-
Editoriais
Trismus, opisthotonus and risus sardonicus: who remembers this disease?
Rev Bras Ter Intensiva. 2011;23(4):383-387
Abstract
EditoriaisTrismus, opisthotonus and risus sardonicus: who remembers this disease?
Rev Bras Ter Intensiva. 2011;23(4):383-387
-
Editoriais
End-of-life care in Brazilian ICUs is not just a legal issue: adequate training and knowledge are essential to improve care
Rev Bras Ter Intensiva. 2011;23(4):388-390
Abstract
EditoriaisEnd-of-life care in Brazilian ICUs is not just a legal issue: adequate training and knowledge are essential to improve care
Rev Bras Ter Intensiva. 2011;23(4):388-390
DOI 10.1590/S0103-507X2011000400002
Views0EDITORIAL End-of-life care in Brazilian ICUs is not just a legal issue: adequate training and knowledge are essential to improve care […]See more -
Editoriais
Adequate nutrition can improve the outcome of premature infants
Rev Bras Ter Intensiva. 2011;23(4):391-393
Abstract
EditoriaisAdequate nutrition can improve the outcome of premature infants
Rev Bras Ter Intensiva. 2011;23(4):391-393
-
Special Articles
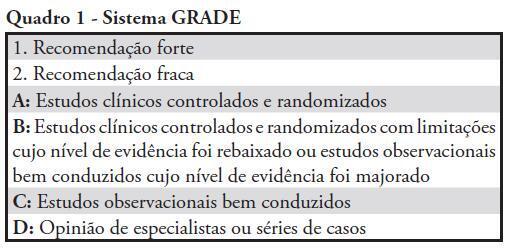
Guidelines for the management of accidental tetanus in adult patients
Rev Bras Ter Intensiva. 2011;23(4):394-409
Abstract
Special ArticlesGuidelines for the management of accidental tetanus in adult patients
Rev Bras Ter Intensiva. 2011;23(4):394-409
DOI 10.1590/S0103-507X2011000400004
Views0See moreAlthough tetanus can be prevented by appropriate immunization, accidental tetanus continues to occur frequently in underdeveloped and developing countries. Tetanus mortality rates remain high in these areas, and studies regarding the best therapy for tetanus are scarce. Because of the paucity of data on accidental tetanus and the clinical relevance of this condition, the Associação de Medicina Intensiva Brasileira (AMIB) organized a group of experts to develop these guidelines, which are based on the best available evidence for the management of tetanus in patients requiring admission to the intensive care unit. The guidelines discuss the management of tetanus patients in the intensive care unit, including the use of immunoglobulin therapy, antibiotic therapy, management of analgesics, sedation and neuromuscular blockade, management of dysautonomia and specific issues related to mechanical ventilation and physiotherapy in this population.

-
Special Articles
Guidelines for potential multiple organ donors (adult). Part III: organ-specific recommendations
Rev Bras Ter Intensiva. 2011;23(4):410-425
Abstract
Special ArticlesGuidelines for potential multiple organ donors (adult). Part III: organ-specific recommendations
Rev Bras Ter Intensiva. 2011;23(4):410-425
DOI 10.1590/S0103-507X2011000400005
Views0See moreBrain death (BD) alters the pathophysiology of patients and may damage the kidneys, the lungs, the heart and the liver. To obtain better quality transplant organs, intensive care physicians in charge of the maintenance of deceased donors should attentively monitor these organs. Careful hemodynamic, ventilatory and bronchial clearance management minimizes the loss of kidneys and lungs. The evaluation of cardiac function and morphology supports the transplant viability assessment of the heart. The monitoring of liver function, the management of the patient’s metabolic status and the evaluation of viral serology are fundamental for organ selection by the transplant teams and for the care of the transplant recipient
-
Original Articles – Basic Research
Association between organ dysfunction and cytokine concentrations during the early phases of septic shock
Rev Bras Ter Intensiva. 2011;23(4):426-433
Abstract
Original Articles – Basic ResearchAssociation between organ dysfunction and cytokine concentrations during the early phases of septic shock
Rev Bras Ter Intensiva. 2011;23(4):426-433
DOI 10.1590/S0103-507X2011000400006
