You searched for:"José Roberto Lapa e Silva"
We found (3) results for your search.-
Original Article
Planning and understanding the intensive care network in the State of Rio de Janeiro (RJ), Brazil: a complex societal problem
Rev Bras Ter Intensiva. 2018;30(3):347-357
Abstract
Original ArticlePlanning and understanding the intensive care network in the State of Rio de Janeiro (RJ), Brazil: a complex societal problem
Rev Bras Ter Intensiva. 2018;30(3):347-357
DOI 10.5935/0103-507X.20180053
Views0ABSTRACT
Objectives:
To determine the optimal number of adult intensive care unit beds to reduce patient’s queue waiting time and to propose policy strategies.
Methods:
Multimethodological approach: (a) quantitative time series and queueing theory were used to predict the demand and estimate intensive care unit beds in different scenarios; (b) qualitative focus group and content analysis were used to explore physicians’ attitudes and provide insights into their behaviors and belief-driven healthcare delivery changes.
Results:
A total of 33,101 requests for 268 regulated intensive care unit beds in one year resulted in 25% admissions, 55% queue abandonment and 20% deaths. Maintaining current intensive care unit arrival and exit rates, there would need 628 beds to ensure a maximum wait time of six hours. A reduction of the current abandonment rates due to clinical improvement or the average intensive care unit length of stay would decrease the number of beds to 471 and 366, respectively. If both were reduced, the number would reach 275 beds. The interviews generated 3 main themes: (1) the doctor’s conflict: fair, legal, ethical and shared priorities in the decision-making process; (2) a failure of access: invisible queues and a lack of infrastructure; and (3) societal drama: deterioration of public policies and health care networks.
Conclusion:
