Abstract
Rev Bras Ter Intensiva. 2011;23(1):36-40
DOI 10.1590/S0103-507X2011000100007
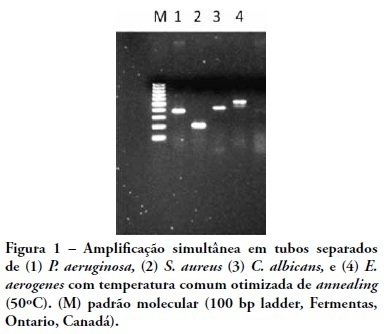
INTRODUCTION: Sepsis is a systemic inflammatory response related to high mortality rates in the hospital environment. Delayed etiological diagnosis and inadequate antimicrobial therapy are associated with treatment failures. Molecular tests based on polymerase chain reaction are regarded as faster and more accurate procedures than culture techniques for microbial identification, providing a higher rate of therapeutic success. OBJECTIVE: To develop a panel of primers for DNA fragments of sepsis-related microorganisms. METHODS: Primers for amplification of Enterobacter spp., Escherichia coli, Pseudomonas aeruginosa, Staphylococcus aureus and Candida spp. were designed and tested for sensitivity and specificity on the basis of their respective standard strains. RESULTS: The intended specificity was obtained for P. aeruginosa, S. aureus and Candida spp primers. Sensitivity tests showed a threshold for detection from 5 ng to 500 fg in blood samples contaminated with microbial DNA. CONCLUSIONS: The molecular panel presented offers the advantage of a flexible 'open' system when compared to other multiplex detection methods.
Abstract
Rev Bras Ter Intensiva. 2011;23(1):41-48
DOI 10.1590/S0103-507X2011000100008
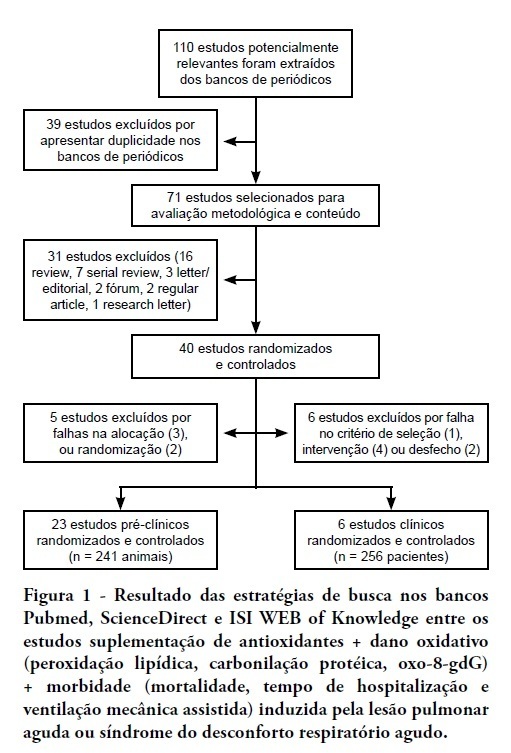
OBJECTIVE: This meta-analysis was performed to evaluate the evidence supporting antioxidant supplementation as an adjunct therapy to prevent oxidative damage and improve the clinical outcomes (mortality, length of hospital stay and duration of mechanical ventilation). METHODS: The search strategy for randomized controlled trials (RCTs) involved the participation of two researchers who independently assessed the methodological quality of each full-text article that was available in the PubMed, ISI WEB of Knowledge and ScienceDirect databases. RESULTS: We extracted 110 studies from the past 10 years, but only 30 articles met the methodological criteria (RCT, blinded and statistically significant results), for a total of 241 animals and 256 patients. This study found an odds ratio (OR) of 0.45 [95% confidence interval (CI): 0.26 to 0.79] for death in the experimental group compared with placebo (six trials, n = 256), an OR of 0.46 [95% CI: 0.26 to 0.87] for hospitalization time and an OR of 0.63 [95% CI: 0.35 to 1.12] for mechanical ventilation time between groups. CONCLUSION: Conflicting evidence makes it impossible to recommend the routine use of antioxidant supplementation in critically ill patients.
