You searched for:"Luís Coelho"
We found (2) results for your search.-
Original Article
What changed between the peak and plateau periods of the first COVID-19 pandemic wave? A multicentric Portuguese cohort study in intensive care
Rev Bras Ter Intensiva. 2022;34(4):433-442
Abstract
Original ArticleWhat changed between the peak and plateau periods of the first COVID-19 pandemic wave? A multicentric Portuguese cohort study in intensive care
Rev Bras Ter Intensiva. 2022;34(4):433-442
DOI 10.5935/0103-507X.20210037-en
Views1ABSTRACT
Objective:
To analyze and compare COVID-19 patient characteristics, clinical management and outcomes between the peak and plateau periods of the first pandemic wave in Portugal.
Methods:
This was a multicentric ambispective cohort study including consecutive severe COVID-19 patients between March and August 2020 from 16 Portuguese intensive care units. The peak and plateau periods, respectively, weeks 10 – 16 and 17 – 34, were defined.
Results:
Five hundred forty-one adult patients with a median age of 65 [57 – 74] years, mostly male (71.2%), were included. There were no significant differences in median age (p = 0.3), Simplified Acute Physiology Score II (40 versus 39; p = 0.8), partial arterial oxygen pressure/fraction of inspired oxygen ratio (139 versus 136; p = 0.6), antibiotic therapy (57% versus 64%; p = 0.2) at admission, or 28-day mortality (24.4% versus 22.8%; p = 0.7) between the peak and plateau periods. During the peak period, patients had fewer comorbidities (1 [0 – 3] versus 2 [0 – 5]; p = 0.002) and presented a higher use of vasopressors (47% versus 36%; p < 0.001) and invasive mechanical ventilation (58.1 versus 49.2%; p < 0.001) at admission, prone positioning (45% versus 36%; p = 0.04), and hydroxychloroquine (59% versus 10%; p < 0.001) and lopinavir/ritonavir (41% versus 10%; p < 0.001) prescriptions. However, a greater use of high-flow nasal cannulas (5% versus 16%, p < 0.001) on admission, remdesivir (0.3% versus 15%; p < 0.001) and corticosteroid (29% versus 52%, p < 0.001) therapy, and a shorter ICU length of stay (12 days versus 8, p < 0.001) were observed during the plateau.
Conclusion:
There were significant changes in patient comorbidities, intensive care unit therapies and length of stay between the peak and plateau periods of the first COVID-19 wave.
Keywords:acute respiratory distress syndromeAdrenal cortex hormonesCoronavirus infectionsCOVID-19Critical care outcomesCritical illnessIntensive carePandemicsSARS-CoV-2See more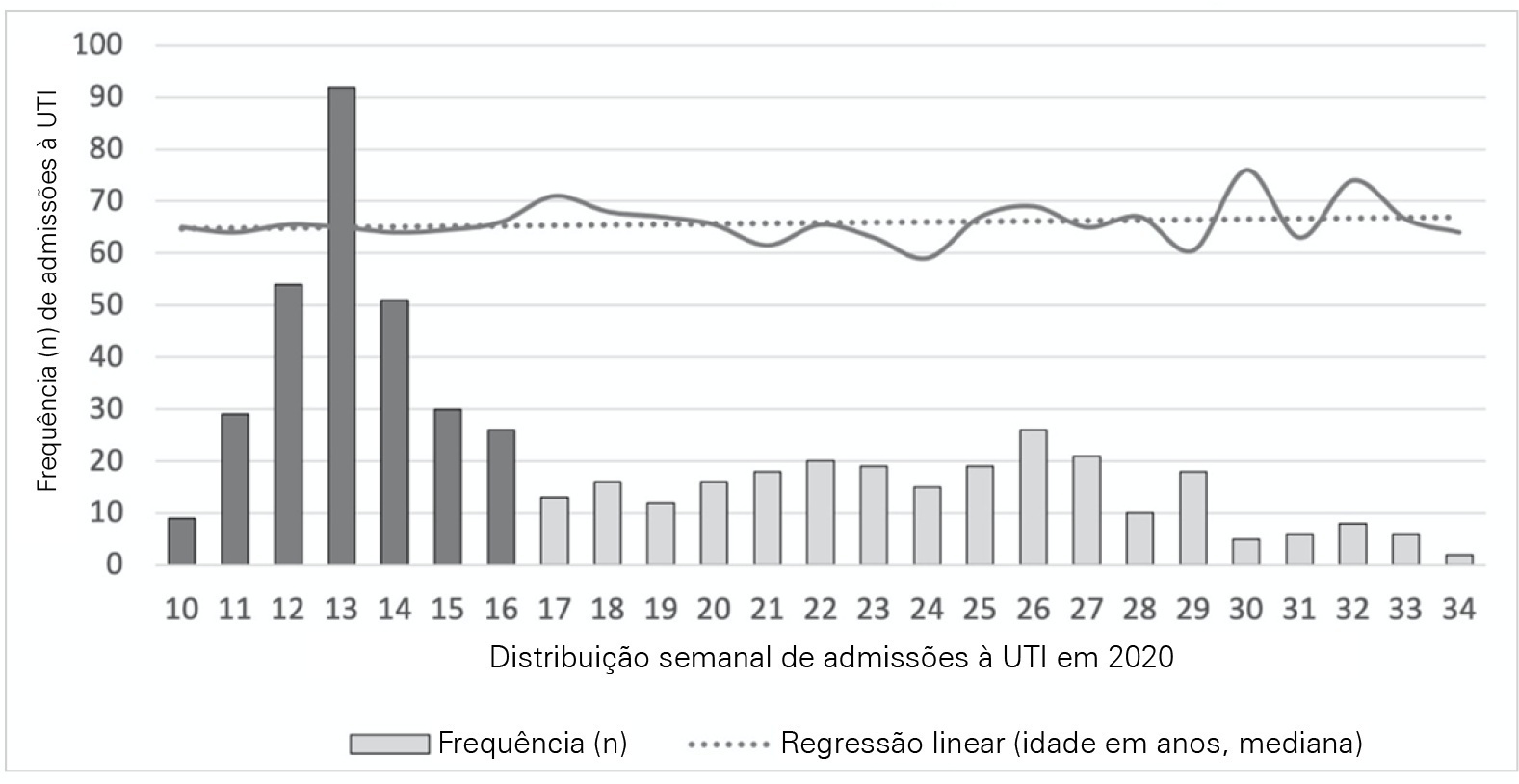
