Abstract
Rev Bras Ter Intensiva. 2015;27(4):406-411
DOI 10.5935/0103-507X.20150068
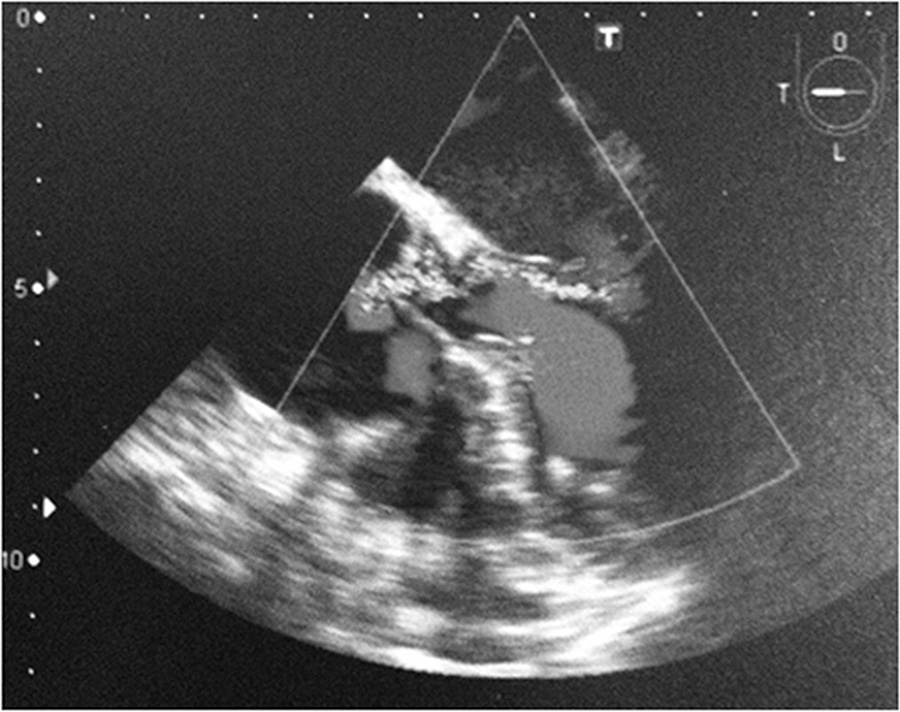
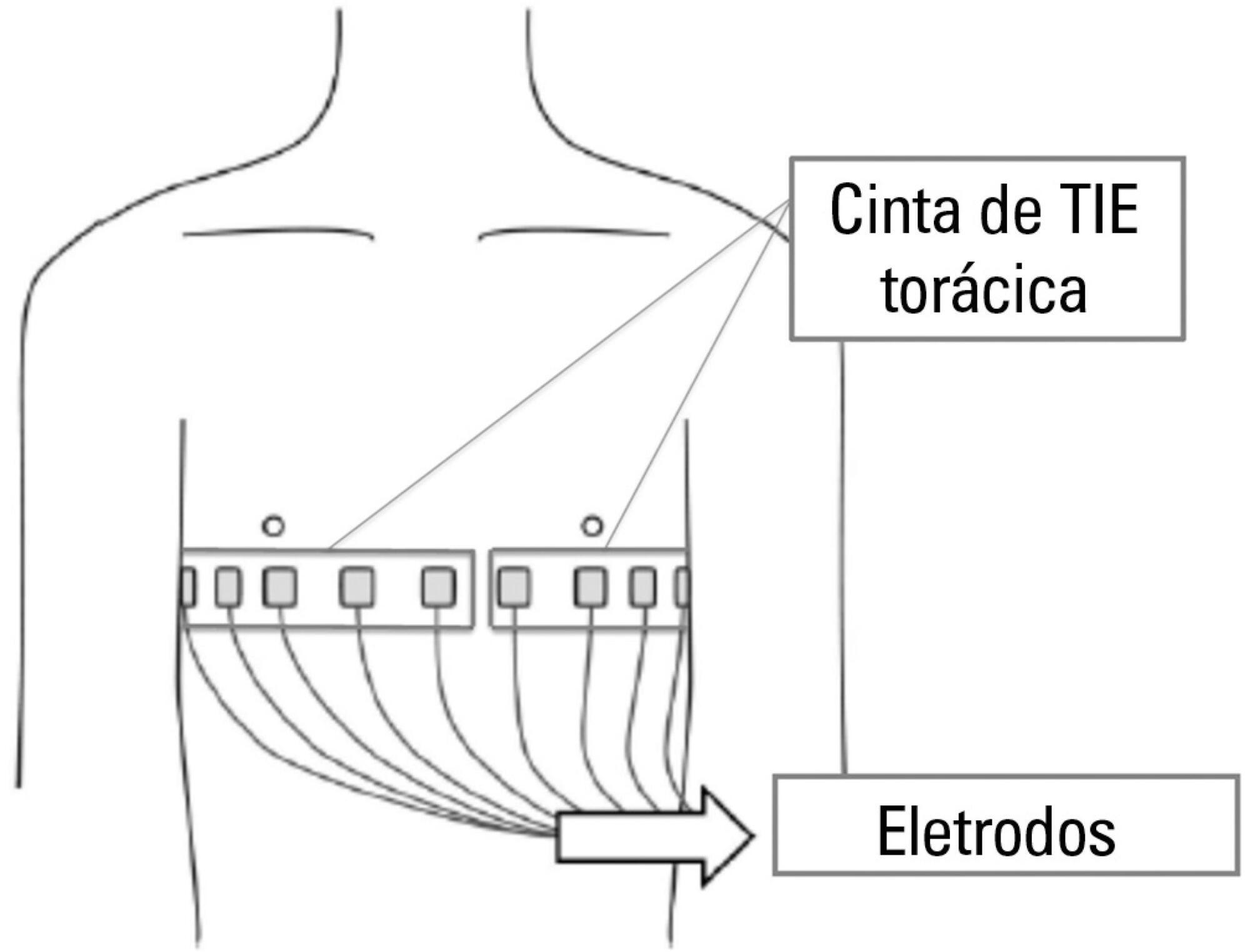
Thoracic electrical impedance tomography is a real-time, noninvasive monitoring tool of the regional pulmonary ventilation distribution. Its bedside use in patients with acute respiratory distress syndrome has the potential to aid in alveolar recruitment maneuvers, which are often necessary in cases of refractory hypoxemia. In this case report, we describe the monitoring results and interpretation of thoracic electrical impedance tomography used during alveolar recruitment maneuvers in a patient with acute respiratory