You searched for:"Lilian Maria Sobreira Tanaka"
We found (3) results for your search.-
Original Article
Perceptions and practices regarding light sedation in mechanically ventilated patients: a survey on the attitudes of Brazilian critical care physicians
Rev Bras Ter Intensiva. 2022;34(4):426-432
Abstract
Original ArticlePerceptions and practices regarding light sedation in mechanically ventilated patients: a survey on the attitudes of Brazilian critical care physicians
Rev Bras Ter Intensiva. 2022;34(4):426-432
DOI 10.5935/0103-507X.20220278-en
Views3ABSTRACT
Objective:
To characterize the knowledge and perceived attitudes toward pharmacologic interventions for light sedation in mechanically ventilated patients and to understand the current gaps comparing current practice with the recommendations of the Clinical Practice Guidelines for the Prevention and Management of Pain, Agitation/Sedation, Delirium, Immobility, and Sleep Disruption in Adult Patients in the Intensive Care Unit.
Methods:
This was a cross-sectional cohort study based on the application of an electronic questionnaire focused on sedation practices.
Results:
A total of 303 critical care physicians provided responses to the survey. Most respondents reported routine use of a structured sedation scale (281; 92.6%). Almost half of the respondents reported performing daily interruptions of sedation (147; 48.4%), and the same percentage of participants (48.0%) agreed that patients are often over sedated. During the COVID-19 pandemic, participants reported that patients had a higher chance of receiving midazolam compared to before the pandemic (178; 58.8% versus 106; 34.0%; p = 0.05), and heavy sedation was more common during the COVID-19 pandemic (241; 79.4% versus 148; 49.0%; p = 0.01).
Conclusion:
