You searched for:"Felipe Dal-Pizzol"
We found (22) results for your search.-
Special Article
Brazilian guidelines for the management of brain-dead potential organ donors. The task force of the Associação de Medicina Intensiva Brasileira, Associação Brasileira de Transplantes de Órgãos, Brazilian Research in Critical Care Network, and the General Coordination of the National Transplant System
Rev Bras Ter Intensiva. 2021;33(1):1-11
Abstract
Special ArticleBrazilian guidelines for the management of brain-dead potential organ donors. The task force of the Associação de Medicina Intensiva Brasileira, Associação Brasileira de Transplantes de Órgãos, Brazilian Research in Critical Care Network, and the General Coordination of the National Transplant System
Rev Bras Ter Intensiva. 2021;33(1):1-11
DOI 10.5935/0103-507X.20210001
Views5See moreAbstract
Objective:
To contribute to updating the recommendations for brain-dead potential organ donor management.
Methods:
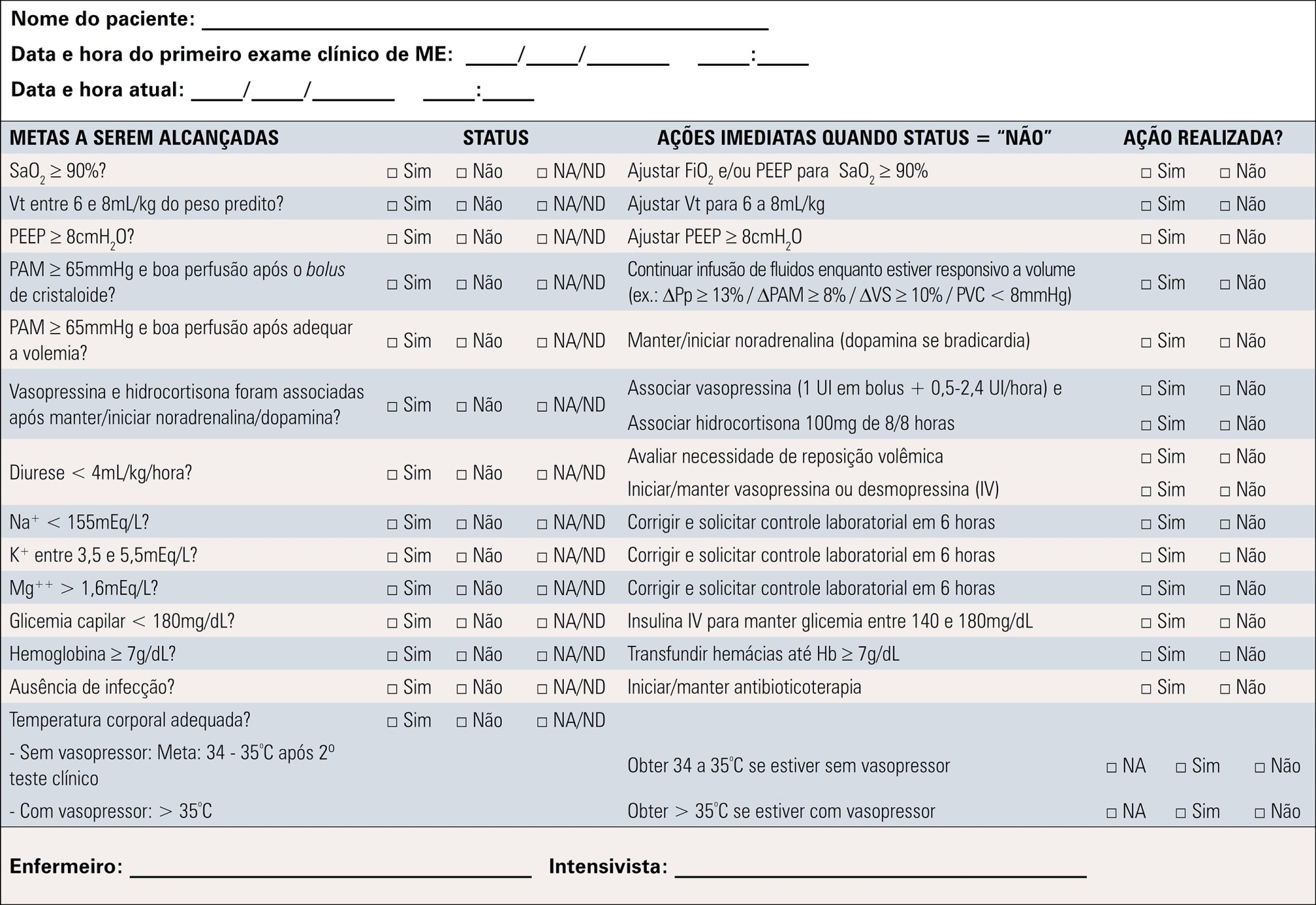
A group of 27 experts, including intensivists, transplant coordinators, transplant surgeons, and epidemiologists, answered questions related to the following topics were divided into mechanical ventilation, hemodynamics, endocrine-metabolic management, infection, body temperature, blood transfusion, and checklists use. The outcomes considered were cardiac arrests, number of organs removed or transplanted as well as function / survival of transplanted organs. The quality of evidence of the recommendations was assessed using the Grading of Recommendations Assessment, Development, and Evaluation system to classify the recommendations.
