Abstract
Rev Bras Ter Intensiva. 2022;34(1):185-196
DOI 10.5935/0103-507X.20220013-en
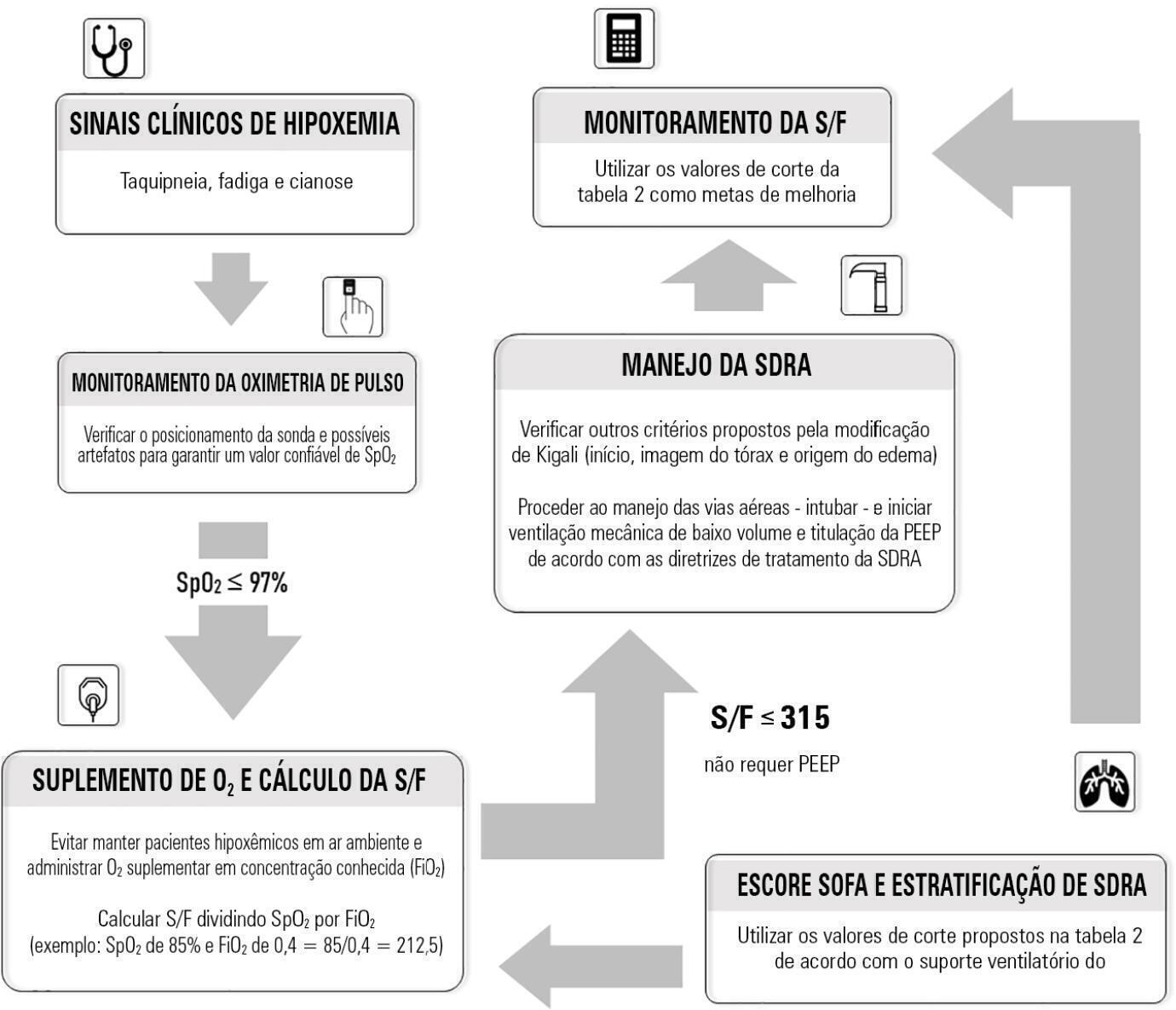
Although the PaO 2/FiO 2 derived from arterial blood gas analysis remains the gold standard for the diagnosis of acute respiratory failure, the SpO2/FiO2 has been investigated as a potential substitute. The current narrative review presents the state of the preclinical and clinical literature on the SpO2/FiO2 as a possible substitute for PaO2/FiO2 and for use as a diagnostic and prognostic marker; provides an overview of pulse oximetry and its limitations, and assesses the utility of SpO2/ FiO2 as a surrogate for PaO2/FiO2 in COVID-19 patients. Overall, 49 studies comparing SpO2/FiO2 and PaO2/FiO2 were found according to a minimal search strategy. Most were conducted on neonates, some were conducted on adults with acute respiratory distress syndrome, and a few were conducted in other clinical scenarios (including a very few on COVID-19 patients). There is some evidence that the SpO2/ FiO2 criteria can be a surrogate for PaO2/FiO2 in different clinical scenarios. This is reinforced by the fact that unnecessary invasive procedures should be avoided in patients with acute respiratory failure. It is undeniable that pulse oximeters are becoming increasingly widespread and can provide costless monitoring. Hence, replacing PaO2/FiO2 with SpO2/FiO2may allow resourcelimited facilities to objectively diagnose acute respiratory failure.
