You searched for:"Ana Fernandes"
We found (5) results for your search.-
Original Article
Myocardial injury and cardiovascular complications in COVID-19: a cohort study in severe and critical patients
Rev Bras Ter Intensiva. 2022;34(4):443-451
Abstract
Original ArticleMyocardial injury and cardiovascular complications in COVID-19: a cohort study in severe and critical patients
Rev Bras Ter Intensiva. 2022;34(4):443-451
DOI 10.5935/0103-507X.20220440-en
Views1ABSTRACT
Objective:
To characterize myocardial injury and cardiovascular complications and their predictors in severe and critical COVID-19 patients admitted to the intensive care unit.
Methods:
This was an observational cohort study of severe and critical COVID-19 patients admitted to the intensive care unit. Myocardial injury was defined as blood levels of cardiac troponin above the 99th percentile upper reference limit. Cardiovascular events considered were the composite of deep vein thrombosis, pulmonary embolism, stroke, myocardial infarction, acute limb ischemia, mesenteric ischemia, heart failure and arrhythmia. Univariate and multivariate logistic regression or Cox proportional hazard models were used to determine predictors of myocardial injury.
Results:
Of 567 patients with severe and critical COVID-19 admitted to the intensive care unit, 273 (48.1%) had myocardial injury. Of the 374 patients with critical COVID-19, 86.1% had myocardial injury, and also showed more organ dysfunction and higher 28-day mortality (56.6% versus 27.1%, p < 0.001). Advanced age, arterial hypertension and immune modulator use were predictors of myocardial injury. Cardiovascular complications occurred in 19.9% of patients with severe and critical COVID-19 admitted to the intensive care unit, with most events occurring in patients with myocardial injury (28.2% versus 12.2%, p < 0.001). The occurrence of an early cardiovascular event during intensive care unit stay was associated with higher 28-day mortality compared with late or no events (57.1% versus 34% versus 41.8%, p = 0.01).
Conclusion:
