You searched for:"Cassiano Teixeira"
We found (44) results for your search.-
Letters to the Editor
The sex gap among visitors during flexible intensive care unit visiting hours
Rev Bras Ter Intensiva. 2019;31(4):592-593
Abstract
Letters to the EditorThe sex gap among visitors during flexible intensive care unit visiting hours
Rev Bras Ter Intensiva. 2019;31(4):592-593
DOI 10.5935/0103-507X.20190089
Views0Dear Editor, Flexible intensive care unit (ICU) visiting hours are increasingly recognized as a means of enhancing patient- and family-centered care.(,) In addition to being safe and associated with better patient and family outcomes,(,) flexible visiting hours are an important approach to acknowledging and showing respect for the patient-family relationship during the course of critical […]See more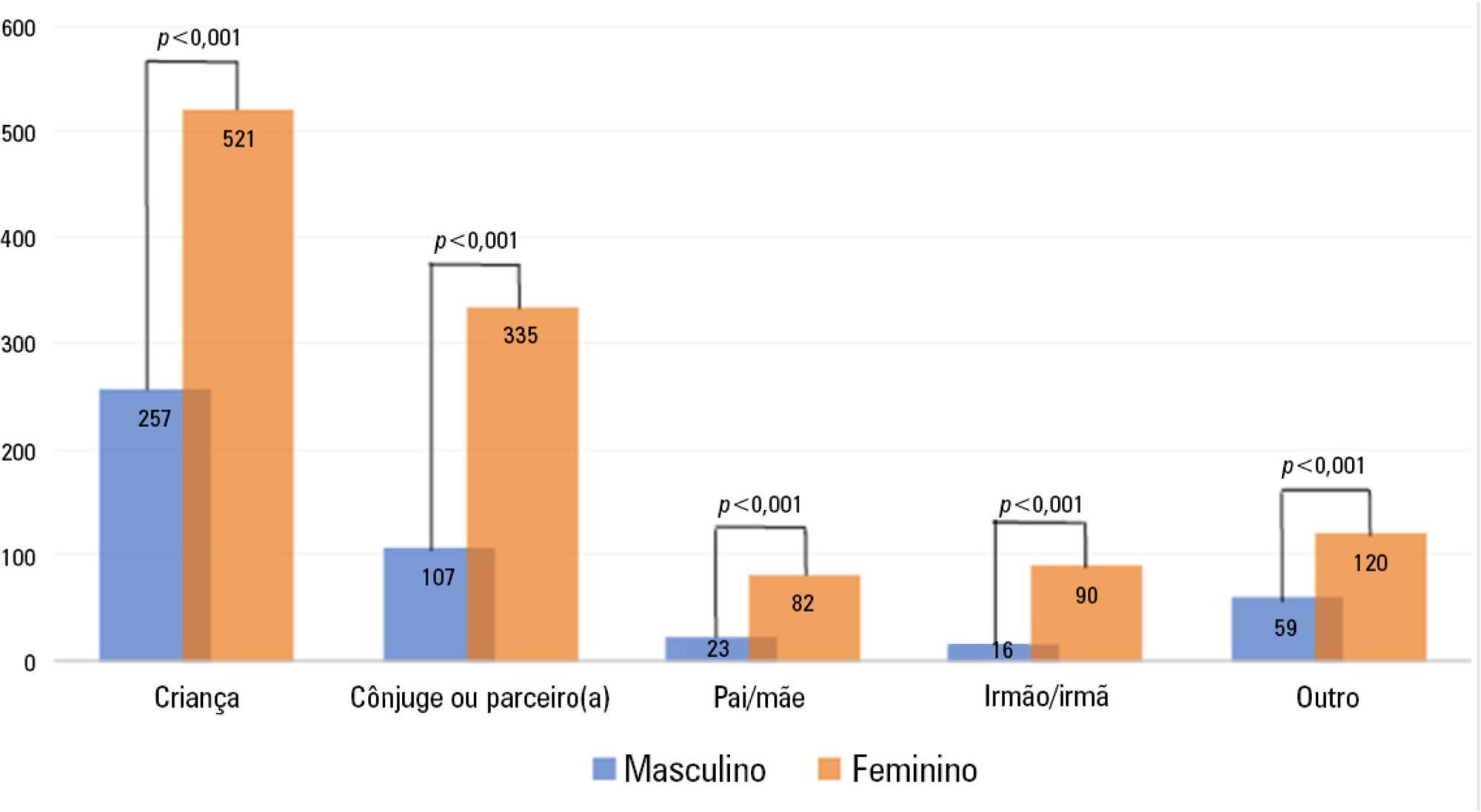
-
Letters to the Editor
To: The Perme scale score as a predictor of functional status and complications after discharge from the intensive care unit in patients undergoing liver transplantation
Rev Bras Ter Intensiva. 2019;31(4):598-599
Abstract
Letters to the EditorTo: The Perme scale score as a predictor of functional status and complications after discharge from the intensive care unit in patients undergoing liver transplantation
Rev Bras Ter Intensiva. 2019;31(4):598-599
DOI 10.5935/0103-507X.20190082
Views0To the Editor I would like to congratulate the authors responsible for the article entitled “The Perme scale score as a predictor of functional status and complications after discharge from the intensive care unit in patients undergoing liver transplantation”, the topic of which is extremely relevant to the academic community.()[…]See more -
Original Articles
Association between electromyographical findings and intensive care unit mortality among mechanically ventilated acute respiratory distress syndrome patients under profound sedation
Rev Bras Ter Intensiva. 2019;31(4):497-503
