You searched for:"Paulo Mergulhão"
We found (4) results for your search.-
Original Article
Prognostic value of hyperlactatemia in infected patients admitted to intensive care units: a multicenter study
Rev Bras Ter Intensiva. 2022;34(1):154-162
Abstract
Original ArticlePrognostic value of hyperlactatemia in infected patients admitted to intensive care units: a multicenter study
Rev Bras Ter Intensiva. 2022;34(1):154-162
DOI 10.5935/0103-507X.20220010-en
Views1See moreABSTRACT
Objective:
To evaluate the influence of patient characteristics on hyperlactatemia in an infected population admitted to intensive care units and the influence of hyperlactatemia severity on hospital mortality.
Methods:
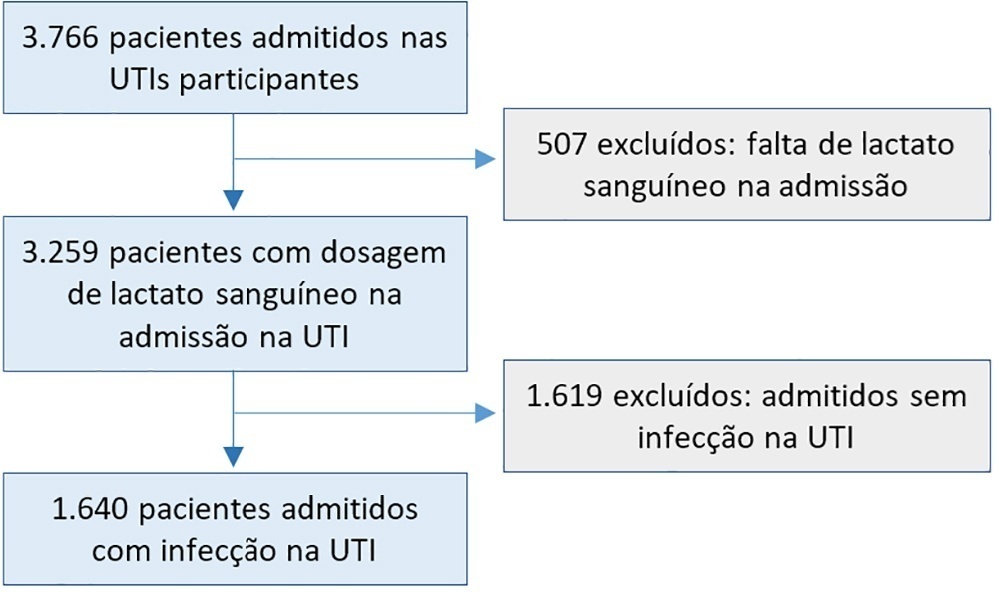
A post hoc analysis of hyperlactatemia in the INFAUCI study, a national prospective, observational, multicenter study, was conducted in 14 Portuguese intensive care units. Infected patients admitted to intensive care units with a lactate measurement in the first 12 hours of admission were selected. Sepsis was identified according to the Sepsis-2 definition accepted at the time of data collection. The severity of hyperlactatemia was classified as mild (2 – 3.9mmol/L), moderate (4.0 – 9.9mmol/L) or severe (> 10mmol/L).
Results:
In a total of 1,640 patients infected on admission, hyperlactatemia occurred in 934 patients (57%), classified as mild, moderate and severe in 57.0%, 34.4% and 8.7% of patients, respectively. The presence of hyperlactatemia and a higher degree of hyperlactatemia were both associated with a higher Simplified Acute Physiology Score II, a higher Charlson Comorbidity Index and the presence of septic shock. The lactate Receiver Operating Characteristic curve for hospital mortality had an area under the curve of 0.64 (95%CI 0.61 – 0.72), which increased to 0.71 (95%CI 0.68 – 0.74) when combined with Sequential Organ Failure Assessment score. In-hospital mortality with other covariates adjusted by Simplified Acute Physiology Score II was associated with moderate and severe hyperlactatemia, with odds ratio of 1.95 (95%CI 1.4 – 2.7; p < 0.001) and 4.54 (95%CI 2.4 - 8.5; p < 0.001), respectively.
