You searched for:"Flávia Del Castanhel"
We found (2) results for your search.-
Original Article
Needs of family members of patients in intensive care and their perception of medical communication
Crit Care Sci. 2023;35(1):73-83
Abstract
Original ArticleNeeds of family members of patients in intensive care and their perception of medical communication
Crit Care Sci. 2023;35(1):73-83
DOI 10.5935/2965-2774.20230374-pt
Views6ABSTRACT
Objective:
To understand the perception of medical communication and needs of family members with loved ones in intensive care.
Methods:
The study was mainly qualitative and exploratory, with thematic analysis of comments made by 92 family members with loved ones in intensive care units when answering in-person interviews comprising the Quality of Communication Questionnaire (QoC) and open-ended questions about their need for additional help, the appropriateness of the place where they received information, and additional comments.
Results:
The participants’ mean age was 46.8 years (SD = 11.8), and most of them were female, married and had incomplete or completed elementary education. The following themes were found: perception of characteristics of medical communication; feelings generated by communication; considerations about specific questions in the QoC; family members’ needs; and strategies to overcome needs regarding communication. Characteristics that facilitated communication included attention and listening. Characteristics that made communication difficult included aspects of information sharing, such as inaccessible language; lack of clarity, objectivity, sincerity, and agreement among the team; limited time; and inadequate location. Feelings such as shame, helplessness, and sadness were cited when communication was inadequate. Family members’ needs related to communication included more details about the loved one’s diagnosis, prognosis, and health condition; participation in decisionmaking; and being asked about feelings, spirituality, dying and death. Others were related to longer visitation time, psychological support, social assistance, and better infrastructure.
Conclusion:
It is necessary to enhance medical communication and improve hospital infrastructure to improve the quality of care for family members.
Keywords:CommunicationCritical illnessFamilyIntensive care unitsProfessional-family relationsSurveys and questionnairesSee more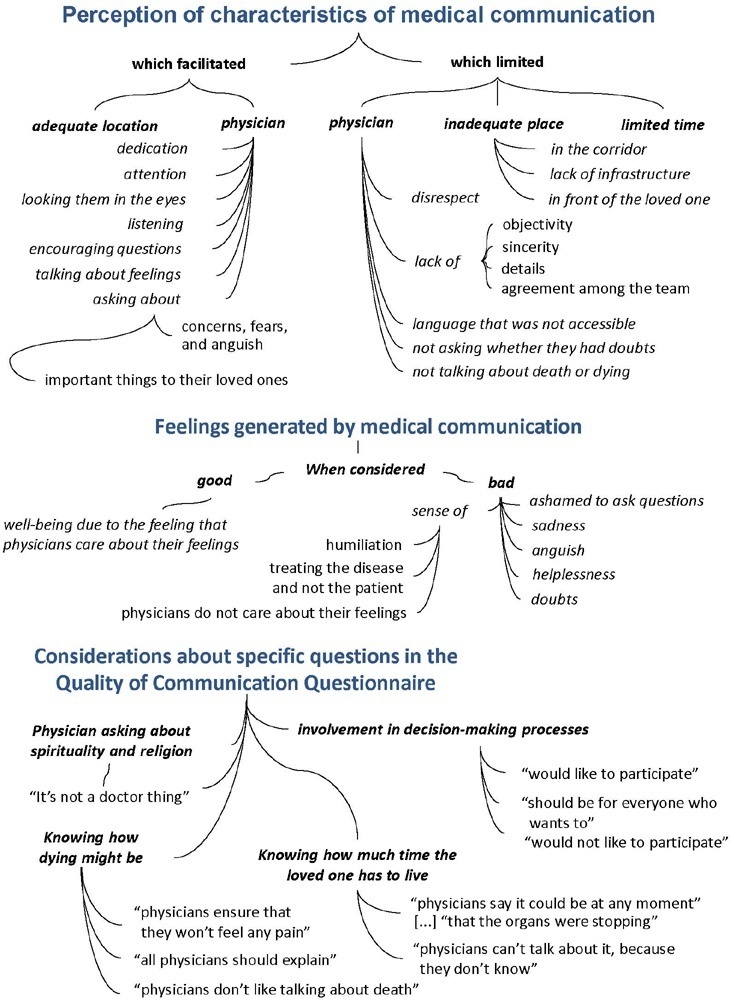
-
Original Article
Patients’ perception of medical communication and their needs during the stay in the intensive care unit
Rev Bras Ter Intensiva. 2021;33(3):401-411
Abstract
Original ArticlePatients’ perception of medical communication and their needs during the stay in the intensive care unit
Rev Bras Ter Intensiva. 2021;33(3):401-411
DOI 10.5935/0103-507X.20210050
Views0ABSTRACT
Objective:
To understand the perception of patients about medical communication as well as their needs during hospitalization in the intensive care unit.
Methods:
This study was cross-sectional descriptive and qualitative exploratory including 103 patients admitted to or recently discharged from the intensive care units of four hospitals in Greater Florianópolis, Santa Catarina state, Brazil. The patients’ sociodemographic and clinical variables were studied, as were the score they gave to the quality of medical communication through the Quality of Communication Questionnaire and their spontaneous comments with reflections or justifications for the scores given, and their responses on how they felt and what complementary help they would have liked to receive. The quantitative data were analyzed by descriptive and analytical statistics, and the qualitative data were analyzed by thematic content analysis.
