You searched for:"Maycon Moura Reboredo"
We found (2) results for your search.-
Original Article
Driving pressure, as opposed to tidal volume based on predicted body weight, is associated with mortality: results from a prospective cohort of COVID-19 acute respiratory distress syndrome patients
Crit Care Sci. 2024;36:e20240208en
Abstract
Original ArticleDriving pressure, as opposed to tidal volume based on predicted body weight, is associated with mortality: results from a prospective cohort of COVID-19 acute respiratory distress syndrome patients
Crit Care Sci. 2024;36:e20240208en
DOI 10.62675/2965-2774.20240208-en
Views27ABSTRACT
Objective:
To evaluate the association between driving pressure and tidal volume based on predicted body weight and mortality in a cohort of patients with acute respiratory distress syndrome caused by COVID-19.
Methods:
This was a prospective, observational study that included patients with acute respiratory distress syndrome due to COVID-19 admitted to two intensive care units. We performed multivariable analyses to determine whether driving pressure and tidal volume/kg predicted body weight on the first day of mechanical ventilation, as independent variables, are associated with hospital mortality.
Results:
We included 231 patients. The mean age was 64 (53 – 74) years, and the mean Simplified Acute and Physiology Score 3 score was 45 (39 – 54). The hospital mortality rate was 51.9%. Driving pressure was independently associated with hospital mortality (odds ratio 1.21, 95%CI 1.04 – 1.41 for each cm H2O increase in driving pressure, p = 0.01). Based on a double stratification analysis, we found that for the same level of tidal volume/kg predicted body weight, the risk of hospital death increased with increasing driving pressure. However, changes in tidal volume/kg predicted body weight were not associated with mortality when they did not lead to an increase in driving pressure.
Conclusion:
In patients with acute respiratory distress syndrome caused by COVID-19, exposure to higher driving pressure, as opposed to higher tidal volume/kg predicted body weight, is associated with greater mortality. These results suggest that driving pressure might be a primary target for lung-protective mechanical ventilation in these patients.