Conclusion:
Blood lactate levels correlate independently with in-hospital mortality for moderate and severe degrees of hyperlactatemia.
-
Special Article
Update of the recommendations of the Sociedade Portuguesa de Cuidados Intensivos and the Infection and Sepsis Group for the approach to COVID-19 in Intensive Care Medicine
Rev Bras Ter Intensiva. 2021;33(4):487-536
Abstract
Special ArticleUpdate of the recommendations of the Sociedade Portuguesa de Cuidados Intensivos and the Infection and Sepsis Group for the approach to COVID-19 in Intensive Care Medicine
Rev Bras Ter Intensiva. 2021;33(4):487-536
DOI 10.5935/0103-507X.0103-507X-rbti-20210080
Views0ABSTRACT
Introduction:
The Sociedade Portuguesa de Cuidados Intensivos and the Infection and Sepsis Group have previously issued health service and management recommendations for critically ill patients with COVID-19. Due to the evolution of knowledge, the panel of experts was again convened to review the current evidence and issue updated recommendations.
Methods:
A national panel of experts who declared that they had no conflicts of interest regarding the development of the recommendations was assembled. Operational questions were developed based on the PICO methodology, and a rapid systematic review was conducted by consulting different bibliographic sources. The panel determined the direction and strength of the recommendations using two Delphi rounds, conducted in accordance with the principles of the GRADE system. A strong recommendation received the wording “is recommended”, and a weak recommendation was written as “is suggested.”
Results:
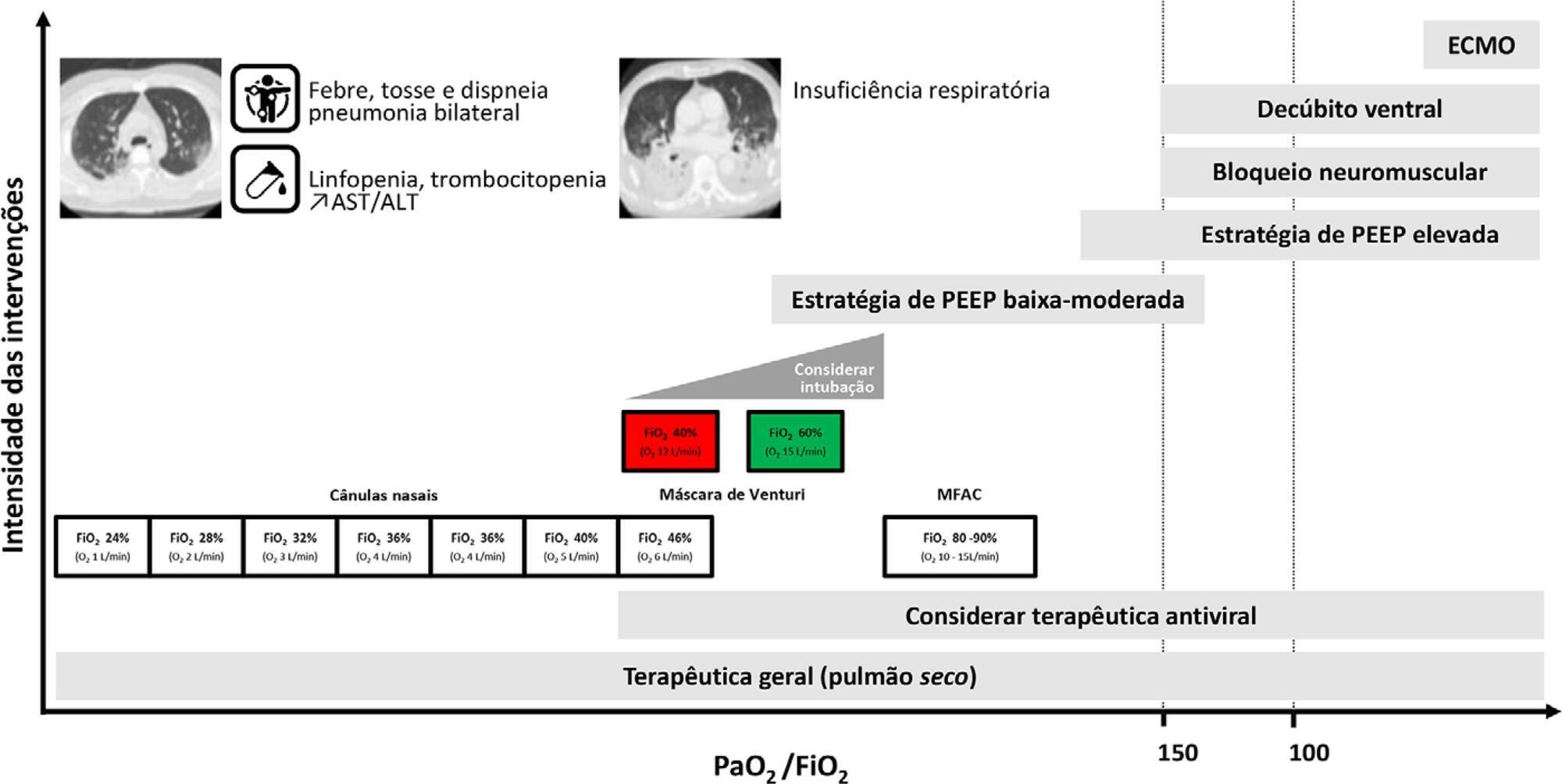
A total of 48 recommendations and 30 suggestions were issued, covering the following topics: diagnosis of SARS-CoV-2 infection, coinfection and superinfection; criteria for admission, cure and suspension of isolation; organization of services; personal protective equipment; and respiratory support and other specific therapies (antivirals, immunomodulators and anticoagulation).
Conclusion:
These recommendations, specifically oriented to the Portuguese reality but that may also apply to Portuguese-speaking African countries and East Timor, aim to support health professionals in the management of critically ill patients with COVID-19. They will be continuously reviewed to reflect the progress of our understanding and the treatment of this pathology.