Myocardial injury and cardiovascular complications were commonly found in patients with severe and critical forms of COVID-19 admitted to the intensive care unit, and both were associated with increased mortality in these patients.
Keywords:Cardiovascular complicationsCoronavirus infectionsCOVID-19Critical careMyocardial injuryMyocarditisSARS-CoV-2See more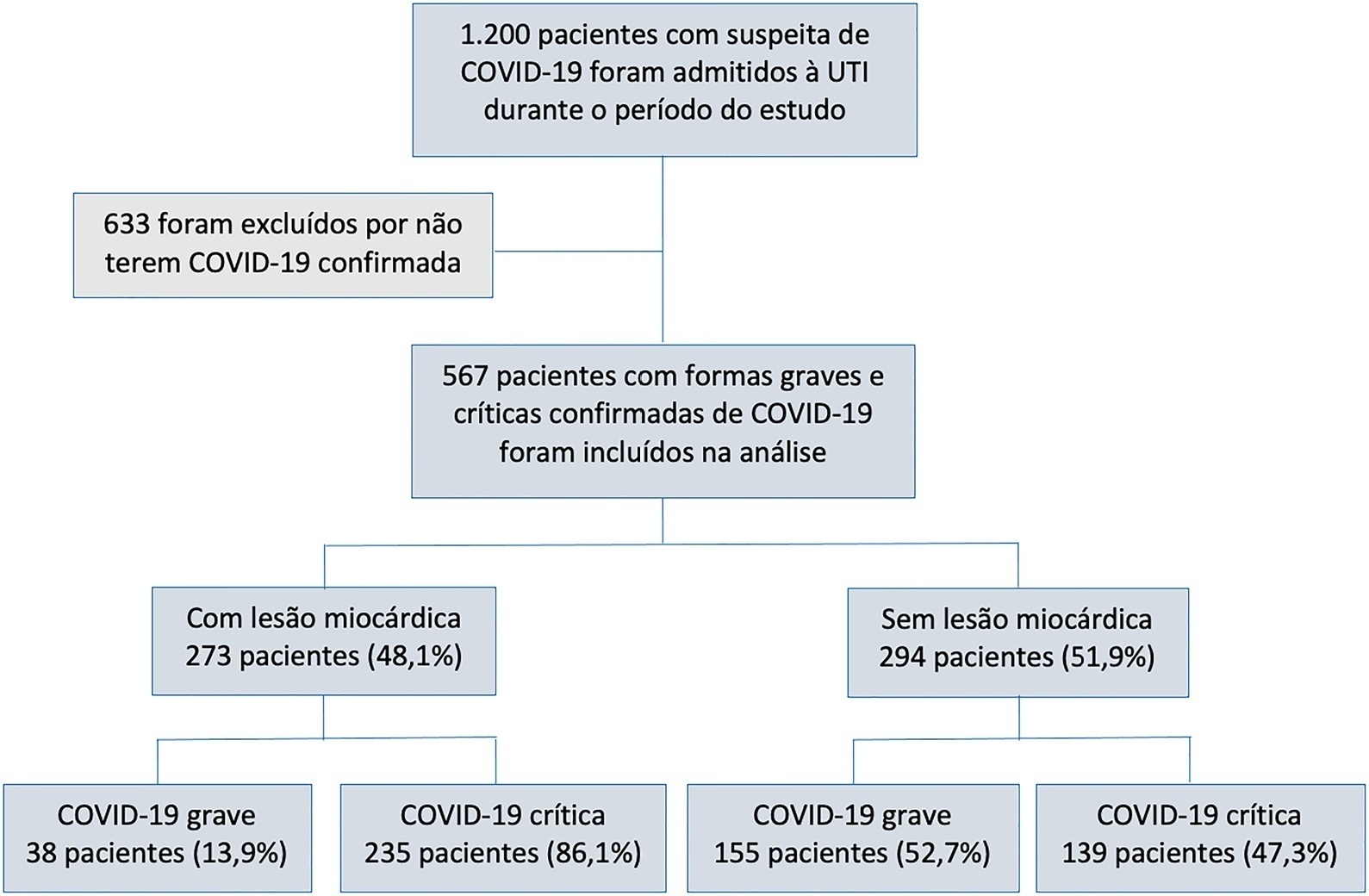
-
Original Article
Rotating nasal masks with nasal prongs reduces the incidence of moderate to severe nasal injury in preterm infants supported by noninvasive ventilation
Rev Bras Ter Intensiva. 2022;34(2):247-254
Abstract
Original ArticleRotating nasal masks with nasal prongs reduces the incidence of moderate to severe nasal injury in preterm infants supported by noninvasive ventilation
Rev Bras Ter Intensiva. 2022;34(2):247-254
DOI 10.5935/0103-507X.20220022-en
Views1ABSTRACT
Objective:
To investigate the association between noninvasive ventilation delivery devices and the incidence of nasal septum injury in preterm infants.
Methods:
This retrospective singlecenter cohort study included preterm infants supported by noninvasive ventilation. The incidence of nasal injury was compared among three groups according to the noninvasive ventilation delivery device (G1 – nasal mask; G2 – binasal prongs; and G3, rotation of nasal mask with prongs). Nasal injury was classified according to the National Pressure Ulcer Advisory Panel as stages 1 – 4. Multivariate regression analyses were performed to estimate relative risks to identify possible predictors associated with medical device-related injuries.
Results:
Among the 300 infants included in the study, the incidence of medical device-related injuries in the rotating group was significantly lower than that in the continuous mask or prong groups (n = 68; 40.48%; p value < 0.01).
Conclusion:
Rotating nasal masks with nasal prongs reduces the incidence of moderate to severe nasal injury in comparison with single devices. The addition of days using noninvasive ventilation seems to contribute to medical device-related injuries, and higher birth weight is a protective factor.
