 0.817). Using the ICDSC, delirium was identified in 18.8% of patients not taking statins in comparison with 10.3% of the patients taking statins (p = 0.191). CONCLUSION: The use of preoperative statins is not correlated with postoperative delirium in patients undergoing cardiac surgery.
Keywords:Cardiac surgeryDeliriumHydroxymethylglutaryl-CoA reductase inhibitorsIntensive care unitsPostoperative periodSee more
Search
Search in:
KEY WORDS
Case reports Child Coronavirus infections COVID-19 Critical care Critical illness Extracorporeal membrane oxygenation Infant, newborn Intensive care Intensive care units Intensive care units, pediatric mechanical ventilation Mortality Physical therapy modalities Prognosis Respiration, artificial Respiratory insufficiency risk factors SARS-CoV-2 Sepsis