-
Original Article
suPAR in the assessment of post intensive care unit prognosis: a pilot study
Rev Bras Ter Intensiva. 2018;30(4):453-459
Abstract
Original ArticlesuPAR in the assessment of post intensive care unit prognosis: a pilot study
Rev Bras Ter Intensiva. 2018;30(4):453-459
DOI 10.5935/0103-507X.20180062
Views0See moreABSTRACT
Objective:
To determine the performance of soluble urokinase-type plasminogen activator receptor upon intensive care unit discharge to predict post intensive care unit mortality.
Methods:
A prospective observational cohort study was conducted during a 24-month period in an 8-bed polyvalent intensive care unit. APACHE II, SOFA, C-reactive protein, white cell count and soluble urokinase-type plasminogen activator receptor on the day of intensive care unit discharge were collected from patients who survived intensive care unit admission.
Results:
Two hundred and two patients were included in this study, 29 patients (18.6%) of whom died after intensive care unit discharge. Nonsurvivors were older and more seriously ill upon intensive care unit admission with higher severity scores, and nonsurvivors required extended use of vasopressors than did survivors. The area under the receiver operating characteristics curves of SOFA, APACHE II, C-reactive protein, white cell count, and soluble urokinase-type plasminogen activator receptor at intensive care unit discharge as prognostic markers of hospital death were 0.78 (95%CI 0.70 – 0.86); 0.70 (95%CI 0.61 – 0.79); 0.54 (95%CI 0.42 – 0.65); 0.48 (95%CI 0.36 – 0.58); and 0.68 (95%CI 0.58 – 0.78), respectively. SOFA was independently associated with a higher risk of in-hospital mortality (OR 1.673; 95%CI 1.252 – 2.234), 28-day mortality (OR 1.861; 95%CI 1.856 – 2.555) and 90-day mortality (OR 1.584; 95%CI 1.241 – 2.022).
Conclusion:
At intensive care unit discharge, soluble urokinase-type plasminogen activator receptor is a poor predictor of post intensive care unit prognosis.
Search
Search in:
KEY WORDS
Case reports Child Coronavirus infections COVID-19 Critical care Critical illness Extracorporeal membrane oxygenation Infant, newborn Intensive care Intensive care units Intensive care units, pediatric mechanical ventilation Mortality Physical therapy modalities Prognosis Respiration, artificial Respiratory insufficiency risk factors SARS-CoV-2 Sepsis




