You searched for:"Pedro Povoa"
We found (19) results for your search.Abstract
Rev Bras Ter Intensiva. 2013;25(1):1-2
Abstract
Rev Bras Ter Intensiva. 2012;24(2):115-116
DOI 10.1590/S0103-507X2012000200003
Abstract
Rev Bras Ter Intensiva. 2020;32(1):14-16
DOI 10.5935/0103-507X.20200004
Abstract
Rev Bras Ter Intensiva. 2015;27(3):196-198
DOI 10.5935/0103-507X.20150038
Abstract
Rev Bras Ter Intensiva. 2022;34(2):227-236
DOI 10.5935/0103-507X.20220020-en
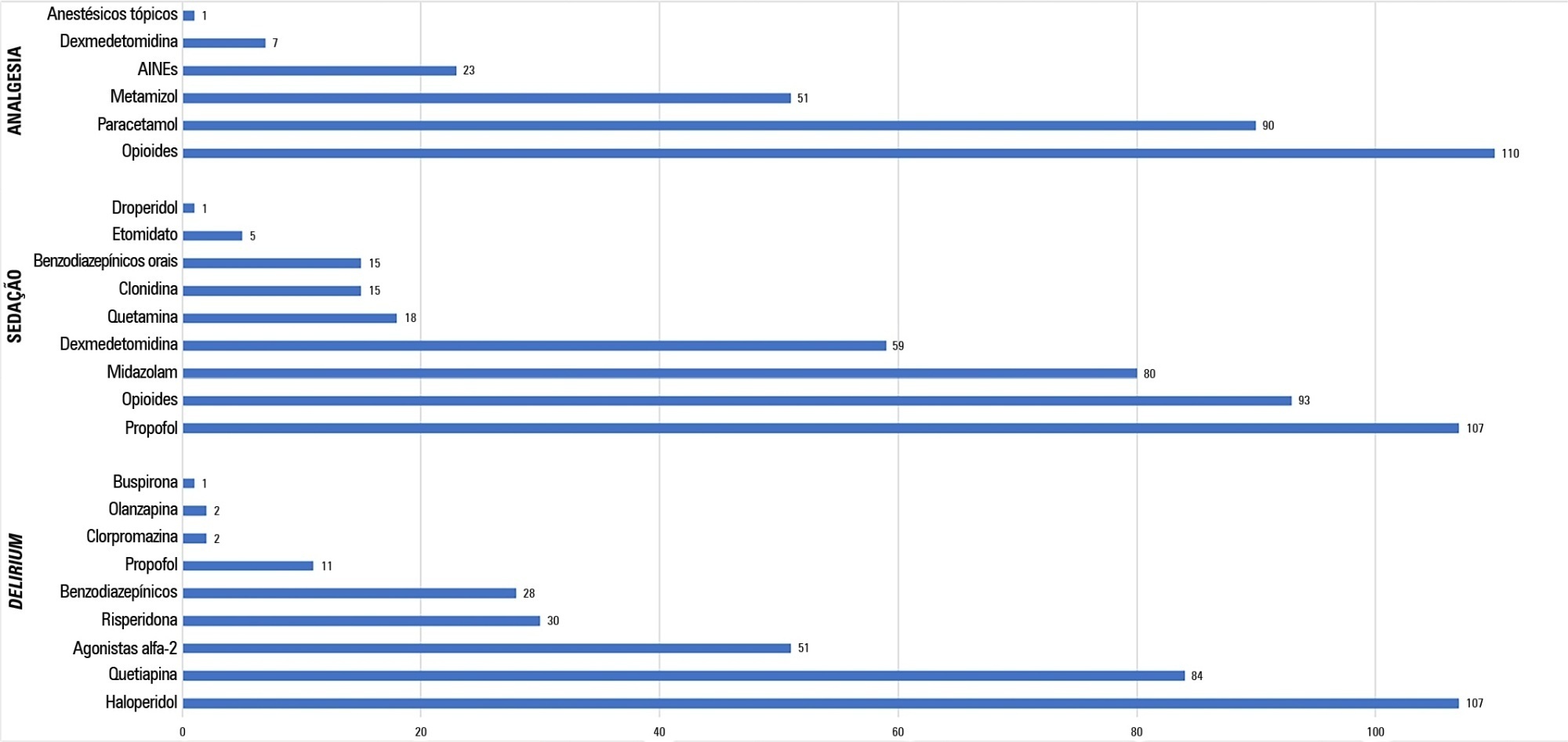
To establish current Portuguese critical care practices regarding analgesia, sedation, and delirium based on a comparison between the activities reported and daily clinical practice.
