You searched for:"Wanderley Marques Bernardo"
We found (3) results for your search.-
Special Article
Brazilian Guidelines for Early Mobilization in Intensive Care Unit
Rev Bras Ter Intensiva. 2019;31(4):434-443
Abstract
Special ArticleBrazilian Guidelines for Early Mobilization in Intensive Care Unit
Rev Bras Ter Intensiva. 2019;31(4):434-443
DOI 10.5935/0103-507X.20190084
Views0ABSTRACT
Immobility can cause several complications, including skeletal muscle atrophy and weakness, that influence the recovery of critically ill patients. This effect can be mitigated by early mobilization. Six key questions guided this research: Is early mobilization safe? Which patients are candidates for early mobilization? What are the contraindications? What is the appropriate dose, and how should it be defined? What results are obtained? What are the prognostic indicators for the use of early mobilization? The objective of this guideline was to produce a document that would provide evidence-based recommendations and suggestions regarding the early mobilization of critically ill adult patients, with the aim of improving understanding of the topic and making a positive impact on patient care. This guideline was based on a systematic review of articles conducted using the PICO search strategy, as recommended by the Guidelines Project of the Associação Médica Brasileira. Randomized clinical trials, prognostic cohort studies, and systematic reviews with or without meta-analysis were selected, and the evidence was classified according to the Oxford Center for Evidence-based Medicine Levels of Evidence. For all the questions addressed, enough evidence was found to support safe and well-defined early mobilization, with prognostic indicators that support and recommend the technique. Early mobilization is associated with better functional outcomes and should be performed whenever indicated. Early mobilization is safe and should be the goal of the entire multidisciplinary team.
Keywords:Critical careEarly ambulationExerciseIntensive care unitsMobilityPatient safetyRespiration, artificialSee more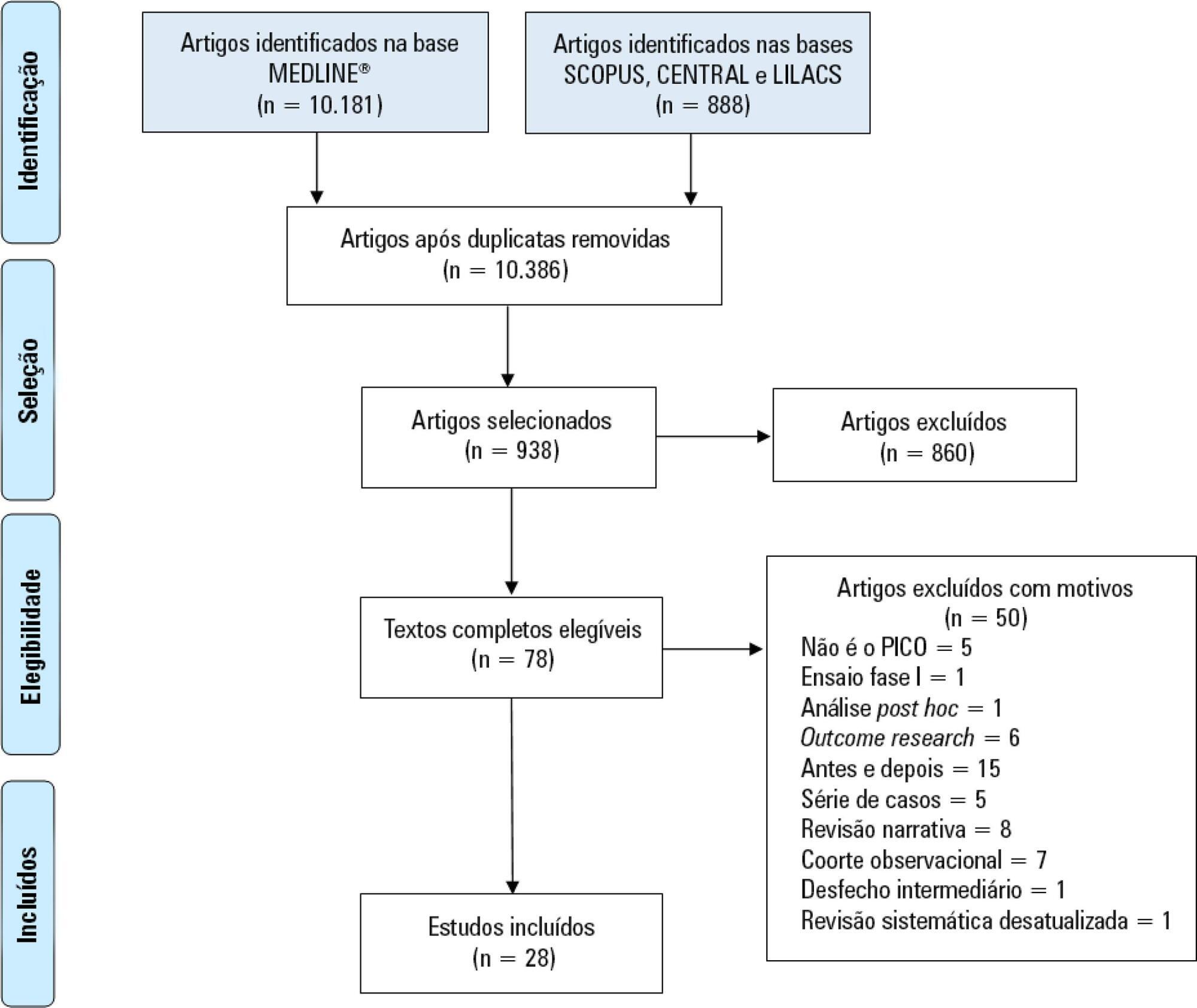
-
Guidelines for treatment of severe sepsis/septic shock: tissue perfusion assessment
Rev Bras Ter Intensiva. 2011;23(1):6-12
Abstract
Guidelines for treatment of severe sepsis/septic shock: tissue perfusion assessment
Rev Bras Ter Intensiva. 2011;23(1):6-12
DOI 10.1590/S0103-507X2011000100003
Views0See moreSepsis is a very frequent condition and causes high mortality rates and healthcare costs; it is the main cause of death in intensive care units. Clear, improved prognosis was shown for early diagnosed and treated patients. Treatment guidelines are fundamental for appropriate therapy. It is clear that hypoperfusion patients should be hemodynamically optimized; therefore, recognition of hypoperfusion signs is one of the main therapeutic steps. This guideline discusses the current literature and available data regarding the evaluation of hemodynamic parameters.
-
Guidelines for the treatment of severe sepsis and septic shock: hemodynamic resuscitation
Rev Bras Ter Intensiva. 2011;23(1):13-23
Abstract
Guidelines for the treatment of severe sepsis and septic shock: hemodynamic resuscitation
Rev Bras Ter Intensiva. 2011;23(1):13-23
DOI 10.1590/S0103-507X2011000100004
Views0See moreSepsis has a high incidence, mortality and cost and is the main cause of death in intensive care units. Early recognition and treatment have been clearly associated with a better prognosis. Establishing new guidelines is a fundamental step for improving treatment. Patients with clear signs of hypoperfusion should undergo hemodynamic optimization. This guideline addresses the main strategies in the literature that are clinically available.
Search
Search in:
KEY WORDS
Case reports Child Coronavirus infections COVID-19 Critical care Critical illness Extracorporeal membrane oxygenation Infant, newborn Intensive care Intensive care units Intensive care units, pediatric mechanical ventilation Mortality Physical therapy modalities Prognosis Respiration, artificial Respiratory insufficiency risk factors SARS-CoV-2 Sepsis




