You searched for:"Pedro Vitale Mendes"
We found (18) results for your search.-
Original Article
Intensivist-led ultrasound-guided percutaneous tracheostomy: a phase IV cohort study
Crit Care Sci. 2023;35(4):402-410
Abstract
Original ArticleIntensivist-led ultrasound-guided percutaneous tracheostomy: a phase IV cohort study
Crit Care Sci. 2023;35(4):402-410
DOI 10.5935/2965-2774.20230174-pt
Views25See moreABSTRACT
Objective:
To describe, with a larger number of patients in a real-world scenario following routine implementation, intensivist-led ultrasound-guided percutaneous dilational tracheostomy and the possible risks and complications of the procedure not identified in clinical trials.
Methods:
This was a phase IV cohort study of patients admitted to three intensive care units of a quaternary academic hospital who underwent intensivist-led ultrasound-guided percutaneous tracheostomy in Brazil from September 2017 to December 2021.
Results:
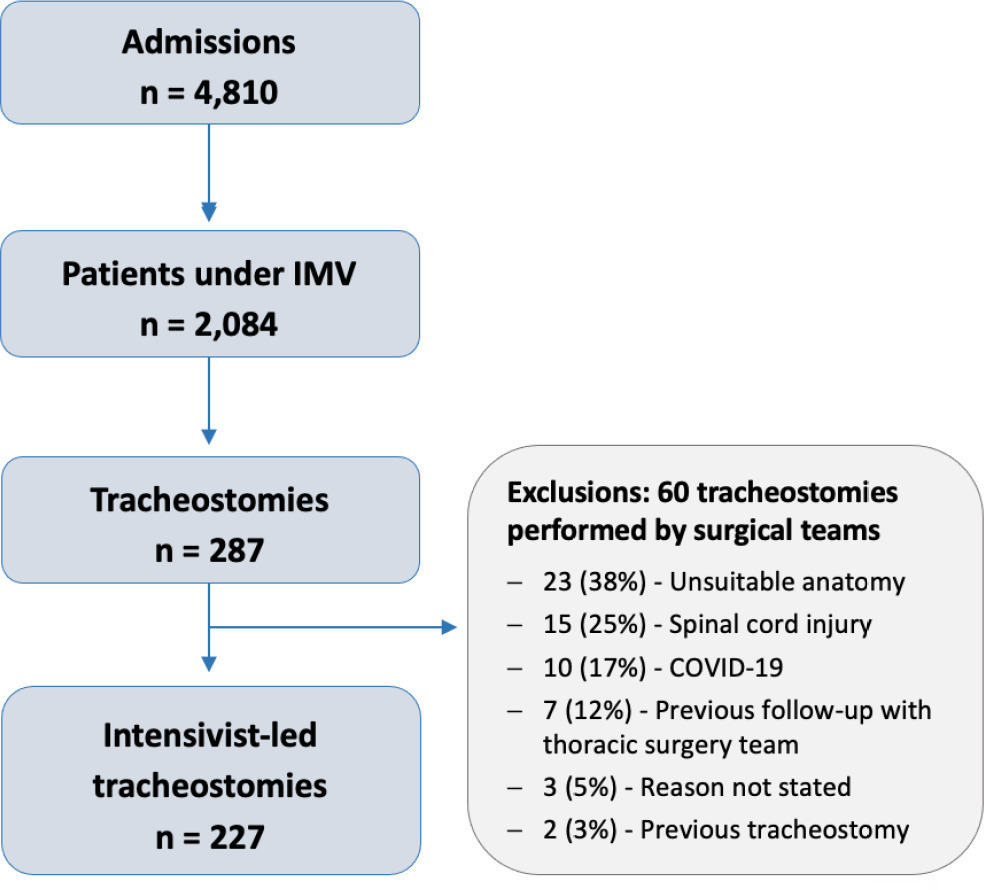
There were 4,810 intensive care unit admissions during the study period; 2,084 patients received mechanical ventilation, and 287 underwent tracheostomy, 227 of which were performed at bedside by the intensive care team. The main reason for intensive care unit admission was trauma, and for perform a tracheostomy it was a neurological impairment or an inability to protect the airways. The median time from intubation to tracheostomy was 14 days. Intensive care residents performed 76% of the procedures. At least one complication occurred in 29.5% of the procedures, the most common being hemodynamic instability and extubation during the procedure, with only 3 serious complications. The intensive care unit mortality was 29.1%, and the hospital mortality was 43.6%.
Conclusion:
Intensivist-led ultrasound-guided percutaneous tracheostomy is feasible out of a clinical trial context with outcomes and complications comparable to those in the literature. Intensivists can acquire this competence during their training but should be aware of potential complications to enhance procedural safety.
