You searched for:"Fernando Suparregui Dias"
We found (14) results for your search.Abstract
Revista Brasileira de Terapia Intensiva. 2011;23(4):410-425
DOI 10.1590/S0103-507X2011000400005
Brain death (BD) alters the pathophysiology of patients and may damage the kidneys, the lungs, the heart and the liver. To obtain better quality transplant organs, intensive care physicians in charge of the maintenance of deceased donors should attentively monitor these organs. Careful hemodynamic, ventilatory and bronchial clearance management minimizes the loss of kidneys and lungs. The evaluation of cardiac function and morphology supports the transplant viability assessment of the heart. The monitoring of liver function, the management of the patient's metabolic status and the evaluation of viral serology are fundamental for organ selection by the transplant teams and for the care of the transplant recipient
Abstract
Revista Brasileira de Terapia Intensiva. 2009;21(4):416-424
DOI 10.1590/S0103-507X2009000400012
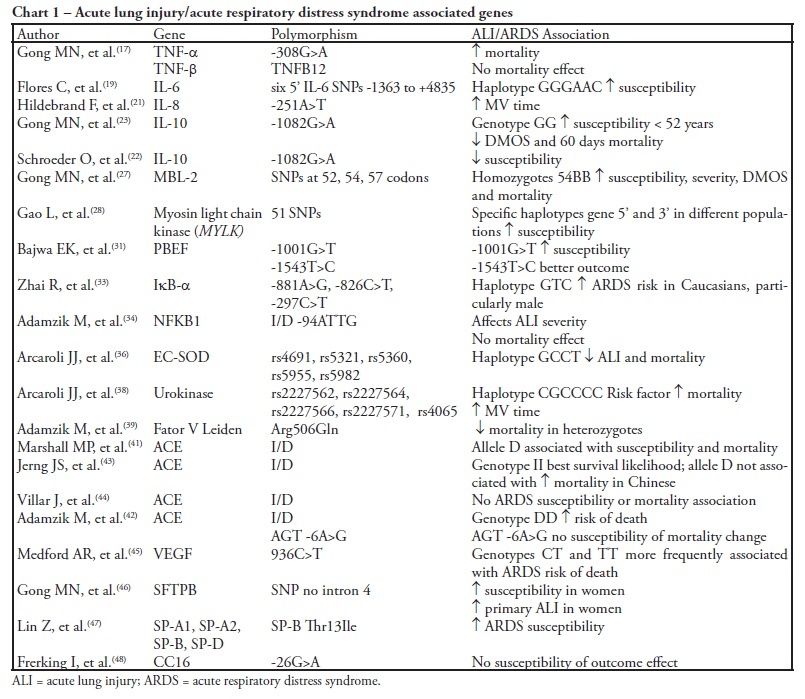
Acute lung injury and its most severe presentation, acute respiratory distress syndrome, are a common denominator for several diseases which can lead to exaggerated lung inflammation. In the last years this variability has been ascribed, at least partially, to genetic issues. This study aims to review the role of the main genes involved in acute lung injury and acute respiratory distress syndrome susceptibility, morbidity and mortality. By search on PubMed and LiLACS databases, using the key words acute lung injury, acute respiratory distress syndrome and adult acute respiratory distress syndrome in combination with genetic polymorphisms, 69 papers were selected, from which 38 were included in this review. Were also considered relevant articles extracted from the reference lists in the articles selected from the databases. Genetic polymorphisms are gene variations in at least 1% population. These gene variations may influence the inflammatory response mediators' expression, directly affecting the susceptibility to acute lung injury, the intensity of lung parenchyma inflammation, the development clinical course and outcome. Association studies reproducible in large populations will definitely allow genomics to be included into the diagnostic and therapeutic armamentarium for acute lung injury/acute respiratory distress syndrome patients.