Results:
A total of 19 recommendations were drawn from the expert panel. Of these, 7 were classified as strong, 11 as weak and 1 was considered a good clinical practice.
Conclusion:
Despite the agreement among panel members on most recommendations, the grade of recommendation was mostly weak.
-
Special Article
Guidelines for the pharmacological treatment of COVID-19. The task-force/consensus guideline of the Brazilian Association of Intensive Care Medicine, the Brazilian Society of Infectious Diseases and the Brazilian Society of Pulmonology and Tisiology
Rev Bras Ter Intensiva. 2020;32(2):166-196
Abstract
Special ArticleGuidelines for the pharmacological treatment of COVID-19. The task-force/consensus guideline of the Brazilian Association of Intensive Care Medicine, the Brazilian Society of Infectious Diseases and the Brazilian Society of Pulmonology and Tisiology
Rev Bras Ter Intensiva. 2020;32(2):166-196
DOI 10.5935/0103-507X.20200039
Views0See moreABSTRACT
Introduction:
Different therapies are currently used, considered, or proposed for the treatment of COVID-19; for many of those therapies, no appropriate assessment of effectiveness and safety was performed. This document aims to provide scientifically available evidence-based information in a transparent interpretation, to subsidize decisions related to the pharmacological therapy of COVID-19 in Brazil.
Methods:
A group of 27 experts and methodologists integrated a task-force formed by professionals from the Brazilian Association of Intensive Care Medicine (Associação de Medicina Intensiva Brasileira – AMIB), the Brazilian Society of Infectious Diseases (Sociedad Brasileira de Infectologia – SBI) and the Brazilian Society of Pulmonology and Tisiology (Sociedade Brasileira de Pneumologia e Tisiologia – SBPT). Rapid systematic reviews, updated on April 28, 2020, were conducted. The assessment of the quality of evidence and the development of recommendations followed the GRADE system. The recommendations were written on May 5, 8, and 13, 2020.
Results:
Eleven recommendations were issued based on low or very-low level evidence. We do not recommend the routine use of hydroxychloroquine, chloroquine, azithromycin, lopinavir/ritonavir, corticosteroids, or tocilizumab for the treatment of COVID-19. Prophylactic heparin should be used in hospitalized patients, however, no anticoagulation should be provided for patients without a specific clinical indication. Antibiotics and oseltamivir should only be considered for patients with suspected bacterial or influenza coinfection, respectively.
Conclusion:
So far no pharmacological intervention was proven effective and safe to warrant its use in the routine treatment of COVID-19 patients; therefore such patients should ideally be treated in the context of clinical trials. The recommendations herein provided will be revised continuously aiming to capture newly generated evidence.
-
Original Article
Stratification to predict the response to antioxidant
Rev Bras Ter Intensiva. 2020;32(1):108-114
Abstract
Original ArticleStratification to predict the response to antioxidant
Rev Bras Ter Intensiva. 2020;32(1):108-114
DOI 10.5935/0103-507X.20200016
Views1See moreABSTRACT
Objective:
To examine the effectiveness of stratification to identify and target antioxidant therapy for animal models of lethal sepsis and in patients who develop sustained hypotension.
Methods:
Rats were subjected to sepsis induced by cecal ligation and puncture. Animals were divided into two groups: those with high and low plasma levels of interleukin-6. Following stratification, N-acetylcysteine plus deferoxamine or saline was administered to animals starting 3 and 12 hours after surgery. N-Acetylcysteine plus deferoxamine or placebo was administered within 12 hours of meeting the inclusion criteria in hypotensive patients.
