You searched for:"Felipe Dal-Pizzol"
We found (22) results for your search.-
Editorial
Searching for the Holy Grail: where do we go with the current biomarkers for sepsis?
Rev Bras Ter Intensiva. 2012;24(2):117-118
Abstract
EditorialSearching for the Holy Grail: where do we go with the current biomarkers for sepsis?
Rev Bras Ter Intensiva. 2012;24(2):117-118
DOI 10.1590/S0103-507X2012000200004
Views0EDITORIAL Searching for the Holy Grail: where do we go with the current biomarkers for sepsis? […]See more -
Original Articles – Basic Research
Inflammatory and oxidative cord blood parameters as predictors of neonatal sepsis severity
Rev Bras Ter Intensiva. 2012;24(1):30-34
Abstract
Original Articles – Basic ResearchInflammatory and oxidative cord blood parameters as predictors of neonatal sepsis severity
Rev Bras Ter Intensiva. 2012;24(1):30-34
DOI 10.1590/S0103-507X2012000100005
Views0OBJECTIVES: Neonatal sepsis is a complex syndrome involving an uncontrolled systemic inflammatory response associated with an infection. It may result in the dysfunction or failure of one or more organs or even death. Given its high incidence in premature neonates, the identification of prognostic factors to optimize the early diagnosis and therapeutic interventions are highly desirable. This objective study determine the relationship between inflammatory markers and oxidative parameters as prognostic factors in early neonatal sepsis. METHODS: We conducted a prospective observational study by collecting data from 120 patients in the maternity unit of a university hospital. Preterm (<37 weeks of pregnancy) infants with at least one additional risk factor for neonatal sepsis were included. The levels of interleukin (IL)-6, IL-10, thiobarbituric acid reactive species (TBARS) and protein carbonyls and their association with sepsis severity were determined in the cord blood. RESULTS: Levels of IL-6 and TBARS, but not IL-10 and protein carbonyls, demonstrated a mild to moderate correlation with the SNAPPE-II severity score (r=0.435, p=0.02 and r = 0.385, p = 0.017, respectively). No correlations were found between these markers and mortality. CONCLUSION: TBARS and IL-6 have a mild to moderate correlation with SNAPPE-II, but none of the studied markers were able to predict mortality in our sample.
Keywords:Fetal bloodInfant, newbornIntensive care units, neonatalInterleukin-10Interleukin-6Oxidative stressSepsisSee more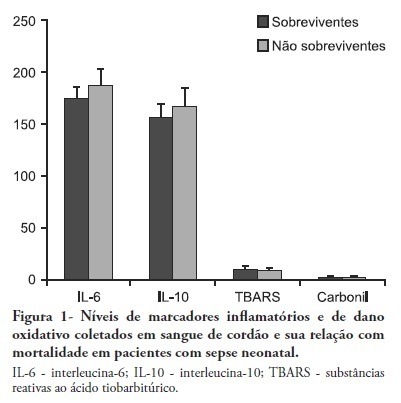
-
Original Articles – Clinical Research
The incidence of delirium in patients pretreated with statins who remain in an intensive care unit after cardiac surgery
Rev Bras Ter Intensiva. 2012;24(1):52-57
Abstract
Original Articles – Clinical ResearchThe incidence of delirium in patients pretreated with statins who remain in an intensive care unit after cardiac surgery
Rev Bras Ter Intensiva. 2012;24(1):52-57
DOI 10.1590/S0103-507X2012000100008
Views0OBJECTIVE: To determine the association between the preoperative administration of statins and postoperative delirium in a prospective cohort of patients undergoing cardiac surgery. METHODS: All adult patients who were admitted to the intensive care unit following cardiac surgery between January and June 2011 were included. Delirium was screened during the postoperative period using the Confusion Assessment Method for Intensive Care Unit (CAM-ICU) and Intensive Care Delirium Screening Checklist (ICDSC). RESULTS: A total of 169 patients underwent elective cardiac surgery, and 40.2% of the patients were treated preoperatively with statins. Delirium was identified using the CAM-ICU in 14.9% of patients not taking preoperative statins in comparison with 11.8% of the patients taking statins (p = 0.817). Using the ICDSC, delirium was identified in 18.8% of patients not taking statins in comparison with 10.3% of the patients taking statins (p = 0.191). CONCLUSION: The use of preoperative statins is not correlated with postoperative delirium in patients undergoing cardiac surgery.
