Abstract
Crit Care Sci. 2024;36:e20240265en
DOI 10.62675/2965-2774.20240265-en
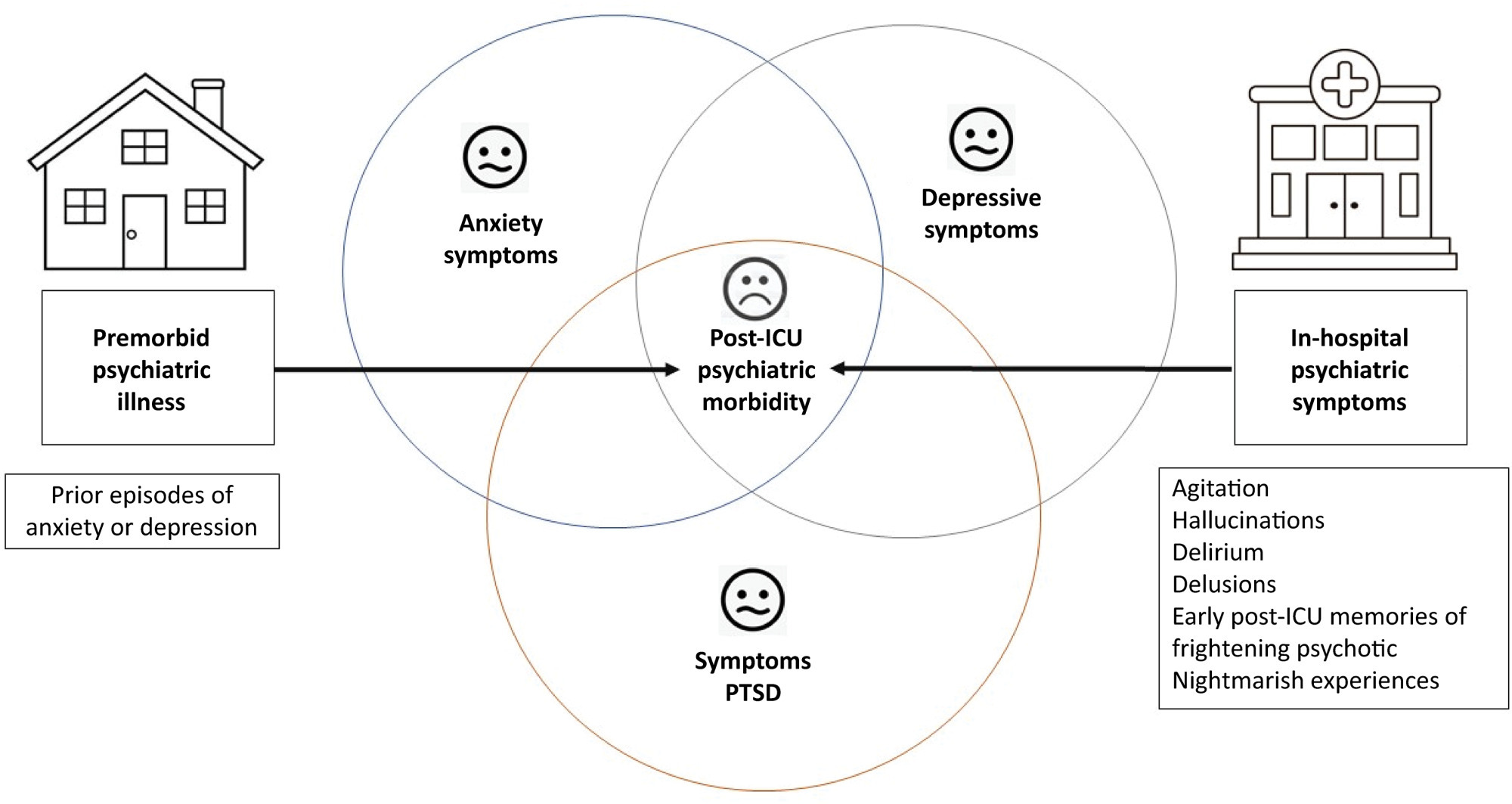
A significant portion of individuals who have experienced critical illness encounter new or exacerbated impairments in their physical, cognitive, or mental health, commonly referred to as postintensive care syndrome. Moreover, those who survive critical illness often face an increased risk of adverse consequences, including infections, major cardiovascular events, readmissions, and elevated mortality rates, during the months following hospitalization. These findings emphasize the critical necessity for effective prevention and management of long-term health deterioration in the critical care environment. Although conclusive evidence from well-designed randomized clinical trials is somewhat limited, potential interventions include strategies such as limiting sedation, early mobilization, maintaining family presence during the intensive care unit stay, implementing multicomponent transition programs (from intensive care unit to ward and from hospital to home), and offering specialized posthospital discharge follow-up. This review seeks to provide a concise summary of recent medical literature concerning long-term outcomes following critical illness and highlight potential approaches for preventing and addressing health decline in critical care survivors.
