Abstract
Rev Bras Ter Intensiva. 2011;23(1):104-107
DOI 10.1590/S0103-507X2011000100016
Intravesical instillation of bacillus Calmette-Guérin (BCG) is the treatment of choice for carcinoma in situ and non-invasive high-grade superficial tumors of the urinary bladder. This treatment is well tolerated overall, but serious complications can occur. An elderly man with coronary disease and recurrent high-grade superficial carcinoma of the bladder underwent intravesical instillation of BCG and developed septic shock. He received wide range antibiotics, tuberculostatic and vasoactive drugs, corticosteroids, mechanical ventilation and renal replacement therapy without improvement. He died nine days after the intravesical instillation of BCG because of multiple organ failure.
Abstract
Rev Bras Ter Intensiva. 2011;23(1):108-111
DOI 10.1590/S0103-507X2011000100017
A case of a mixed fungal yeast infection involving Saccharomyces cerevisiae - well known for its use in the bread and wine industries - and Candida albicans, is described in an intensive care unit patient. Mortality due to mixed fungal infections in the intensive care unit is high. An elderly smoker patient with chronic pulmonary obstructive disease and untreated bladder neoplasm was admitted to the hospital with diarrhea and progressed to septic shock. The above-mentioned yeasts were identified in blood cultures. This case with fatal outcome provides an opportunity to discuss one of the emergent germs found in the intensive care unit, in a case with an atypical presentation.
Abstract
Rev Bras Ter Intensiva. 2011;23(1):112-113
DOI 10.1590/S0103-507X2011000100018
Abstract
Rev Bras Ter Intensiva. 2011;23(1):113-113
Abstract
Rev Bras Ter Intensiva. 2011;23(1):13-23
DOI 10.1590/S0103-507X2011000100004
Sepsis has a high incidence, mortality and cost and is the main cause of death in intensive care units. Early recognition and treatment have been clearly associated with a better prognosis. Establishing new guidelines is a fundamental step for improving treatment. Patients with clear signs of hypoperfusion should undergo hemodynamic optimization. This guideline addresses the main strategies in the literature that are clinically available.
Abstract
Rev Bras Ter Intensiva. 2011;23(1):24-29
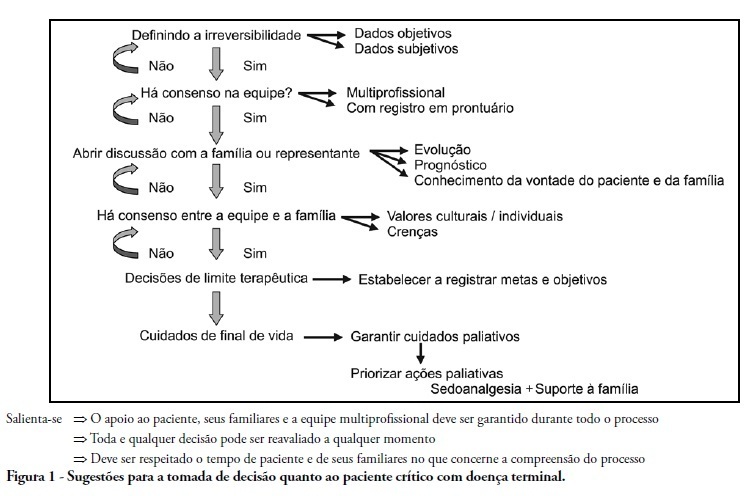
DOI 10.1590/S0103-507X2011000100005
Palliative care is aimed to improve the quality of life of both patients and their family members during the course of life-threatening diseases through the prevention, early identification and treatment of the symptoms of physical, psychological, spiritual and social suffering. Palliative care should be provided to every critically ill patient; this requirement renders the training of intensive care practitioners and education initiatives fundamental. Continuing the Technical Council on End of Life and Palliative Care of the Brazilian Association of Intensive Medicine activities and considering previously established concepts, the II Forum of the End of Life Study Group of the Southern Cone of America was conducted in October 2010. The forum aimed to develop palliative care recommendations for critically ill patients.
Abstract
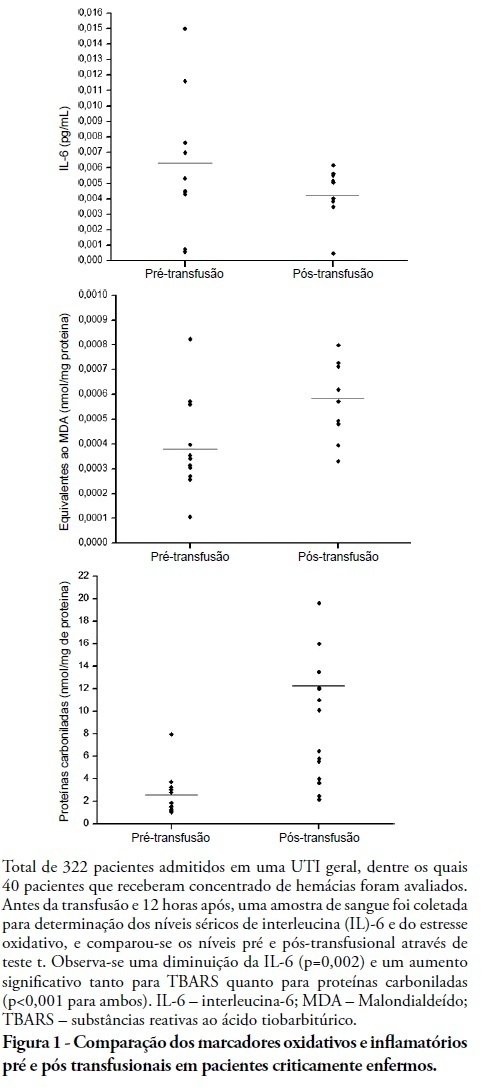
Rev Bras Ter Intensiva. 2011;23(1):30-35
DOI 10.1590/S0103-507X2011000100006
INTRODUCTION: Red blood cell transfusions are common in intensive care units. For many years, transfusions of red blood were thought to have obvious clinical benefits. However, in recent years, the risks and benefits of blood transfusions have been examined more carefully, including the risk of increased morbidity and mortality due to transfusion-related immunomodulation effects. OBJECTIVES: To evaluate red blood cell transfusion effects and the relationship of this procedure to the production of inflammatory cytokines and oxidative damage in critically ill patients admitted to an intensive care unit. METHODS: For 6 months in 2008, we evaluated patients admitted to an intensive care unit who underwent packed red blood cell transfusions. Pre- and post-transfusion levels of interleukin-6, carbonylated proteins and thiobarbituric acid reactive substances were assessed. RESULTS: Serum post-transfusion interleukin-6 levels were reduced, and thiobarbituric acid reactive substances and carbonylated proteins were significantly increased. No statistically significant relationship was found between the levels of pre- and post-transfusion interleukin-6 and thiobarbituric acid reactive substances and the mortality rate. However, there was a significant relationship between levels of post-transfusion carbonylated proteins and mortality. CONCLUSION: Red blood cell transfusion is associated with increased oxidative damage markers and reduced interleukin-6 levels in critically ill patients.