Views1OBJECTIVE: To investigate the correlation of organ dysfunction and its progression with inflammatory response during the early phases of septic shock by assessing baseline cytokine concentrations. METHODS: This study included patients over 18 years old with septic shock within the first 48 hours after the onset of organ dysfunction. Interleukin 6 (IL-6), interleukin 8 (IL-8), interleukin 10 (IL-10) and C-reactive protein levels were assessed at inclusion and after 24 hours, and the differences between these values were calculated. The progression of organ dysfunction was assessed using the Sequential Organ Failure Assessment (SOFA) score upon admission and 24 hours later for a delta-SOFA determination and were categorized as either worsened or improved. The results were expressed as means + standard deviation or median (25-75% percentiles). Values with descriptive p values of 0.05 or less were considered significant. RESULTS: Overall, we included 41 patients with median SOFA scores of 8.0 (6.5-10.0) upon admission (T0) and 8.0 (6.0-10.0) 24 hours later (T1). Worsened, improved or unchanged SOFA scores were observed in 11 (Group 1), 17 (Group 2) and 13 (Group 3) patients, respectively. For Group 1, the baseline IL-6, IL-8 and IL-10 values were higher, and a significant increase of IL-8 levels was found after 24 hours. The change in the SOFA score after 24 hours was significantly, although weakly, correlated with baseline IL-6 and IL-8 concentrations. CONCLUSIONS: Higher baseline IL-6, IL-8 and IL-10 levels are associated with unfavorable organ dysfunction outcomes. Increased IL-8 levels within the first 24 hours are correlated with a worsening dysfunction.
Keywords:CytokinesetiologyMultiple organ failureShock, septicsystemic inflammatory response syndromeSee more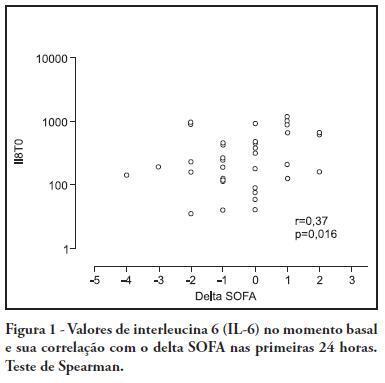
-
Original Articles – Clinical Research
Lethality and osteomuscular and cardiovascular complications in tetanus
Rev Bras Ter Intensiva. 2011;23(4):434-441
Abstract
Original Articles – Clinical ResearchLethality and osteomuscular and cardiovascular complications in tetanus
Rev Bras Ter Intensiva. 2011;23(4):434-441
DOI 10.1590/S0103-507X2011000400007
Views0See moreOBJECTIVE: Despite the decline in the incidence of tetanus, this disease is still neglected in the developing world and remains a major cause of morbidity and mortality. With improvements in intensive care, it is important to better understand the complications of this serious condition. We aim to evaluate 1) the lethality and osteomuscular and cardiovascular complications of patients with tetanus who are admitted to the intensive care unit (ICU) and 2) the risk factors associated with a poor prognosis. METHODS: This was a retrospective study that analyzed the medical records of all of the patients diagnosed with tetanus who were admitted to an infectious diseases ICU between January 2000 and December 2001. A standardized form that included demographic, clinical and laboratory data was completed. The clinical variables that were related to lethality and osteomuscular and cardiovascular complications were described. RESULTS: A total of 22 tetanus patients were admitted (81.8% male, mean age of 47.8 years).The tetanus infection was associated with professional activities in 54.5% of cases. The majority of patients (20 patients) presented with the generalized form of disease. Eighty-one percent of the patients had never received a tetanus vaccine or were unaware of their vaccine status. Following the injury, none had received appropriated passive prophylaxis, only two patients had received surgical debridement of wound and six patients received antibiotic therapy. Eleven patients (52.4%) experienced some cardiovascular complication. A pressure ulcer was the most frequent cardiovascular complication (38.1%), followed by arrhythmias (28.6%). Two of the patients developed bone fractures secondary to tetanus spasms, corresponding to 9.6% of sample. The tetanus lethality rate was 9.1%. Higher APACHE II severity scores and very severe status based on the Veronesi tetanus classification were significantly associated with the risk of death (p=0.04 and 0.03, respectively). The Veronesi classification was also associated with the risk of cardiovascular complications (p=0.013) and the length of the ICU stay (p=0.009). CONCLUSION: The present study demonstrates the failure of primary medical care in vaccination and post-traumatic tetanus prophylaxis. Despite improvements in intensive care support, cardiovascular complications are still frequent in these patients. Individuals exhibiting high APACHE II scores and severe clinical forms of tetanus should be monitored closely due to a risk of death and cardiovascular complications.