-
Letter to the Editor
Capillary leak syndrome during continuous renal replacement therapy after renal hilum ligation in a hypercapnic landrace pig
Crit Care Sci. 2023;35(4):413-415
Abstract
Letter to the EditorCapillary leak syndrome during continuous renal replacement therapy after renal hilum ligation in a hypercapnic landrace pig
Crit Care Sci. 2023;35(4):413-415
DOI 10.5935/2965-2774.20230139-pt
Views11Literature on dialysis in pigs is scarce, and there is no description of capillary leak syndrome during dialysis in pigs. Our aim in this paper is to bring attention to the possible occurrence of this syndrome, at least in the described specific condition.In an ongoing experimental line of research, we are investigating the impact of […]See more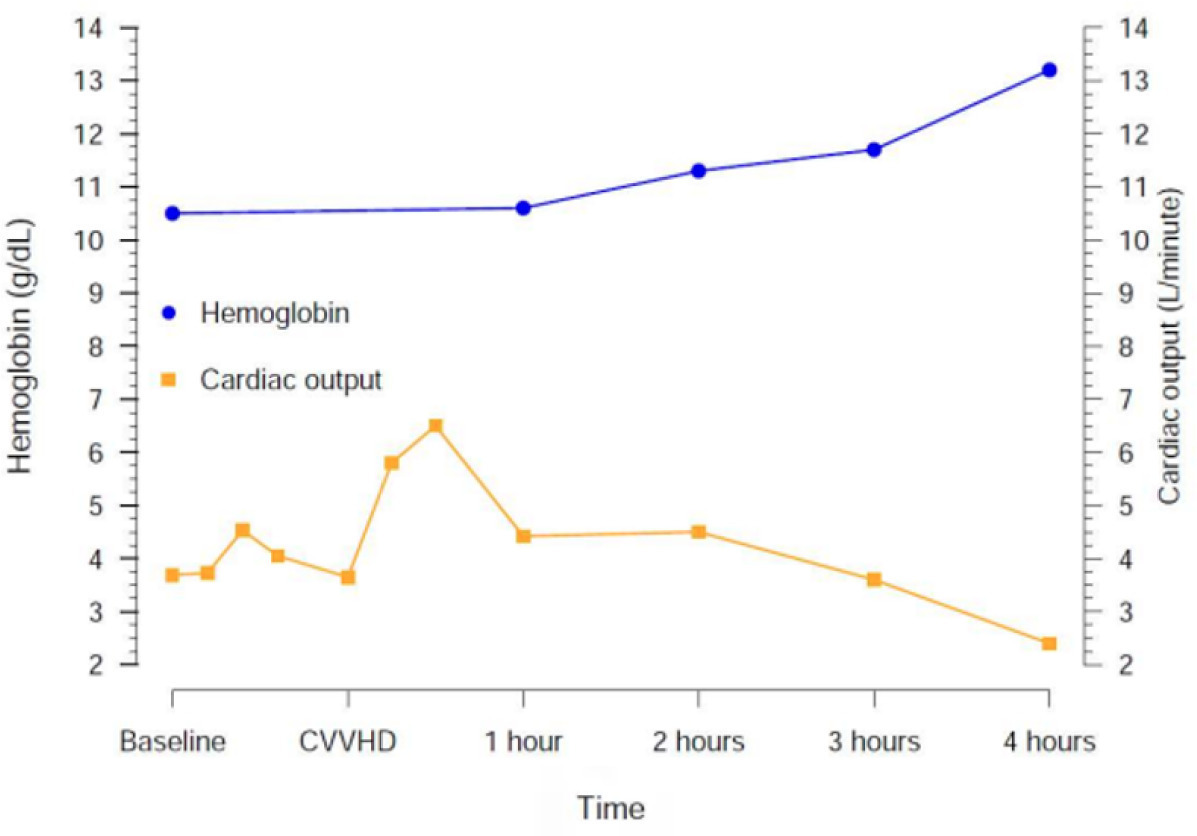
-
Letter to the Editor
Sulfonamide-induced acute eosinophilic pneumonia requiring extracorporeal membrane oxygenation support: a case report
Crit Care Sci. 2023;35(2):239-242
Abstract
Letter to the EditorSulfonamide-induced acute eosinophilic pneumonia requiring extracorporeal membrane oxygenation support: a case report
Crit Care Sci. 2023;35(2):239-242
DOI 10.5935/2965-2774.20230404-pt
Views3INTRODUCTIONAcute eosinophilic pneumonia (AEP) is a rare cause of acute respiratory failure that affects people aged 20-40 years old.() Patients with AEP present with rapid onset of cough, dyspnea, tachypnea and fever of usually less than 7 days of duration. Hypoxemia is present in all cases, and most patients do not have peripheral blood eosinophilia. […]See more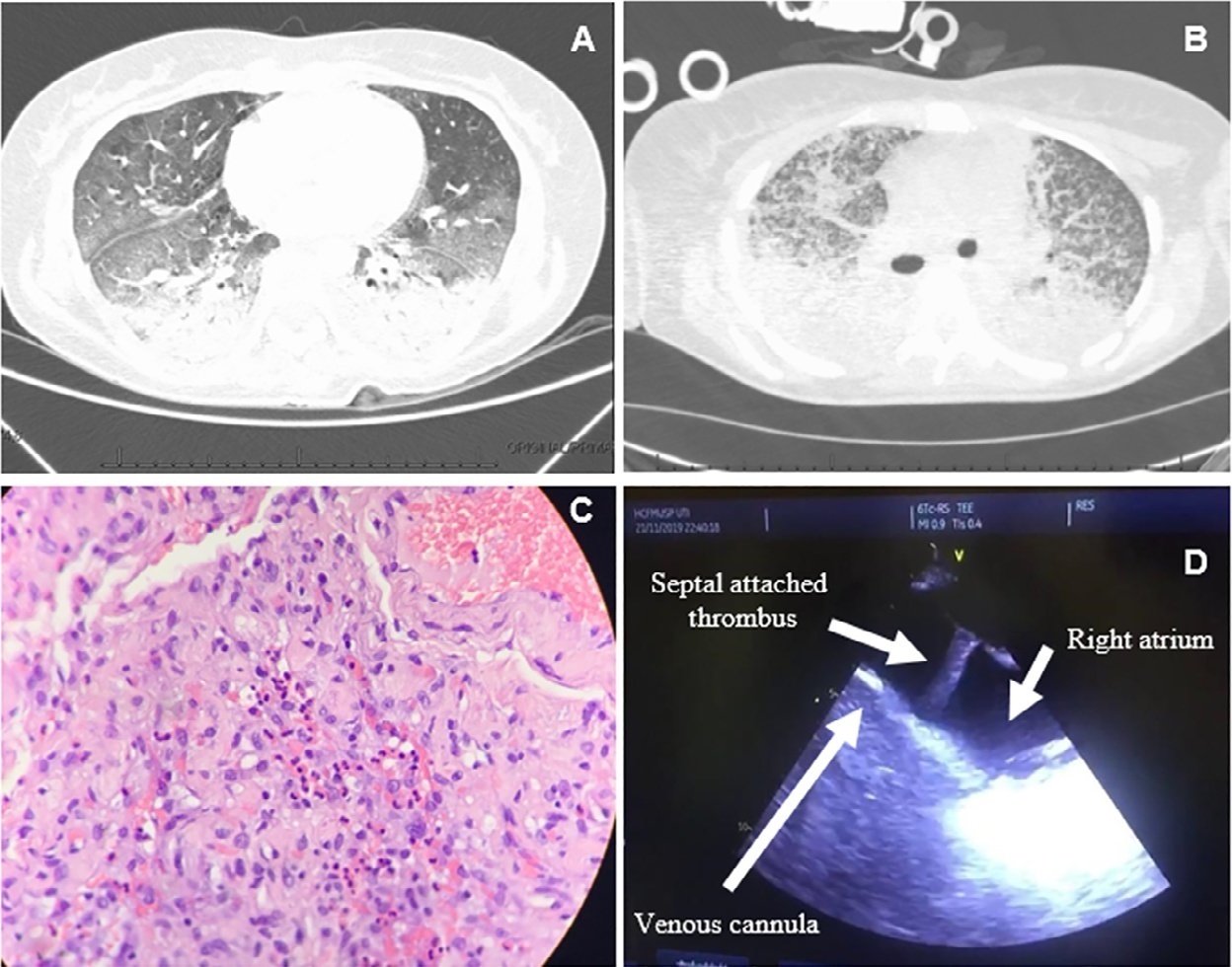