Abstract
Rev Bras Ter Intensiva. 2011;23(1):49-55
DOI 10.1590/S0103-507X2011000100009
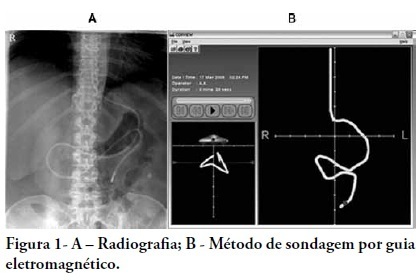
OBJECTIVE: Appropriate nutritional support is important to the outcomes of critically ill patients. However, a significant portion of these patients experience intestinal motility problems. Administration of enteral nutrition by means of tubes placed in the post-pyloric position has been suggested to improve the nutrition tolerance. The aim of this study was to compare the rate of successful post-pyloric placement using a real-time electromagnetic positioning device to the success rate using the conventional placement method. METHODS: This was a prospective, randomized and controlled study, conducted in a tertiary hospital over a period of three months. The patients were randomized to one of two groups: electromagnetically guided system group, whose patients underwent real-time monitoring of post-pyloric tube placement; or the control group, whose patients underwent tube placment using to the conventional blinded technique. The rates of successful post-pyloric placement and the procedure times were assessed and compared between the groups. RESULTS: Thirty-seven patients were enrolled, 18 in the electromagnetic group and 19 in the control group. The final tube position was evaluated using radiography. The electromagnetic guided group showed better success rates and shorter procedure times when compared to the control group. Additionally, in the electromagnetic guided group, higher pH values were found in the fluids aspirated from the probe, suggesting successful postpyloric placement. CONCLUSION: The electromagnetically guided method provided better placement accuracy than did the conventional technique.
Abstract
Rev Bras Ter Intensiva. 2011;23(1):56-61
DOI 10.1590/S0103-507X2011000100010
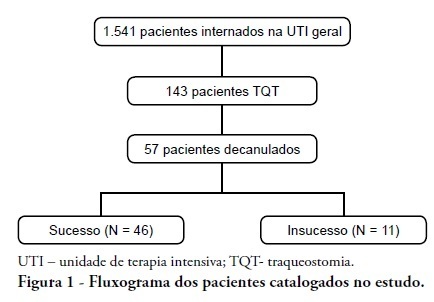
INTRODUCTION: Tracheostomy is probably the most common surgical procedure in critically ill patients and is generally performed to facilitate mechanical ventilation weaning. Evidence-based guidelines have confirmed the benefits of tracheostomy weaning protocols and of the physiotherapists engagement in this process; however, no consensus decannulation criteria are currently available. Therefore, this study aimed to evaluate the influence of peripheral muscle strength and other indicators on decannulation success. METHODS: This was an observational retrospective study that analyzed the medical records of patients admitted to the medical and surgical intensive care unit of Hospital Agamenon Magalhães between March 2007 and August 2009. Respiratory and peripheral muscle strengths were evaluated in decannulated patients. RESULTS: Overall, 1,541 patients were evaluated, 143 of which had been tracheostomized, and only 57 of which had been decannulated. Forty-six patients had a satisfactory decannulation outcome, while 11 had decannulation failure, requiring the return to an artificial airway within 2 weeks. The calculated Medical Research Council peripheral muscle strength score was significantly lower for the failure group than for the successful decannulation group (28.33 ± 15.31 vs. 41.11 ± 11.52; P = 0.04). Scores above or equal 26 had 94.4% sensitivity and 50.0% specificity for the decannulation outcome, with an area under the ROC curve of 0.7593. In addition, white blood cell counts were higher in decannulation failure group patients (14,070 ± 3,073 vs. 10,520 ± 3,402 cells/μL; P = 0.00). CONCLUSION: This study has shown that peripheral muscle strength and blood leucocyte counts evaluated on the day of decannulation may influence the tracheostomy decannulation success rate.