-
Original Articles – Clinical Research
Clinical-pathological discrepancies in critically ill patients with difficult premortem diagnoses
Rev Bras Ter Intensiva. 2011;23(4):442-447
Abstract
Original Articles – Clinical ResearchClinical-pathological discrepancies in critically ill patients with difficult premortem diagnoses
Rev Bras Ter Intensiva. 2011;23(4):442-447
DOI 10.1590/S0103-507X2011000400008
Views0See moreINTRODUCTION: The importance of autopsies is a common theme of discussions both in Brazil and around the world as it elucidates causes of death and has wide ranging social value. However this is a practice that is gradually being considered unnecessary and there have been a decline in the number of postmortems examinations. OBJECTIVES: To compare clinical and pathological diagnosis in critically ill patients with difficult premortem diagnosis. METHODS: All autopsy cases (total of 98) from any of the three general medical/surgical intensive care units (78 beds in total) affiliated to the medical school from January 2003 to December 2006 were analyzed. We analyzed the clinical and pathological diagnosis based on the Goldman criteria. RESULTS: In 49 (50%) cases, there were class I and II of Goldman. In contrast, only 30 (30.6%) had a complete agreement between premortem and postmortem diagnosis and were classified as class V. Infections had a significantly greater rate of concordant diagnosis than cardiovascular diseases. CONCLUSION: We found significant discrepancies between clinical and pathological findings, reinforcing the value of postmortem examination.
-
Original Articles – Clinical Research
End of life in intensive care: family members’ acceptance of orthotanasia
Rev Bras Ter Intensiva. 2011;23(4):448-454
Abstract
Original Articles – Clinical ResearchEnd of life in intensive care: family members’ acceptance of orthotanasia
Rev Bras Ter Intensiva. 2011;23(4):448-454
DOI 10.1590/S0103-507X2011000400009
Views1See moreOBJECTIVES: This study aimed to assess family member acceptance of orthotanasia as related to symptom management, patient preference and the influence of the medical team’s communication on therapy. METHODS: This was a descriptive one-year study conducted at the adult intensive care unit of the Hospital do Servidor Público Estadual. A structured questionnaire based on the Quality of Dying and Death (QODD 22) instrument and prior informal interviews were used. RESULTS: Sixty family members were assessed; the mean age was 51.7 + 12.1 years, and 81.7% were female. The patients were hospitalized for a mean of 31 + 26.9 days, and 17.0% of these days were spent in the intensive care unit. Most of the patients had neurological conditions. Most of the patients (53.3%) had discussed their end-of-life care wishes with family members; however, 76.7% of them had not discussed this issue with their doctors (p < 0.00). The family members reported being favorable to orthotanasia in 83.3% of the cases. Most (85.0%) desired the medical team to clearly approach the subject, and 65.0% wished to take part in the quality of end-of-life decision making process. The family members were generally satisfied with information they received from the doctors: 93.3% believed they had received appropriately frequent communications about the clinical conditions; 81.7% were able to clarify their doubts regarding the patient's clinical status; the communication was understood by 83.3% of the respondents; and 80.0% believed that clear and honest information had been provided. Only 43.3% of the respondents wished to be present at the time of their loved ones' deaths. A significant association between family member acceptance of orthotanasia and participation in end-of-life decisions (p = 0.042) was observed. CONCLUSIONS: Most of the respondents were favorable to orthotanasia and wished to participate in end-of-life discussions.
