You searched for:"Luciana Leal do Rego"
We found (1) results for your search.-
Original Article
Delirium severity and outcomes of critically ill COVID-19 patients
- Luciana Leal do Rego
 ,
, - Jorge Ibrain Figueira Salluh
 ,
, - Vicente Cés de Souza-Dantas
 ,
, - José Roberto Lapa e Silva
 ,
, - Pedro Póvoa
 , [ … ],
, [ … ], - Rodrigo Bernardo Serafim

Abstract
Original ArticleDelirium severity and outcomes of critically ill COVID-19 patients
Crit Care Sci. 2023;35(4):394-401
DOI 10.5935/2965-2774.20230170-pt
- Luciana Leal do Rego
 ,
, - Jorge Ibrain Figueira Salluh
 ,
, - Vicente Cés de Souza-Dantas
 ,
, - José Roberto Lapa e Silva
 ,
, - Pedro Póvoa
 ,
, - Rodrigo Bernardo Serafim

Views10ABSTRACT
Objective:
To investigate the impact of delirium severity in critically ill COVID-19 patients and its association with outcomes.
Methods:
This prospective cohort study was performed in two tertiary intensive care units in Rio de Janeiro, Brazil. COVID-19 patients were evaluated daily during the first 7 days of intensive care unit stay using the Richmond Agitation Sedation Scale, Confusion Assessment Method for Intensive Care Unit (CAM-ICU) and Confusion Method Assessment for Intensive Care Unit-7 (CAM-ICU-7). Delirium severity was correlated with outcomes and one-year mortality.
Results:
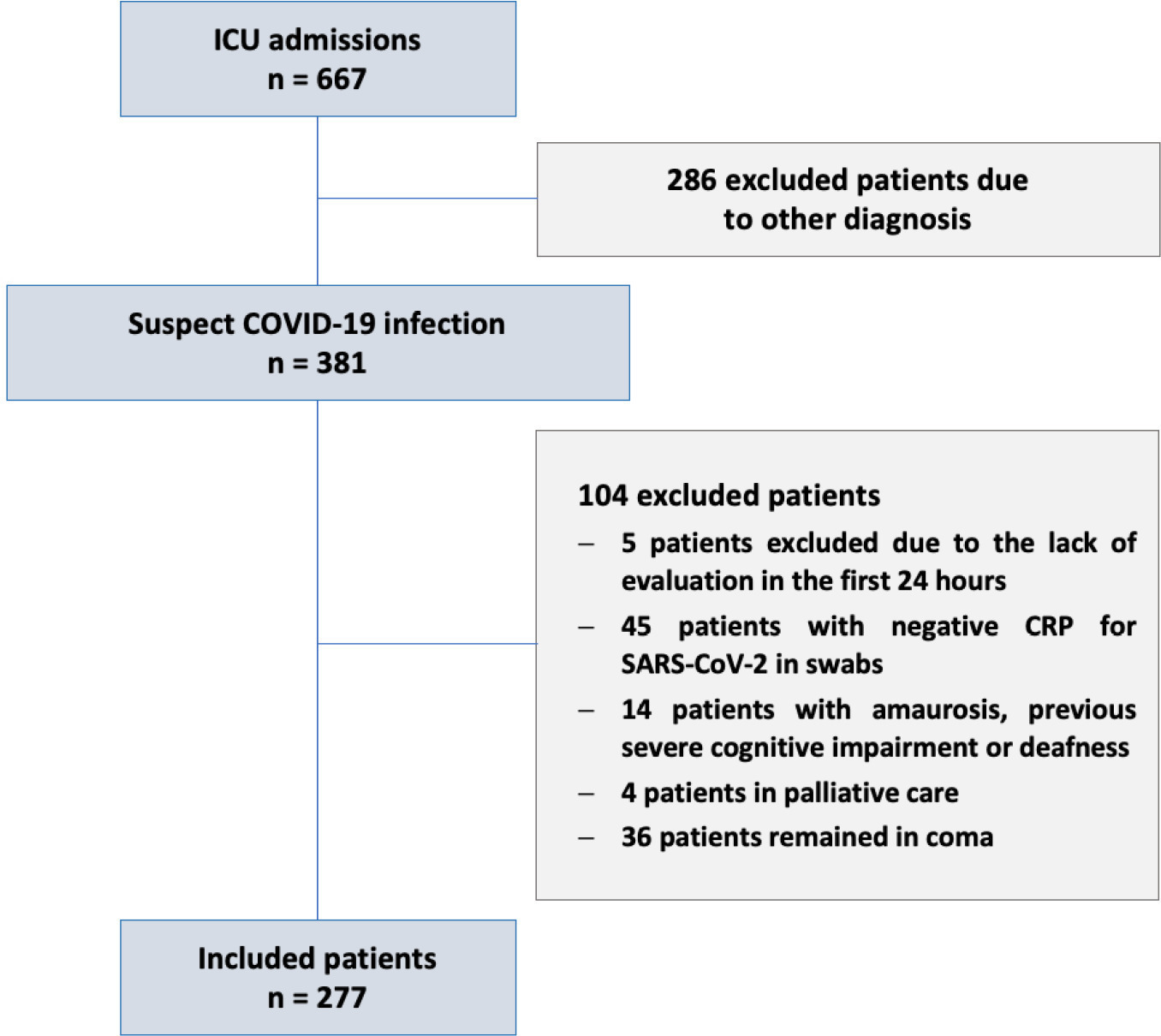
Among the 277 COVID-19 patients included, delirium occurred in 101 (36.5%) during the first 7 days of intensive care unit stay, and it was associated with a higher length of intensive care unit stay in days (IQR 13 [7 – 25] versus 6 [4 – 12]; p < 0.001), higher hospital mortality (25.74% versus 5.11%; p < 0.001) and additional higher one-year mortality (5.3% versus 0.6%, p < 0.001). Delirium was classified by CAM-ICU-7 in terms of severity, and higher scores were associated with higher in-hospital mortality (17.86% versus 34.38% versus 38.46%, 95%CI, p value < 0.001). Severe delirium was associated with a higher risk of progression to coma (OR 7.1; 95%CI 1.9 – 31.0; p = 0.005) and to mechanical ventilation (OR 11.09; 95%CI 2.8 – 58.5; p = 0.002) in the multivariate analysis, adjusted by severity and frailty.
Conclusion:
In patients admitted with COVID-19 in the intensive care unit, delirium was an independent risk factor for the worst prognosis, including mortality. The delirium severity assessed by the CAM-ICU-7 during the first week in the intensive care unit was associated with poor outcomes, including progression to coma and to mechanical ventilation.
Keywords:Coronavirus infectionsCOVID-19Critical care outcomesCritical illnessDeliriumIntensive care unitsPrognosisPsychiatric status rating scalesrisk factorsSurveys and questionnairesSee moreViews10