Abstract
Rev Bras Ter Intensiva. 2012;24(2):162-166
DOI 10.1590/S0103-507X2012000200011
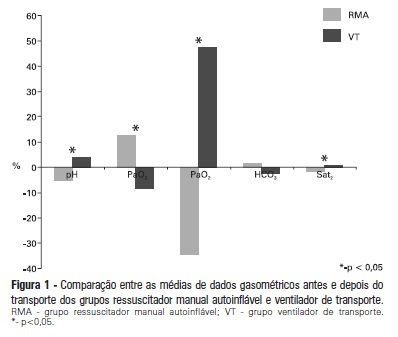
OBJECTIVE: To evaluate the effects on blood gases by two methods of ventilation (with transport ventilation or self-inflating manual resuscitator) during intra-hospital transport of patients after cardiac surgery. METHODS: Observational, longitudinal, prospective, randomized study. Two samples of arterial blood were collected at the end of the surgery and another at the end of patient transport. RESULTS: We included 23 patients: 13 in the Group with transport ventilation and 10 in the Group with self-inflating manual resuscitator. Baseline characteristics were similar between both groups, except for higher acute severity of illness in the Group with transport ventilation. We observed significant differences in comparisons of percentage variations of gasometric data: pH (transport ventilation + 4% x MR -5%, p=0.007), PaCO2 (-8% x +13%, p=0.006), PaO2 (+47% x -34%, p=0.01) and SatO2 (+0.6% x -1.7%, p=0.001). CONCLUSION: The use of mechanical ventilation results in fewer repercussions for blood gas analysis in the intra-hospital transport of cardiac surgery patients.
Abstract
Rev Bras Ter Intensiva. 2007;19(3):322-326
DOI 10.1590/S0103-507X2007000300009
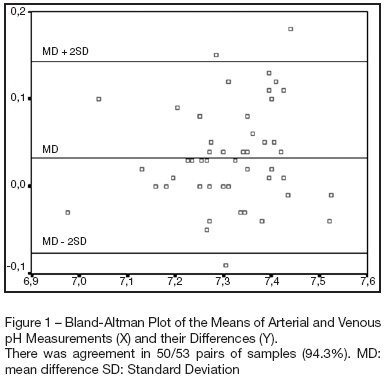
BACKGROUND AND OBJECTIVES: Determine the extent of agreement and correlation between arterial samples and venous (obtained from a venous umbilical catheter), with respect to measurements of pH, bicarbonate, base excess and lactate, in critically ill term and premature newborns. METHODS: Arterial blood samples (0.5-1 mL) were obtained for gas analysis by radial artery puncture, and, within the limit of 5 minutes, samples were obtained from venous umbilical catheters. Bland-Altman plots were used to depict agreement between arterial and venous measurements. Limits of agreement were defined as the mean difference ± 2SD (Standard Deviation). Correlation was assessed by Pearson's method. RESULTS: A hundred and six samples (53 pairs) were taken from 53 patients for analysis of bicarbonate, pH and base excess. Lactate was analyzed in 49 pairs of samples. Differences were within the limits of agreement in 94.3% of pairs of samples for pH, and the same percentage was observed for bicarbonate. There was agreement in 96.2% of pairs for base excess, and in 91.8% for lactate. Mean differences were 0.03 units for pH, -1.2 mmol/L for bicarbonate, -0.24 mmol/L for base excess and 0.33 mmol/L for lactate. Pearson's correlation coefficients (r) were 0.87 for pH, 0.76 for bicarbonate, 0.86 for base excess and 0.95 for lactate. CONCLUSIONS: Although single venous values cannot be used as equivalent to arterial for assessing acid base status in newborns, venous blood samples can be used serially for monitoring trends over time.
Search
Search in:
Case reports (56) Child (53) Coronavirus infections (34) COVID-19 (46) Critical care (116) Critical illness (54) Extracorporeal membrane oxygenation (26) Infant, newborn (27) Intensive care (72) Intensive care units (256) Intensive care units, pediatric (31) mechanical ventilation (38) Mortality (76) Physical therapy modalities (28) Prognosis (61) Respiration, artificial (119) Respiratory insufficiency (26) risk factors (34) SARS-CoV-2 (28) Sepsis (98)