-
Original Articles – Clinical Research
The neuroprotective role of therapeutic hypothermia after cardiac arrest
Rev Bras Ter Intensiva. 2011;23(4):455-461
Abstract
Original Articles – Clinical ResearchThe neuroprotective role of therapeutic hypothermia after cardiac arrest
Rev Bras Ter Intensiva. 2011;23(4):455-461
DOI 10.1590/S0103-507X2011000400010
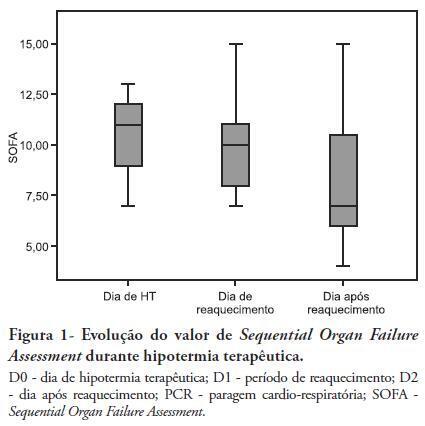
Views0See moreOBJECTIVES: Therapeutic hypothermia following cardiorespiratory arrest has been demonstrated to have cardio- and neuroprotective effects, resulting in improved survival and better neurological outcomes. The objective of this study was to assess the outcomes of patients undergoing therapeutic hypothermia following cardiorespiratory arrest. METHODS: A prospective, 10-month observational study of patients admitted to an intensive care unit and undergoing therapeutic hypothermia after cardiorespiratory arrest was undertaken. Therapeutic hypothermia was induced by cold fluid administration and body surface cooling in patients admitted no more than 12 hours after resuscitation from cardiorespiratory arrest. A target temperature of 33ºC was maintained for 24 hours. RESULTS: Overall, 12 patients were included (median age 64 years, 58% male). Half of the cardiorespiratory arrests were in-hospital. The median first-day Charlson Index, Sequential Organ Failure Assessment (SOFA) and Acute Physiology and Chronic Health Evaluation II scores were of 2.9, 11 and 24.5, respectively. The intensive care unit mortality rate was 42% (N=5). Five of the 7 surviving patients recovered their pre-cardiorespiratory arrest neurological status. Hypothermia was initiated 120 min (median) after recovery of spontaneous circulation. Most patients (75%) required vasopressor support. During the first 3 days after cardiorespiratory arrest and therapeutic hypothermia, a progressive SOFA score decrease (median 11 on day 0, 10 on day 1 and 7 on day 2) was observed. DISCUSSION: In this study, therapeutic hypothermia was applied to all post-cardiorespiratory arrest patients and demonstrated good neurological outcome in surviving patients.
-
Original Articles – Clinical Research
Professional profile of pediatric intensivists in Rio de Janeiro, southeastern Brazil
Rev Bras Ter Intensiva. 2011;23(4):462-469
Abstract
Original Articles – Clinical ResearchProfessional profile of pediatric intensivists in Rio de Janeiro, southeastern Brazil
Rev Bras Ter Intensiva. 2011;23(4):462-469
DOI 10.1590/S0103-507X2011000400011
Views0OBJECTIVE: This study described the sociodemographic profile and professional qualifications of pediatric intensive care physicians in the State of Rio de Janeiro (RJ), southeastern Brazil. METHODS: This investigation was an observational, cross-sectional and descriptive study that was conducted in neonatal, pediatric and mixed intensive care units in the State of Rio de Janeiro. Physicians working in the participating intensive care units voluntarily completed a semistructured and anonymous questionnaire. Questionnaires that were not returned within 30 days were considered lost, and questionnaires with less than 75% questions completed were excluded. The differences in neonatal and pediatric intensive care physicians’ medical training were compared using the Chi-squared test with a 5% significance level. RESULTS: A total of 410 physicians were included in this study: 84% female, 48% between 30 and 39 years old and 45% with monthly incomes between US $1,700 to 2,700. Forty percent of these physicians worked exclusively in this specialty, and 72% worked in more than one intensive care unit. Only 50% of the participants had received specific training (either medical residency or specialization) in neonatology, and only 33% were board-certified specialists in this area. Only 27% of the physicians had received specific training in pediatric intensive care medicine, and only 17% were board-certified specialists (p < 0.0005 for both comparisons). Most (87%) physicians had participated in scientific events within the past 5 years, and 55% used the internet for continued medical education. However, only 25% had participated in any research. Most (63%) physicians were dissatisfied with their professional activity; 49% were dissatisfied due to working conditions, 23% due to low incomes and 18% due to training-related issues. CONCLUSION: These results suggested that the medical qualifications of neonatal and pediatric intensive care physicians in the State of Rio de Janeiro, Brazil are inadequate, especially in pediatric intensive care medicine. A high level of dissatisfaction was reported, which may jeopardize the quality of medical assistance that is provided by these professionals.