-
Original Article
Exploring the association of two oxygenators in parallel or in series during respiratory support using extracorporeal membrane oxygenation
Rev Bras Ter Intensiva. 2022;34(4):402-409
Abstract
Original ArticleExploring the association of two oxygenators in parallel or in series during respiratory support using extracorporeal membrane oxygenation
Rev Bras Ter Intensiva. 2022;34(4):402-409
DOI 10.5935/0103-507X.20220299-en
Views3ABSTRACT
Objective:
To characterize the pressures, resistances, oxygenation, and decarboxylation efficacy of two oxygenators associated in series or in parallel during venous-venous extracorporeal membrane oxygenation support.
Methods:
Using the results of a swine severe respiratory failure associated with multiple organ dysfunction venous-venous extracorporeal membrane oxygenation support model and mathematical modeling, we explored the effects on oxygenation, decarboxylation and circuit pressures of in-parallel and in-series associations of oxygenators.
Results:
Five animals with a median weight of 80kg were tested. Both configurations increased the oxygen partial pressure after the oxygenators. The return cannula oxygen content was also slightly higher, but the impact on systemic oxygenation was minimal using oxygenators with a high rated flow (~ 7L/minute). Both configurations significantly reduced the systemic carbon dioxide partial pressure. As the extracorporeal membrane oxygenation blood flow increased, the oxygenator resistance decreased initially with a further increase with higher blood flows but with a small clinical impact.
