Abstract
Rev Bras Ter Intensiva. 2022;34(4):469-476
DOI 10.5935/0103-507X.20220429-en
To evaluate the effects of critical illness on the functional status of children aged zero to 4 years with or without a history of prematurity after discharge from the pediatric intensive care unit.
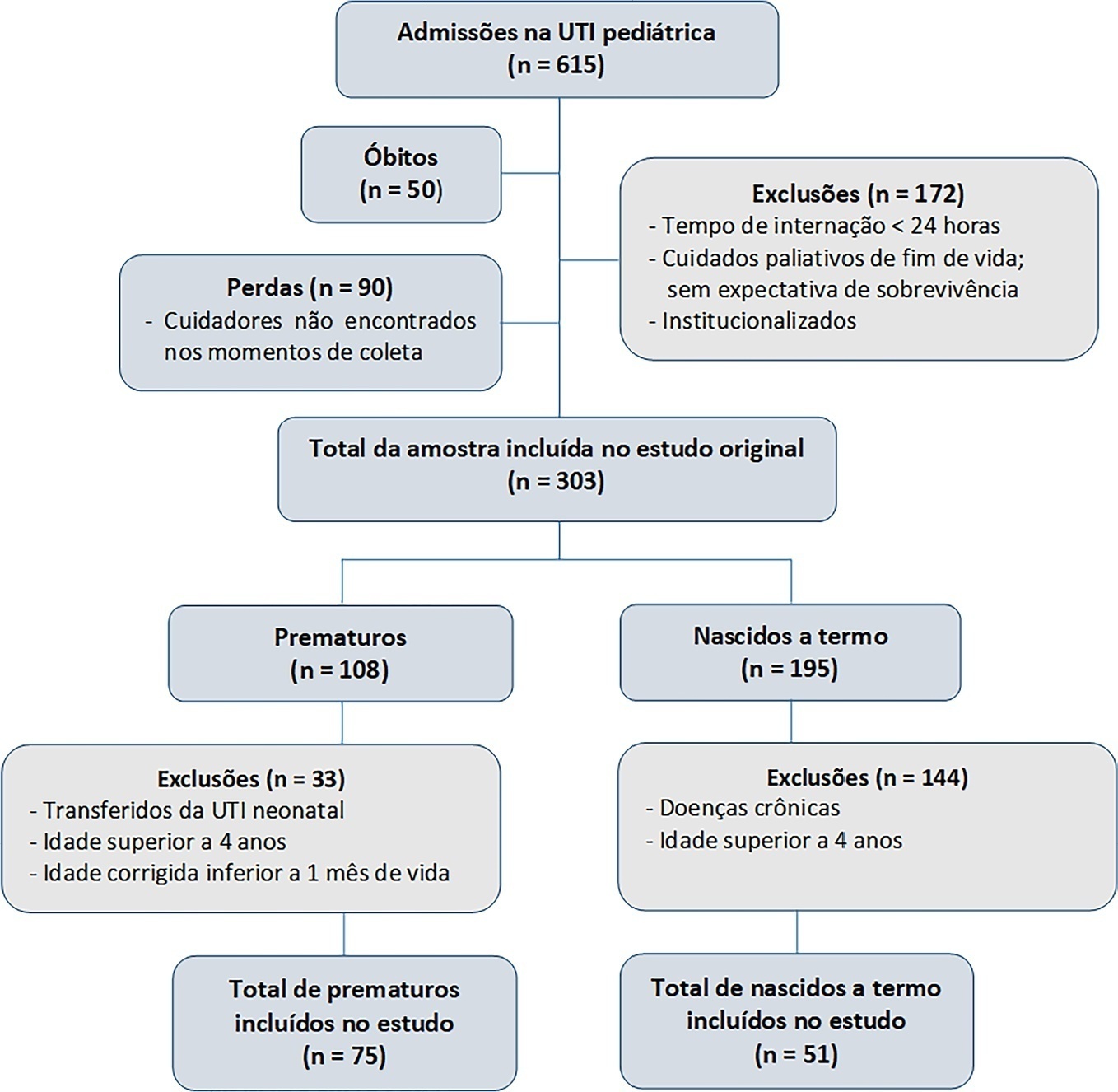
This was a secondary cross-sectional study nested in an observational cohort of survivors from a pediatric intensive care unit. Functional assessment was performed using the Functional Status Scale within 48 hours after discharge from the pediatric intensive care unit.
A total of 126 patients participated in the study, 75 of whom were premature, and 51 of whom were born at term. Comparing the baseline and functional status at pediatric intensive care unit discharge, both groups showed significant differences (p < 0.001). Preterm patients exhibited greater functional decline at discharge from the pediatric intensive care unit (61%). Among patients born at term, there was a significant correlation between the Pediatric Index of Mortality, duration of sedation, duration of mechanical ventilation and length of hospital stay with the functional outcomes (p = 0.05).
Most patients showed a functional decline at discharge from the pediatric intensive care unit. Although preterm patients had a greater functional decline at discharge, sedation and mechanical ventilation duration influenced functional status among patients born at term.
Abstract
Rev Bras Ter Intensiva. 2021;33(3):353-361
DOI 10.5935/0103-507X.20210051
To translate and cross-culturally adapt the Early Rehabilitation Index to Brazilian Portuguese and validate the Early Rehabilitation Barthel Index for use in the intensive care unit to assess functional status.