Keywords:BrazilEducation, medicalIntensive careIntensive care units, neonatalIntensive care units, pediatricProfessional practiceSee more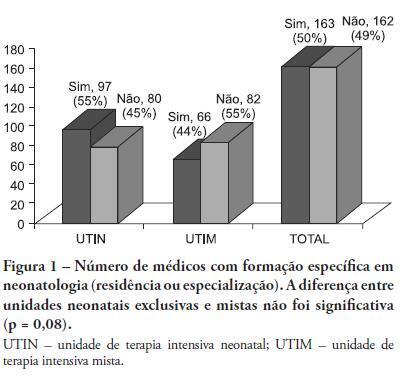
-
Original Articles – Clinical Research
Evaluation of postoperative pain experience in intensive care unit patients
Rev Bras Ter Intensiva. 2011;23(4):470-477
Abstract
Original Articles – Clinical ResearchEvaluation of postoperative pain experience in intensive care unit patients
Rev Bras Ter Intensiva. 2011;23(4):470-477
DOI 10.1590/S0103-507X2011000400012
Views0See moreOBJECTIVE: This study assessed the role of the nursing staff in pain management and verified the pain experiences of patients undergoing major surgery and receiving postoperative care in the intensive care unit. METHOD: This was a prospective, observational study of postoperative patients who were admitted to the intensive care unit and later discharged to one of the hospital’s regular wards. Patients with impaired communication were excluded. All patients signed an informed consent form. Data were collected using a questionnaire of 13 pain-related questions. RESULTS: A total of 167 patients were included, and 69.5% were male. Patient age ranged from 50-59 years, and the intensive care unit stay was one to three days. The majority of the patients (85%) reported no difficulties in expressing their painful symptoms, and the nursing approach in 54.5% of patients was only to recognize the presence or absence of pain. No pain scale was used. The most painful conditions included the surgical wound and bed positioning. CONCLUSION: The nursing team was apparently more concerned with the presence of pain than with its quality, severity or possible painful stimuli. Pain scales were not used, which suggests the need for continued education of the nursing professionals on the manner of approaching their patients and assessing their patients’ pain.
-
Original Articles – Clinical Research
Adrenal insufficiency in children with sepsis
Rev Bras Ter Intensiva. 2011;23(4):478-483
Abstract
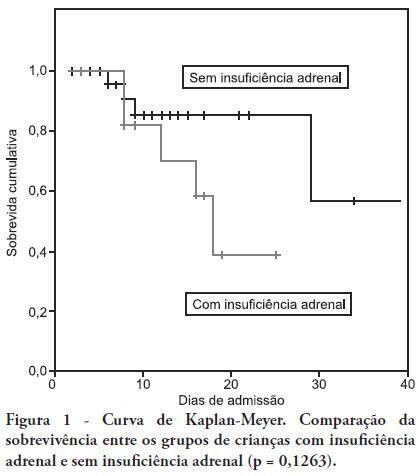
Original Articles – Clinical ResearchAdrenal insufficiency in children with sepsis
Rev Bras Ter Intensiva. 2011;23(4):478-483
DOI 10.1590/S0103-507X2011000400013
Views0See moreOBJECTIVE: To determine the frequency of adrenal insufficiency in children diagnosed with sepsis that were staying in pediatric intensive care units and to establish the association between adrenal function and the use of vasoactive drugs, mechanical ventilation time and mortality. METHODS: A cohort-designed study was conducted to assess the incidence of adrenal insufficiency in children aged 29 days to 12 years who were diagnosed with sepsis using the adrenocorticotropic hormone (ACTH) stimulation test. RESULTS: Thirty-nine children were included in the study. The frequency of adrenal insufficiency was 30.7% (12 patients). Children with adrenal insufficiency had an increased need for vasoactive drugs as well as longer mechanical ventilation times; however, the differences were not statistically significant. A Kaplan-Meier curve indicated lower survival rates among the adrenal insufficiency children, but the differences were not statistically significant (p = 0.1263). No differences were identified between the adrenal sufficiency and adrenal insufficiency groups in regards to mechanical ventilation time, use of vasoactive drugs, infection type and chronic disease. CONCLUSION: This study determined the frequency of adrenal insufficiency in children with sepsis and its relationship to increased mortality within the first 28 post-admission days. No statistically significant association was found between adrenal insufficiency and mechanical ventilation time or the use of vasoactive drugs.