The queue should be treated as a complex societal problem with a multifactorial origin requiring integrated solutions. Improving intensive care unit protocols and reengineering the general wards may decrease the length of stay. It is essential to redefine and consolidate the regulatory centers to organize the queue and provide available resources in a timely manner, by using priority criteria, working with stakeholders to guarantee clinical governance and network organization.
Keywords:Health policy, planning and managementHealth services accessibilityHospital bed capacityIntensive care unit organization & administrationManagementQualitative researchUnified Health SystemSee more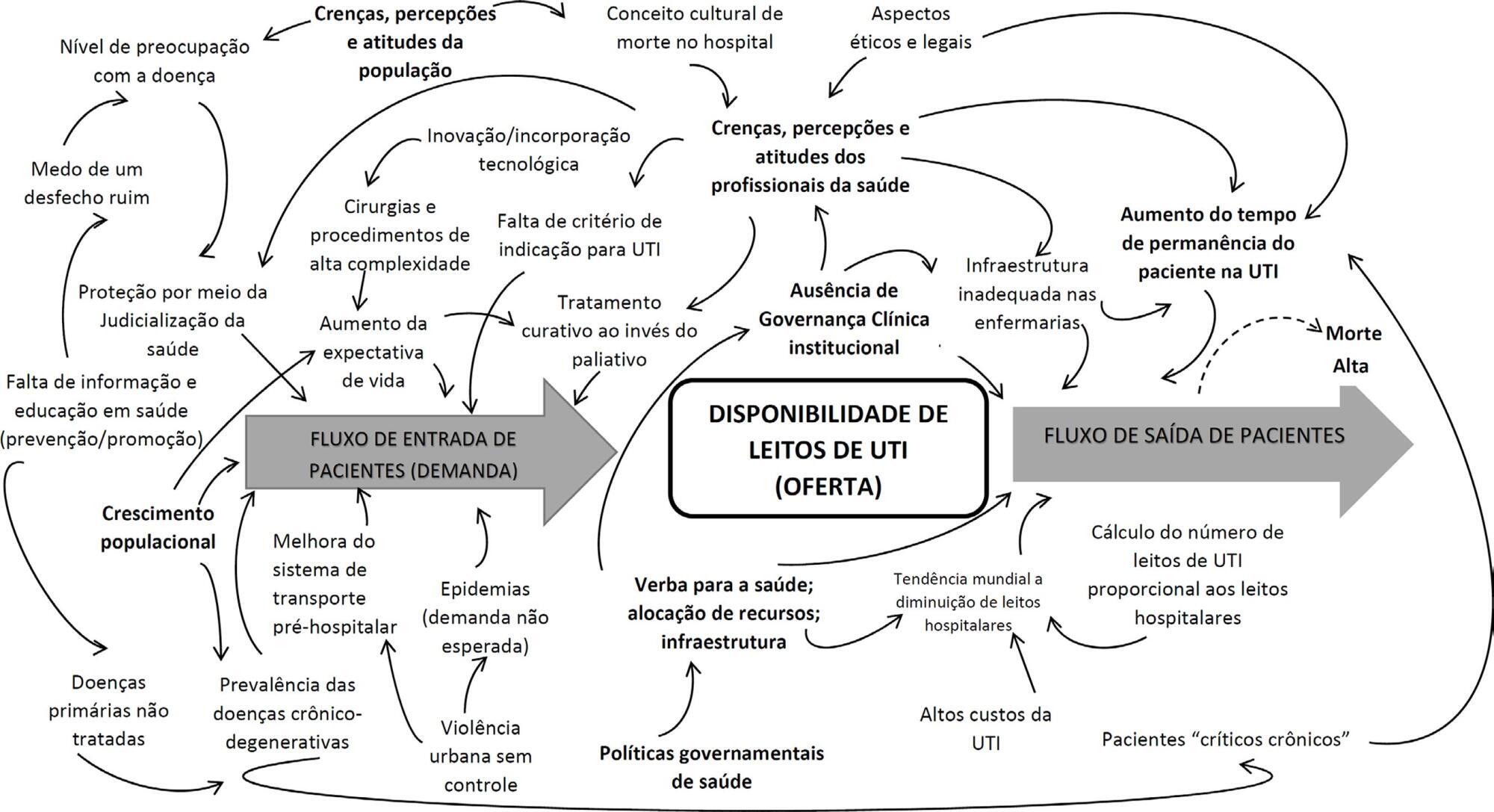
-
Review Articles
Use of biomarkers in pediatric sepsis: literature review
Rev Bras Ter Intensiva. 2016;28(4):472-482
Abstract
Review ArticlesUse of biomarkers in pediatric sepsis: literature review
Rev Bras Ter Intensiva. 2016;28(4):472-482
DOI 10.5935/0103-507X.20160080
Views0See moreABSTRACT
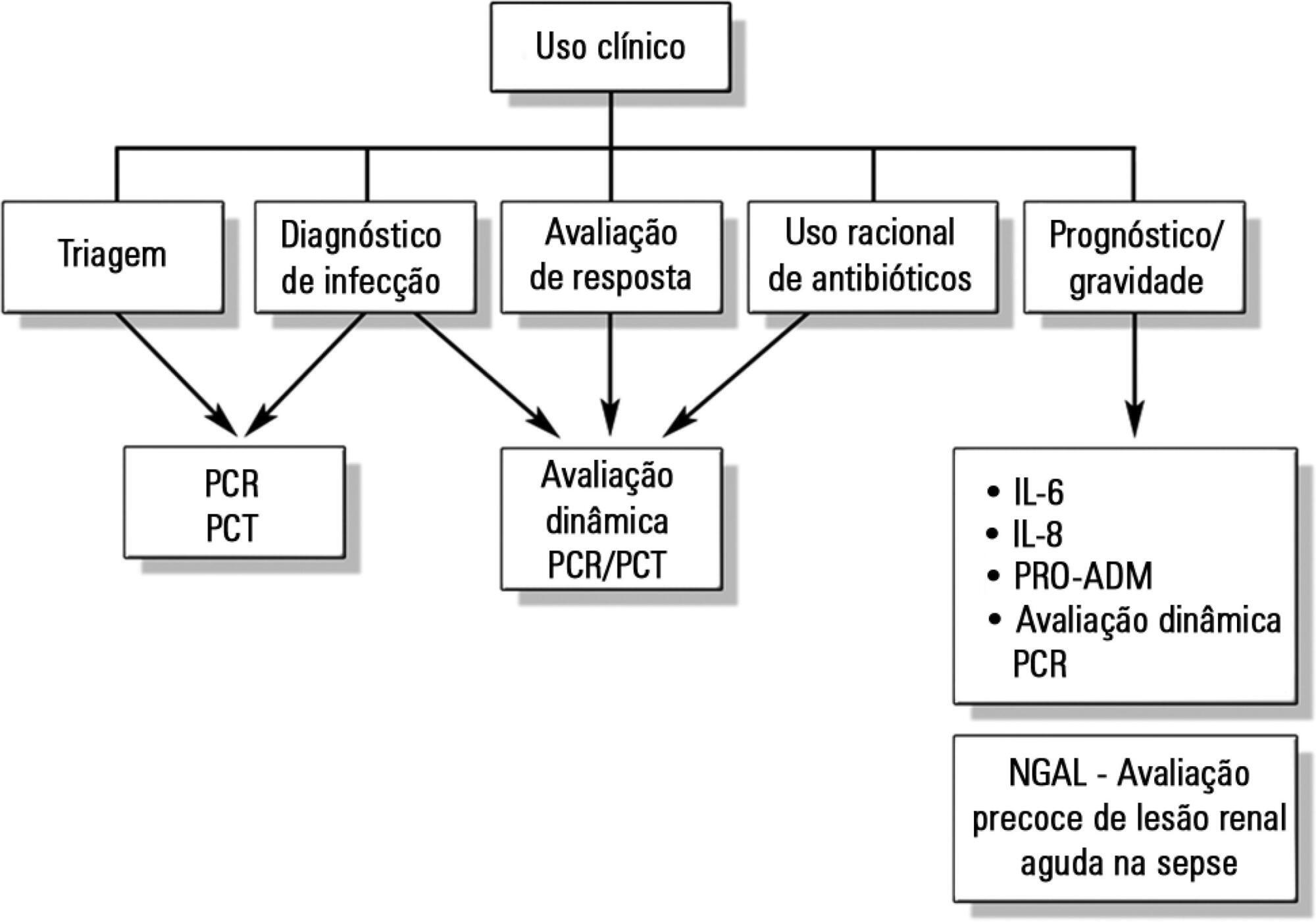
Despite advances in recent years, sepsis is still a leading cause of hospitalization and mortality in infants and children. The presence of biomarkers during the response to an infectious insult makes it possible to use such biomarkers in screening, diagnosis, prognosis (risk stratification), monitoring of therapeutic response, and rational use of antibiotics (for example, the determination of adequate treatment length). Studies of biomarkers in sepsis in children are still relatively scarce. This review addresses the use of biomarkers in sepsis in pediatric patients with emphasis on C-reactive protein, procalcitonin, interleukins 6, 8, and 18, human neutrophil gelatinase, and proadrenomedullin. Assessment of these biomarkers may be useful in the management of pediatric sepsis.
Search
Search in:
KEY WORDS
Case reports Child Coronavirus infections COVID-19 Critical care Critical illness Extracorporeal membrane oxygenation Infant, newborn Intensive care Intensive care units Intensive care units, pediatric mechanical ventilation Mortality Physical therapy modalities Prognosis Respiration, artificial Respiratory insufficiency risk factors SARS-CoV-2 Sepsis