distress syndrome, with transient application of high alveolar pressures and optimal positive end-expiratory pressure titration. Furthermore, we provide a brief literature review regarding the use of alveolar recruitment maneuvers and monitoring using thoracic electrical impedance tomography in patients with acute respiratory distress syndrome.
Abstract
Rev Bras Ter Intensiva. 2015;27(4):412-415
DOI 10.5935/0103-507X.20150069
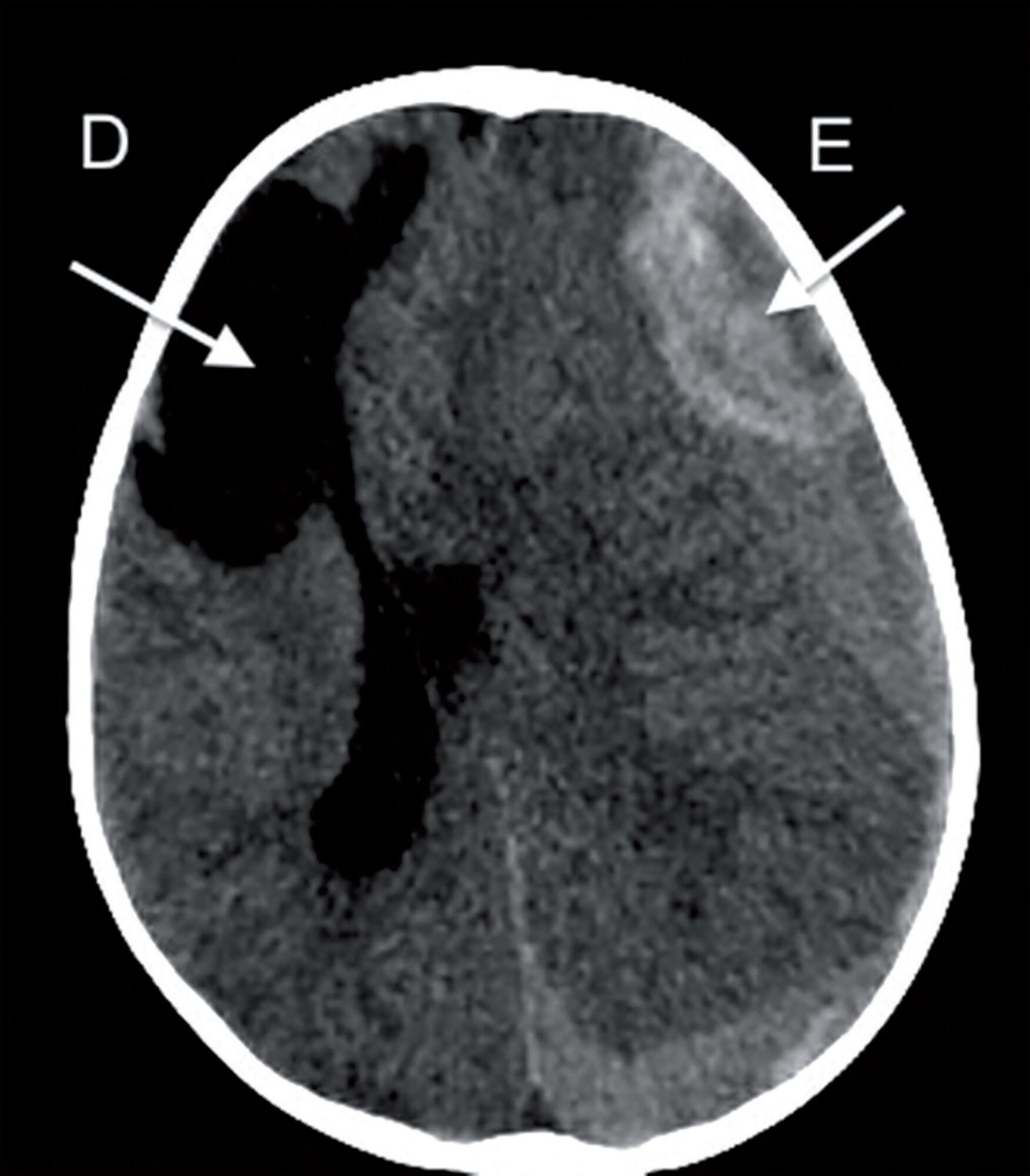
We report the case of a 2-year-old child who survived an acute episode of severe spontaneous intracranial hemorrhage with clinical and radiological signs of intracranial hypertension and transtentorial herniation. The patient underwent emergency surgery to drain the hematoma, and a catheter was inserted to monitor intracranial pressure. In the initial computed tomography analysis performed prior to hematoma drainage, a brain cyst was evident contralateral to the hematoma, which, based on the analysis by the care team, possibly helped to avoid a worse outcome because the cyst accommodated the brain after the massive hemorrhage. After the investigation, the patient was determined to have previously undiagnosed hemophilia A. The patient underwent treatment in intensive care, which included the control of intracranial pressure, factor VIII replacement and discharge without signs of neurological impairment.
