Abstract
Rev Bras Ter Intensiva. 2009;21(1):45-50
DOI 10.1590/S0103-507X2009000100007
OBJECTIVE: A randomized clinical trial is a prospective study that compares the effect and value of interventions in human beings, of one or more groups vs. a control group. The objective of this study was to evaluate the quality of published randomized clinical trials in Intensive care in Brazil. METHODS: All randomized clinical trials in intensive care found by manual search in Revista Brasileira de Terapia Intensiva from January 2001 to March 2008 were assessed to evaluate their description by the quality scale. Descriptive statistics and a 95 % confidence interval were used for the primary outcome. Our primary outcome was the randomized clinical trial quality. RESULTS: Our search found 185 original articles, of which 14 were randomized clinical trials. Only one original article (7.1%) showed good quality. There was no statistical significance between the collected data and the data shown in the hypothesis of this search. CONCLUSION: It can be concluded that in the sample of assessed articles 7% of the randomized clinical trials in intensive care published in a single intensive care journal in Brazil, present good methodological quality.

Abstract
Rev Bras Ter Intensiva. 2009;21(1):80-88
DOI 10.1590/S0103-507X2009000100012
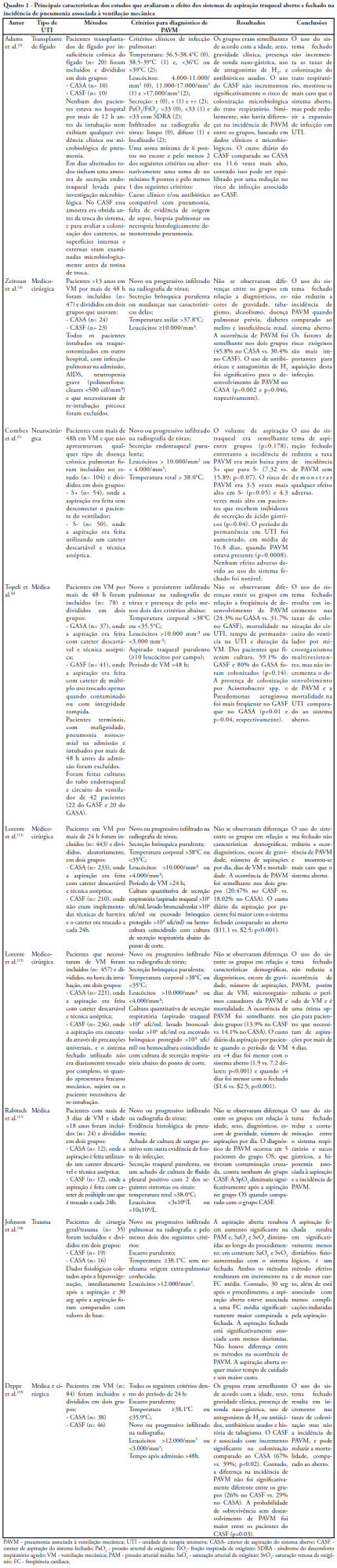
Pneumonia is the most common nosocominal infection in intensive care units and mechanical ventilation is a significant factor associated to its development. The objective of this study was to describe the impact of the open and closed tracheal suction systems on the incidence of ventilation-associated pneumonia. A search in the Pubmed database was performed to identify randomized controlled trials, published from 1990 to November 2008. Nine studies were included. Of the studies reviewed, seven did not disclose any significant advantages of using the closed system when compared to th e open, whereas two reported that use of the closed system increased colonization rates but not incidence of ventilation-associated pneumonia and one observed that use of the closed system did not increase colonization of the respiratory tract but reduced the spread of infection resulting in decreased sepsis rates. Only two studies found a reduction in the incidence of ventilation-associated pneumonia with use of the closed system, and one revealed a 3.5 times greater risk of developing this infection with the open system. Results suggest that the impact of the open and closed tracheal suction system is similar on development of ventilation-associated pneumonia, choice of the suction system should therefore be based on other parameters. While the closed system increases risk of colonization of the respiratory tract, but has the advantages of continuing mechanical ventilation and lessening hemodynamic impairment.