Keywords:InfantMasksNasal septumNoninvasive ventilationNose/injuriesprematureProtective factorsSoft tissue injuriesSee more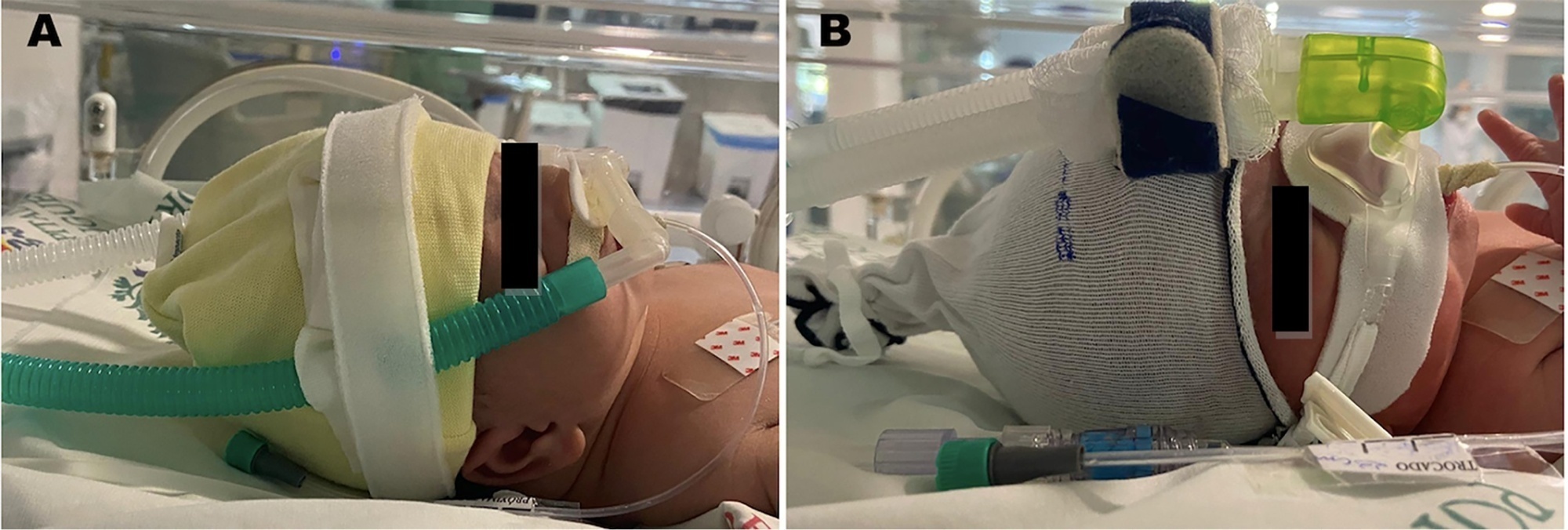
-
Original Article
Resuscitation fluid practices in Brazilian intensive care units: a secondary analysis of Fluid-TRIPS
Rev Bras Ter Intensiva. 2021;33(2):206-218
Abstract
Original ArticleResuscitation fluid practices in Brazilian intensive care units: a secondary analysis of Fluid-TRIPS
Rev Bras Ter Intensiva. 2021;33(2):206-218
DOI 10.5935/0103-507X.20210028
Views1See moreAbstract
Objective:
To describe fluid resuscitation practices in Brazilian intensive care units and to compare them with those of other countries participating in the Fluid-TRIPS.
Methods:
This was a prospective, international, cross-sectional, observational study in a convenience sample of intensive care units in 27 countries (including Brazil) using the Fluid-TRIPS database compiled in 2014. We described the patterns of fluid resuscitation use in Brazil compared with those in other countries and identified the factors associated with fluid choice.
Results:
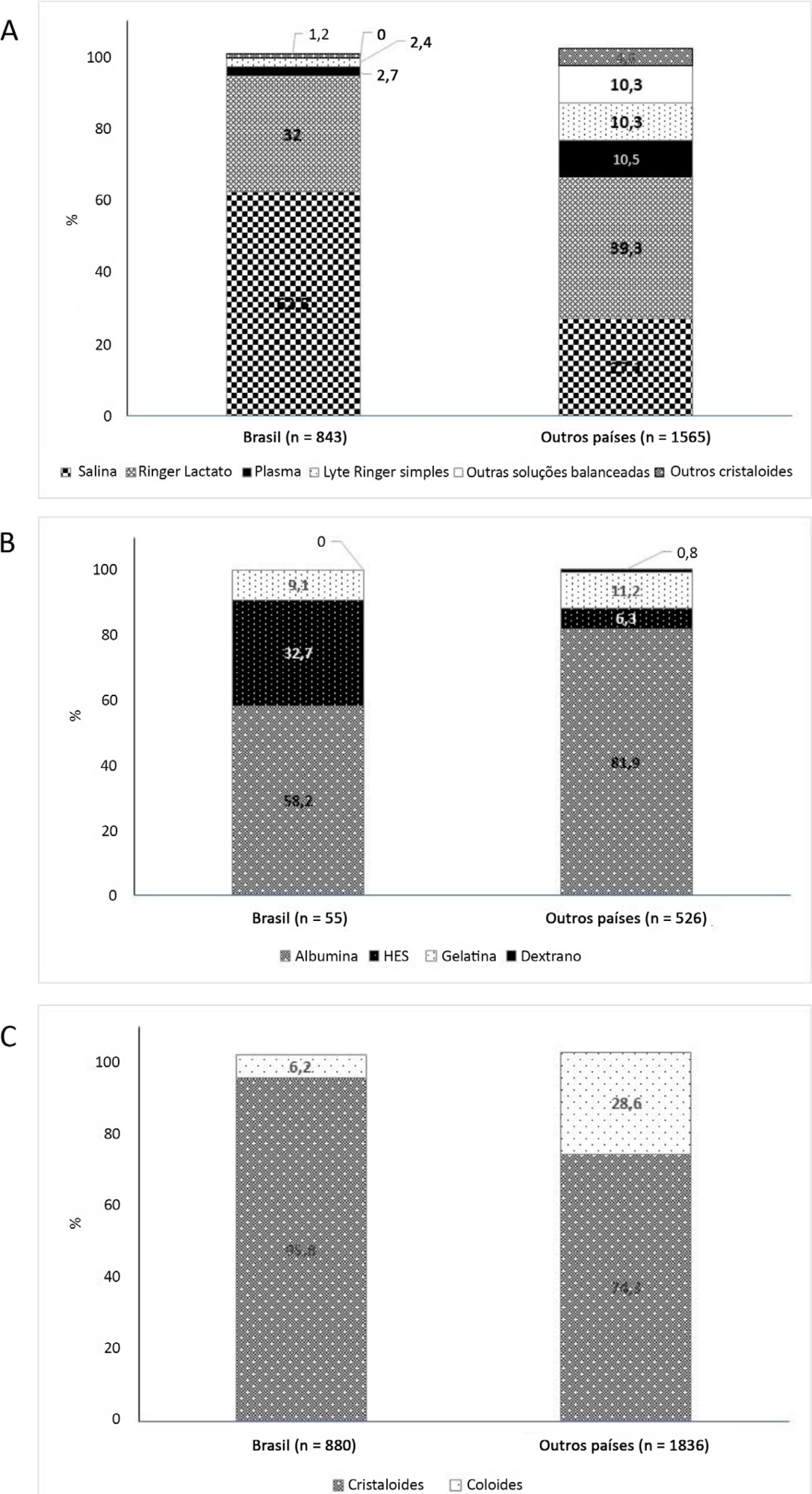
On the study day, 3,214 patients in Brazil and 3,493 patients in other countries were included, of whom 16.1% and 26.8% (p < 0.001) received fluids, respectively. The main indication for fluid resuscitation was impaired perfusion and/or low cardiac output (Brazil: 71.7% versus other countries: 56.4%, p < 0.001). In Brazil, the percentage of patients receiving crystalloid solutions was higher (97.7% versus 76.8%, p < 0.001), and 0.9% sodium chloride was the most commonly used crystalloid (62.5% versus 27.1%, p < 0.001). The multivariable analysis suggested that the albumin levels were associated with the use of both crystalloids and colloids, whereas the type of fluid prescriber was associated with crystalloid use only.
Conclusion:
