Abstract
Rev Bras Ter Intensiva. 2022;34(4):484-491
DOI 10.5935/0103-507X.20220264-en
To obtain data on bed refusal in intensive care units in Brazil and to evaluate the use of triage systems by professionals.
A cross-sectional survey. Using the Delphi methodology, a questionnaire was created contemplating the objectives of the study. Physicians and nurses enrolled in the research network of the Associação de Medicina Intensiva Brasileira (AMIBnet) were invited to participate. A web platform (SurveyMonkey®) was used to distribute the questionnaire. The variables in this study were measured in categories and expressed as proportions. The chi-square test or Fisher’s exact test was used to verify associations. The significance level was set at 5%.
In total, 231 professionals answered the questionnaire, representing all regions of the country. The national intensive care units had an occupancy rate of more than 90% always or frequently for 90.8% of the participants. Among the participants, 84.4% had already refused admitting patients to the intensive care unit due to the capacity of the unit. Half of the Brazilian institutions (49.7%) did not have triage protocols for admission to intensive beds.
Bed refusal due to high occupancy rates is common in Brazilian intensive care units. Even so, half of the services in Brazil do not adopt protocols for triage of beds.
Abstract
Rev Bras Ter Intensiva. 2020;32(3):412-417
DOI 10.5935/0103-507X.20200070
To evaluate the vacancy and occupancy times of intensive care unit beds; to analyze differences in these times between the day and night shifts and weekdays, weekends, and holidays; and to identify predictors of vacancy and occupancy times.
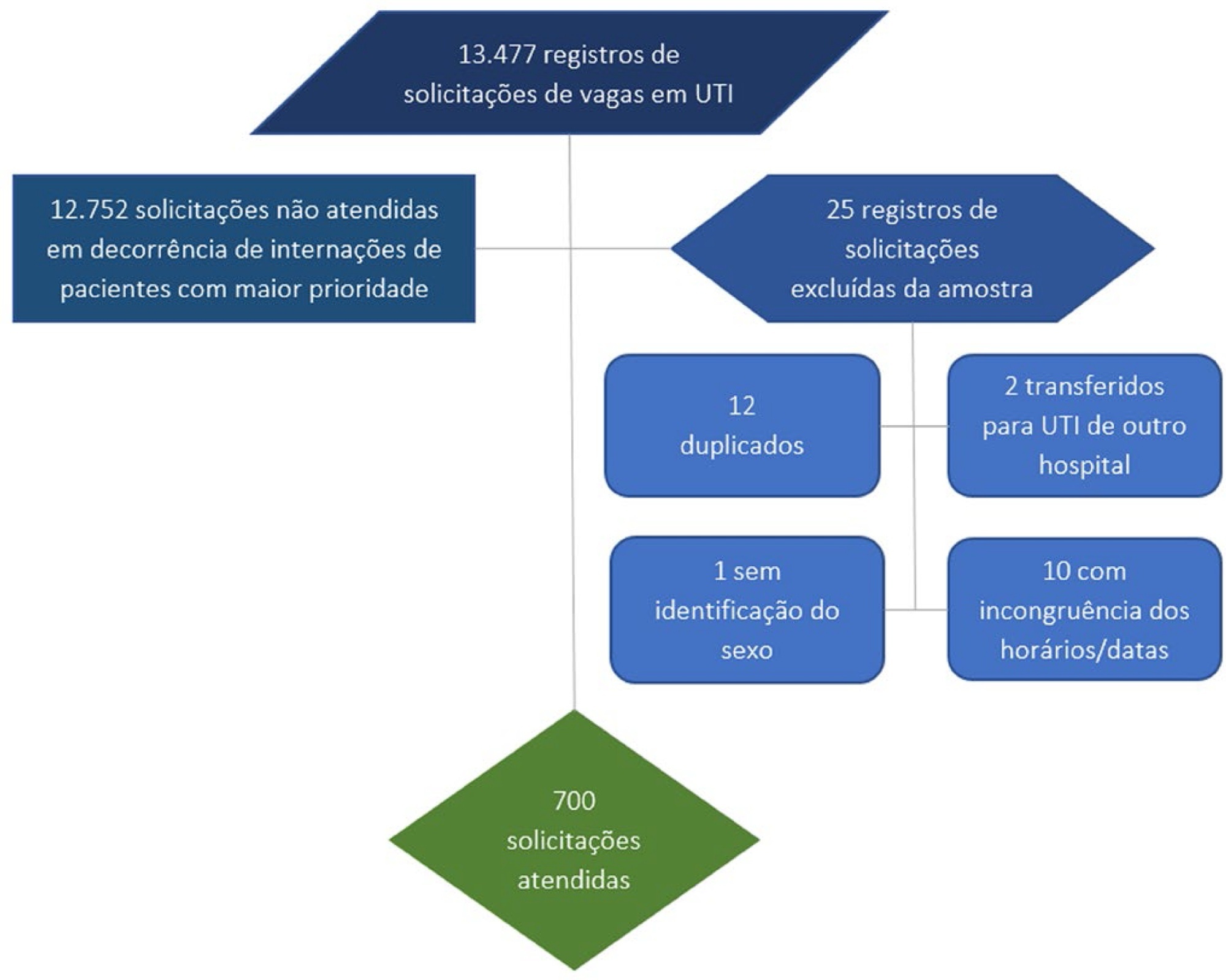
This was a cross-sectional, observational, descriptive, analytical, inferential study. A total of 700 vacancy-to-occupancy records from 54 beds of an adult intensive care unit of a public hospital in Sergipe, Brazil, dated between January and December 2018 were analyzed. The nonparametric Mann-Whitney test was used for comparisons between groups. Several predictive models of length of stay were constructed. The incidence rate ratio was used to estimate the effect size.
During the study period, there were 13,477 requests for the 54 intensive care unit beds, and only 5% (700 patients) were granted. The vacancy-to-occupancy times were shorter when beds were occupied at night (incidence rate ratio of 0.658; 95%CI 0.550 - 0.787; p < 0.0001) or on weekends (incidence rate ratio of 0.566; 95%CI 0.382 - 0.838; p = 0.004). Female sex (incidence rate ratio of 0.749; 95%CI 0.657 - 0.856; p < 0.0001) was a predictor of shorter vacancy-to-occupancy time. This time tended to increase with patient age (incidence rate ratio of 1.006; 95% CI 1.003 - 1.009; p < 0.0001).
Disparities in the waiting time for intensive care unit beds were identified, as the time was greater in the daytime and on weekdays, and women and younger patients experienced shorter vacancy-to-occupancy times.