Conclusion:
Association of oxygenators in parallel or in series during venous-venous extracorporeal membrane oxygenation support provides a modest increase in carbon dioxide partial pressure removal with a slight improvement in oxygenation. The effect of oxygenator associations on extracorporeal circuit pressures is minimal.
Keywords:acute respiratory distress syndromeDecarboxylationExtracorporeal membrane oxygenationHypercapniaHypoxiaOxygenatorsSwineSee more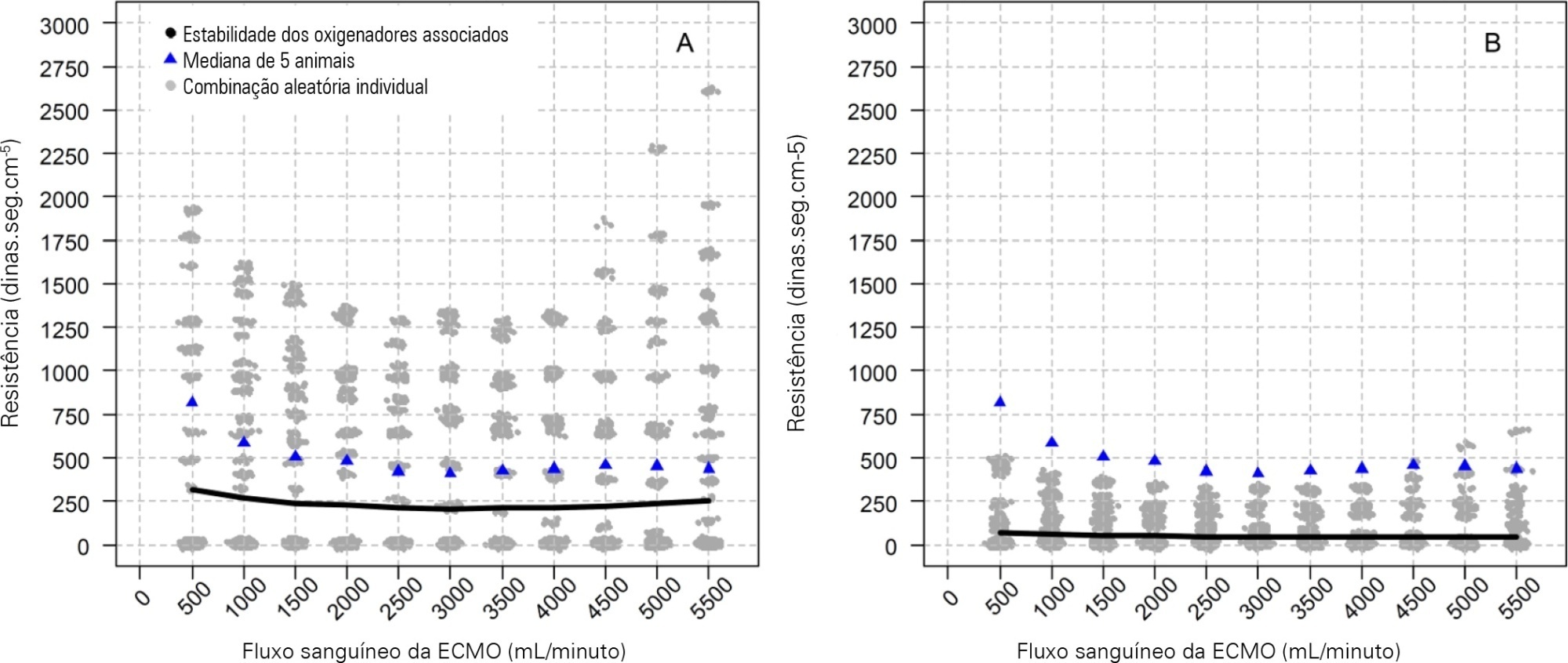
-
Letter to the Editor
The hemoglobin level impact on arterial oxygen saturation during venous-venous-extracorporeal membrane oxygenation support of acute respiratory distress syndrome patients: a mathematical marginal approach
Rev Bras Ter Intensiva. 2022;34(3):393-395
Abstract
Letter to the EditorThe hemoglobin level impact on arterial oxygen saturation during venous-venous-extracorporeal membrane oxygenation support of acute respiratory distress syndrome patients: a mathematical marginal approach
Rev Bras Ter Intensiva. 2022;34(3):393-395
DOI 10.5935/0103-507X.20220465-en
Views1TO THE EDITORHemoglobin (Hb) levels in the range of 7 – 14g/dL have been targeted in extracorporeal membrane oxygenation (ECMO)-supported acute respiratory distress syndrome (ARDS) patients. There is an association between low Hb levels and prolonged duration of mechanical ventilation and bleeding episodes. In contrast, higher Hb levels are associated with lower ECMO blood flow, […]See more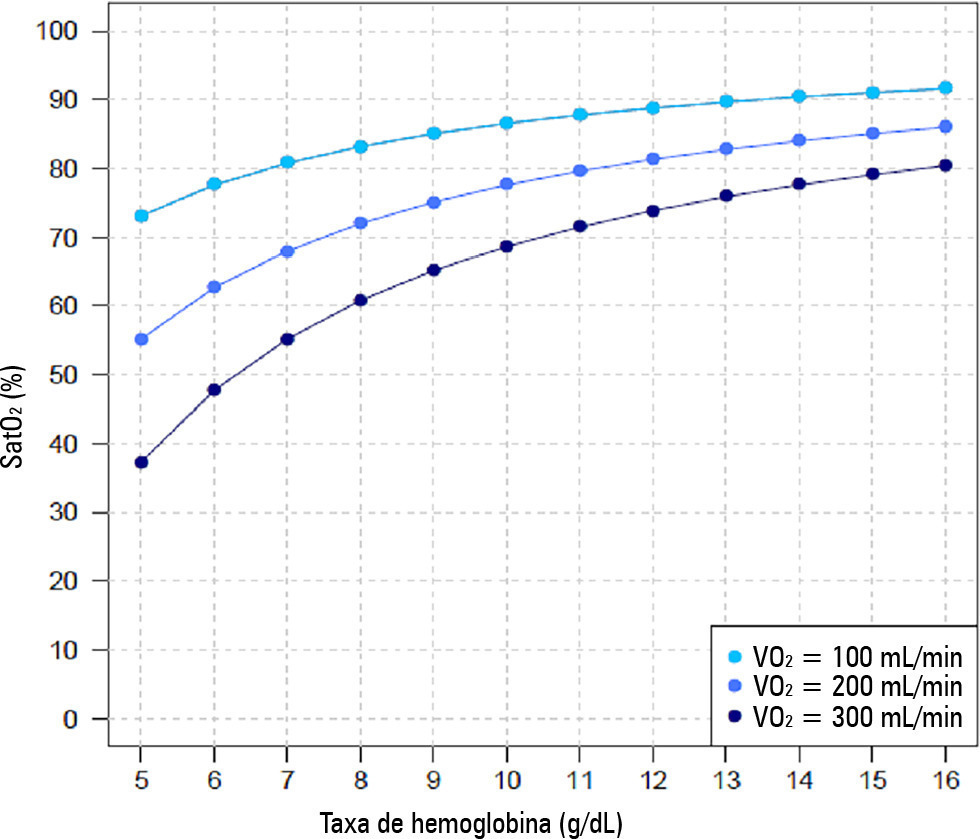
-
Original Article
Comparison of the accuracy of residents, senior physicians and surrogate decision-makers for predicting hospital mortality of critically ill patients
Rev Bras Ter Intensiva. 2022;34(2):220-226
Abstract
Original ArticleComparison of the accuracy of residents, senior physicians and surrogate decision-makers for predicting hospital mortality of critically ill patients