Our results suggest that crystalloids are more frequently used than colloids for fluid resuscitation in Brazil, and this discrepancy in frequencies is higher than that in other countries. Sodium chloride (0.9%) was the crystalloid most commonly prescribed. Serum albumin levels and the type of fluid prescriber were the factors associated with the choice of crystalloids or colloids for fluid resuscitation.
-
Original Articles
Long-term psychological outcome after discharge from intensive care
Rev Bras Ter Intensiva. 2018;30(1):28-34
Abstract
Original ArticlesLong-term psychological outcome after discharge from intensive care
Rev Bras Ter Intensiva. 2018;30(1):28-34
DOI 10.5935/0103-507X.20180008
Views0ABSTRACT
Objective:
To investigate the longterm psychological outcome in survivors of critical illness after intensive care unit discharge.
Methods:
A prospective cohort of survivors admitted to a mixed intensive care unit between January and September 2010 was evaluated six months and five years after hospital discharge. The Dementia Rating Scale-2, the Hospital Anxiety and Depression Scale, the Posttraumatic stress syndrome 14-questions inventory, the Euro Quality of Life 5 Dimensions (EQ-5-D), and the Visual Analogue Scale (EQ VAS) were assessed at both follow-up periods.
Results:
Of 267 patients, 25 patients were evaluated at 6 months after discharge (62 ± 16 years); 12 (48%) presented cognitive impairment, 6 (24%) anxiety, 4 (16%) depression, and 4 (16%) post-traumatic stress disorder. Among those re-evaluated five years after discharge (n = 17; 65 ± 15 years), the frequency of cognitive impairment dropped from 8 (47%) to 3 (18%) (p = 0.063), due to improvement in these patients over time, and other patients did not acquire any dysfunction after discharge. At five years after discharge, only two patients (12%) reported anxiety, and none had depression or post-traumatic stress disorder. No differences were found between the six-month and five-year follow-ups regarding EQ-5-D and EQ VAS.