Results:
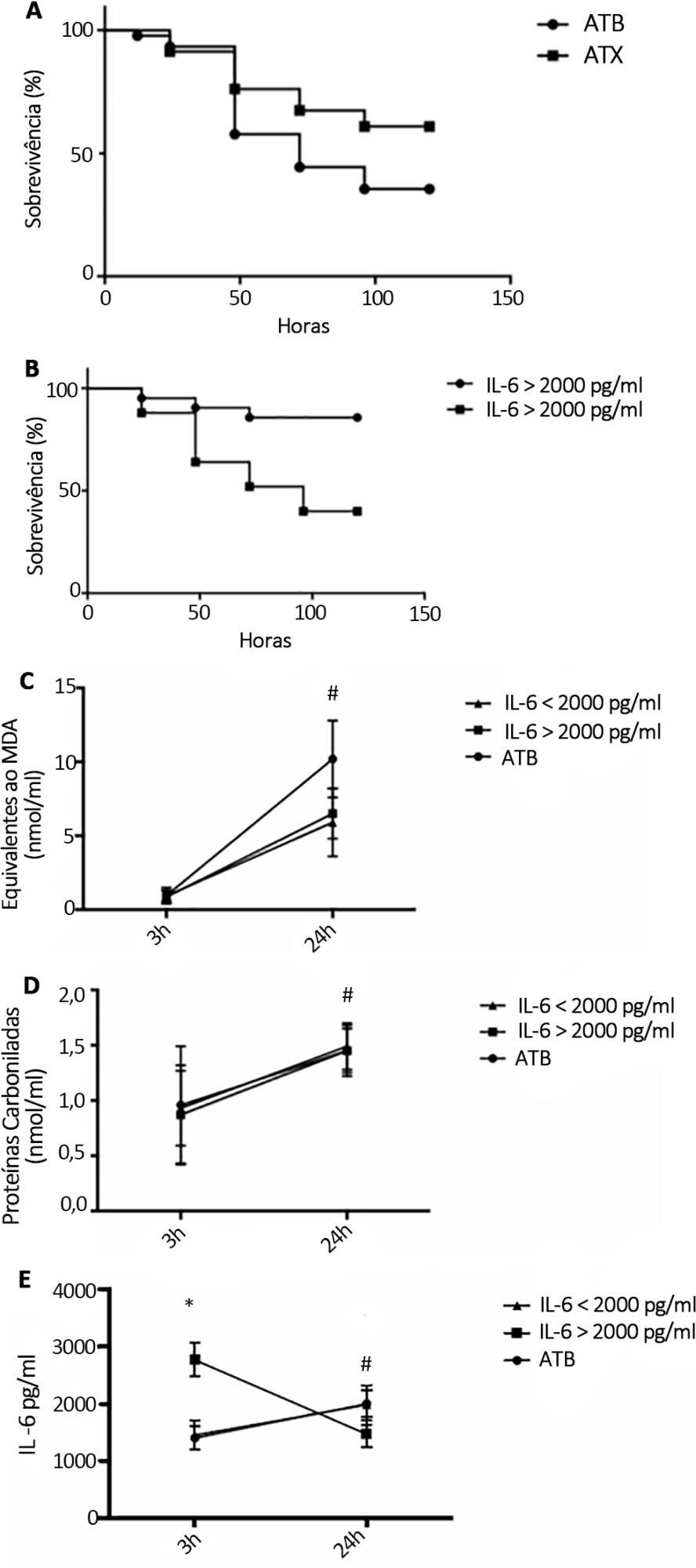
N-Acetylcysteine plus deferoxamine increased survival in the cecal ligation and puncture model when administered 3 and 12 hours after sepsis induction. When dividing animals that received antioxidants using plasma interleukin-6 levels, the protective effect was observed only in those animals with high IL-6 levels. The antioxidant effect of N-acetylcysteine + deferoxamine was similar in the two groups, but a significant decrease in plasma interleukin-6 levels was observed in the high-interleukin-6-level group. Compared with patients treated with antioxidants in the low-interleukin-6 subgroup, those in the high-interleukin-6 subgroup had a lower incidence of acute kidney injury but were not different in terms of acute kidney injury severity or intensive care unit mortality.
Conclusion:
Targeting antioxidant therapy to a high inflammatory phenotype would select a responsive population.