Abstract
Revista Brasileira de Terapia Intensiva. 2017;29(4):520-521
DOI 10.5935/0103-507X.20170074
Abstract
Revista Brasileira de Terapia Intensiva. 2006;18(1):63-77
DOI 10.1590/S0103-507X2006000100012
BACKGROUND AND OBJECTIVES: Monitoring of vital functions is one of the most important tools in the management of critically ill patients. Nowadays is possible to detect and analyze a great deal of physiologic data using a lot of invasive and non-invasive methods. The intensivist must be able to select and carry out the most appropriate monitoring technique according to the patient requirements and taking into account the benefit/risk ratio. Despite the fast development of non invasive monitoring techniques, invasive hemodynamic monitoring using Pulmonary Artery Catheter still is one of the basic procedures in Critical Care. The aim was to define recommendations about clinical utility of basic hemodynamic monitoring methods and the Use of Pulmonary Artery Catheter. METHODS: Modified Delphi methodology was used to create and quantify the consensus between the participants. AMIB indicated a coordinator who invited more six experts in the area of monitoring and hemodynamic support to constitute the Consensus Advisory Board. Twenty-five physicians and nurses selected from different regions of the country completed the expert panel, which reviewed the pertinent bibliography listed at the MEDLINE in the period from 1996 to 2004. RESULTS: Recommendations were made based on 55 questions about the use of central venous pressure, invasive arterial pressure, pulmonary artery catheter and its indications in different settings. CONCLUSIONS: Evaluation of central venous pressure and invasive arterial pressure, besides variables obtained by the PAC allow the understanding of cardiovascular physiology that is of great value to the care of critically ill patients. However, the correct use of these tools is fundamental to achieve the benefits due to its use.
Abstract
Revista brasileira de terapia intensiva. 2014;26(2):77-78
DOI 10.5935/0103-507X.20140012
Abstract
Revista Brasileira de Terapia Intensiva. 2006;18(1):9-17
DOI 10.1590/S0103-507X2006000100003
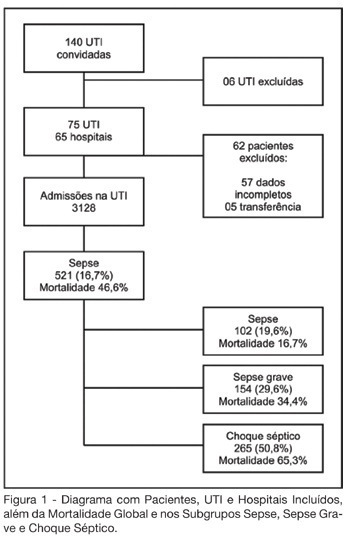
BACKGROUND AND OBJECTIVES: Sepsis represents the major cause of death in the ICUs all over the world. Many studies have shown an increasing incidence over time and only a slight reduce in mortality. Many new treatment strategies are arising and we should define the incidence and features of sepsis in Brazil. METHODS: Prospective cohort study in sixty-five hospitals all over Brazil. The patients who were admitted or who developed sepsis during the month of September, 2003 were enrolled. They were followed until the 28th day and/or until their discharge. The diagnoses were made in accordance to the criteria proposed by ACCP/SCCM. It were evaluated demographic features, APACHE II score, SOFA (Sepsis-related Organ Failure Assessment) score, mortality, sources of infections, microbiology, morbidities and length of stay (LOS). RESULTS: Seventy-five ICUs from all regions of Brazil took part in the study.3128 patients were identified and 521 (16.7%) filled the criteria of sepsis, severe sepsis or septic shock. Mean age was 61.7 (IQR 39-79), 293 (55.7%) were males, and the overall 28-day mortality rate was 46.6%. Average APACHE II score was 20 and SOFA score on the first day was 7 (IQR 4-10). SOFA score in the mortality group was higher on day 1 (8, IQR 5-11), and had increased on day 3 (9, IQR 6-12). The mortality rate for sepsis, severe sepsis and septic shock was 16.7%, 34.4% and 65.3%, respectively. The average LOS was 15 days (IQR 5-22). The two main sources of infection were the respiratory tract (69%) and the abdomen one (23.1%). Gram-negative bacilli were more prevalent (40.1%). Gram-positive cocci were identified in 32.8% and fungi infections in 5%. Mechanical ventilation was observed in 82.1% of the patients, Swan-Ganz catheter in 18.8%, vasopressors in 66.2% and hemotransfusion in 44.7%. CONCLUSIONS: It was observed a high mortality of sepsis in the ICUs in Brazil. The high frequency of septic shock demonstrated a group at high risk of death. In order to have a better use of the resources and reduce in mortality during the next 5 years, it is very important to identify our specific features related to this syndrome.