Conclusion:
Survivors do not show a progressive decline in cognitive function or quality of life within five years after intensive care unit discharge. Psychopathological symptoms tend to decrease with time.
Keywords:AnxietyCognitive dysfunctionDepressionIntensive care unitsPatient dischargeQuality of lifeStress disorders, post-traumaticSee more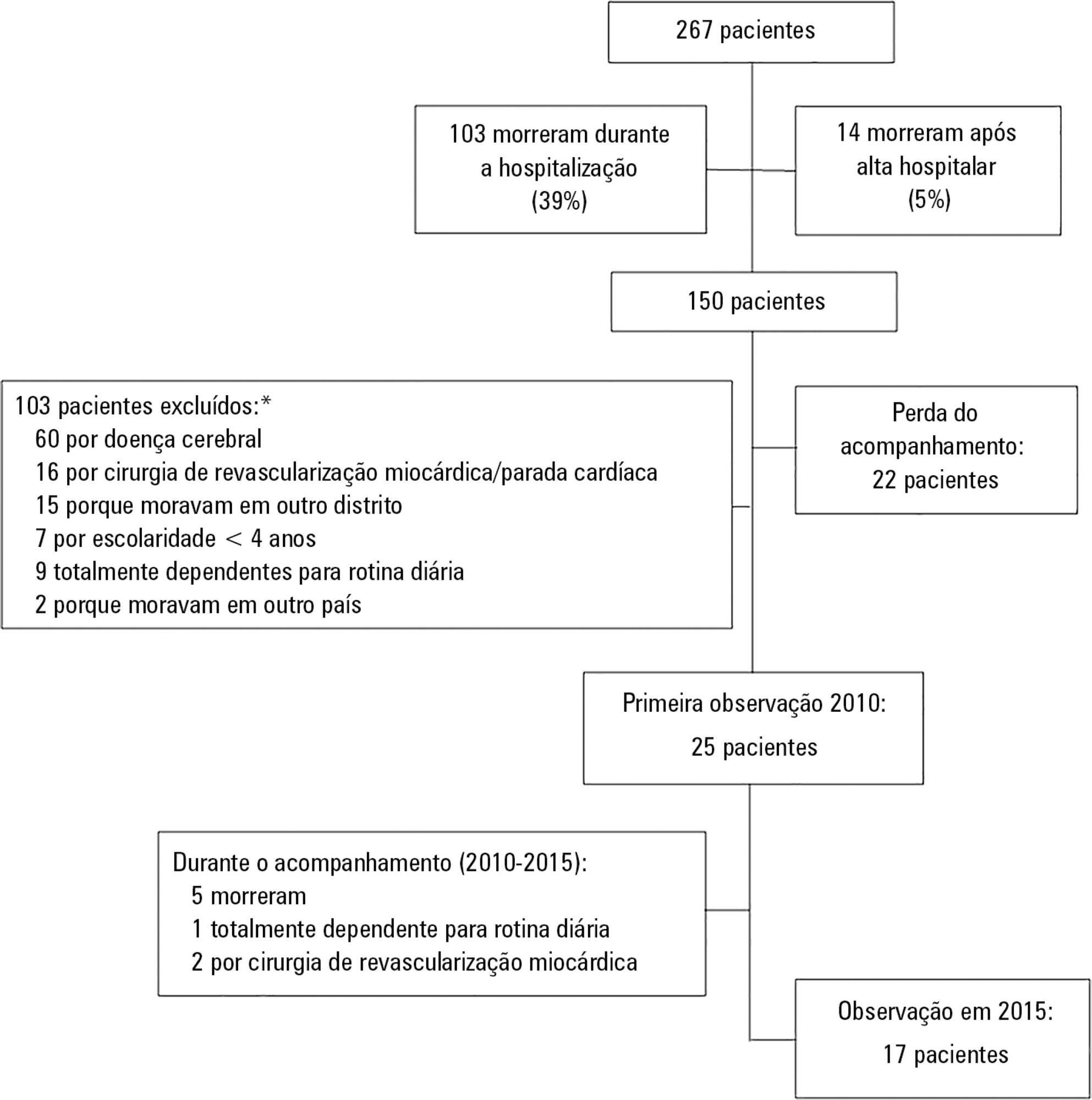
-
Original Articles
Predictors of de novo atrial fibrillation in a non-cardiac intensive care unit
Rev Bras Ter Intensiva. 2018;30(2):166-173
Abstract
Original ArticlesPredictors of de novo atrial fibrillation in a non-cardiac intensive care unit
Rev Bras Ter Intensiva. 2018;30(2):166-173
DOI 10.5935/0103-507X.20180022
Views1See moreABSTRACT
Objective:
To assess the predictors of de novo atrial fibrillation in patients in a non-cardiac intensive care unit.