Abstract
Rev Bras Ter Intensiva. 2015;27(2):185-189
DOI 10.5935/0103-507X.20150031
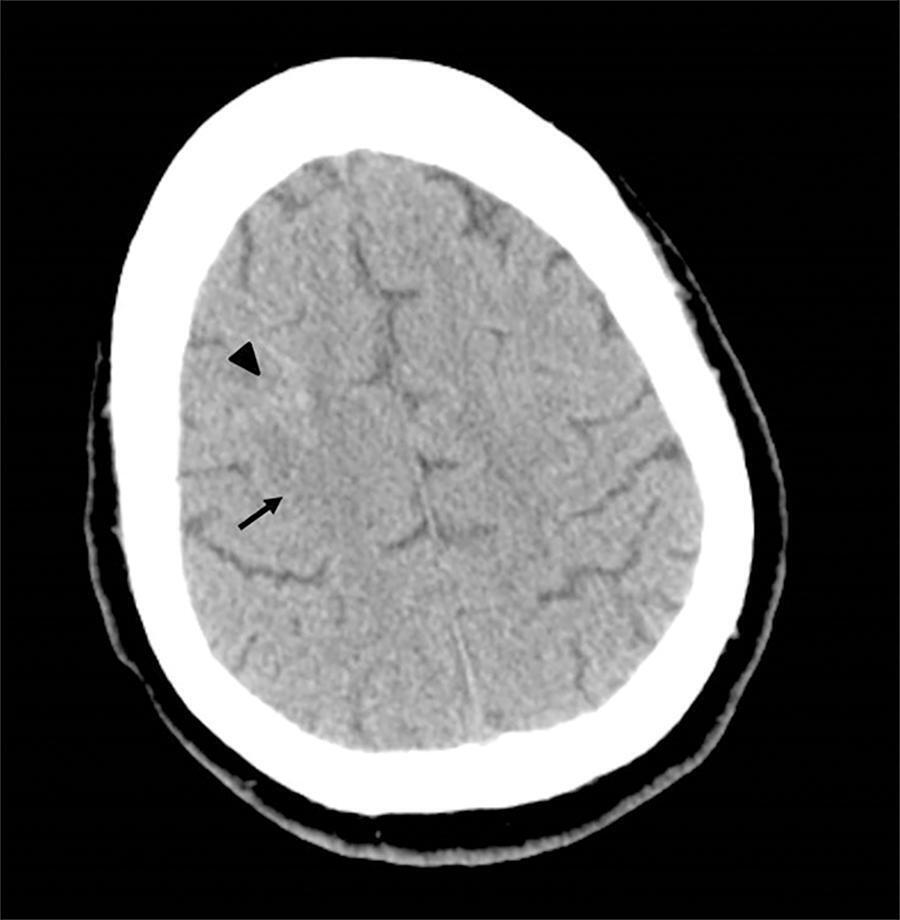
This is a case report of a 43-year-old Caucasian male with end-stage renal disease being treated with hemodialysis and infective endocarditis in the aortic and tricuspid valves. The clinical presentation was dominated by neurologic impairment with cerebral embolism and hemorrhagic components. A thoracoabdominal computerized tomography scan revealed septic pulmonary embolus. The patient underwent empirical antibiotherapy with ceftriaxone, gentamicin and vancomycin, and the therapy was changed to flucloxacilin and gentamicin after the isolation of S. aureus in blood cultures. The multidisciplinary team determined that the patient should undergo valve replacement after the stabilization of the intracranial hemorrhage; however, on the 8th day of hospitalization, the patient entered cardiac arrest due to a massive septic pulmonary embolism and died. Despite the risk of aggravation of the hemorrhagic cerebral lesion, early surgical intervention should be considered in high-risk patients.
Abstract
Rev Bras Ter Intensiva. 2015;27(4):397-401
DOI 10.5935/0103-507X.20150066
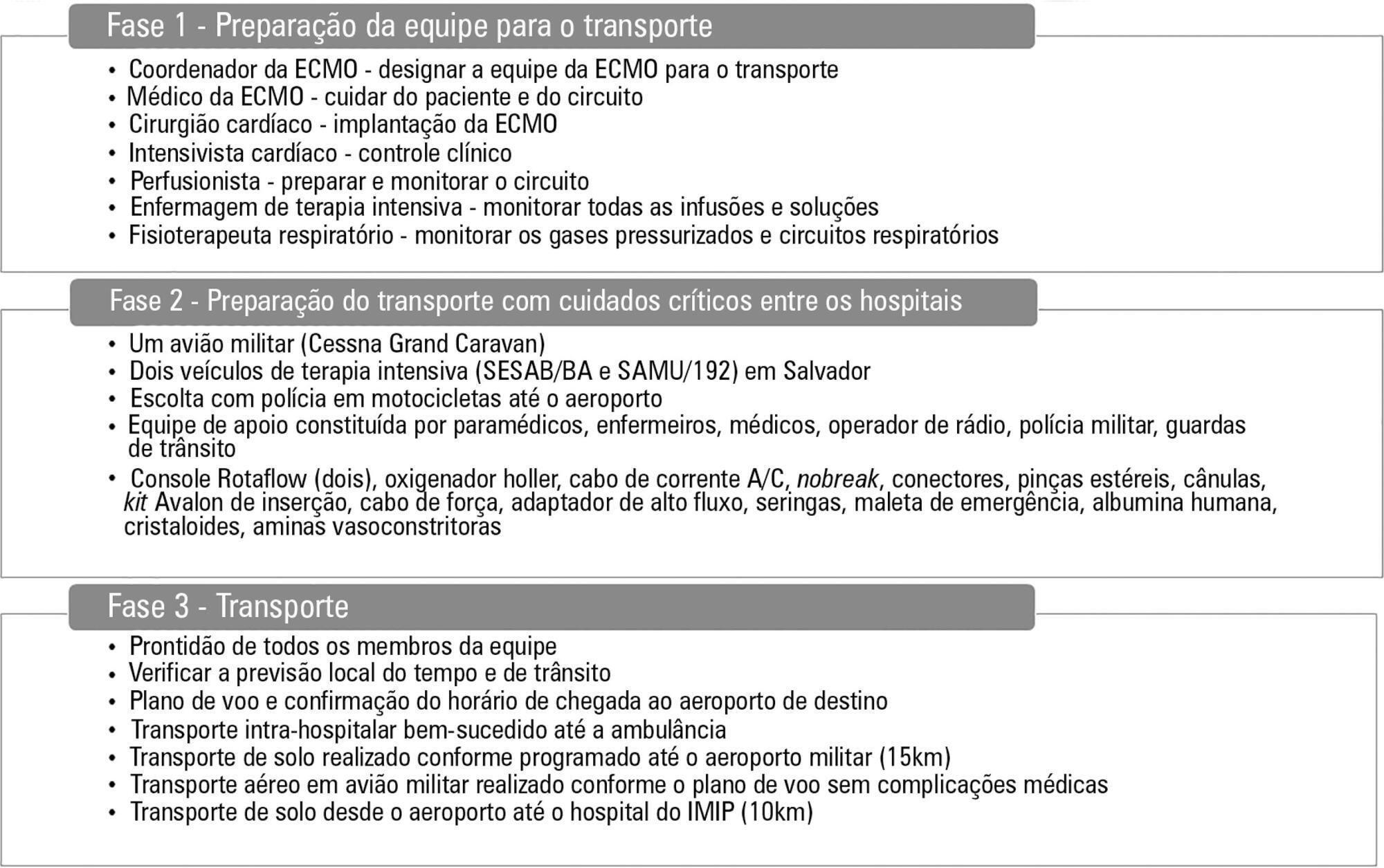
A 17-year-old Brazilian male presented with progressive dyspnea for 15 days, worsening in the last 24 hours, and was admitted in respiratory failure and cardiogenic shock, with multiple organ dysfunctions. Echocardiography showed a left ventricle ejection fraction of 11%, severe