This survey provides valuable data on the perceived attitudes of Brazilian intensive care physicians regarding sedation. Although daily interruption of sedation was a well-known concept and sedation scales were often used by the respondents, insufficient effort was put into frequent monitoring, use of protocols and systematic implementation of sedation strategies. Despite the perception of the benefits linked with light sedation, there is a need to identify improvement targets to propose educational strategies to improve current practices.
Keywords:artificialattitudesConscious sedationHealth knowledgeIntensive care unitspracticeRespirationSurveys and questionnairesSee more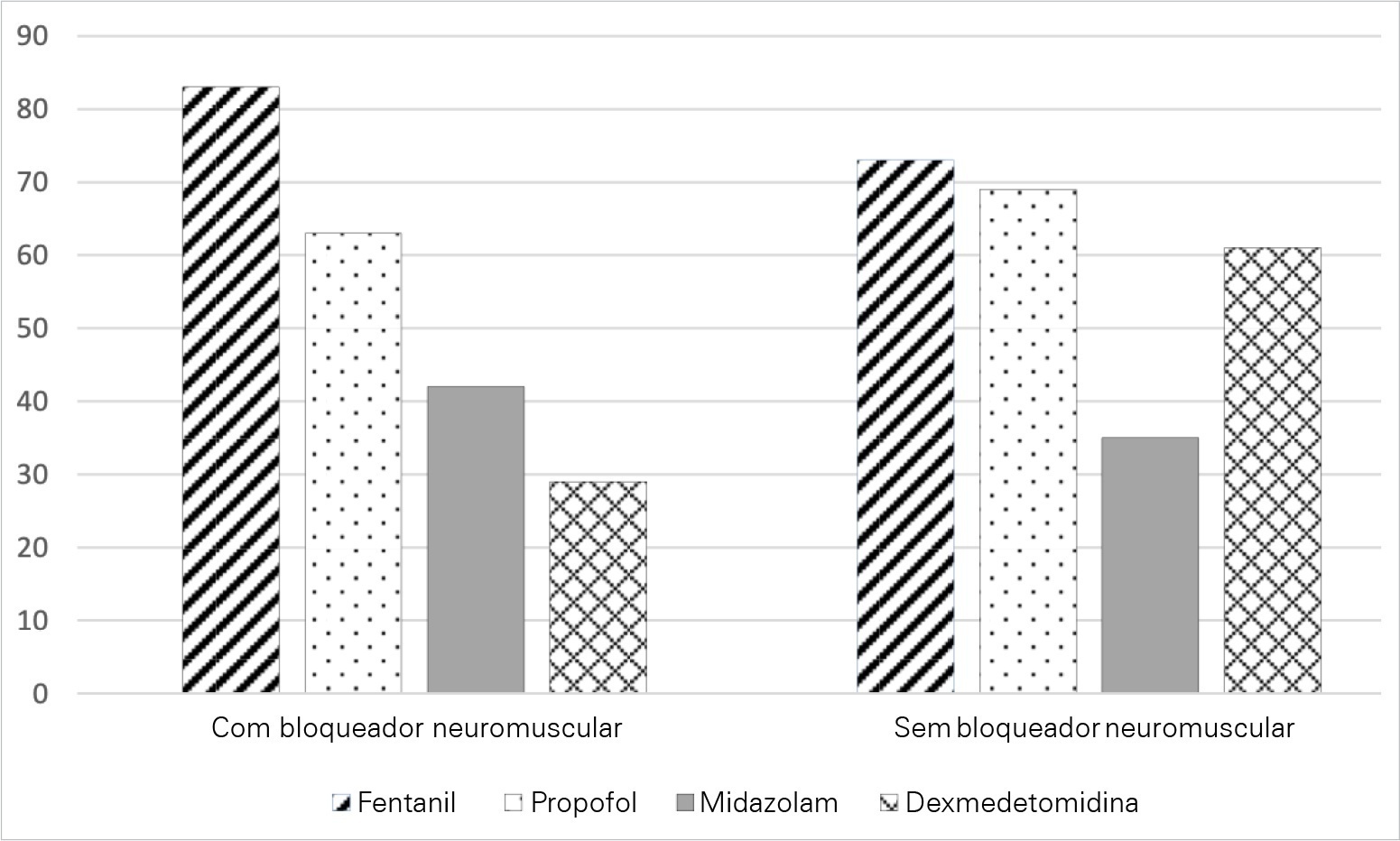
-
Commentary
What every intensivist should know about light sedation for mechanically ventilated patients
Rev Bras Ter Intensiva. 2021;33(4):480-482
Abstract
CommentaryWhat every intensivist should know about light sedation for mechanically ventilated patients
Rev Bras Ter Intensiva. 2021;33(4):480-482
DOI 10.5935/0103-507X.20210069
Views3INTRODUCTIONPain, agitation and anxiety are frequently experienced by patients requiring intensive care unit (ICU) admission. These events are often associated with tracheal intubation, mechanical ventilation (MV) and bedside procedures. Sedatives and analgesics can be used to minimize distress, ensure comfort, and decrease the work of breathing to achieve better synchrony with the ventilator. A number […]See more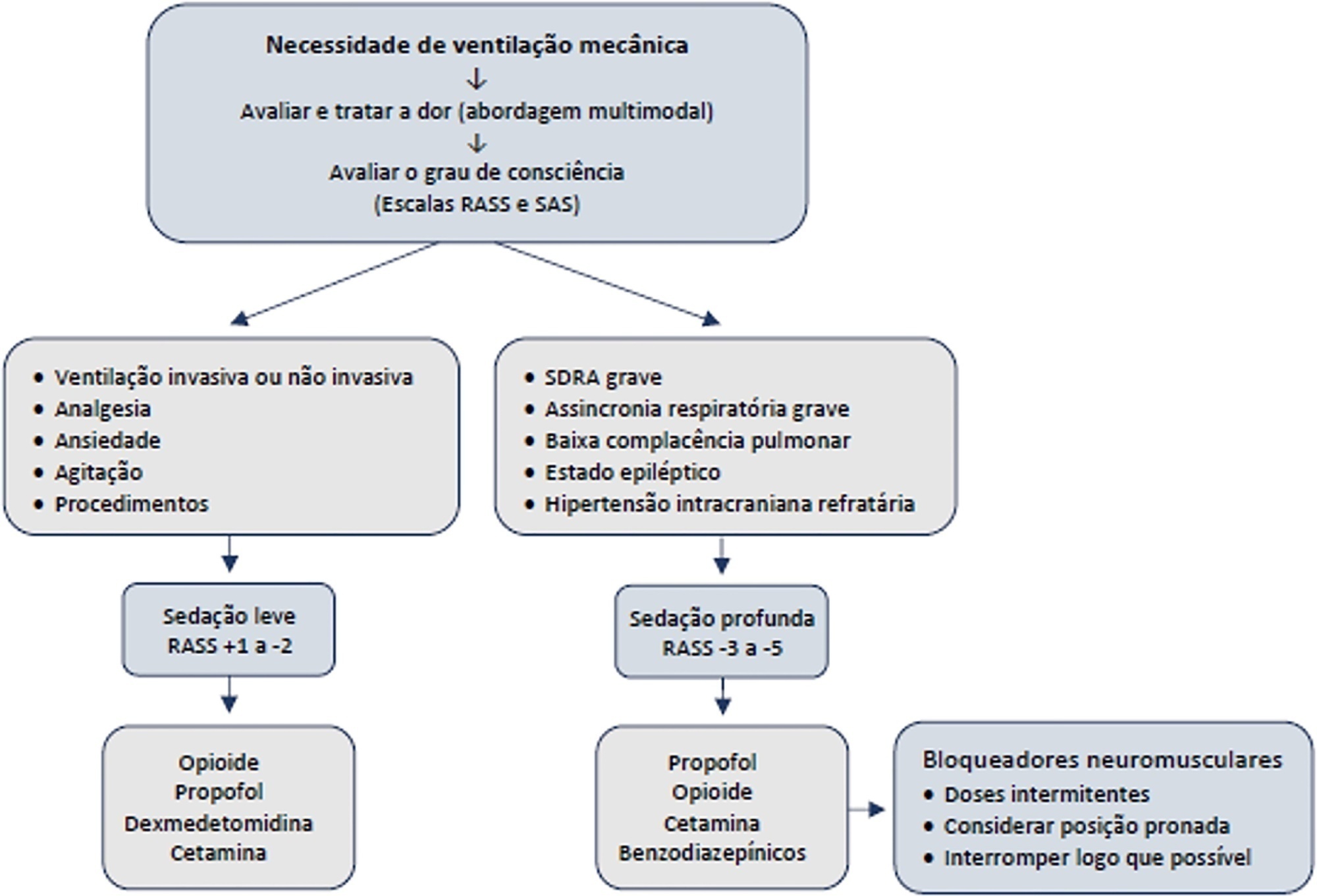
-
Original Article
Delirium in intensive care unit patients under noninvasive ventilation: a multinational survey
Rev Bras Ter Intensiva. 2015;27(4):360-368
Abstract
Original ArticleDelirium in intensive care unit patients under noninvasive ventilation: a multinational survey