Abstract
Original ArticlesAssociation between electromyographical findings and intensive care unit mortality among mechanically ventilated acute respiratory distress syndrome patients under profound sedation
Rev Bras Ter Intensiva. 2019;31(4):497-503
DOI 10.5935/0103-507X.20190087
Views0ABSTRACT
Objective:
To evaluate whether electromyographical findings could predict intensive care unit mortality among mechanically ventilated septic patients under profound sedation.
Methods:
A prospective cohort study that consecutively enrolled moderate-severe acute respiratory distress syndrome (partial pressure of oxygen/fraction of inspired oxygen < 200) patients who were ≥ 18 years of age, dependent on mechanical ventilation for ≥ 7 days, and under profound sedation (Richmond Agitation Sedation Scale ≤ -4) was conducted. Electromyographic studies of the limbs were performed in all patients between the 7th and the 10th day of mechanical ventilation. Sensory nerve action potentials were recorded from the median and sural nerves. The compound muscle action potentials were recorded from the median (abductor pollicis brevis muscle) and common peroneal (extensor digitorum brevis muscle) nerves.
Results:
Seventeen patients were enrolled during the seven months of the study. Nine patients (53%) had electromyographic signs of critical illness myopathy or neuropathy. The risk of death during the intensive care unit stay was increased in patients with electromyographical signs of critical illness myopathy or neuropathy in comparison to those without these diagnostics (77.7% versus 12.5%, log-rank p = 0.02).
Conclusion:
Electromyographical signs of critical illness myopathy or neuropathy between the 7th and the 10th day of mechanical ventilation may be associated with intensive care unit mortality among moderate-severe acute respiratory distress syndrome patients under profound sedation, in whom clinical strength assessment is not possible.