Rev Bras Ter Intensiva. 2022;34(2):220-226
DOI 10.5935/0103-507X.20220019-en
Views1ABSTRACT
Objective:
To compare the predictive performance of residents, senior intensive care unit physicians and surrogates early during intensive care unit stays and to evaluate whether different presentations of prognostic data (probability of survival versus probability of death) influenced their performance.
Methods:
We questioned surrogates and physicians in charge of critically ill patients during the first 48 hours of intensive care unit admission on the patient’s probability of hospital outcome. The question framing (i.e., probability of survival versus probability of death during hospitalization) was randomized. To evaluate the predictive performance, we compared the areas under the ROC curves (AUCs) for hospital outcome between surrogates and physicians’ categories. We also stratified the results according to randomized question framing.
Results:
We interviewed surrogates and physicians on the hospital outcomes of 118 patients. The predictive performance of surrogate decisionmakers was significantly lower than that of physicians (AUC of 0.63 for surrogates, 0.82 for residents, 0.80 for intensive care unit fellows and 0.81 for intensive care unit senior physicians). There was no increase in predictive performance related to physicians’ experience (i.e., senior physicians did not predict outcomes better than junior physicians). Surrogate decisionmakers worsened their prediction performance when they were asked about probability of death instead of probability of survival, but there was no difference for physicians.
Conclusion:
Different predictive performance was observed when comparing surrogate decision-makers and physicians, with no effect of experience on health care professionals’ prediction. Question framing affected the predictive performance of surrogates but not of physicians.