Keywords:acute respiratory distress syndromeCoronavirus infectionsCOVID-19Intensive care unitsMortalityRespiration, artificialTidal VolumeSee more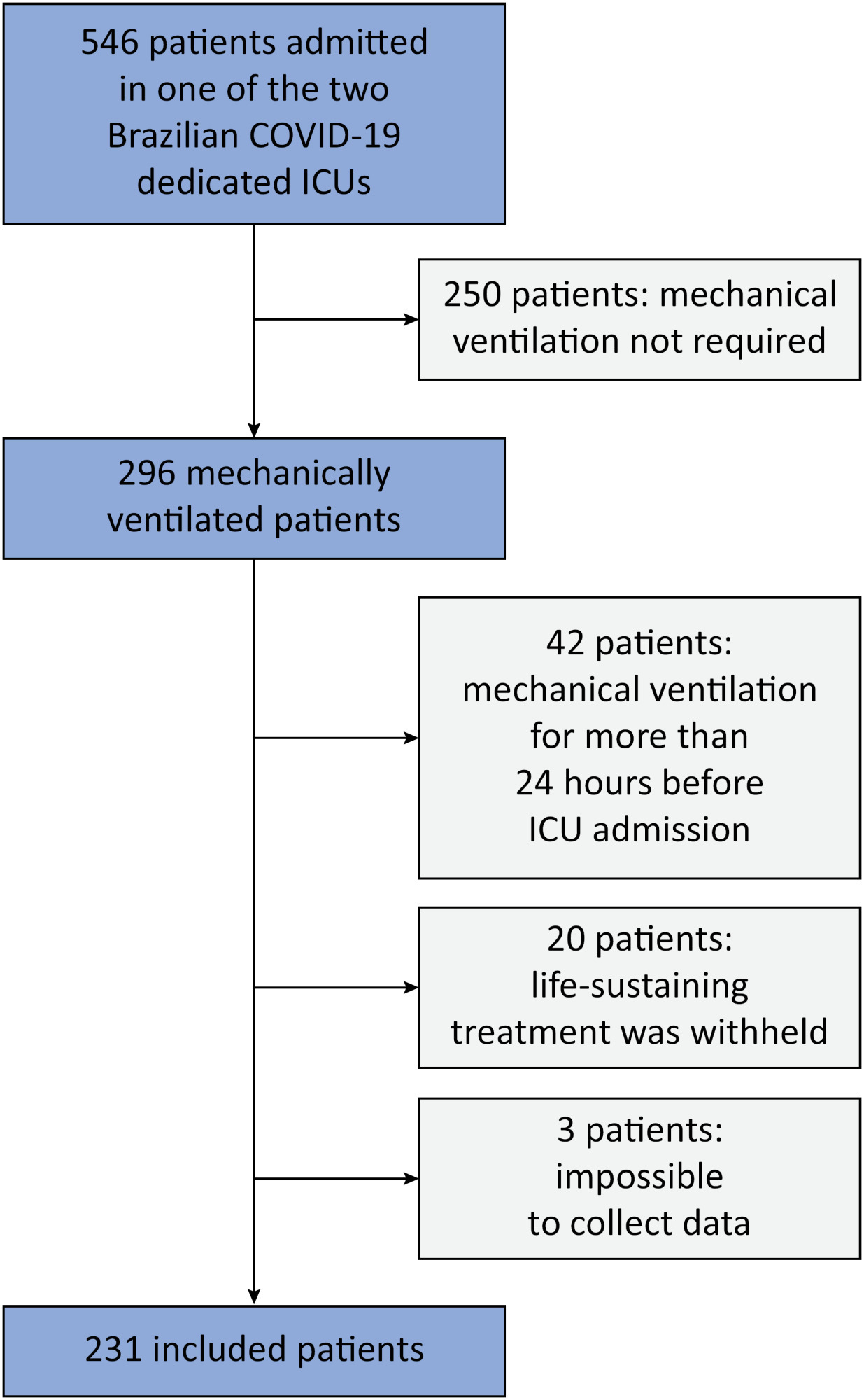
-
Original Article
Effects of atelectatic areas on the surrounding lung tissue during mechanical ventilation in an experimental model of acute lung injury induced by lipopolysaccharide
Crit Care Sci. 2023;35(4):386-393
Abstract
Original ArticleEffects of atelectatic areas on the surrounding lung tissue during mechanical ventilation in an experimental model of acute lung injury induced by lipopolysaccharide
Crit Care Sci. 2023;35(4):386-393
DOI 10.5935/2965-2774.20230190-pt
Views4ABSTRACT
Objective:
To assess the effect of atelectasis during mechanical ventilation on the periatelectatic and normal lung regions in a model of atelectasis in rats with acute lung injury induced by lipopolysaccharide.
Methods:
Twenty-four rats were randomized into the following four groups, each with 6 animals: the Saline-Control Group, Lipopolysaccharide Control Group, Saline-Atelectasis Group, and Lipopolysaccharide Atelectasis Group. Acute lung injury was induced by intraperitoneal injection of lipopolysaccharide. After 24 hours, atelectasis was induced by bronchial blocking. The animals underwent mechanical ventilation for two hours with protective parameters, and respiratory mechanics were monitored during this period. Thereafter, histologic analyses of two regions of interest, periatelectatic areas and the normally-aerated lung contralateral to the atelectatic areas, were performed.
Results:
The lung injury score was significantly higher in the Lipopolysaccharide Control Group (0.41 ± 0.13) than in the Saline Control Group (0.15 ± 0.51), p < 0.05. Periatelectatic regions showed higher lung injury scores than normally-aerated regions in both the Saline-Atelectasis (0.44 ± 0.06 x 0.27 ± 0.74 p < 0.05) and Lipopolysaccharide Atelectasis (0.56 ± 0.09 x 0.35 ± 0.04 p < 0.05) Groups. The lung injury score in the periatelectatic regions was higher in the Lipopolysaccharide Atelectasis Group (0.56 ± 0.09) than in the periatelectatic region of the Saline-Atelectasis Group (0.44 ± 0.06), p < 0.05.
Conclusion:
Atelectasis may cause injury to the surrounding tissue after a period of mechanical ventilation with protective parameters. Its effect was more significant in previously injured lungs.