Keywords:Critical illnessElectromyographyIntensive care unitsMortalityPolyneuropathiesPrognosisRespiration, artificialRespiratory distress syndromesedationSee more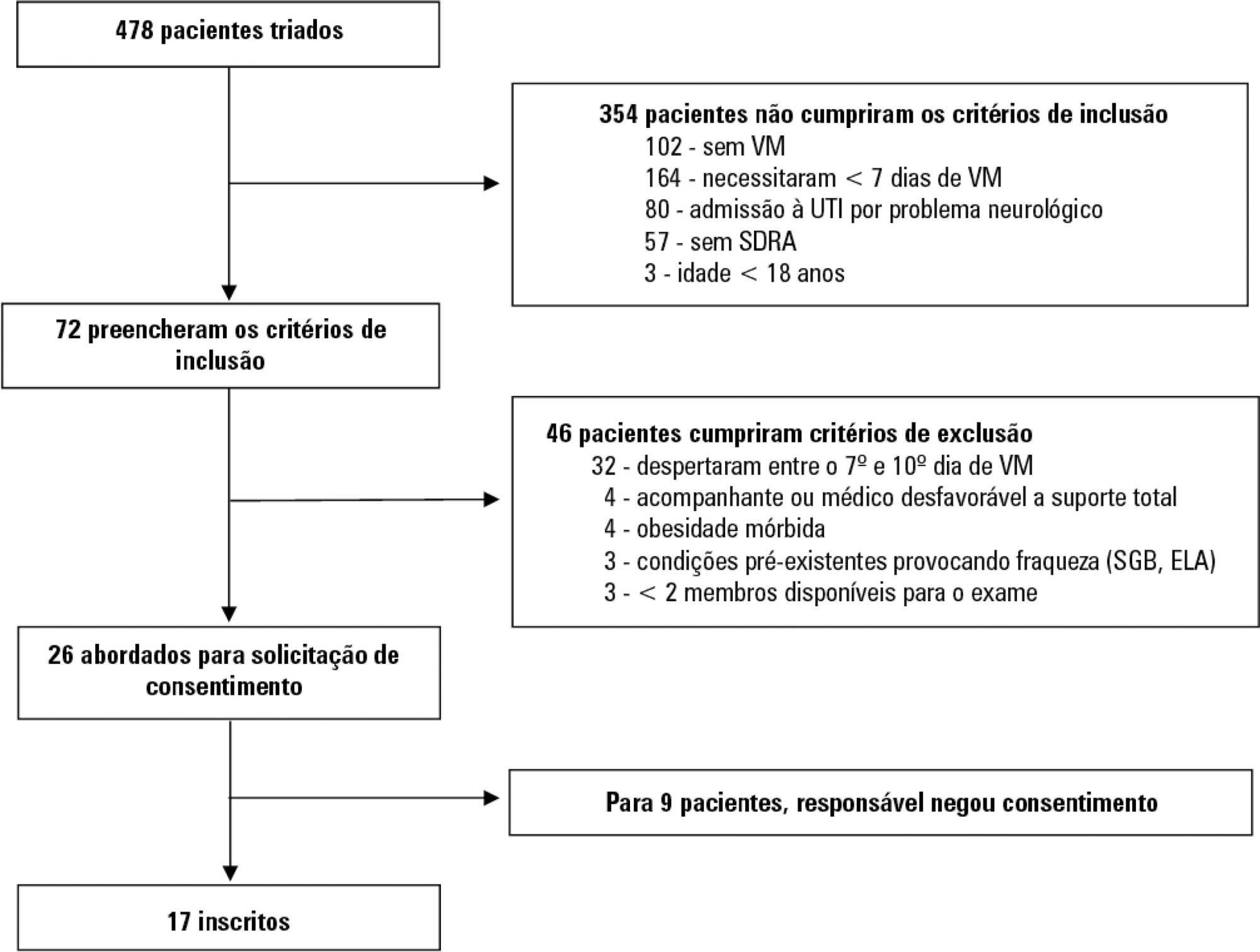
-
Review Articles
How to discuss about do-not-resuscitate in the intensive care unit?
Rev Bras Ter Intensiva. 2019;31(3):386-392
Abstract
Review ArticlesHow to discuss about do-not-resuscitate in the intensive care unit?
Rev Bras Ter Intensiva. 2019;31(3):386-392
DOI 10.5935/0103-507X.20190051
Views0See moreAbstract
The improvement in cardiopulmonary resuscitation quality has reduced the mortality of individuals treated for cardiac arrest. However, survivors have a high risk of severe brain damage in cases of return of spontaneous circulation. Data suggest that cases of cardiac arrest in critically ill patients with non-shockable rhythms have only a 6% chance of returning of spontaneous circulation, and of these, only one-third recover their autonomy. Should we, therefore, opt for a procedure in which the chance of survival is minimal and the risk of hospital death or severe and definitive brain damage is approximately 70%? Is it worth discussing patient resuscitation in cases of cardiac arrest? Would this discussion bring any benefit to the patients and their family members? Advanced discussions on do-not-resuscitate are based on the ethical principle of respect for patient autonomy, as the wishes of family members and physicians often do not match those of patients. In addition to the issue of autonomy, advanced discussions can help the medical and care team anticipate future problems and, thus, better plan patient care. Our opinion is that discussions regarding the resuscitation of critically ill patients should be performed for all patients within the first 24 to 48 hours after admission to the intensive care unit.
