You searched for:"Sebastián Welsh"
We found (2) results for your search.-
Original Article
Prognostic value of ventricular diastolic dysfunction in patients with severe sepsis and septic shock
Rev Bras Ter Intensiva. 2015;27(4):333-339
Abstract
Original ArticlePrognostic value of ventricular diastolic dysfunction in patients with severe sepsis and septic shock
Rev Bras Ter Intensiva. 2015;27(4):333-339
DOI 10.5935/0103-507X.20150057
Views0See moreABSTRACT
Objectives:
To evaluate the prevalence of myocardial dysfunction and its prognostic value in patients with severe sepsis and septic shock.
Methods:
Adult septic patients admitted to an intensive care unit were prospectively studied using transthoracic echocardiography within the first 48 hours after admission and thereafter on the 7th-10th days. Echocardiographic variables of biventricular function, including the E/e’ ratio, were compared between survivors and non-survivors.
Results:
A total of 99 echocardiograms (53 at admission and 46 between days 7 – 10) were performed on 53 patients with a mean age of 74 (SD 13) years. Systolic and diastolic dysfunction was present in 14 (26%) and 42 (83%) patients, respectively, and both types of dysfunction were present in 12 (23%) patients. The E/e’ ratio, an index of diastolic dysfunction, was the best predictor of hospital mortality according to the area under the ROC curve (0.71) and was an independent predictor of outcome, as determined by multivariate analysis (OR = 1.36 [1.05 – 1.76], p = 0.02).
Conclusion:
In septic patients admitted to an intensive care unit, echocardiographic systolic dysfunction is not associated with increased mortality. In contrast, diastolic dysfunction is an independent predictor of outcome.
-
Original Article
Lack of agreement between different observers and methods in the measurement of capillary refill time in healthy volunteers: an observational study
Rev Bras Ter Intensiva. 2014;26(3):269-276
Abstract
Original ArticleLack of agreement between different observers and methods in the measurement of capillary refill time in healthy volunteers: an observational study
Rev Bras Ter Intensiva. 2014;26(3):269-276
DOI 10.5935/0103-507X.20140038
Views0See moreObjective:
Peripheral perfusion abnormalities are relevant manifestations of shock. Capillary refill time is commonly used for their evaluation. However, the reproducibility of capillary refill time measurements and their correlation with other variables of peripheral perfusion, have not been comprehensively evaluated. Our goal was to determine, in healthy volunteers, the agreement between different methods of capillary refill time quantification and different observers, as well as their correlation with other markers of peripheral perfusion.
Methods:
We studied 63 healthy volunteers. Two observers measured capillary refill time by means of two methods, direct view (CRTchronometer) and video analysis (CRTvideo). We also measured perfusion index (PI) derived from pulse plethysmography and finger pad temperature (Tºperipheral). The agreement between observers and methods was assessed using the Bland and Altman method. Correlations were calculated using Pearson’s correlation. A p-value<0.05 was considered significant.