diffuse hypokinesia, and a systolic pulmonary artery pressure of 50mmHg, resulting in the need for hemodynamic support with dobutamine (20mcg/kg/min) and noradrenaline (1.7mcg/kg/min). After 48 hours with no clinical or hemodynamic improvement, an extracorporeal membrane oxygenation was implanted. The patient presented with hemodynamic, systemic perfusion and renal and liver function improvements; however, his cardiac function did not recover after 72 hours, and he was transfer to another hospital. Air transport was conducted from Salvador to Recife in Brazil. A heart transplant was performed with rapid recovery of both liver and kidney functions, as well as good graft function. Histopathology of the explanted heart showed chronic active myocarditis and amastigotes of Trypanosoma cruzi. The estimated global prevalence of T. cruzi infections declined from 18 million in 1991, when the first regional control initiative began, to 5.7 million in 2010. Myocarditis is an inflammatory disease due to infectious or non-infectious conditions. Clinical manifestation is variable, ranging from subclinical presentation to refractory heart failure and cardiogenic shock. Several reports suggest that the use of extracorporeal membrane oxygenation in patients presenting with severe refractory myocarditis is a potential bridging therapy to heart transplant when there is no spontaneous recovery of ventricular function. In a 6-month follow-up outpatient consult, the patient presented well and was asymptomatic.