-
Original Articles
Baseline acetylcholinesterase activity and serotonin plasma levels are not associated with delirium in critically ill patients
Rev Bras Ter Intensiva. 2015;27(2):170-177
Abstract
Original ArticlesBaseline acetylcholinesterase activity and serotonin plasma levels are not associated with delirium in critically ill patients
Rev Bras Ter Intensiva. 2015;27(2):170-177
DOI 10.5935/0103-507X.20150029
Views0See moreABSTRACT
Objective:
The aim of this study was to investigate whether plasma serotonin levels or acetylcholinesterase activities determined upon intensive care unit admission could predict the occurrence of acute brain dysfunction in intensive care unit patients.
Methods:
A prospective cohort study was conducted with a sample of 77 non-consecutive patients observed between May 2009 and September 2010. Delirium was determined using the Confusion Assessment Method for the Intensive Care Unit tool, and the acetylcholinesterase and serotonin measurements were determined from blood samples collected up to a maximum of 24 h after the admission of the patient to the intensive care unit.
Results:
In the present study, 38 (49.6%) patients developed delirium during their intensive care unit stays. Neither serum acetylcholinesterase activity nor serotonin level was independently associated with delirium. No significant correlations of acetylcholinesterase activity or serotonin level with delirium/coma-free days were observed, but in the patients who developed delirium, there was a strong negative correlation between the acetylcholinesterase level and the number of delirium/coma-free days, indicating that higher acetylcholinesterase levels are associated with fewer days alive without delirium or coma. No associations were found between the biomarkers and mortality.
Conclusions:
Neither serum acetylcholinesterase activity nor serotonin level was associated with delirium or acute brain dysfunction in critically ill patients. Sepsis did not modify these relationships.
-
Original Article
Delirium in intensive care unit patients under noninvasive ventilation: a multinational survey
Rev Bras Ter Intensiva. 2015;27(4):360-368
Abstract
Original ArticleDelirium in intensive care unit patients under noninvasive ventilation: a multinational survey
Rev Bras Ter Intensiva. 2015;27(4):360-368
DOI 10.5935/0103-507X.20150061
Views0ABSTRACT
Objective:
To conduct a multinational survey of intensive care unit professionals to determine the practices on delirium assessment and management, in addition to their perceptions and attitudes toward the evaluation and impact of delirium in patients requiring noninvasive ventilation.
Methods:
An electronic questionnaire was created to evaluate the profiles of the respondents and their related intensive care units, the systematic delirium assessment and management and the respondents’ perceptions and attitudes regarding delirium in patients requiring noninvasive ventilation. The questionnaire was distributed to the cooperative network for research of the Associação de Medicina Intensiva Brasileira (AMIB-Net) mailing list and to researchers in different centers in Latin America and Europe.
Results:
Four hundred thirty-six questionnaires were available for analysis; the majority of the questionnaires were from Brazil (61.9%), followed by Turkey (8.7%) and Italy (4.8%). Approximately 61% of the respondents reported no delirium assessment in the intensive care unit, and 31% evaluated delirium in patients under noninvasive ventilation. The Confusion Assessment Method for the intensive care unit was the most reported validated diagnostic tool (66.9%). Concerning the indication of noninvasive ventilation in patients already presenting with delirium, 16.3% of respondents never allow the use of noninvasive ventilation in this clinical context.
Conclusion:
This survey provides data that strongly reemphasizes poor efforts toward delirium assessment and management in the intensive care unit setting, especially regarding patients requiring noninvasive ventilation.