Rev Bras Ter Intensiva. 2015;27(4):360-368
DOI 10.5935/0103-507X.20150061
Views0ABSTRACT
Objective:
To conduct a multinational survey of intensive care unit professionals to determine the practices on delirium assessment and management, in addition to their perceptions and attitudes toward the evaluation and impact of delirium in patients requiring noninvasive ventilation.
Methods:
An electronic questionnaire was created to evaluate the profiles of the respondents and their related intensive care units, the systematic delirium assessment and management and the respondents’ perceptions and attitudes regarding delirium in patients requiring noninvasive ventilation. The questionnaire was distributed to the cooperative network for research of the Associação de Medicina Intensiva Brasileira (AMIB-Net) mailing list and to researchers in different centers in Latin America and Europe.
Results:
Four hundred thirty-six questionnaires were available for analysis; the majority of the questionnaires were from Brazil (61.9%), followed by Turkey (8.7%) and Italy (4.8%). Approximately 61% of the respondents reported no delirium assessment in the intensive care unit, and 31% evaluated delirium in patients under noninvasive ventilation. The Confusion Assessment Method for the intensive care unit was the most reported validated diagnostic tool (66.9%). Concerning the indication of noninvasive ventilation in patients already presenting with delirium, 16.3% of respondents never allow the use of noninvasive ventilation in this clinical context.
Conclusion:
This survey provides data that strongly reemphasizes poor efforts toward delirium assessment and management in the intensive care unit setting, especially regarding patients requiring noninvasive ventilation.