Keywords:Cardiac surgeryDeliriumHydroxymethylglutaryl-CoA reductase inhibitorsIntensive care unitsPostoperative periodSee more -
Special Articles
Guidelines for potential multiple organ donors (adult): part II. Mechanical ventilation, endocrine metabolic management, hematological and infectious aspects
Rev Bras Ter Intensiva. 2011;23(3):269-282
Abstract
Special ArticlesGuidelines for potential multiple organ donors (adult): part II. Mechanical ventilation, endocrine metabolic management, hematological and infectious aspects
Rev Bras Ter Intensiva. 2011;23(3):269-282
DOI 10.1590/S0103-507X2011000300004
Views0See moreThe role of intensive care specialists in the maintenance of deceased potential donors is not restricted to hemodynamics. Appropriate endocrine-metabolic management is fundamental to maintaining energy support and hydroelectrolytic control, which cooperate for hemodynamic stability. Hematological changes are also important, especially considering the issues caused by inappropriate transfusions. In addition, this article discusses the role of appropriate protective ventilation to prevent inflammatory responses and to provide more transplantable lungs. Finally, judicious assessment of infections and antibiotic therapy is discussed
-
Risk factors for early-onset neonatal sepsis in Brazilian public hospital short-title: early-onset neonatal sepsis
Rev Bras Ter Intensiva. 2006;18(2):148-153
Abstract
Risk factors for early-onset neonatal sepsis in Brazilian public hospital short-title: early-onset neonatal sepsis
Rev Bras Ter Intensiva. 2006;18(2):148-153
DOI 10.1590/S0103-507X2006000200008
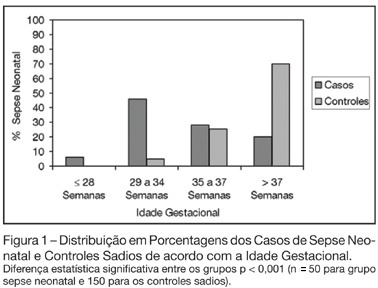
Views0See moreBACKGROUND AND OBJECTIVES: The determination of the risk factors to early-onset neonatal sepsis in our country is essential to prevent and reduce the mortality associated with this syndrome. Thus, the objective of this study was to determine the frequency and associated risk factors to early-onset neonatal sepsis in public hospital in Southern Brazil. METHODS: Observational, case-control study. Were included neonates with diagnostic of early-onset neonatal sepsis and as controls, neonates without neonatal infection. Were included 50 cases and 3 controls for each case resulting in a total sample of 200 patients. Associations were considered significant when p < 0.05. RESULTS: The sepsis frequency was 50.3 per 1000 born-alive. Risk factors associated to the development of neonatal sepsis were prematurity (OR 9.33; p < 0.001), low birth weight (OR 11.74; p < 0.001), maternal infection (OR 2.28; p = 0.009), mother with history of previous infant with neonatal sepsis (OR 6.43; p = 0.035) and rupture of the membranes more than 18 hours before delivery (OR 9.33; p = 0.001). CONCLUSIONS: Neonatal sepsis was very frequent in the study. Prematurity, low birth weight, maternal infection and mother’s having had a previous infant with neonatal sepsis are risk factors for early-onset neonatal sepsis.
Search
Search in:
KEY WORDS
Case reports Child Coronavirus infections COVID-19 Critical care Critical illness Extracorporeal membrane oxygenation Infant, newborn Intensive care Intensive care units Intensive care units, pediatric mechanical ventilation Mortality Physical therapy modalities Prognosis Respiration, artificial Respiratory insufficiency risk factors SARS-CoV-2 Sepsis