Abstract
Rev Bras Ter Intensiva. 2009;21(1):1-8
DOI 10.1590/S0103-507X2009000100001
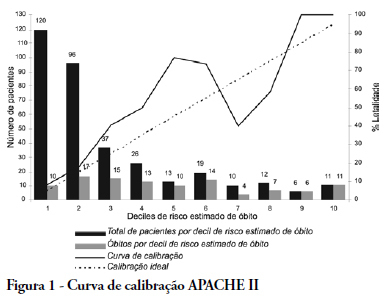
OBJECTIVE: The elderly constitute a population with their own features and frequent admissions in intensive care units. This study has the objective to evaluate the ability to predict the survival of these patients through the APACHE II, UNICAMP II, SAPS II and SAPS 3 indexes, global and Central America/South equations. METHODS: Elderly patients admitted from 01/01/2006 to 12/3/2006, defined as age > 60 years, were included in this study. Those who were readmitted were excluded. The rate of lethality standardized, calibration and discrimination for each index in the remaining patients were analysed. The outcome were death or hospital discharge. RESULTS: Three hundred eighty six elderly patients were included in this study, being 36 excluded by readmission, remaining 350 for analysis. The rate of lethality standardized came near to the unit in all indexes, except the SAPS II (TLP=1.5455) which underestimated the lethality. The calibration, via Hosmer-Lemeshow tests was inadequate (p < 0.05), except for the UNICAMP II (p > 0.5). On the calibration curve, the models have distanced themselves from the pattern line. All of them presented an excellent discrimination via receiver operating characteristics curves (> 0.8). CONCLUSIONS: In the studied population, the models presented an excellent discrimination and inadequate calibration. SAPS II underestimated the lethality.
Abstract
Rev Bras Ter Intensiva. 2009;21(1):18-24
DOI 10.1590/S0103-507X2009000100003
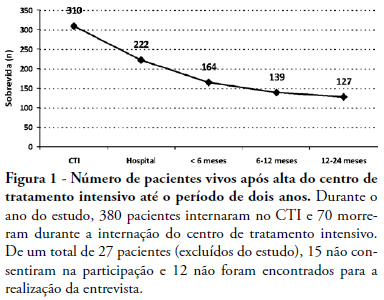
OBJECTIVES: To evaluate mortality and long term quality of life of patients who were discharged from the intensive care unit. METHODS: A prospective cohort, in which all the admitted patients in a intensive care unit (ICU) during 6 months were evaluated and interviewed by telephone after two years of discharge, aiming the completion of two quality of live scales: Karnofsky scale and activities of daily living (ADL) scale. RESULTS: From a total of 380 patients, 100 (26.5%) individuals were alive at the time of interview, 94% living in their homes and 90% without the need for family or specialized care. There was a significant reduction in quality of life of the survivors (Karnofsky pre-ICU = 90±10 vs. Karnofsky after two years = 79±11; p<0.05), although maintaining their functional capacity (ADL pre-ICU = 28±4 vs. ADL after two years = 25±8; p=0.09). This drop in the quality of life occurred mainly to patients who suffered stroke (Karnofsky pre-ICU = 88±7 vs. Karnofsky after two years = 60±15; p<0. 01). CONCLUSION: These preliminary data suggest that the performance of patients after two years of the intensive care discharge is preserved, since they retain the ability to perform self care, except in those with brain damage which shows an inferior quality of life.
Abstract
Rev Bras Ter Intensiva. 2009;21(1):32-37
DOI 10.1590/S0103-507X2009000100005
OBJECTIVES: To know the needs and level of family members' satisfaction is an essential part of the care provided to critically ill patients in intensive care units. The objective of this study was to identify the level of family members' satisfaction in an intensive care unit. METHODS: A descriptive survey was carried out in the general adult intensive care unit of the Hospital Português (Salvador - BA) from November 2007 to January 2008. Jonhson's 14-question modified version of the Critical Care Family Needs Inventory was used to evaluate satisfaction of family members. RESULTS: Fifty three family members were included, mean age was 44 years and 68% were female. The median of family members satisfaction level was 11 (IQI = 9-13). Critical Care Family Need Inventory, questions with higher percentiles of satisfaction were those stating that family members felt that the patient was receiving the best possible care (96%) and that the information provided was honest (96%). The questions with lower percentiles of satisfaction were those stating that family members believed that someone in the intensive care unit had shown interest in their feelings (45%) and that a healthcare professional had explained how the intensive care unit equipment was used (41%). CONCLUSIONS: Most family members positively evaluated the intensive care unit professionals in the questions related to communication, attitude and patient care. However, there was a lower level of satisfaction in the questions related to the intensive care unit professionals' ability to comfort family members.