Abstract
Rev Bras Ter Intensiva. 2011;23(1):6-12
DOI 10.1590/S0103-507X2011000100003
Sepsis is a very frequent condition and causes high mortality rates and healthcare costs; it is the main cause of death in intensive care units. Clear, improved prognosis was shown for early diagnosed and treated patients. Treatment guidelines are fundamental for appropriate therapy. It is clear that hypoperfusion patients should be hemodynamically optimized; therefore, recognition of hypoperfusion signs is one of the main therapeutic steps. This guideline discusses the current literature and available data regarding the evaluation of hemodynamic parameters.
Abstract
Rev Bras Ter Intensiva. 2011;23(1):62-67
DOI 10.1590/S0103-507X2011000100011
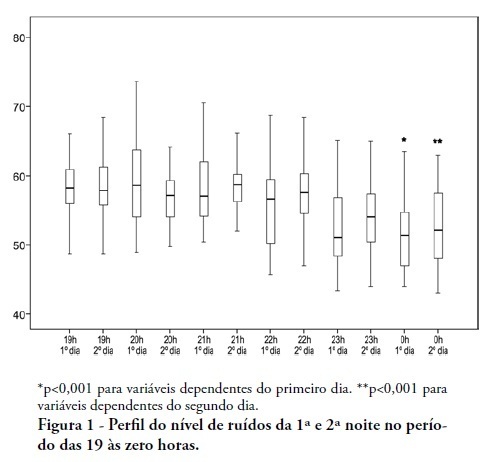
OBJECTIVES: To identify the main causes of stress in patients staying in a coronary unit and to assess the influence of noise levels on their perception of stress. METHODS: This was a prospective, descriptive and quantitative study conducted between June and November 2009 in the Coronary Unit of the Hospital de Clínicas da Universidade Estadual de Campinas. The Intensive Care Unit Environmental Stressor Scale was used on the first, second and third days of hospitalization to identify stressors. The noise level was measured on the first and second nights using an Instrutherm DEC-460 decibel meter. RESULTS: Overall, 32 clinical heart disease patients were included. The median Intensive Care Unit Environmental Stressor Scale scores were 67.5, 60.5 and 59.5 for the first, second and third days, respectively. The differences were not statistically significant. The highest noise level (a median of 58.7 dB) was detected on the second night at 9:00 pm; the lowest level (51.5 dB) was measured on the first night at 12:00 am. In a multiple linear regression model, the first-night noise level had a 33% correlation with the second-day stress scale score, and for the second night, the correlation with the third-day stress scale score was 32.8% (p = 0.001). CONCLUSION: Patients admitted into a coronary unit have an increased perception of stress. Higher noise levels are also responsible for the perception of stress in these patients.
Abstract
Rev Bras Ter Intensiva. 2011;23(1):68-77
DOI 10.1590/S0103-507X2011000100012
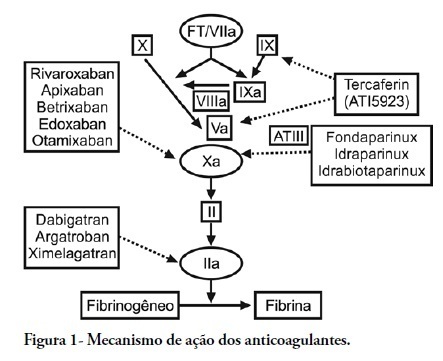
Thromboembolic events commonly occur in critically ill patients, and although they do not consistently present with specific signs and symptoms, they are associated with high morbity and mortality. Antithrombotic agents are the mainstay of the prevention and treatment of venous thromboembolism, and they are also used for stroke prevention in atrial fibrillation, embolism prevention in heart failure, and anticoagulation of prosthetic valves. These drugs have been combined with antiplatelet therapy for the prevention of secondary acute coronary syndrome. Antithrombotic agents such as Aspirin, clopidogrel, vitamin K antagonists and fondaparinux, an indirect Factor Xa inhibitor, are already incorporated into our clinical practice. New small-molecule, selective Factor Xa and thrombin inhibitors that simultaneously inhibit free plasma and clot-associated factor activities have received considerable attention recently. These new oral anticoagulants are in various phases of clinical development. dabigatran, rivaroxaban and apixaban are in more advanced phases of clinical development and are already available in a number of countries. This review article highlights the studies describing the use of these three anticoagulants in an intensive care setting.