You searched for:"Thiago Bragança Ataíde"
We found (1) results for your search.-
Original Articles
Use of reactive hyperemia – peripheral arterial tonometry and circulating biological markers to predict outcomes in sepsis
- Vandack Nobre,
- Thiago Bragança Ataíde,
- Luisa Caldeira Brant,
- Clara Rodrigues Oliveira,
- Lucas Vieira Rodrigues, [ … ],
- Marcus Vinícius Andrade
Abstract
Original ArticlesUse of reactive hyperemia – peripheral arterial tonometry and circulating biological markers to predict outcomes in sepsis
Rev Bras Ter Intensiva. 2016;28(4):387-396
DOI 10.5935/0103-507X.20160072
- Vandack Nobre,
- Thiago Bragança Ataíde,
- Luisa Caldeira Brant,
- Clara Rodrigues Oliveira,
- Lucas Vieira Rodrigues,
- Antonio Luiz Pinho Ribeiro,
- Fernanda Barbosa Lopes,
- Ivan Euclides Saraiva,
- Marcus Vinícius Andrade
Views1See moreABSTRACT
Objective:
To evaluate the usefulness and prognostic value of reactive hyperemia – peripheral arterial tonometry in patients with sepsis. Moreover, we investigated the association of reactive hyperemia – peripheral arterial tonometry results with serum levels of certain inflammatory molecules.
Methods:
Prospective study, conducted in an 18-bed mixed intensive care unit for adults. The exclusion criteria included severe immunosuppression or antibiotic therapy initiated more than 48 hours before assessment. We measured the reactive hyperemia – peripheral arterial tonometry on inclusion (day 1) and on day 3. Interleukin-6, interleukin-10, high-mobility group box 1 protein and soluble ST2 levels were measured in the blood obtained upon inclusion.
Results:
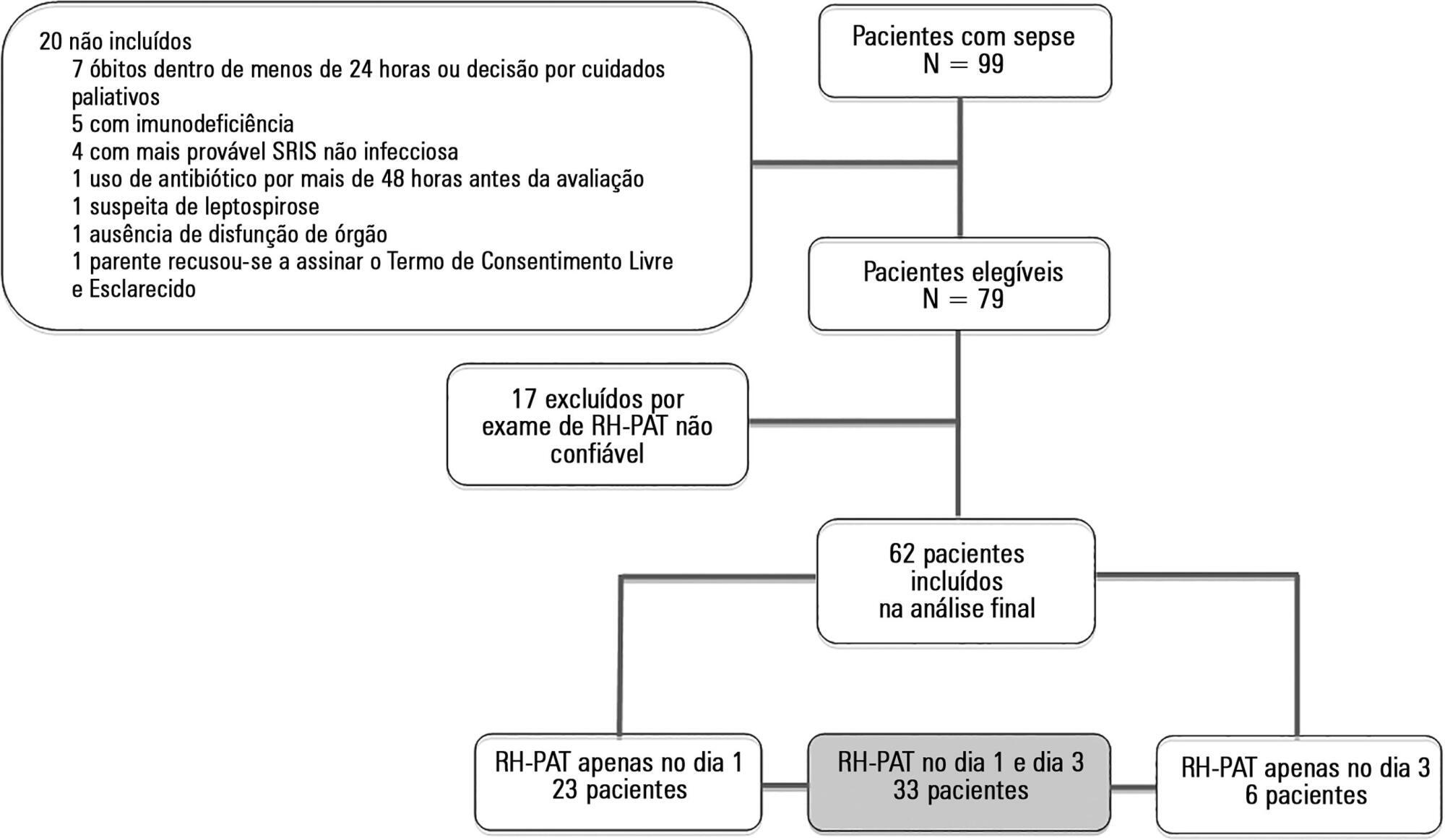
Seventeen of the 79 patients (21.6%) enrolled were determined to have reactive hyperemia – peripheral arterial tonometry signals considered technically unreliable and were excluded from the study. Thus, 62 patients were included in the final analysis, and they underwent a total of 95 reactive hyperemia – peripheral arterial tonometry exams within the first 48 hours after inclusion. The mean age was 51.5 (SD: 18.9), and 49 (62%) of the patients were male. Reactive hyperemia indexes from days 1 and 3 were not associated with vasopressor need, Sequential Organ Failure Assessment score, Acute Physiology and Chronic Health Evaluation II score, or 28-day mortality. Among the patients who died, compared with survivors, there was a significant increase in the day 3 reactive hyperemia index compared with day 1 (p = 0.045). There was a weak negative correlation between the day 1 reactive hyperemia – peripheral arterial tonometry index and the levels of high-mobility group box 1 protein (r = -0.287).
Conclusion:
Technical difficulties and the lack of clear associations between the exam results and clinical severity or outcomes strongly limits the utility of reactive hyperemia – peripheral arterial tonometry in septic patients admitted to the intensive care unit.