Keywords:Attitude of health personnelCritical careDeliriumDiagnostic techniques, neurologicalNoninvasive ventilationQuestionnairesSee more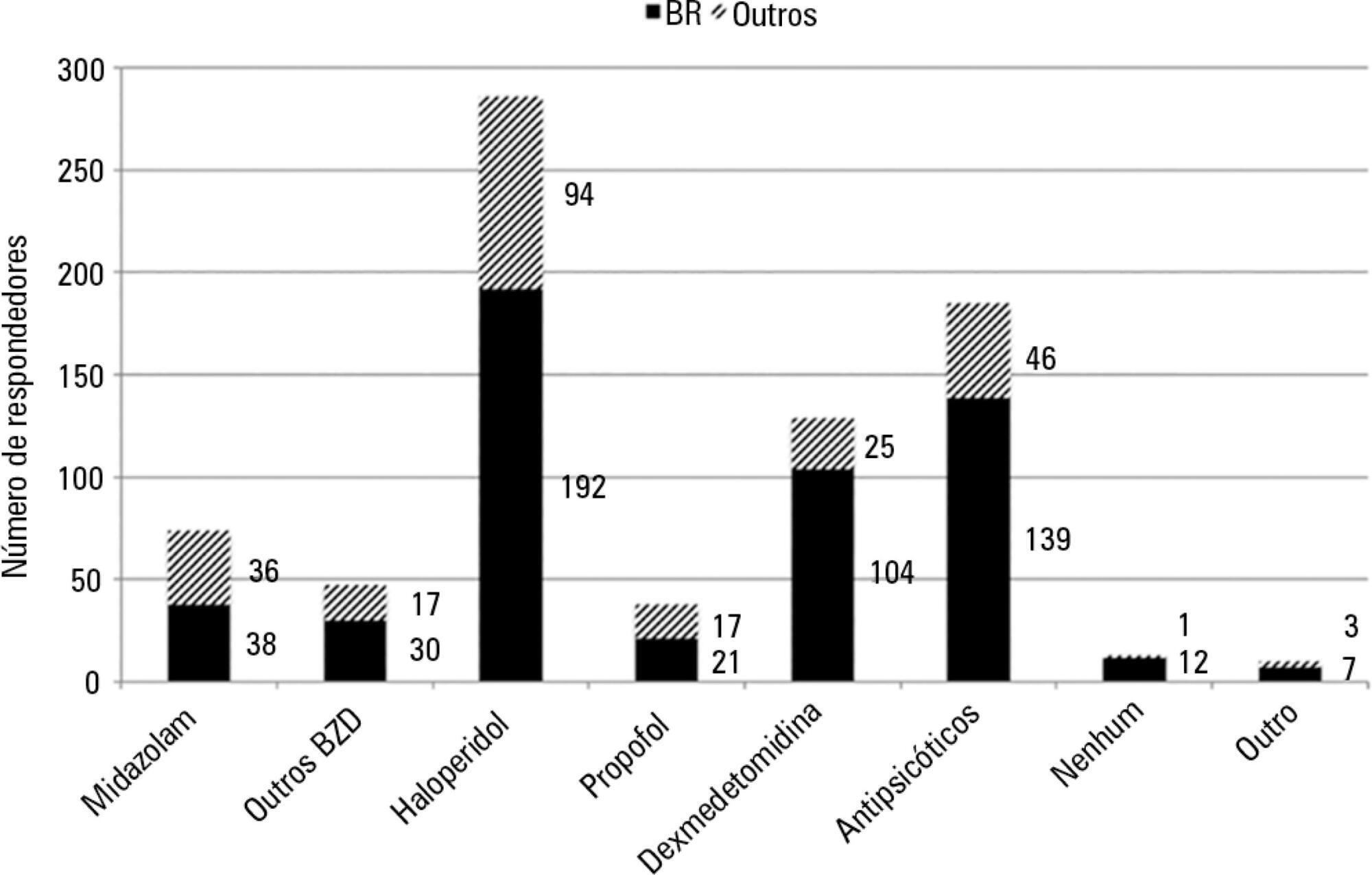
Search
Search in:
KEY WORDS
Case reports Child Coronavirus infections COVID-19 Critical care Critical illness Extracorporeal membrane oxygenation Infant, newborn Intensive care Intensive care units Intensive care units, pediatric mechanical ventilation Mortality Physical therapy modalities Prognosis Respiration, artificial Respiratory insufficiency risk factors SARS-CoV-2 Sepsis