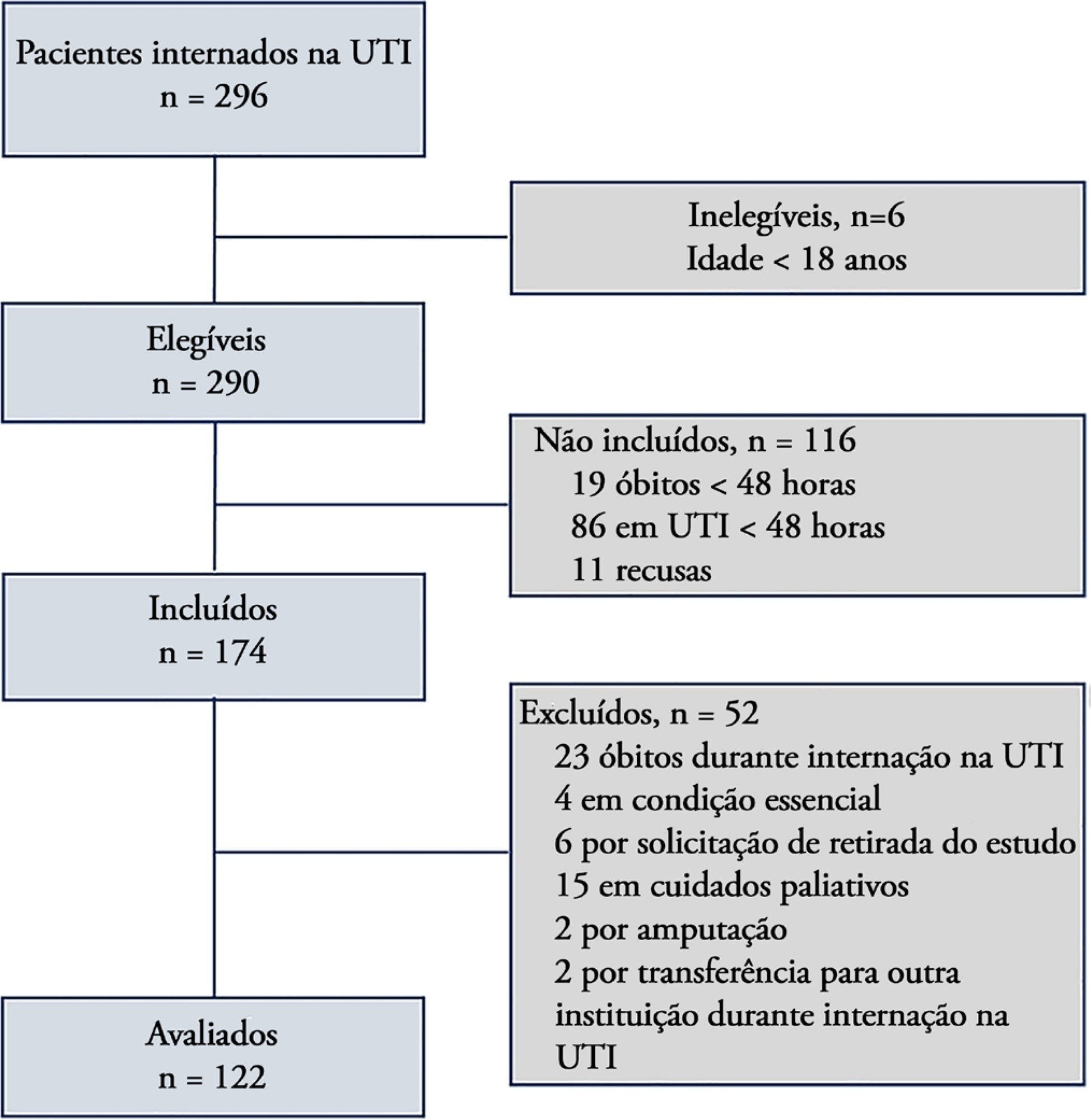
The following steps were performed: preparation, translation, reconciliation, back-translation, revision, harmonization, pretesting, and psychometric evaluation. After this initial process, the Portuguese version was applied by two evaluators to patients hospitalized in the intensive care unit for at least 48 hours. The reliability of the scale was assessed by internal consistency, interrater reliability, and floor and ceiling effects. To measure construct validity, the Early Rehabilitation Barthel Index was correlated with instruments typically used to assess functional status in the intensive care unit.
A total of 122 patients with a median age of 56 (46.8 - 66) years participated in the study. The Early Rehabilitation Barthel Index had adequate reliability, with a Cronbach’s alpha coefficient of 0.65. The interrater reliability was excellent, with an intraclass correlation coefficient of 0.94 (95%CI 0.92 - 0.96), and agreement was moderate to excellent, with a kappa agreement index of 0.54 to 1.0. The floor and ceiling effects were minimal. The validity of the Early Rehabilitation Barthel Index was observed through its correlations with the total Perme score (rho = 0.72), the Functional Status Score for the ICU (rho = 0.77), the Physical Function in the Intensive Care Test score (rho = 0.69), and the Medical Research Council sum score (rho = 0.58), in addition to handgrip strength (rho = 0.58) and knee extensor strength measured by hand-held dynamometry (rho = 0.55), all with p < 0.001.
The adapted versions of the Early Rehabilitation Index for Brazilian Portuguese and, in its entirety, the Early Rehabilitation Barthel Index are reliable and valid for assessing the functional status of patients at discharge from the intensive care unit.
Search
Search in:
Case reports (56) Child (53) Coronavirus infections (34) COVID-19 (46) Critical care (116) Critical illness (54) Extracorporeal membrane oxygenation (26) Infant, newborn (27) Intensive care (72) Intensive care units (256) Intensive care units, pediatric (31) mechanical ventilation (38) Mortality (76) Physical therapy modalities (28) Prognosis (61) Respiration, artificial (119) Respiratory insufficiency (26) risk factors (34) SARS-CoV-2 (28) Sepsis (98)