Keywords:Attitude of health personnelCritical careDeliriumDiagnostic techniques, neurologicalNoninvasive ventilationQuestionnairesSee more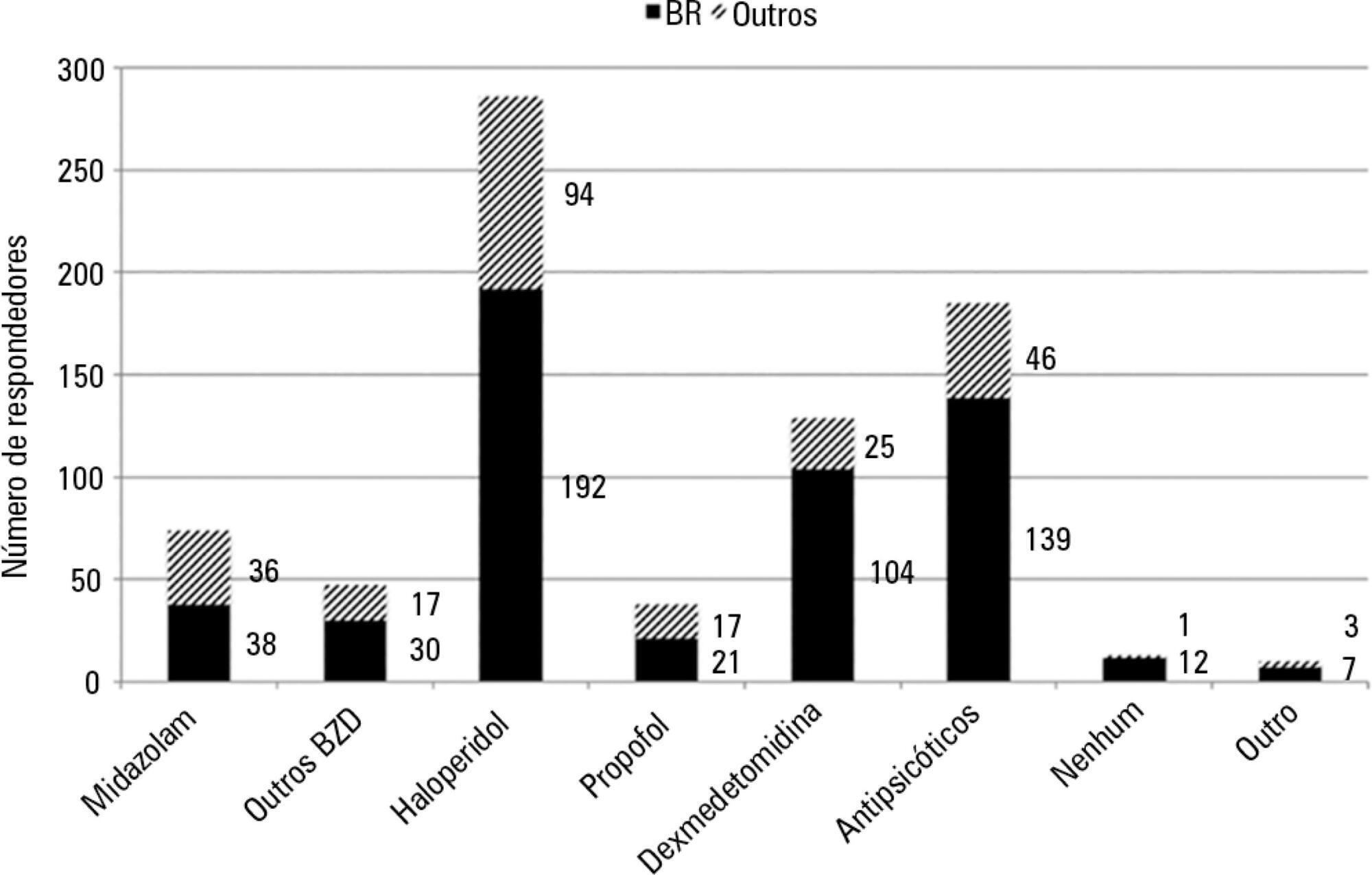
-
How do you prefer your resuscitation solution?: do you want a little bit more salt?
Rev Bras Ter Intensiva. 2012;24(4):315-315
Abstract
How do you prefer your resuscitation solution?: do you want a little bit more salt?