Keywords:Coronavirus infectionsCOVID-19/diagnosisCOVID-19/therapyPractice guidelines as topicSARS-CoV-2See more -
Commentary
What every intensivist must know about antimicrobial stewardship: its pitfalls and its challenges
Rev Bras Ter Intensiva. 2020;32(2):207-212
Abstract
CommentaryWhat every intensivist must know about antimicrobial stewardship: its pitfalls and its challenges
Rev Bras Ter Intensiva. 2020;32(2):207-212
DOI 10.5935/0103-507X.20200037
Views0Antimicrobial stewardship should not be performed addressing cost containment as the main purposeThe absence of a universal definition for AMS combined with the lack of international guidance and standards are among the many barriers to the implementation of these programs globally. The purpose of AMS is to promote the optimal/prudent/responsible use of antibiotics to optimize […]See more -
Special Article
Recommendations from the Sociedade Portuguesa de Cuidados Intensivos and Infection & Sepsis Group for intensive care approach to COVID-19
Rev Bras Ter Intensiva. 2020;32(1):2-10
Abstract
Special ArticleRecommendations from the Sociedade Portuguesa de Cuidados Intensivos and Infection & Sepsis Group for intensive care approach to COVID-19
Rev Bras Ter Intensiva. 2020;32(1):2-10
DOI 10.5935/0103-507X.20200002
Views0See moreABSTRACT
Current COVID-19 epidemics was declared on December 31, 2019 at the Wuhan city seafood market, rapidly spreading throughout China, and later reaching several countries (mainly South Korea, Japan, Italy and Iran) and, since March 1, reaching Portugal. Most of the infected patients present with mild symptoms, not requiring hospitalization. Among those admitted to the hospital, 6% to 10% require admission to the intensive care unit. These recommendations are aimed to support the organization of intensive care services to respond COVID-19, providing optimized care to the patient and protection for healthcare professionals.
Search
Search in:
KEY WORDS
Case reports Child Coronavirus infections COVID-19 Critical care Critical illness Extracorporeal membrane oxygenation Infant, newborn Intensive care Intensive care units Intensive care units, pediatric mechanical ventilation Mortality Physical therapy modalities Prognosis Respiration, artificial Respiratory insufficiency risk factors SARS-CoV-2 Sepsis