Methods:
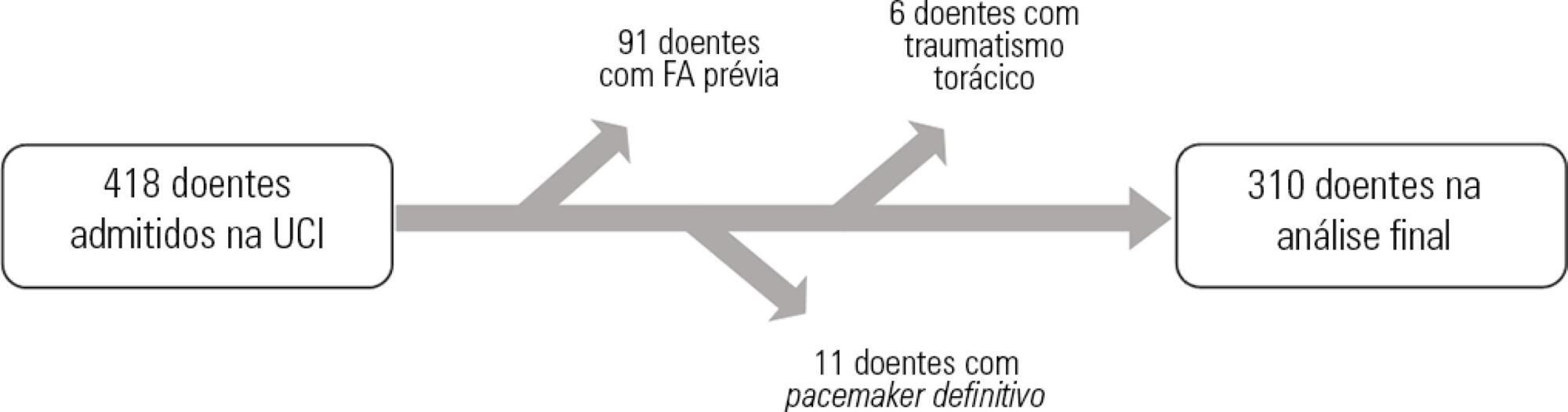
A total of 418 hospitalized patients were analyzed between January and September 2016 in a non-cardiac intensive care unit. Clinical characteristics, interventions, and biochemical markers were recorded during hospitalization. In-hospital mortality and length of hospital stay in the intensive care unit were also evaluated.
Results:
A total of 310 patients were included. The mean age of the patients was 61.0 ± 18.3 years, 49.4% were male, and 23.5% presented de novo atrial fibrillation. The multivariate model identified previous stroke (OR = 10.09; p = 0.016) and elevated levels of pro-B type natriuretic peptide (proBNP, OR = 1.28 for each 1,000pg/mL increment; p = 0.004) as independent predictors of de novo atrial fibrillation. Analysis of the proBNP receiver operating characteristic curve for prediction of de novo atrial fibrillation revealed an area under the curve of 0.816 (p < 0.001), with a sensitivity of 65.2% and a specificity of 82% for proBNP > 5,666pg/mL. There were no differences in mortality (p = 0.370), but the lengths of hospital stay (p = 0.002) and stay in the intensive care unit (p = 0.031) were higher in patients with de novo atrial fibrillation.
Conclusions:
A history of previous stroke and elevated proBNP during hospitalization were independent predictors of de novo atrial fibrillation in the polyvalent intensive care unit. The proBNP is a useful and easy- and quick-access tool in the stratification of atrial fibrillation risk.
Search
Search in:
KEY WORDS
Case reports Child Coronavirus infections COVID-19 Critical care Critical illness Extracorporeal membrane oxygenation Infant, newborn Intensive care Intensive care units Intensive care units, pediatric mechanical ventilation Mortality Physical therapy modalities Prognosis Respiration, artificial Respiratory insufficiency risk factors SARS-CoV-2 Sepsis