Keywords:Critical illnessDecision MakingDelivery of health careHospitalizationIntensive care unitsInternship and residencyMortalityPrognosisSee more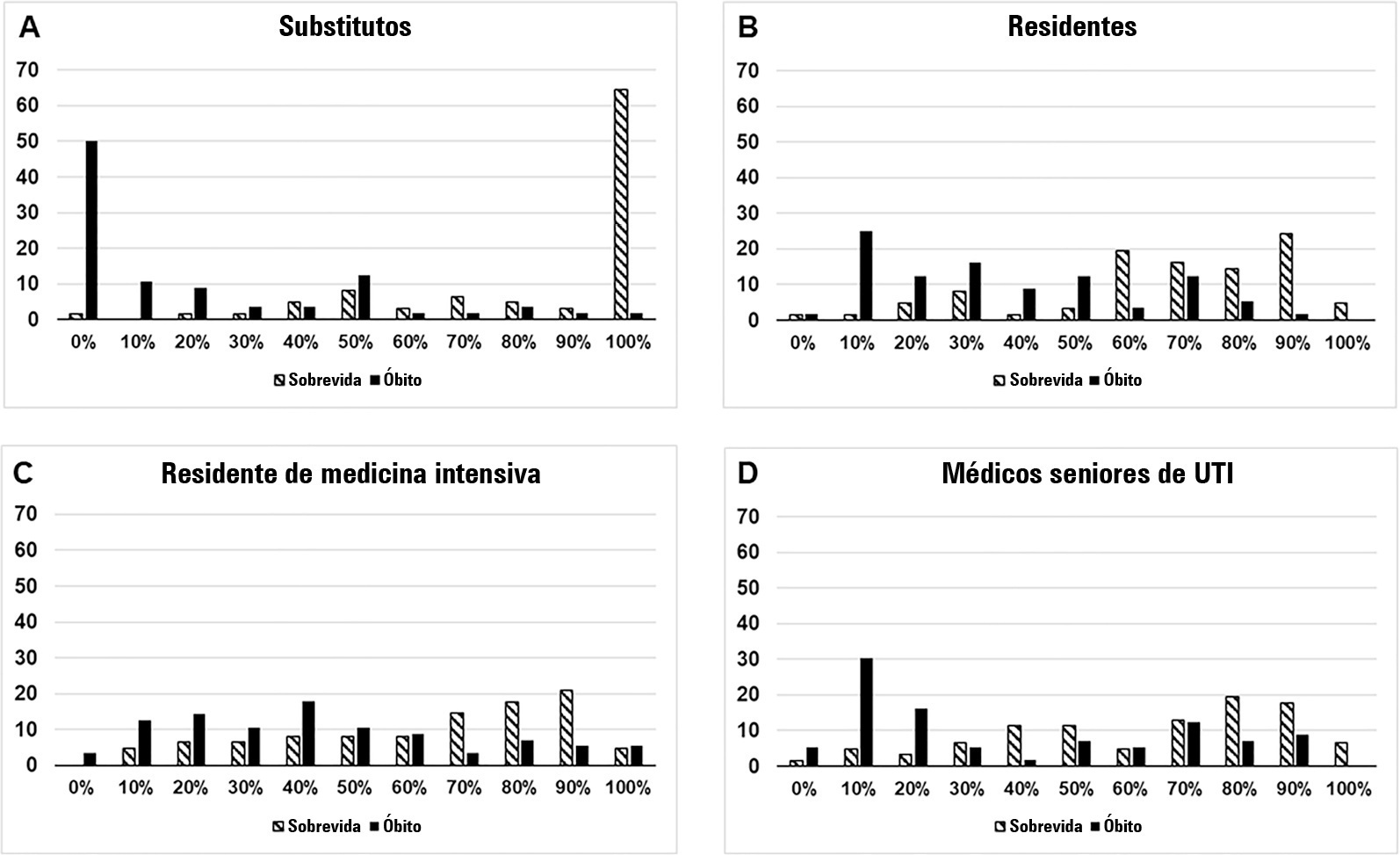
-
Letter to the Editor
Endotracheal intubation in COVID-19 patients in Brazil: a nationwide survey
Rev Bras Ter Intensiva. 2022;34(1):202-204
Abstract
Letter to the EditorEndotracheal intubation in COVID-19 patients in Brazil: a nationwide survey
Rev Bras Ter Intensiva. 2022;34(1):202-204
DOI 10.5935/0103-507X.20220015-en
Views2To the Editor Endotracheal intubation is a life-saving procedure in acute respiratory distress syndrome. However, complications such as hypoxia, hypotension and cardiovascular collapse may occur in almost 40% of the procedures in the intensive care unit (ICU).