Abstract
Original ArticleDelirium severity and outcomes of critically ill COVID-19 patients
Crit Care Sci. 2023;35(4):394-401
DOI 10.5935/2965-2774.20230170-pt
- Luciana Leal do Rego
 ,
, - Jorge Ibrain Figueira Salluh
 ,
, - Vicente Cés de Souza-Dantas
 ,
, - José Roberto Lapa e Silva
 ,
, - Pedro Póvoa
 ,
, - Rodrigo Bernardo Serafim

Views10ABSTRACT
Objective:
To investigate the impact of delirium severity in critically ill COVID-19 patients and its association with outcomes.
Methods:
This prospective cohort study was performed in two tertiary intensive care units in Rio de Janeiro, Brazil. COVID-19 patients were evaluated daily during the first 7 days of intensive care unit stay using the Richmond Agitation Sedation Scale, Confusion Assessment Method for Intensive Care Unit (CAM-ICU) and Confusion Method Assessment for Intensive Care Unit-7 (CAM-ICU-7). Delirium severity was correlated with outcomes and one-year mortality.
Results:
Among the 277 COVID-19 patients included, delirium occurred in 101 (36.5%) during the first 7 days of intensive care unit stay, and it was associated with a higher length of intensive care unit stay in days (IQR 13 [7 – 25] versus 6 [4 – 12]; p < 0.001), higher hospital mortality (25.74% versus 5.11%; p < 0.001) and additional higher one-year mortality (5.3% versus 0.6%, p < 0.001). Delirium was classified by CAM-ICU-7 in terms of severity, and higher scores were associated with higher in-hospital mortality (17.86% versus 34.38% versus 38.46%, 95%CI, p value < 0.001). Severe delirium was associated with a higher risk of progression to coma (OR 7.1; 95%CI 1.9 – 31.0; p = 0.005) and to mechanical ventilation (OR 11.09; 95%CI 2.8 – 58.5; p = 0.002) in the multivariate analysis, adjusted by severity and frailty.
Conclusion:
In patients admitted with COVID-19 in the intensive care unit, delirium was an independent risk factor for the worst prognosis, including mortality. The delirium severity assessed by the CAM-ICU-7 during the first week in the intensive care unit was associated with poor outcomes, including progression to coma and to mechanical ventilation.
Keywords:Coronavirus infectionsCOVID-19Critical care outcomesCritical illnessDeliriumIntensive care unitsPrognosisPsychiatric status rating scalesrisk factorsSurveys and questionnairesSee more

- Luciana Leal do Rego
Search
Search in:
KEY WORDS
Case reports Child Coronavirus infections COVID-19 Critical care Critical illness Extracorporeal membrane oxygenation Infant, newborn Intensive care Intensive care units Intensive care units, pediatric mechanical ventilation Mortality Physical therapy modalities Prognosis Respiration, artificial Respiratory insufficiency risk factors SARS-CoV-2 Sepsis