Results:
The mean Quality of Communication Questionnaire score was 5.1 (standard deviation – SD = 1.3), with 8.6 (SD = 1.3) on the general communication subscale and 2.1 (SD = 1.8) on the end-of-life communication subscale. The patients had a variable understanding of medical language. Some physicians seemed to be “rushed”, according to some patients. Other patients would like to receive more frequent and detailed information and/or be respected and taken “more seriously” when they reported pain. Anxiety, sadness, and fear were among the reported feelings. Other needs included silence, more time for visits, the presence of a companion, psychological and social-work care, a bathroom that they could use, and better food in the intensive care unit.
Conclusion:
The quality of medical communication with patients is good but could improve if physicians and the healthcare team had more time for patients. Other felt needs included respect, pain relief, and adjustments in the intensive care unit dynamics and environment.
Keywords:CommunicationCritical carePatient comfortPatient preferencePatient satisfactionPhysician-patient relationsSee more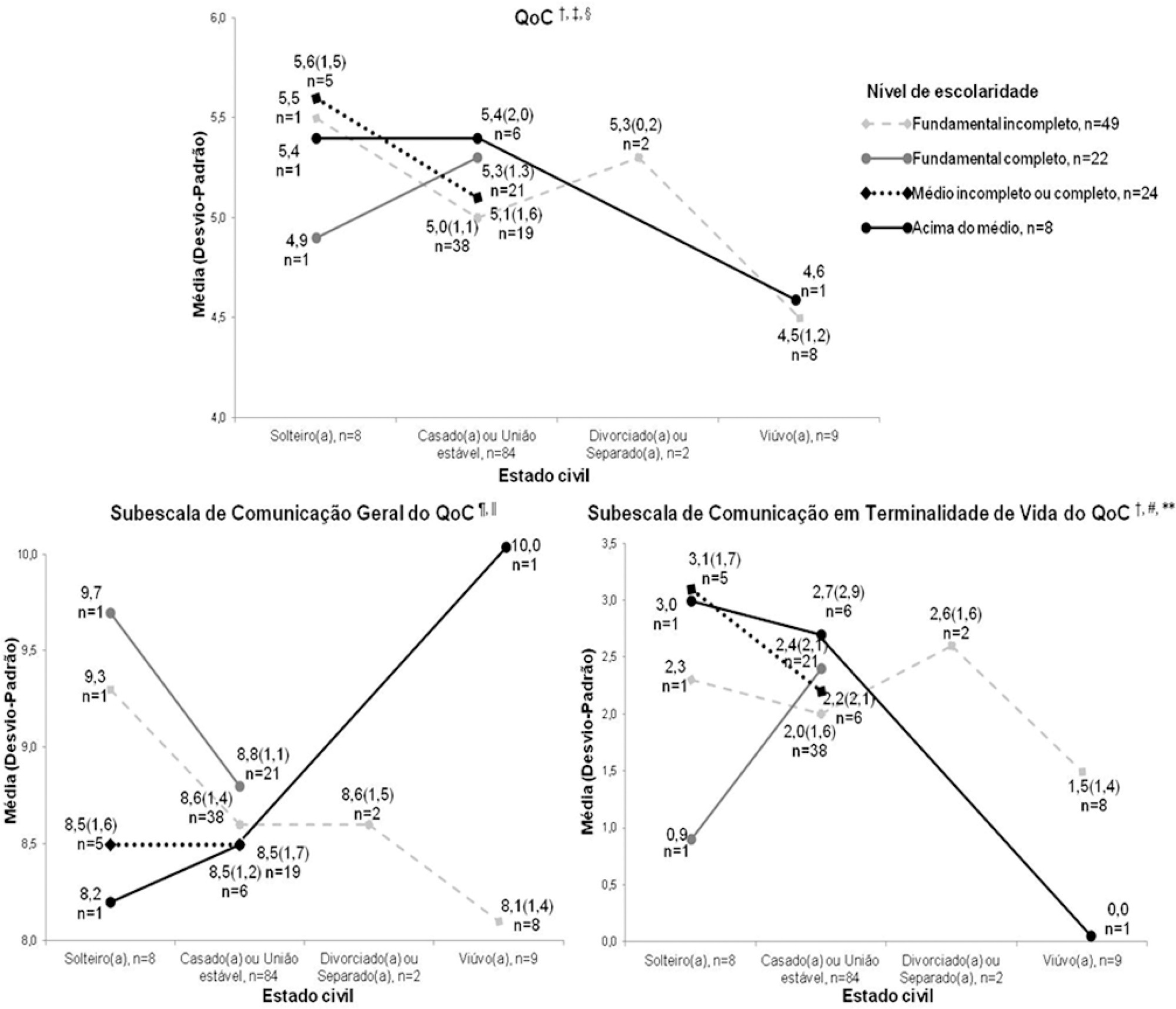
Search
Search in:
KEY WORDS
Case reports Child Coronavirus infections COVID-19 Critical care Critical illness Extracorporeal membrane oxygenation Infant, newborn Intensive care Intensive care units Intensive care units, pediatric mechanical ventilation Mortality Physical therapy modalities Prognosis Respiration, artificial Respiratory insufficiency risk factors SARS-CoV-2 Sepsis