Abstract
Rev Bras Ter Intensiva. 2009;21(1):38-44
DOI 10.1590/S0103-507X2009000100006
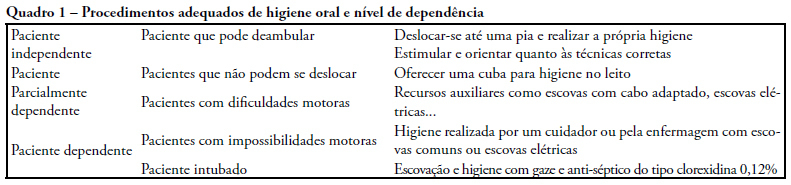
OBJECTIVES: A study was carried out, by means of a questionnaire for guided interviews seeking to establish a profile of perceptions and oral care given by ICU nursing team to patients in intensive care units. METHODS: The target population consisted of nursing practitioners divided in three education categories: nurses, nursing technicians and auxiliary nurses working at public and private hospital institutions providing for intensive care unit patients in Belem-PA. Dentistry experience has developed in this field reporting scientific findings and practical applications on prevention and reestablishment of the oral health in question. RESULTS: This survey disclosed results suggesting that oral hygiene care given to intensive care units patients is insufficient and inadequate requiring changes be made in the care now provided in the nosocomial environment by the nursing team. CONCLUSION: Presence of a dentist, knowledge of preventive dentistry, dissemination and use of oral hygiene specific resources are means suggested in an attempt to resolve difficulties found in oral health maintenance and treatment of oral diseases that affect the general health of hospitalized individuals. Interdisciplinary action for these individuals is advocated to achieve a better quality of life by preventing or minimizing oral pathologies.
Abstract
Rev Bras Ter Intensiva. 2008;20(4):344-348
DOI 10.1590/S0103-507X2008000400005
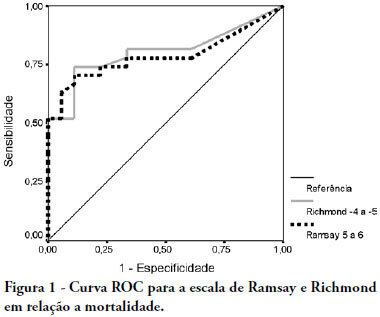
OBJECTIVE: The main purpose of this study was to compare performance of the Ramsay and Richmond sedation scores on mechanically ventilated critically ill patients, in a university-affiliated hospital. METHODS: This was a 4-month prospective study, which included a total of 45 patients mechanically ventilated, with at least 48 hours stay in the intensive care unit. Each patient was assessed daily for sedation mode, sedative and analgesic doses and sedation level using the Ramsay and Richmond scores. Statistical analysis was made using Student's t-test, Pearson's and Spearman's correlation, and constructing ROC-curves. RESULTS: A high general mortality of 60% was observed. The length of sedation and daily dose of medication did not correlate with mortality. Deep sedation (Ramsay > 4 or Richmond < -3) was positively correlated with probability of death with an AUC > 0.78. An adequate level of sedation (Ramsay 2 to 4 or Richmond 0 to -3) was sensitively correlated with probability of survival with an AUC > 0.80. A low level of sedation was observed in 63 days evaluated (8.64%), and no correlation was found between occurrence of agitation and unfavorable outcomes. Correlation between Ramsay and Richmond scores (Pearson's > 0.810 - p<0.0001) was good. CONCLUSION: In this study, Ramsay and Richmond sedation scores were similar for the assessment of deep, insufficient and adequate sedation. Both have good correlation with mortality in over sedated patients.
Abstract
Rev Bras Ter Intensiva. 2008;20(4):355-361
DOI 10.1590/S0103-507X2008000400007
OBJECTIVES: Students of Salvador - BA, Brazil were trained in critical care medicine by accomplishing extracurricular internships. This study aims to detect changes in attitude and interest of students who concluded these internships as well as the most frequent activities developed. METHODS: Descriptive cross-sectional survey conducted with students who did extracurricular internships in adult intensive care units during the second semester of 2006. A self-administered questionnaire was given using objective questions. RESULTS: We evaluated 49 students. Interest in becoming an intensivist was classified as high/very high by 32.7% before internship, after which 61.2% reported increased interest. Before internship, students on a 1 to 5 scale rated the importance of critical care medicine as 4.55 ± 0.70. After internship, 98% felt more confident to refer a patient to the intensive care unit, 95.9% to evaluate with supervision, patients admitted to intensive care units and 89.8% to attend patients in the emergency room. The most common procedures observed were: central venous access (100%), peripheral venous access (91.8%) and orotracheal intubation (91.8%). Topics ranked in terms of interest from 1 to 5 were: systemic inflammatory response syndrome/sepsis (4.82 ± 0.48), shock (4.81 ± 0.44) and cardiopulmonary resuscitation (4.77 ± 0.55). CONCLUSIONS: This study showed that internships in adult intensive care units of Salvador (BA), Brazil provided students with greater assurance to evaluate critical patients, increased their interest to follow an intensivist physician career and allowed contact with the main procedures and topics related to critical care medicine.