Rev Bras Ter Intensiva. 2012;24(4):315-315
DOI 10.1590/S0103-507X2012000400001
Views0EDITORIAL How do you prefer your resuscitation solution? Do you want a little bit more salt?[…]See more -
Original Article – Basic Research
N-acetylcysteine and deferrioxamine protects against acute renal failure induced by ischemia/reperfusion in rats
Rev Bras Ter Intensiva. 2012;24(3):219-223
Abstract
Original Article – Basic ResearchN-acetylcysteine and deferrioxamine protects against acute renal failure induced by ischemia/reperfusion in rats
Rev Bras Ter Intensiva. 2012;24(3):219-223
DOI 10.1590/S0103-507X2012000300003
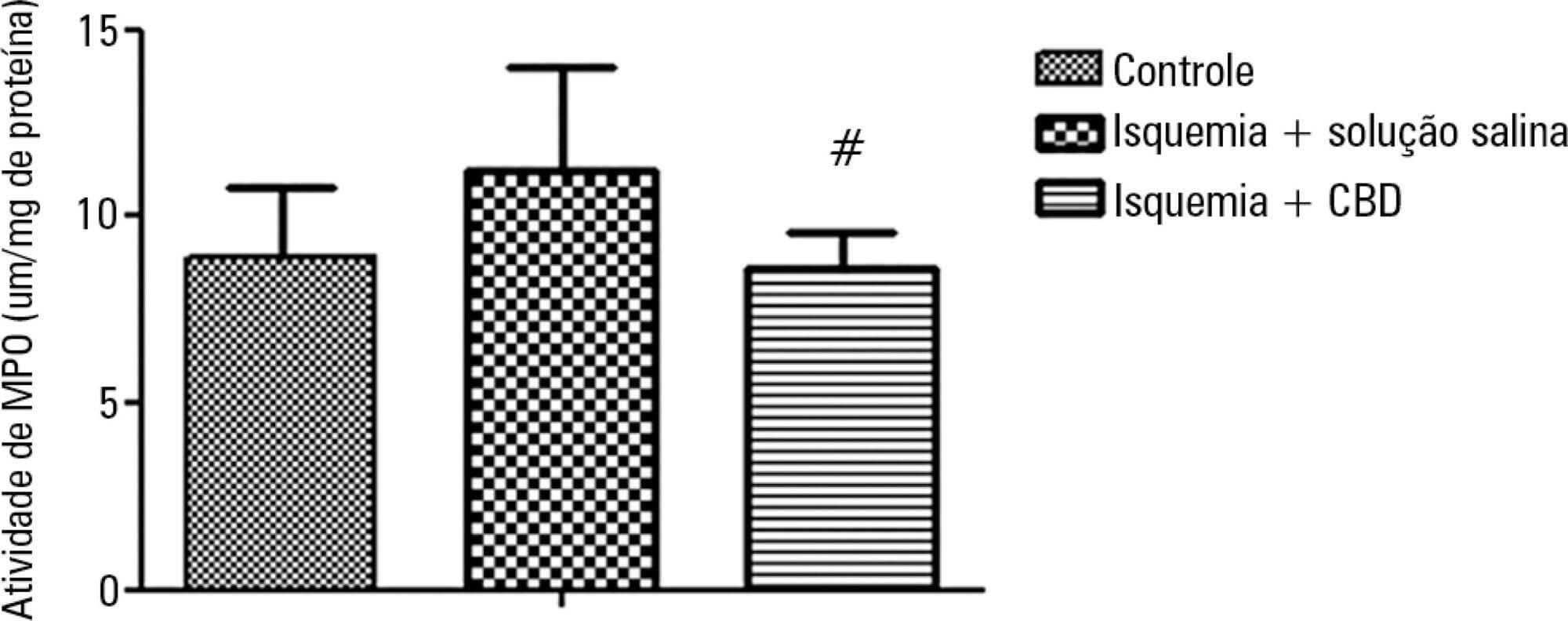
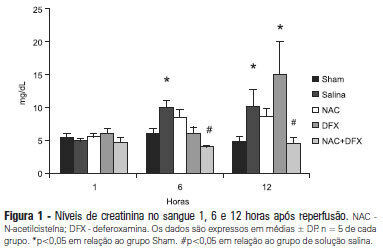
Views0See moreOBJECTIVE: Antioxidants are widely used in animal models to prevent renal injury after ischemia/reperfusion, but it is unknown if the benefits of antioxidants are additive. In this study, we aimed to investigate the protective effects of N-acetylcysteine plus deferoxamine in an animal model of kidney ischemia/reperfusion injury. METHODS: Bilateral kidney ischemia was mastintained for 45 minutes. N-acetylcysteine, deferoxamine or both were administered into the aorta above the renal arteries immediately prior to induction of ischemia. Five rats from each group were sacrificed 1, 6 or 12 hours after reperfusion for the determination of blood creatinine, kidney oxidative damage parameters and myeloperoxidase activity. RESULTS: The combination of N-acetylcysteine and deferoxamine, but not their isolated use, prevented the increase in creatinine after ischemia/reperfusion. This prevention was followed by a consistent decrease in myeloperoxidase activity and oxidative damage parameters both in the kidney cortex and medulla. CONCLUSION: Treatment with N-acetylcysteine and deferoxamine was superior to the isolated use of either compound in an animal model of kidney ischemia/reperfusion.
Search
Search in:
KEY WORDS
Case reports Child Coronavirus infections COVID-19 Critical care Critical illness Extracorporeal membrane oxygenation Infant, newborn Intensive care Intensive care units Intensive care units, pediatric mechanical ventilation Mortality Physical therapy modalities Prognosis Respiration, artificial Respiratory insufficiency risk factors SARS-CoV-2 Sepsis