Abstract
Rev Bras Ter Intensiva. 2022;34(4):499-506
DOI 10.5935/0103-507X.20220080-en
To evaluate the prevalence and factors associated with depression in family members of people hospitalized in intensive care units.
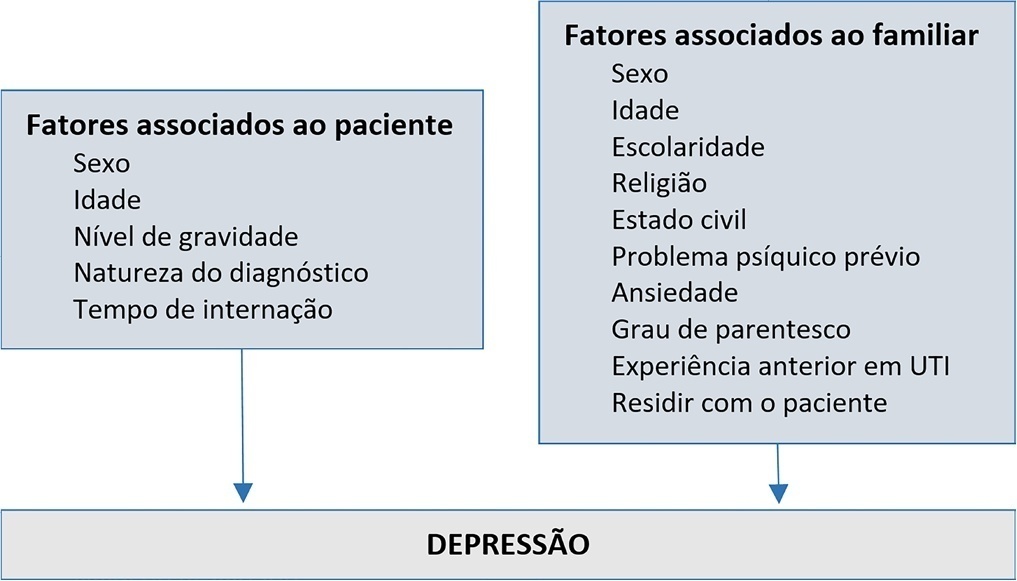
A cross-sectional study was conducted with 980 family members of patients admitted to the intensive care units of a large public hospital in the interior of Bahia. Depression was measured using the Patient Health Questionnaire-8. The multivariate model consisted of the following variables: sex and age of the patient, sex and age of the family member, education level, religion, living with the family member, previous mental illness and anxiety.
Depression had a prevalence of 43.5%. In the multivariate analysis, the model with the best representativeness indicated that factors associated with a higher prevalence of depression were being female (39%), age younger than 40 years (26%) and previous mental illness (38%). A higher education level was associated with a 19% lower prevalence of depression in family members.
The increase in the prevalence of depression was associated with female sex, age younger than 40 years and previous psychological problems. Such elements should be valued in actions aimed at family members of people hospitalized in intensive care.