Abstract
Rev Bras Ter Intensiva. 2009;21(1):9-17
DOI 10.1590/S0103-507X2009000100002
OBJECTIVES: The objective of this study was to evaluate variables related to intra hospital mortality at 28 days, of aged persons with severe sepsis and septic shock in a clinical ICU. METHODS: One hundred and fifty-two patients aged > 65 years with severe sepsis and septic shock were followed for 28 days and the variables were collected on days 1, 3, 5, 7, 14 and 28 of stay. To compare categorical variables the Chi-square test was used and the Mann-Whitney or t test for continuous variables. All tests were double-tailed, alpha error of 0.05. RESULTS: Mean age was 82.0 ± 9.0 years and 64.5% were female. Mortality was of 47.4%. Related to death were the following: Acute Physiological and Chronic Heath Evaluation II score (p < 0.001), Sequential Organ Failure Assessment score on days 1, 3, 5, 7 (p < 0.001), length of stay in intensive care (p < 0.001), number of organ failures (p < 0.001), high serum lactate on day 3 (p = 0.05), positive troponin I (p < 0.01), echocardiographic variables (systolic diameter p = 0.005; diastolic diameter p = 0.05; shortening fraction p = 0.02), previous renal disease (p = 0.03), shock (p < 0.001), mechanical ventilation (p < 0.001) and Lawton scale (p = 0.04). CONCLUSIONS: Shock, elevated lactate, organ failure, especially respiratory were more prevalent in non-survivors. Heart dysfunction detected by echocardiographic variables and positive troponin I may play an important role in the mortality of aged patients with sepsis.
Abstract
Rev Bras Ter Intensiva. 2008;20(3):226-234
DOI 10.1590/S0103-507X2008000300004
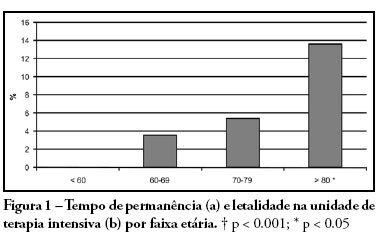
PURPOSE: Due to the increasing longevity of the and high prevalence of coronary heart disease in the aged , coronary artery bypass graft surgery has become frequent in older patients. The purpose of this study is to describe operative features, length of stay, complications and short term outcomes after coronary artery bypass graft in such patients. METHODS: From February 2005 to October 2007, 269 patients underwent coronary artery bypass graft. Demographic data, comorbidities, prognostic scores, coronary artery bypass graft elective versus urgent indication, intensive care unit length of stay, postoperative complications and intensive care unit mortality were recorded. Intra-operative characteristics, such as total surgery time, use of bypass device, on-pump time, urine output, fluid balance, use of blood products and number of grafts, were analyzed. Patients were divided in four age groups: group I (< 60 n = 68), II (60 to 69 n = 86), III (70 to 79 n = 93) IV and older than 80 years (n = 22). RESULTS: Group IV patients were more frequently submitted to coronary artery bypass graft combined with valve replacement, emergency surgery, and had longer stay in the intensive care unit (p < 0.01). The incidence of at least one postoperative complication was also higher among patients older than 80 (p < 0.001). Multivariate analysis identified age and on-pump time as independent risk factors for development of complications. Mortality increased in patients older than 70 years (p = 0.03). CONCLUSIONS: Octogenarian patients undergoing coronary artery bypass graft have longer intensive care unit length of stay, incidence of complications and mortality. Age and on-pump time were independent risk factors associated with the incidence of postoperative complications.
Abstract
Rev Bras Ter Intensiva. 2007;19(3):304-309
DOI 10.1590/S0103-507X2007000300006
BACKGROUND AND OBJECTIVES: The intensive care Medicine was initiated in the State of the Acre in 1998. The aim of the present study was to establish clinical-epidemiological characteristics of adults and aged interned in a public intensive care unit (ICU) in the Amazon. METHODS: In 2004, a prospective study evaluated patients interned through the application of a questionnaire containing socioeconomics variables, invasive procedures, mechanical ventilation, nutritional support, surgical interventions and dialitic treatment. The gravity was established by APACHE II applied after 24 hours of internment. The follow up continued until the final destination in the unit: discharge or death. The statistical analysis used program SPSS, considering differences significant when p < 0.05. RESULTS: A total of 79 patients were assessed; 67.1% men; 59.5% white; 59.5% married; 50.4% came from other hospitals; 41.8% from the interior and 13.9% from others States and country (Bolivia) in frontier. The age varied from 20 to 104 (53.3 ± 18.6) years old; 30 (36.1%) aged (60 y old or more); 35 (44.3%) in surgical treatment; the median APACHE II was 18.4 ± 9.1. The stay in the UCI was of 10.2 ± 9.6 days; death occurred in 30 (38%) patients. Association between mortality and dialitic treatment, clinical indication, mechanical ventilation, vasoactive therapy, number of surgical interventions, hypoalbuminemia, lymphocytopenia and gravity was observed. CONCLUSIONS: The admission of severely ill patients coming from all over the State of Acre and frontier regions reflects the lack of ICU beds in the region.