-
Review Articles
Clostridium tetani infections in newborn infants: a tetanus neonatorum review
Rev Bras Ter Intensiva. 2011;23(4):484-491
Abstract
Review ArticlesClostridium tetani infections in newborn infants: a tetanus neonatorum review
Rev Bras Ter Intensiva. 2011;23(4):484-491
DOI 10.1590/S0103-507X2011000400014
Views0See moreAlthough tetanus is a preventable disease by vaccination, it continues to claim lives around the world. Whereas cases of accidental origin reflect insufficient population immunization, tetanus neonatorum reveals a double-nature fault-poor vaccination coverage of adults coupled with difficulties accessing appropriate prenatal care; this situation is aggravated by the extreme severity of tetanus in this age group in which the mortality rate can reach up to 80%. The early detection of tetanus in neonates is essential for immediately initiating the proper therapy. Therefore, although reaching an early diagnosis of tetanus is important, the most relevant aspect is related to the appropriate management and prophylaxis of this disease. Consequently, the aim of this article is to review neonatorum tetanus with an emphasis on its therapy and prevention.

-
Review Articles
Nutritional therapy and neonatal sepsis
Rev Bras Ter Intensiva. 2011;23(4):492-498
Abstract
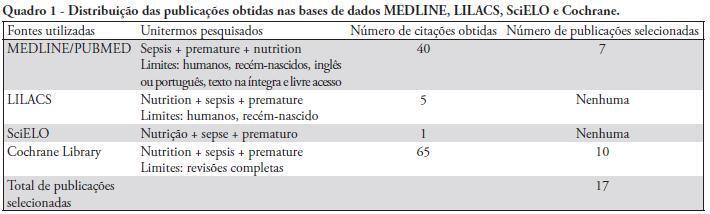
Review ArticlesNutritional therapy and neonatal sepsis
Rev Bras Ter Intensiva. 2011;23(4):492-498
DOI 10.1590/S0103-507X2011000400015
Views0See moreThis article reviews the current understanding of enteral and parenteral nutrition therapy in preterm infants, with an emphasis on very low birth weight babies. The protective effects of nutrition therapy against neonatal sepsis and necrotizing enterocolitis are discussed. Different methods of feeding preterm infants are evaluated. Special attention is given to the problems of very low birth weight babies and the protective effects of nutrition to counteract complications, especially infection. The preferential use of breast milk for enteral nutrition, the management of protein and energy offers, the use of early and minimal enteral nutrition, the early introduction of parenteral nutrition (within the first 24 hours of life) and the use of immunonutrients that are appropriately supported by a sufficient number of studies can provide good adjuvant therapy guidelines to prevent neonatal sepsis and necrotizing enterocolitis. However, we conclude that additional multicenter, randomized controlled studies are necessary to clarify the protective role of nutrition in preterm infants. Appropriate nutrition is not only effective in treating and preventing infective complications, but it also promotes neurodevelopment and prevents future harmful consequences.