Results:
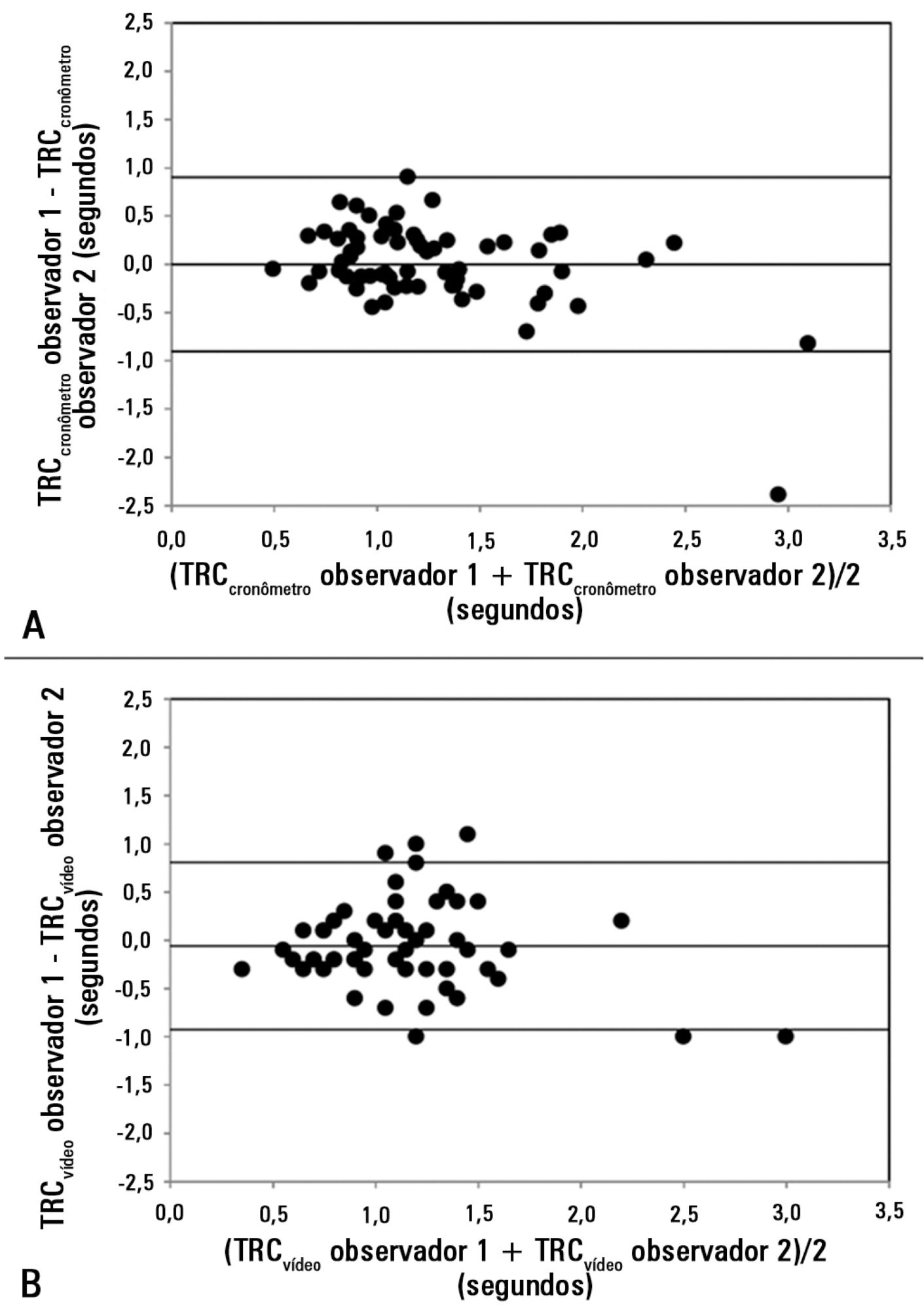
The 95% limits of agreement between the two observers were 1.9 sec for CRTchronometer and 1.7 sec for CRTvideo. The 95% limits of agreement between CRTchronometer and CRTvideo were 1.7 sec for observer 1 and 2.3 sec for observer 2. Measurements of CRTchronometer performed by the two observers were correlated with Tºperipheral. Measurements of CRTvideo performed by the two observers were correlated with Tºperipheral and perfusion index.
Conclusion:
In healthy volunteers, measurements of capillary refill time performed by either different observers or different methods showed poor agreement. Nevertheless, capillary refill time still reflected peripheral perfusion as shown by its correlation with objective variables of peripheral perfusion.
Search
Search in:
KEY WORDS
Case reports Child Coronavirus infections COVID-19 Critical care Critical illness Extracorporeal membrane oxygenation Infant, newborn Intensive care Intensive care units Intensive care units, pediatric mechanical ventilation Mortality Physical therapy modalities Prognosis Respiration, artificial Respiratory insufficiency risk factors SARS-CoV-2 Sepsis