() Evidence regarding the best practice of endotracheal intubation in this context is scarce, and most data have been […]See more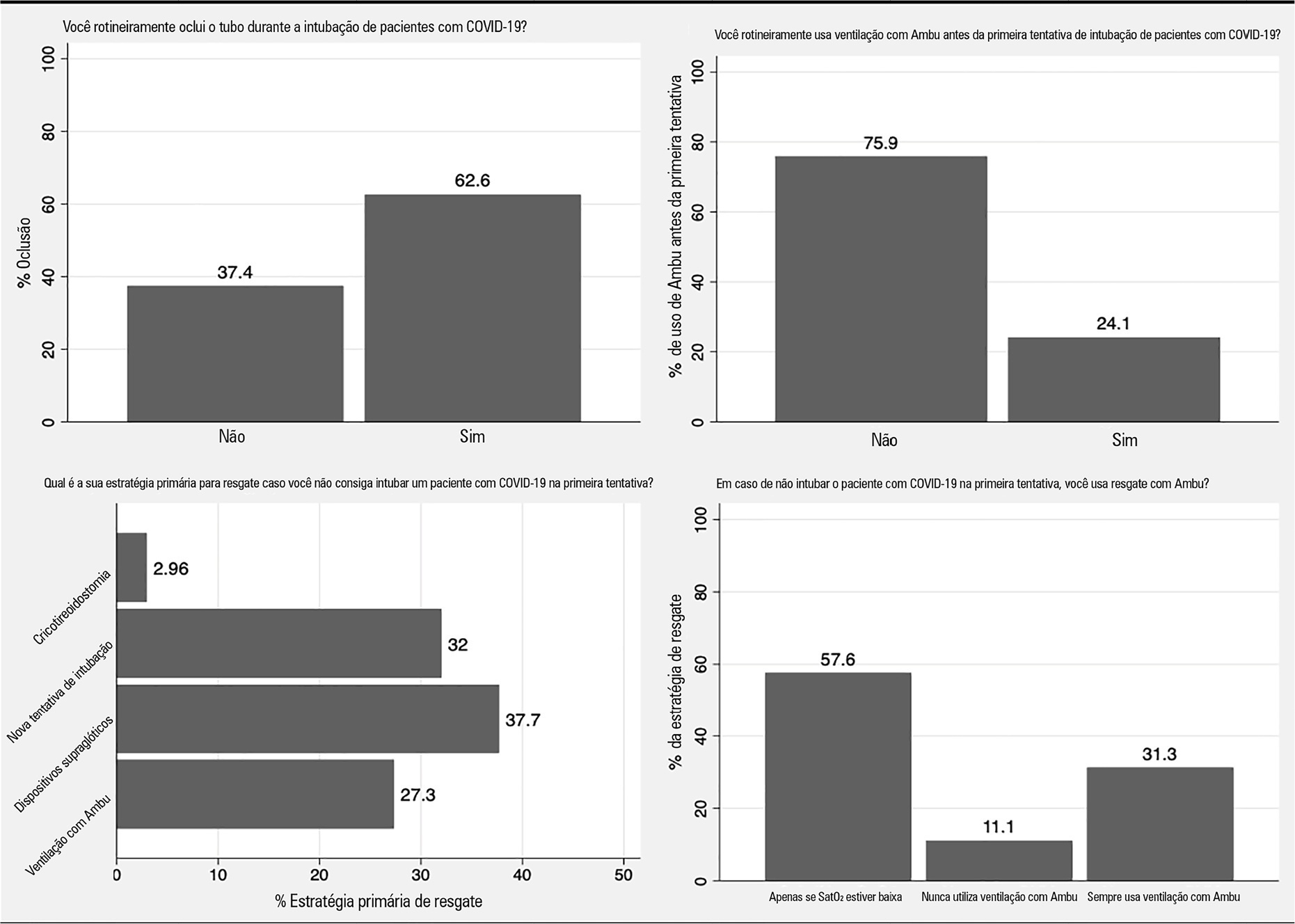
-
Original Article
Bedside clinical data subphenotypes of critically ill COVID-19 patients: a cohort study
Rev Bras Ter Intensiva. 2021;33(2):196-205
Abstract
Original ArticleBedside clinical data subphenotypes of critically ill COVID-19 patients: a cohort study
Rev Bras Ter Intensiva. 2021;33(2):196-205
DOI 10.5935/0103-507X.20210027
Views0See moreAbstract
Objective:
To identify more severe COVID-19 presentations.
Methods:
Consecutive intensive care unit-admitted patients were subjected to a stepwise clustering method.
