You searched for:"Fernando Godinho Zampieri"
We found (28) results for your search.-
Original Articles
HLA-A*31 as a marker of genetic susceptibility to sepsis
Rev Bras Ter Intensiva. 2013;25(4):284-289
Abstract
Original ArticlesHLA-A*31 as a marker of genetic susceptibility to sepsis
Rev Bras Ter Intensiva. 2013;25(4):284-289
DOI 10.5935/0103-507X.20130049
Views0See moreObjective:
The HLA haplotype has been associated with many autoimmune diseases, but no associations have been described in sepsis. This study aims to investigate the HLA system as a possible marker of genetic sepsis susceptibility.
Methods:
This is a prospective cohort study including patients admitted to an intensive care unit and healthy controls from a list of renal transplant donors. Patients with less 18 years of age; pregnant or HIV positive patients; those with metastatic malignancies or receiving chemotherapy; or with advanced liver disease; or with end-of-life conditions were excluded. The DNA was extracted from the whole blood and HLA haplotypes determined using MiliPlex® technology.
Results:
From October 2010 to October 2012, 1,121 patients were included (1,078 kidney donors, 20 patients admitted with severe sepsis and 23 with septic shock). HLA-A*31 positive subjects had increased risk of developing sepsis (OR 2.36, 95%CI 1.26-5.35). Considering a p value <0.01, no other significant association was identified.
Conclusion:
HLA-A*31 expression is associated to risk of developing sepsis.
-
Factors associated with variation in intracranial pressure in a model of intra-abdominal hypertension with acute lung injury
Rev Bras Ter Intensiva. 2011;23(2):164-169
Abstract
Factors associated with variation in intracranial pressure in a model of intra-abdominal hypertension with acute lung injury
Rev Bras Ter Intensiva. 2011;23(2):164-169
DOI 10.1590/S0103-507X2011000200008
Views0OBJECTIVE: To evaluate the effects of hemodynamic, respiratory and metabolic changes on intracranial pressure in a model of acute lung injury and abdominal compartment syndrome. METHODS: Eight Agroceres pigs were submitted to five different clinical scenarios after instrumentation: 1) a baseline condition with low intra-abdominal pressure and healthy lungs; 2) pneumoperitoneum with 20 mmHg intra-abdominal pressure; 3) acute lung injury induced by pulmonary lavage with surfactant deactivation; 4) pneumoperitoneum with 20 mmHg intra-abdominal pressure with lung pulmonary injury and low positive end-expiratory pressure; and 5) 27 cmH2O positive end-expiratory pressure with pneumoperitoneum and acute lung injury. Respiratory and hemodynamic variables were collected. A multivariate analysis was conducted to search for variables associated with increased intracranial pressure in the five scenarios. RESULTS: Only plateau airway pressure showed a positive correlation with intracranial pressure in the multivariate analysis. In the models with acute lung injury, plateau airway pressure, CO2 arterial pressure, end tidal CO2 and central venous pressure were positively correlated with increased intracranial pressure. CONCLUSION: In a model of multiple organ dysfunction with associated clinical conditions causing increased intra-thoracic and abdominal pressure, increased intracranial pressure triggered by elevated intra-abdominal pressure is apparently caused by worsened respiratory system compliance and a reduced brain venous drainage gradient due to increased central venous pressure.
Keywords:Acute Lung InjuryCompartment syndromesDiseases models, animalIntensive care unitsIntracranial pressureRespiration, artificialSwineSee more -
Physicochemical characterization of metabolic acidosis induced by normal saline resuscitation of patients with severe sepsis and septic shock
Rev Bras Ter Intensiva. 2011;23(2):176-182
Abstract
Physicochemical characterization of metabolic acidosis induced by normal saline resuscitation of patients with severe sepsis and septic shock
Rev Bras Ter Intensiva. 2011;23(2):176-182
DOI 10.1590/S0103-507X2011000200010
Views0OBJECTIVE: The aim of this study was to characterize and quantify metabolic acidosis that was caused by initial volume expansion during the reanimation of patients with severe sepsis and septic shock. METHODS: A blood sample was drawn for physicochemical characterization of the patient’s acid-base equilibrium both before and after volume expansion using 30 mL/kg 0.9% saline solution. The diagnosis and quantification of metabolic acidosis were based on the standard base excess (SBE). RESULTS: Eight patients with a mean age of 58 ± 13 years and mean APACHE II scores of 20 ± 4 were expanded using 2,000 ± 370 mL of 0.9% saline solution. Blood pH dropped from 7.404 ± 0.080 to 7.367 ± 0.086 (p=0.018), and PC O2 increased from 30 ± 5 to 32 ± 2 mmHg (p=0.215); SBE dropped from -4.4 ± 5.6 to -6.0 ± 5.7 mEq/L (p=0.039). The drop in SBE was associated with the acidifying power of two factors, namely, a significant increase in the strong ion gap (SIG) from 6.1 ± 3.4 to 7.7 ± 4.0 mEq/L (p = 0.134) and a non-significant drop in the apparent inorganic strong ion differences (SIDai) from 40 ± 5 to 38 ± 4 mEq/L (p = 0.318). Conversely, the serum albumin levels decreased from 3.1 ± 1.0 to 2.6 ± 0.8 mEq/L (p = 0.003) with an alkalinizing effect on SBE. Increased serum chloride levels from 103 ± 10 to 106 ± 7 mEq/L (p < 0.001) led to a drop in SIDai. CONCLUSION: Initial resuscitation using 30 mL/kg of 0.9% saline solution for patients with severe sepsis and septic shock is associated with worsened metabolic acidosis, as measured by SBE. This worsened SBE can be ascribed to a serum increase in the levels of unmeasurable anions and chloride.
Keywords:Acid-base equilibriumIntensive care unitsKetosisSaline solution, hypertonic/therapeutic useSepsisShock, septic/therapySee more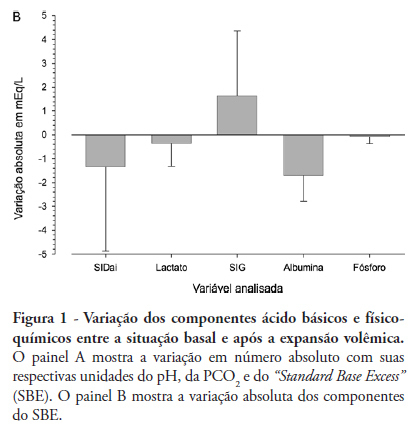
-
Starch solutions for volume resuscitation in intensive care units
Rev Bras Ter Intensiva. 2011;23(1):1-3
Search
Search in:
KEY WORDS
Case reports Child Coronavirus infections COVID-19 Critical care Critical illness Extracorporeal membrane oxygenation Infant, newborn Intensive care Intensive care units Intensive care units, pediatric mechanical ventilation Mortality Physical therapy modalities Prognosis Respiration, artificial Respiratory insufficiency risk factors SARS-CoV-2 Sepsis