-
Letters to the Editor
Mortality, morbidity, and quality-of-life outcomes of patients requiring ≥ 14 days of mechanical ventilation: a 12-month post-intensive-care-unit cohort study
Rev Bras Ter Intensiva. 2019;31(3):425-427
Abstract
Letters to the EditorMortality, morbidity, and quality-of-life outcomes of patients requiring ≥ 14 days of mechanical ventilation: a 12-month post-intensive-care-unit cohort study
Rev Bras Ter Intensiva. 2019;31(3):425-427
DOI 10.5935/0103-507X.20190046
Views0Dear Editor, Intensive care unit (ICU) survivors suffer significant morbidity,(,) and longer mechanical ventilation (MV)-dependency increases the probability that these subjects will suffer a “persistent inflammation-immunosuppression and catabolism syndrome”.(–) These patients have ongoing inflammation, manageable organ failure, ongoing protein catabolism, and poor nutrition, leading to cachexia; poor wound healing and immunosuppression with increased susceptibility to […]See more -
Letter to the Editor
Multiple organ dysfunction – we must take a closer look at muscle wasting!
Rev Bras Ter Intensiva. 2019;31(2):269-270
Abstract
Letter to the EditorMultiple organ dysfunction – we must take a closer look at muscle wasting!
Rev Bras Ter Intensiva. 2019;31(2):269-270
DOI 10.5935/0103-507X.20190021
Views1To the editor Organ dysfunction is quantified routinely by scores such as: the Sequential Organ Failure Assessment (SOFA) score, the Multiple Organ Dysfunction Score (MODS), and the Logistic Organ Dysfunction Score (LODS).() Once the number of organs failure is associated with intensive care unit (ICU) and hospital-mortality, these scores are helpful to only predict acute […]See more -
Original Article
Quality of life after intensive care unit: a multicenter cohort study protocol for assessment of long-term outcomes among intensive care survivors in Brazil
Rev Bras Ter Intensiva. 2018;30(4):405-413
Abstract
Original ArticleQuality of life after intensive care unit: a multicenter cohort study protocol for assessment of long-term outcomes among intensive care survivors in Brazil
Rev Bras Ter Intensiva. 2018;30(4):405-413
DOI 10.5935/0103-507X.20180063
Views0ABSTRACT
Objective:
To establish the prevalence of physical, cognitive and psychiatric disabilities, associated factors and their relationship with the qualities of life of intensive care survivors in Brazil.
Methods:
A prospective multicenter cohort study is currently being conducted at 10 adult medical-surgical intensive care units representative of the 5 Brazilian geopolitical regions. Patients aged ≥ 18 years who are discharged from the participating intensive care units and stay 72 hours or more in the intensive care unit for medical or emergency surgery admissions or 120 hours or more for elective surgery admissions are consecutively included. Patients are followed up for a period of one year by means of structured telephone interviews conducted at 3, 6 and 12 months after discharge from the intensive care unit. The outcomes are functional dependence, cognitive dysfunction, anxiety and depression symptoms, posttraumatic stress symptoms, health-related quality of life, rehospitalization and long-term mortality.
Discussion:
The present study has the potential to contribute to current knowledge of the prevalence and factors associated with postintensive care syndrome among adult intensive care survivors in Brazil. In addition, an association might be established between postintensive care syndrome and health-related quality of life.