Views1

Abstract
Original ArticlesUse of reactive hyperemia – peripheral arterial tonometry and circulating biological markers to predict outcomes in sepsis
Rev Bras Ter Intensiva. 2016;28(4):387-396
DOI 10.5935/0103-507X.20160072
- Vandack Nobre,
- Thiago Bragança Ataíde,
- Luisa Caldeira Brant,
- Clara Rodrigues Oliveira,
- Lucas Vieira Rodrigues,
- Antonio Luiz Pinho Ribeiro,
- Fernanda Barbosa Lopes,
- Ivan Euclides Saraiva,
- Marcus Vinícius Andrade
Views1See moreABSTRACT
Objective:
To evaluate the usefulness and prognostic value of reactive hyperemia – peripheral arterial tonometry in patients with sepsis. Moreover, we investigated the association of reactive hyperemia – peripheral arterial tonometry results with serum levels of certain inflammatory molecules.
Methods:
Prospective study, conducted in an 18-bed mixed intensive care unit for adults. The exclusion criteria included severe immunosuppression or antibiotic therapy initiated more than 48 hours before assessment. We measured the reactive hyperemia – peripheral arterial tonometry on inclusion (day 1) and on day 3. Interleukin-6, interleukin-10, high-mobility group box 1 protein and soluble ST2 levels were measured in the blood obtained upon inclusion.
Results:
Seventeen of the 79 patients (21.6%) enrolled were determined to have reactive hyperemia – peripheral arterial tonometry signals considered technically unreliable and were excluded from the study. Thus, 62 patients were included in the final analysis, and they underwent a total of 95 reactive hyperemia – peripheral arterial tonometry exams within the first 48 hours after inclusion. The mean age was 51.5 (SD: 18.9), and 49 (62%) of the patients were male. Reactive hyperemia indexes from days 1 and 3 were not associated with vasopressor need, Sequential Organ Failure Assessment score, Acute Physiology and Chronic Health Evaluation II score, or 28-day mortality. Among the patients who died, compared with survivors, there was a significant increase in the day 3 reactive hyperemia index compared with day 1 (p = 0.045). There was a weak negative correlation between the day 1 reactive hyperemia – peripheral arterial tonometry index and the levels of high-mobility group box 1 protein (r = -0.287).
Conclusion:
Technical difficulties and the lack of clear associations between the exam results and clinical severity or outcomes strongly limits the utility of reactive hyperemia – peripheral arterial tonometry in septic patients admitted to the intensive care unit.


Search
Search in:
KEY WORDS
Case reports Child Coronavirus infections COVID-19 Critical care Critical illness Extracorporeal membrane oxygenation Infant, newborn Intensive care Intensive care units Intensive care units, pediatric mechanical ventilation Mortality Physical therapy modalities Prognosis Respiration, artificial Respiratory insufficiency risk factors SARS-CoV-2 Sepsis