Abstract
Rev Bras Ter Intensiva. 2015;27(4):402-405
DOI 10.5935/0103-507X.20150067
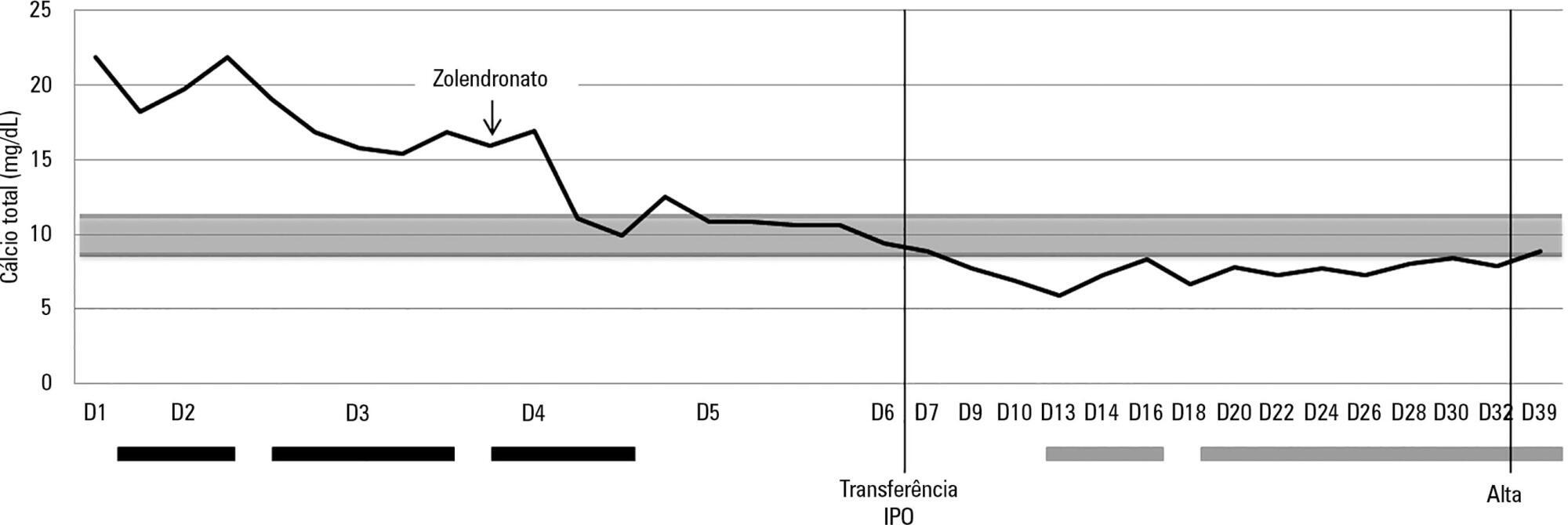
Hypercalcemia is a rare metabolic disorder in children and is potentially fatal. It has a wide differential diagnosis, including cancer. Here, we report the case of a previously healthy 3-year-old who was admitted to the emergency room with fatigue, hyporeactivity, fever and limping gait that had evolved over 5 days and that was progressively worsening. On examination the patient was unconscious (Glasgow coma score: 8). Laboratory tests indicated severe hypercalcemia (total calcium 21.39mg/dL, ionized calcium 2.93mmol/L) and microcytic anemia. Hyperhydration was initiated, and the child was transferred to the pediatric intensive care unit. Continuous venovenous hemodiafiltration with calcium-free solution was instituted, which brought progressive normalization of serum calcium and an improved state of consciousness. Zoledronate was administered, and metabolic and infectious causes and poisoning were excluded. The bone marrow smear revealed a diagnosis of acute lymphoblastic leukemia. Hypercalcemia associated with malignancy in children is rare and occurs as a form of cancer presentation or recurrence. Continuous venovenous hemodiafiltration should be considered in situations where there is imminent risk to life.