A national survey was conducted among physicians invited to report their practice toward analgesia, sedation, and delirium in intensive care units. A point prevalence study was performed to analyze daily practices.
A total of 117 physicians answered the survey, and 192 patients were included in the point prevalence study. Survey and point prevalence studies reflect a high sedation assessment (92%; 88.5%), with the Richmond Agitated Sedation Scale being the most reported and used scale (41.7%; 58.2%) and propofol being the most reported and used medication (91.4%; 58.6%). Midazolam prescribing was reported by 68.4% of responders, but a point prevalence study revealed a use of 27.6%.
The results from the survey did not accurately reflect the common practices in Portuguese intensive care units, as reported in the point prevalence study. Efforts should be made specifically to avoid oversedation and to promote delirium assessment.
Abstract
Rev Bras Ter Intensiva. 2007;19(3):337-341
DOI 10.1590/S0103-507X2007000300012
BACKGROUND AND OBJECTIVES: Pressure ulcers (PU) constitute an important health problem in particular in the intensive care unit (ICU). The objective of the study was to identify the number, degree and total score of PU on admission, ICU stay and discharge as well as to recognize factors influencing the appearance or development of PU and to identify the number of healed PU, thus so the incidence and prevalence. METHODS: All patients admitted > 24 hrs were prospectively included during one year. Seventy patients were excluded for insufficient data. The prevention protocol (Norton scale; positioning according the risk grade) and therapeutic protocol (hydrocolloid dressings; hydrogel dressings if tissue necrosis and/or devitalized and alginate dressings if ulcer bleeds) was applied to all patients. RESULTS: One hundred and fifty five patients were studied. Eighteen patients were admitted already with PU. During ICU stay, 40 patients developed a total of 125 PU. The prevalence of PU was 37.41% and incidence was 25.8%. The development of new PU occurred on average by the 7th day. Patients with PU presented 2.6 PU on the average. Seventy nine percent of the patients admitted in the ICU remained stable or improved. Patients admitted with PU had a SAPS 2 significantly higher than those without, 54 ± 8.7 and 44 ± 17, respectively (p = 0.015). At the day of discharge, patients classified as high risk had significantly more PU (p = 0.039). Non-survivors had significantly more PU than survivors (p < 0.001). Patients with longer ICU stay had more PU (p < 0.001) CONCLUSIONS: In our patient population we found 37.41% prevalence and 25.8% incidence of PU. The present prevention protocol of PU was effective in 79% of the patients; severely ill patients developed PU more frequently.
Abstract
Rev Bras Ter Intensiva. 2022;34(3):351-359
DOI 10.5935/0103-507X.20220383-en
To develop a simple, robust, safe and efficient invasive mechanical ventilator that can be used in remote areas of the world or war zones where the practical utility of more sophisticated equipment is limited by considerations of maintainability, availability of parts, transportation and/or cost.
The device implements the pressure-controlled continuous mandatory ventilation mode, complemented by a simple assist-control mode. Continuous positive airway pressure is also possible. The consumption of compressed gases is minimized by avoiding a continuous flow of oxygen or air. Respiratory rates and inspiration/expiration time ratios are electronically determined, and an apnea/power loss alarm is provided.
The pressure profiles were measured for a range of conditions and found to be adjustable within a ± 2.5cmH2O error margin and stable well within this range over a 41-hour period. Respiratory cycle timing parameters were precise within a few percentage points over the same period. The device was tested for durability for an equivalent period of four months. Chemical and biological tests failed to identify any contamination of the gas by volatile organic compounds or microorganisms. A ventilation test on a large animal, in comparison with a well established ventilator, showed that the animal could be adequately ventilated over a period of 60 minutes, without any noticeable negative aftereffects during the subsequent 24-hour period.
This ventilator design may be viable, after further animal tests and formal approval by the competent authorities, for clinical application in the abovementioned atypical circumstances.