Keywords:AnxietyCognitive dysfunctionCritical care outcomesDepressionDisabled personsQuality of lifeStress disorders, PosttraumaticSee more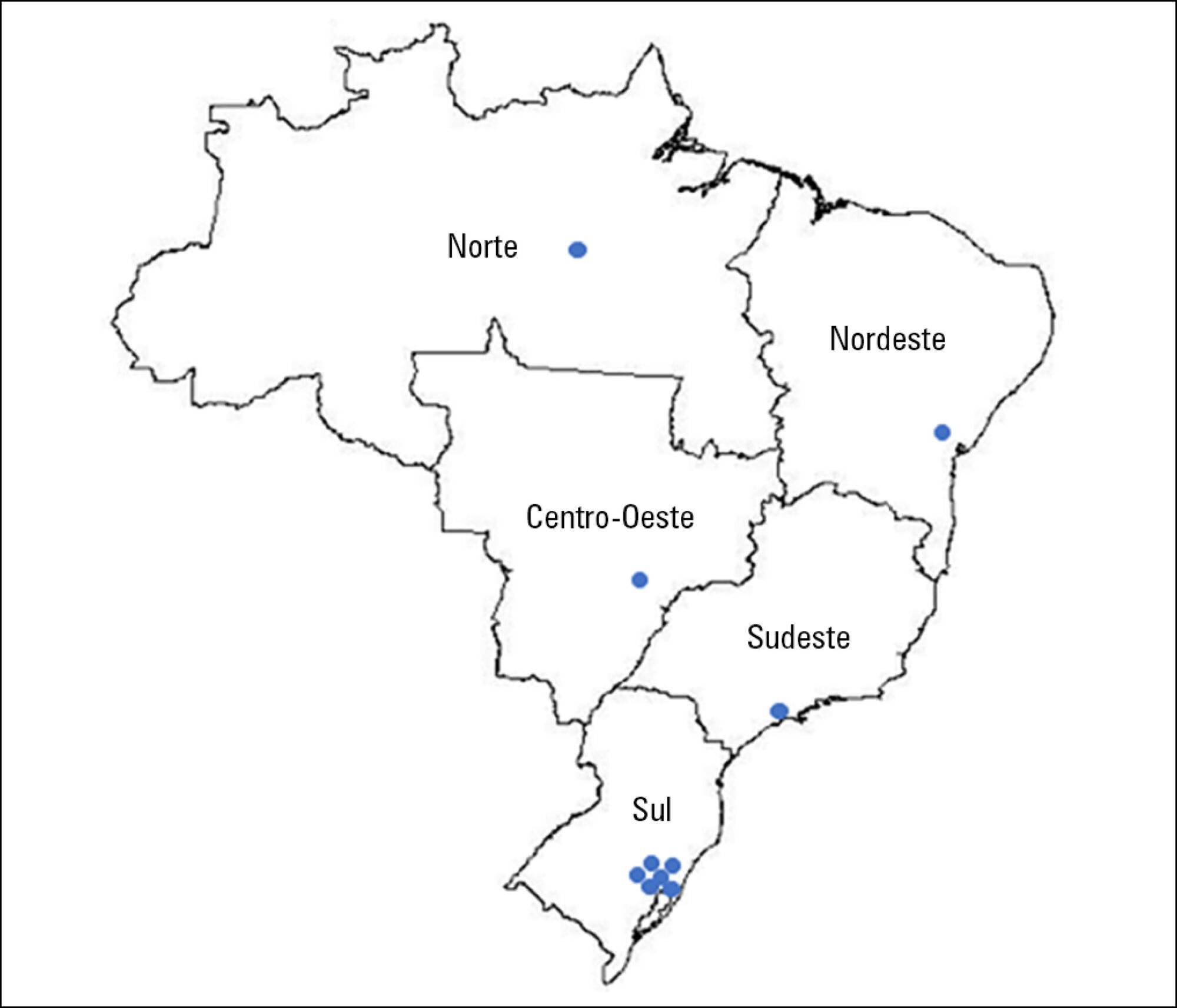
Search
Search in:
KEY WORDS
Case reports Child Coronavirus infections COVID-19 Critical care Critical illness Extracorporeal membrane oxygenation Infant, newborn Intensive care Intensive care units Intensive care units, pediatric mechanical ventilation Mortality Physical therapy modalities Prognosis Respiration, artificial Respiratory insufficiency risk factors SARS-CoV-2 Sepsis