Abstract
Rev Bras Ter Intensiva. 2014;26(4):421-429
DOI 10.5935/0103-507X.20140065
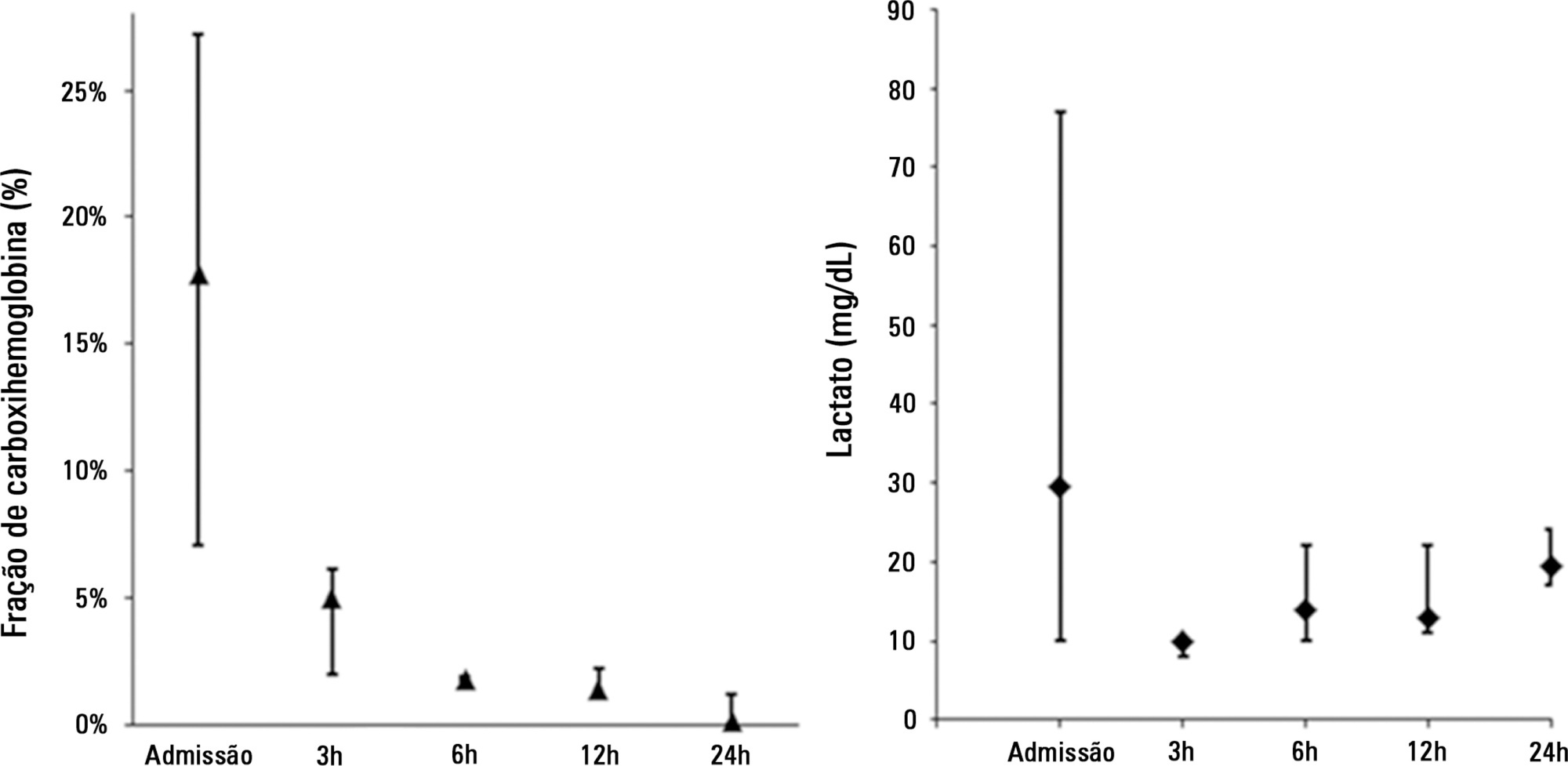
On January 2013, a disaster at Santa Maria (RS) due to a fire in a confined space caused 242 deaths, most of them by inhalation injury. On November 2013, four individuals required intensive care following smoke inhalation from a fire at the Memorial da América Latina in São Paulo (SP). The present article reports the clinical progression and management of disaster victims presenting with inhalation injury. Patients ERL and OC exhibited early respiratory failure, bronchial aspiration of carbonaceous material, and carbon monoxide poisoning. Ventilation support was performed with 100% oxygen, the aspirated material was removed by bronchoscopy, and cyanide poisoning was empirically treated with sodium nitrite and sodium thiosulfate. Patient RP initially exhibited cough and retrosternal burning and subsequently progressed to respiratory failure due to upper airway swelling and early-onset pulmonary infection, which were treated with protective ventilation and antimicrobial agents. This patient was extubated following improvement of edema on bronchoscopy. Patient MA, an asthmatic, exhibited carbon monoxide poisoning and bronchospasm and was treated with normobaric hyperoxia, bronchodilators, and corticosteroids. The length of stay in the intensive care unit varied from four to 10 days, and all four patients exhibited satisfactory functional recovery. To conclude, inhalation injury has a preponderant role in fires in confined spaces. Invasive ventilation should not be delayed in cases with significant airway swelling. Hyperoxia should be induced early as a therapeutic means against carbon monoxide poisoning, in addition to empiric pharmacological treatment in suspected cases of cyanide poisoning.