Results:
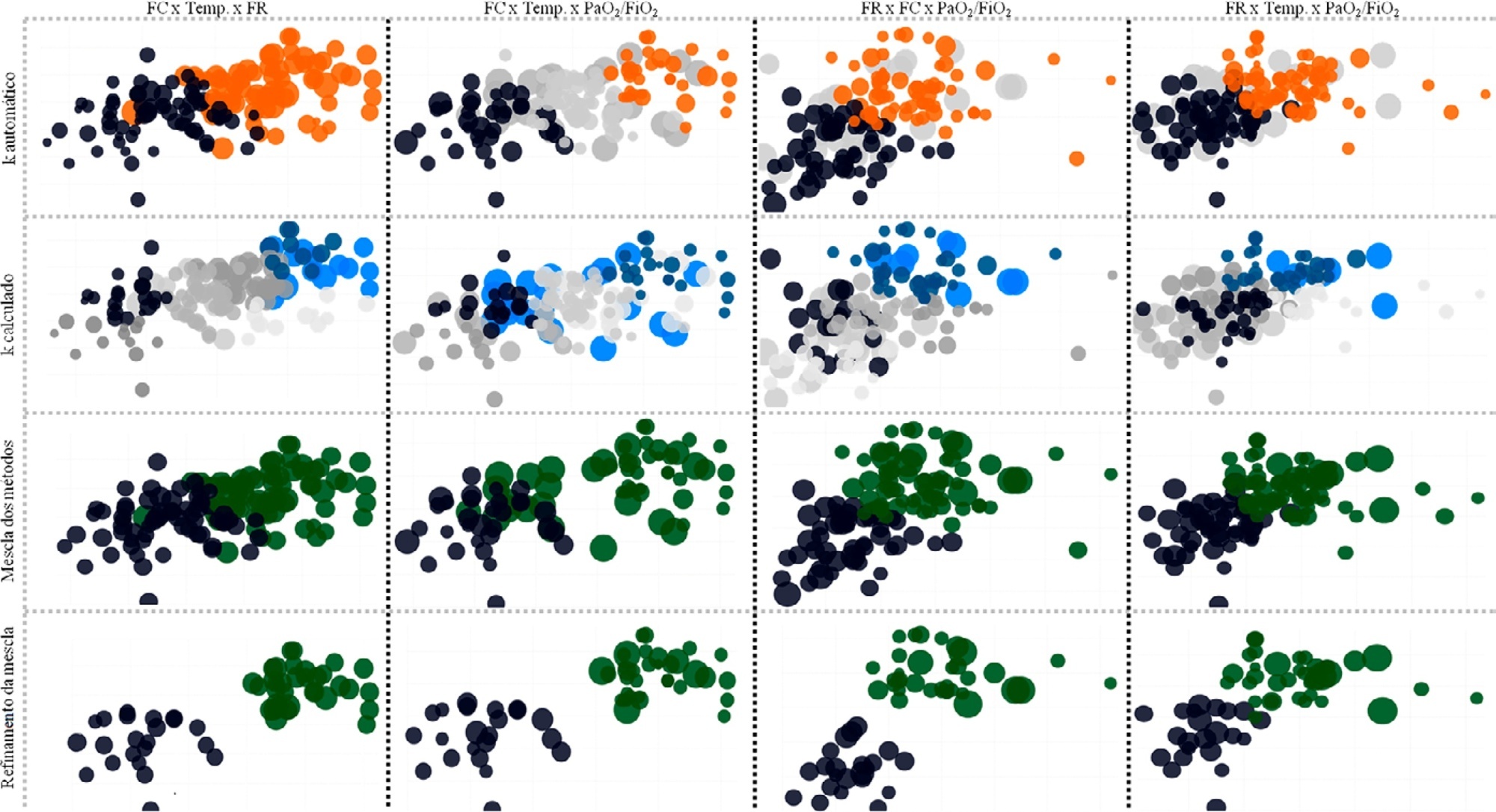
Data from 147 patients who were on average 56 ± 16 years old with a Simplified Acute Physiological Score 3 of 72 ± 18, of which 103 (70%) needed mechanical ventilation and 46 (31%) died in the intensive care unit, were analyzed. From the clustering algorithm, two well-defined groups were found based on maximal heart rate [Cluster A: 104 (95%CI 99 – 109) beats per minute versus Cluster B: 159 (95%CI 155 – 163) beats per minute], maximal respiratory rate [Cluster A: 33 (95%CI 31 – 35) breaths per minute versus Cluster B: 50 (95%CI 47 – 53) breaths per minute], and maximal body temperature [Cluster A: 37.4 (95%CI 37.1 – 37.7)°C versus Cluster B: 39.3 (95%CI 39.1 – 39.5)°C] during the intensive care unit stay, as well as the oxygen partial pressure in the blood over the oxygen inspiratory fraction at intensive care unit admission [Cluster A: 116 (95%CI 99 – 133) mmHg versus Cluster B: 78 (95%CI 63 – 93) mmHg]. Subphenotypes were distinct in inflammation profiles, organ dysfunction, organ support, intensive care unit length of stay, and intensive care unit mortality (with a ratio of 4.2 between the groups).
Conclusion:
Our findings, based on common clinical data, revealed two distinct subphenotypes with different disease courses. These results could help health professionals allocate resources and select patients for testing novel therapies.
Search
Search in:
KEY WORDS
Case reports Child Coronavirus infections COVID-19 Critical care Critical illness Infant, newborn Intensive care Intensive care units Intensive care units, pediatric mechanical ventilation Mortality Physical therapy modalities Prognosis Respiration, artificial Respiratory insufficiency risk factors SARS-CoV-2 Sepsis Septic shock




