Abstract
Revista Brasileira de Terapia Intensiva. 2006;18(1):95-98
DOI 10.1590/S0103-507X2006000100015
BACKGROUND AND OBJECTIVES: Iatrogenic conditions was due of the medical, correctly intervention or not, justified or not, which harmful consequences to the patient. The cares in Intensive Care Medicine present substantial challenges with relation to the security of the patient. The objective of this article is to make one brief revision of literature on the iatrogenic in its concepts and basic terms and its taxes prevalence in Intensive Care Medicine. CONTENTS: Intensive Care Medicine supplies subsidies that improve the morbidity and mortality, but that also the significant risks of adverse events and serious errors associate. The Iatrogenic can be minimized with the adequate monitorization or can be friction as waited aggravation, idiopathic and if to perpetuate in the anonymity. CONCLUSIONS: It is basic to recognize the necessity of the constant learning and recycling and conscience of the susceptibilities to the error; in this context, the respect for the human being must guide the professional behavior.

Abstract
Revista Brasileira de Terapia Intensiva. 2006;18(2):196-199
DOI 10.1590/S0103-507X2006000200014
BACKGROUND AND OBJECTIVES: The hemodynamic support of sepsis is now formulated trying to insert terlipressin as salvage drug in catecholamine resistant shock, justifying a broad critical analysis. CONTENTS: The analysis included hemodynamic therapies with defined specific goals and new recommendations for fluid resuscitation, vasopressor therapy, and inotropic therapy of septic in adult and pediatric patients. CONCLUSIONS: Terlipressin appears as a new but controversial alternative for vasopressor therapy in sepsis.
Abstract
Revista Brasileira de Terapia Intensiva. 2006;18(2):190-195
DOI 10.1590/S0103-507X2006000200013
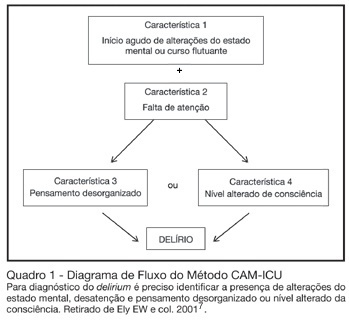
BACKGROUND AND OBJECTIVES: Delirium is a frequent finding in the critically ill patient. Although it is associated with increased morbidity and mortality, it is often not recognized by intensive care doctors. This review will address the main issues regarding delirium in critically ill patients. CONTENTS: Definition, incidence, mortality, risk factors, diagnosis, and treatment of delirium in the critically ill. CONCLUSIONS: Deliriumis defined as a disturbance of consciousness, attention, cognition and perception that occurs frequently in critically ill patients. It occurs in as many as 80% of mechanically ventilated ICU patients. Risk factors for delirium include acute systemic illnesses, older age, pre-existing cognitive impairment, sleep deprivation, and medications with anticholinergic activity. Although new assessment tools are available for rapidly and accurately measuring deliriumin critically ill patients, healthcare professionals still do not regularly monitor for this condition. In recent years, the emphasis in the approach to delirium has shifted to systematic screening and prevention. Haloperidol remains the standard treatment for delirium, but there is some evidence for the efficacy of risperidone.
Abstract
Revista Brasileira de Terapia Intensiva. 2006;18(2):186-189
DOI 10.1590/S0103-507X2006000200012
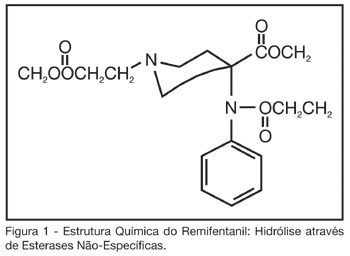
BACKGROUND AND OBJECTIVES: Critically ill patients frequently need to use sedative and analgesic drugs, as part of their treatment or during several procedures. It is a challenge for all intensive care providers to determine the best drug to be used for each patient, with less collateral effects. The objective of this study is to describe the background to give the use of remifentanil in intensive care clinical practice. CONTENTS: Remifentanil is a short acting opioid agonist little used in intensive care medicine. Several studies have been published, showing that remifentanil is a safe drug to be used for the sedation and analgesia for intensive care patients, still needing more information regardless to septic shock patients. CONCLUSIONS: Because remifentanil is a relatively new drug, it is not yet part of the routine drugs used for intensive care providers, although solid evidences of its safety and efficiency for critically ill patients.