-
Review Articles
Novel biomarkers in severe community-acquired pneumonia
Rev Bras Ter Intensiva. 2011;23(4):499-506
Abstract
Review ArticlesNovel biomarkers in severe community-acquired pneumonia
Rev Bras Ter Intensiva. 2011;23(4):499-506
DOI 10.1590/S0103-507X2011000400016
Views0See moreCommunity-acquired pneumonia (CAP) is the most common infectious disease requiring admission to intensive care units (ICUs), and achieving an early and precise diagnosis of CAP remains a challenge. Biomarkers play an important role in improving clinical judgment in the emergency room and are adjuvant in evaluating treatment responses. Novel biomarkers, such as cortisol, pro-adrenomedullin and endothelin-1, have been shown to be associated with disease severity and short-term outcomes. This review article focuses on the clinical use of novel biomarkers, severity prediction and treatment monitoring as well as future directions of the field.
-
Case Report
Meningitis and infective endocarditis caused by Rhodotorula mucilaginosa in an immunocompetent patient
Rev Bras Ter Intensiva. 2011;23(4):507-509
Abstract
Case ReportMeningitis and infective endocarditis caused by Rhodotorula mucilaginosa in an immunocompetent patient
Rev Bras Ter Intensiva. 2011;23(4):507-509
DOI 10.1590/S0103-507X2011000400017
Views0The authors report the case of an immunocompetent man who presented with acute impairment of the neurological system, hypertensive crisis and renal failure. The patient was eventually diagnosed with Rhodotorula mucilaginosa meningitis and infective endocarditis. To the best of our knowledge, this is the first description of simultaneous infection of the meninges and endothelium caused by Rhodotorula in a non-immunocompromised patient.
Keywords:Case reportsComacomplicationsendocarditisetiologyHypertensionMeningitis, fungalRenal insufficiencyRhodotorulaSee more -
Case Report
Acute intermittent porphyria, an important and rare differential diagnosis of acute abdomen: case report and literature review
Rev Bras Ter Intensiva. 2011;23(4):510-514
Abstract
Case ReportAcute intermittent porphyria, an important and rare differential diagnosis of acute abdomen: case report and literature review
Rev Bras Ter Intensiva. 2011;23(4):510-514
DOI 10.1590/S0103-507X2011000400018
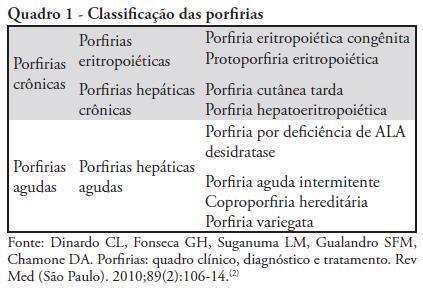
Views0Porphyrias are metabolic disorders related to heme biosynthesis pathway enzyme dysfunctions. The heme pathway is fundamental for the formation of a number of molecules, and such defects cause noxious precursors (porphyrins) to build up. Porphyrias are heterogeneously manifested by symptoms that can either be neurovisceral, cutaneous, or both, usually during outburst episodes called porphyric crises. This article presents a literature review and reports on a case of porphyric crisis initially diagnosed as acute abdomen and treated with an inconclusive exploratory laparotomy During the postoperative period, the patient progressed with tetraparesis, tetraplegia and respiratory distress, suggesting Guillain-Barre syndrome, which was precluded after cerebrospinal fluid analysis revealed no albumin-cytological dissociation. The patient was admitted to the intensive care unit due to her neurological disorders, which required ventilation support. After admission, she progressed with choluria and seizures. A porphyric crisis was suspected and confirmed upon a 24 hour urine porphyrins test. Supportive therapy was initiated, but due to unavailability in our hospital, heme derivatives were not given. The patient progressed with nosocomial infection, organ dysfunctions and eventually died. Porphyria should be considered as a differential diagnosis in acute abdomen cases of unknown origin and associated with neurological disorders such as paresis, hydroelectrolytic and psychiatric disorders, especially in patients with triggering factors, with a history of recurring crises and a family history of porphyria.
Keywords:Acute abdomenCase reportsDifferential diagnosisIntermittent acute porphyriaLiver porphyriaPorphyriaSee more