Abstract
Rev Bras Ter Intensiva. 2014;26(4):430-434
DOI 10.5935/0103-507X.20140066
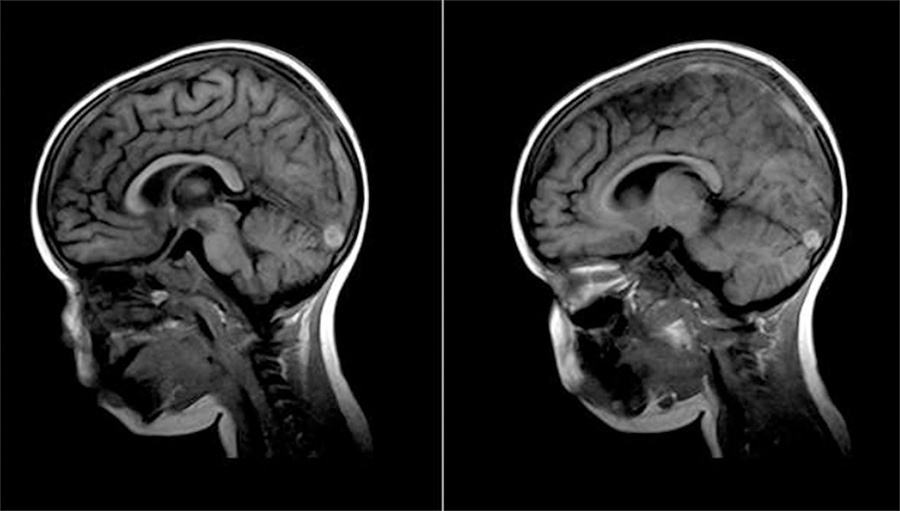
Nephrotic syndrome is associated with a hypercoagulable state and an increased risk of thromboembolic complications. Cerebral venous sinus thrombosis is a rare complication of nephrotic syndrome, with few cases described in the literature, although the disease may be under-diagnosis. The true incidence of cerebral venous sinus thrombosis may be underestimated because many events are asymptomatic or are not diagnosed in time. Here, we describe the case of a male child, 2 years and 10 months old, with nephrotic syndrome presenting with headache, epileptic seizures and sensory inhibition who was diagnosed with superior sagittal and transverse sinuses thrombosis. An international literature review was performed with a defined search strategy in the PubMed, SciELO and Lilacs databases using the terms ‘nephrotic syndrome’ and ‘cerebral sinovenous thrombosis’. The diagnosis of venous thrombosis should be considered in any patient with nephrotic syndrome who presents with neurological signs and symptoms, as early clinical diagnosis promotes favorable outcomes.
Abstract
Rev Bras Ter Intensiva. 2014;26(3):313-316
DOI 10.5935/0103-507X.20140044
We describe herein a case of a patient who, when in orthostatic positions, had severe hypoxemia and ventilatory dysfunction. Although the severity of symptoms required hospitalization in an intensive care setting, the initial tests only identified the presence of enlarged aortic root, which did not explain the condition. The association of these events with an unusual etiology, namely intracardiac shunt, characterized the diagnosis of platypnea-orthodeoxia syndrome. The literature review shows that, with advancing research methods, there was a progressive increase in the identification of this condition, and this association should be part of the differential diagnosis of dyspnea in patients with enlarged aortic root.