Keywords:acute respiratory distress syndromeLipopolysaccharidesModels, animalPulmonary atelectasisRespiration, artificialSepsisVentilator-induced lung injurySee more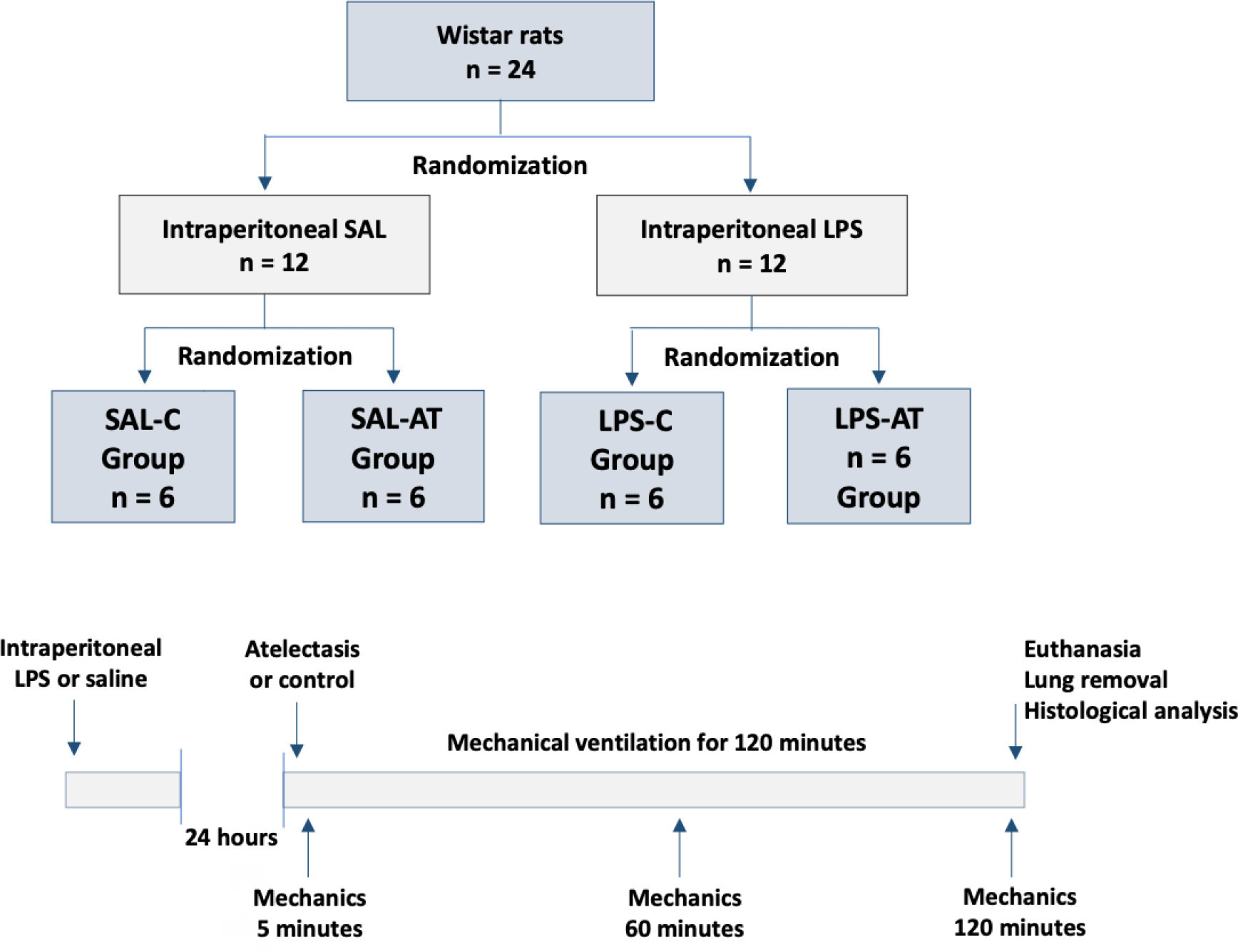
Search
Search in:
KEY WORDS
Case reports Child Coronavirus infections COVID-19 Critical care Critical illness Extracorporeal membrane oxygenation Infant, newborn Intensive care Intensive care units Intensive care units, pediatric mechanical ventilation Mortality Physical therapy modalities Prognosis Respiration, artificial Respiratory insufficiency risk factors SARS-CoV-2 Sepsis