Abstract
Revista Brasileira de Terapia Intensiva. 2006;18(2):177-185
DOI 10.1590/S0103-507X2006000200011
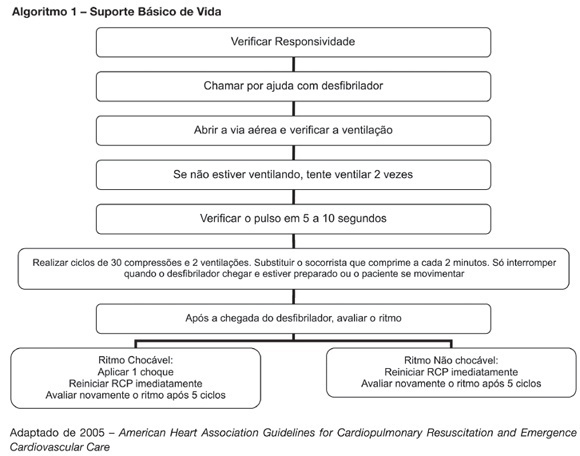
BACKGROUND AND OBJECTIVES: New resuscitation guidelines contain significant changes intended to improve resuscitation practice and survival from cardiac arrest. This article provides an overview of the key changes on resuscitation for healthcare provider. CONTENTS: There are several new recommendations on cardiopulmonary resuscitation (CPR), the major are intended to provide good circulation during cardiac arrest. The most important change is the emphasis on high-quality chest compressions with minimal interruptions. The universal 30:2 ratio is recommended to simplify training, to achieve optimal compression rates and to reduce the frequency of interruptions. Only one shock is delivered when indicated, followed immediately by CPR. This shock should be of 120-200J on a biphasic wave or 360J on a monophasic wave. Rescuers should not interrupt chest compressions to check rhythm until after about 5 cycles or approximately 2 minutes of CPR. After this period, if an organized rhythm is present, the healthcare provider should check for a pulse. There are several little changes about the drugs administrated during CPR according to the rhythm. Given the lack of documented effect of drug therapy in improving long-term outcome from cardiac arrest, the sequence for CPR deemphasizes drug administration and reemphasizes basic life support. CONCLUSIONS: The update on the new resuscitation guidelines is important to improve the quality of resuscitation and achieve better survival rates from our critical care patients.
Abstract
Revista Brasileira de Terapia Intensiva. 2007;19(3):369-373
DOI 10.1590/S0103-507X2007000300019
BACKGROUND AND OBJECTIVES: Magnesium sulfate has been shown to benefit asthmatic children and adults with poor responses to initial beta-agonist therapy and systemic corticoids in the emergency department. The aim of this study was to realize a no systematic review about the treatment of the acute asthma with intravenous and nebulized magnesium sulfate in the emergence. CONTENTS: The first investigations that demonstrate the benefit in the use of the magnesium sulfate in asthma date to 1938. The effects of magnesium sulfate may be mediated through its action as a calcium antagonist or through its function as a cofactor in enzyme systems involving ion flux across cell membranes. We realized a literature review using MedLine database of the last six years (2000 to 2006). Articles published in English were included by the crossing of keywords asthma and magnesium sulfate. CONCLUSIONS: The routine administration of intravenous and nebulized magnesium sulfate to severely ill patients with acute asthma presents in the emergence department is not recommended, however as an adjunct therapy brings some benefit.